Oppositional defiant disorder (ODD) is a disruptive behavior disorder characterized by a pattern of angry or irritable mood, argumentative or defiant behavior, or vindictiveness lasting for at least six months. Children and adolescents with ODD may have trouble controlling their temper and are often disobedient and defiant toward others. There are no tools specifically designed for diagnosing ODD, but multiple questionnaires can aid in diagnosis while assessing for other psychiatric conditions. ODD is often comorbid with attention-deficit/hyperactivity disorder, conduct disorder, and mood disorders, including anxiety and depression. Behavioral therapy for the child and family members improves symptoms of ODD. Medications are not recommended as first-line treatment for ODD; however, treatment of comorbid mental health conditions with medications often improves ODD symptoms. Adults and adolescents with a history of ODD have a greater than 90% chance of being diagnosed with another mental illness in their lifetime. They are at high risk of developing social and emotional problems as adults, including suicide and substance use disorders. Early intervention seeks to prevent the development of conduct disorder, substance abuse, and delinquency that can cause lifelong social, occupational, and academic impairments.
Oppositional defiant disorder (ODD) is a disruptive behavior disorder characterized by a pattern of angry or irritable mood, argumentative or defiant behavior, or vindictiveness lasting for at least six months (Table 1).1 Children and adolescents with ODD may have trouble controlling their temper and are often disobedient and defiant toward others. ODD usually manifests in children by late preschool or early elementary school, although it can also begin in adolescence.2,3
BEST PRACTICES IN PSYCHIATRY: RECOMMENDATIONS FROM THE CHOOSING WISELY CAMPAIGN

| Recommendation | Sponsoring organization |
|---|---|
| Do not routinely prescribe antipsychotic medications as a first-line intervention for children and adolescents for any diagnosis other than psychotic disorders. | American Psychiatric Association |
Source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
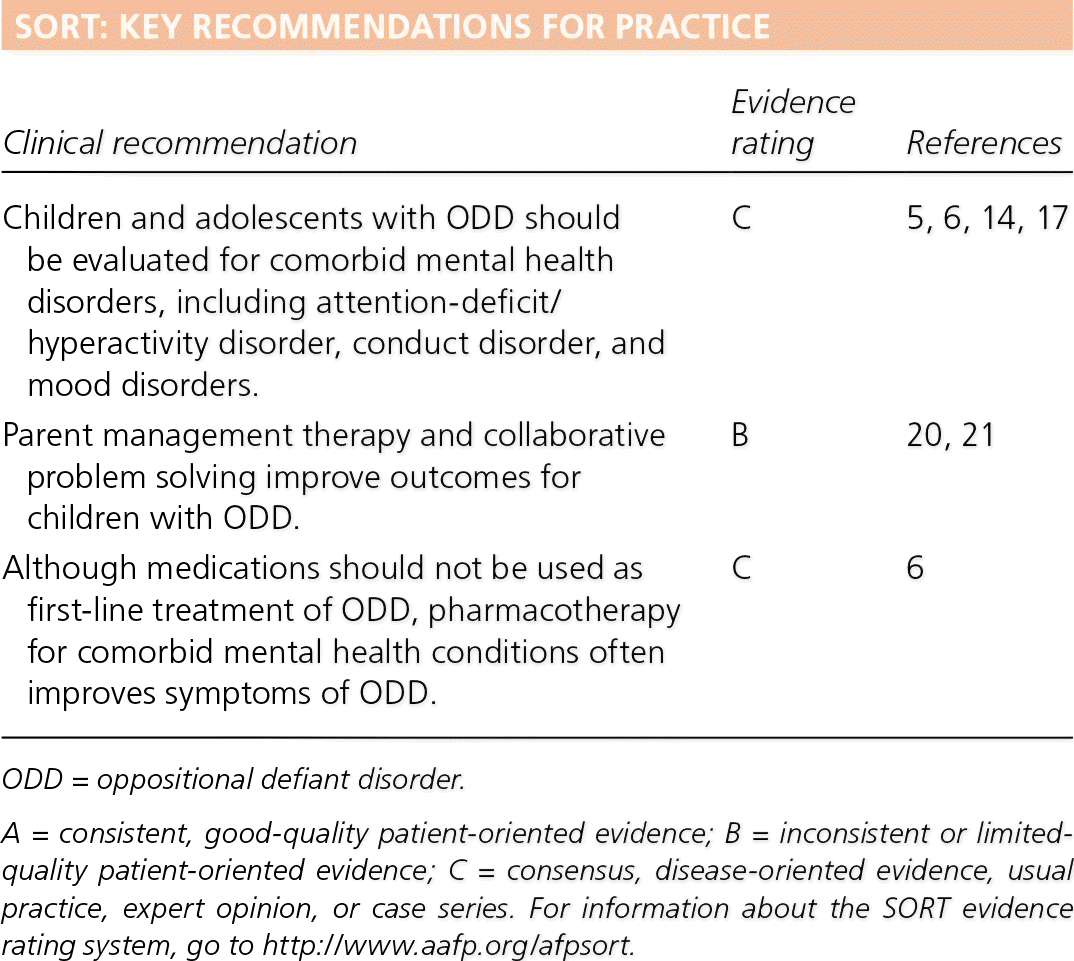
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Children and adolescents with ODD should be evaluated for comorbid mental health disorders, including attention-deficit/hyperactivity disorder, conduct disorder, and mood disorders. | C | 5, 6, 14, 17 |
| Parent management therapy and collaborative problem solving improve outcomes for children with ODD. | B | 20, 21 |
| Although medications should not be used as first-line treatment of ODD, pharmacotherapy for comorbid mental health conditions often improves symptoms of ODD. | C | 6 |
ODD = oppositional defiant disorder.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Table 1. Diagnostic Criteria for Oppositional Defiant Disorder

| A. A pattern of angry/irritable mood, argumentative/defiant behavior, or vindictiveness lasting at least 6 months as evidenced by at least four symptoms from any of the following categories, and exhibited during interaction with at least one individual who is not a sibling. | |
| Angry/Irritable Mood | |
| 1. Often loses temper. | |
| 2. Is often touchy or easily annoyed. | |
| 3. Is often angry and resentful. | |
| Argumentative/Defiant Behavior | |
| 4. Often argues with authority figures or, for children and adolescents, with adults. | |
| 5. Often actively defies or refuses to comply with requests from authority figures or with rules. | |
| 6. Often deliberately annoys others. | |
| 7. Often blames others for his or her mistakes or misbehavior. | |
| Vindictiveness | |
| 8. Has been spiteful or vindictive at least twice within the past 6 months. | |
| B. The disturbance in behavior is associated with distress in the individual or others in his or her immediate social context (e.g., family, peer group, work colleagues), or it impacts negatively on social, educational, occupational, or other important areas of functioning. | |
| C. The behaviors do not occur exclusively during the course of a psychotic, substance use, depressive, or bipolar disorder. Also, the criteria are not met for disruptive mood dysregulation disorder. | |
| Specify current severity: | |
| Mild: Symptoms are confined to only one setting (e.g., at home, at school, at work, with peers). | |
| Moderate: Some symptoms are present in at least two settings. | |
| Severe: Some symptoms are present in three or more settings. | |
Reprinted with permission from the American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 5th ed. Washington, DC: American Psychiatric Association; 2013:462–463.
A systematic review found that the prevalence of ODD is approximately 3.3% across multiple cultures; other reports listed a prevalence of 1% to 16%.3,4 ODD is more common in children who live in poverty, and before adolescence it is slightly more prevalent in boys, although this difference resolves in adolescence.1,4,5 Concern about ODD is among the most common reasons children are referred for mental health services.4
Family physicians are uniquely positioned to help assess children at risk of ODD and refer their families to community programs and resources. Once a child has begun displaying symptoms, prompt diagnosis and referral to local mental health professionals with experience in treating ODD are essential.
What Causes ODD?
The etiology of ODD is not clearly defined. Most experts think it is caused by the cumulative effect of multiple risk factors that stem from biologic, psychological, and social issues. Social support is a protective factor.
EVIDENCE SUMMARY
The etiology of ODD is multifactorial with a cumulative nature. Biologic factors associated with ODD may include nicotine use by parents, prenatal nutritional deficiencies, and developmental delay.6–9 Familial clustering suggests an underlying genetic component, but hereditary connections are variable. Psychological factors associated with ODD may include insecure attachment and unresponsive parents.6 Parental psychopathology, including maternal aggression, is associated with ODD; abuse, harsh punishment, and inconsistent discipline are common correlates.10 Newer studies confirm that parental behavior is likely causal rather than a response to the child's symptoms.11 Additional social factors that may contribute to ODD include poverty, lack of structure, peer rejection, and community violence.6 Protective factors are less clear but include social support, such as peer acceptance and time spent in supportive environments.10
What Are the Diagnostic Criteria?
To meet the Diagnostic and Statistical Manual of Mental Disorders, 5th ed., (DSM-5) diagnostic criteria for ODD, the child must have at least four symptoms of angry/irritable mood, argumentative/defiant behavior, or vindictiveness. Symptoms must be present for at least six months and have a negative impact on social, educational, or occupational functioning.
EVIDENCE SUMMARY
A number of changes in the diagnostic criteria for ODD were made in the DSM-5. Symptoms are now grouped by mood, behaviors, and vindictiveness, and the exclusion criterion for conduct disorder has been removed. Because many oppositional behaviors are a normal part of early childhood and adolescence, the DSM-5 now provides guidance on when these behaviors are a departure from normal development. For example, the DSM-5 notes that temper outbursts for preschool-aged children are common, but they may be abnormal if they occur on most days and are associated with significant impairment, such as being asked to leave school.1
The DSM-5 also provides severity criteria depending on the number of settings in which symptoms are present. In contrast with attention-deficit/hyperactivity disorder (ADHD), in which impairment must be pervasive across multiple settings, ODD symptoms must be present in only one setting to make the diagnosis.1 This means that a child who has no behavioral problems in school may be diagnosed with ODD as a result of oppositional issues at home. However, ODD more commonly causes impairment in multiple settings, and pervasiveness across settings indicates a more severe disorder.12 Children with ODD who have symptoms in only one setting may still have significant problems with current and future adjustment, and warrant further evaluation and treatment.
Are There Tools for Diagnosing ODD?
No questionnaires are specifically designed for diagnosing ODD, but multiple tools can aid in diagnosis while assessing for other psychiatric conditions.
EVIDENCE SUMMARY
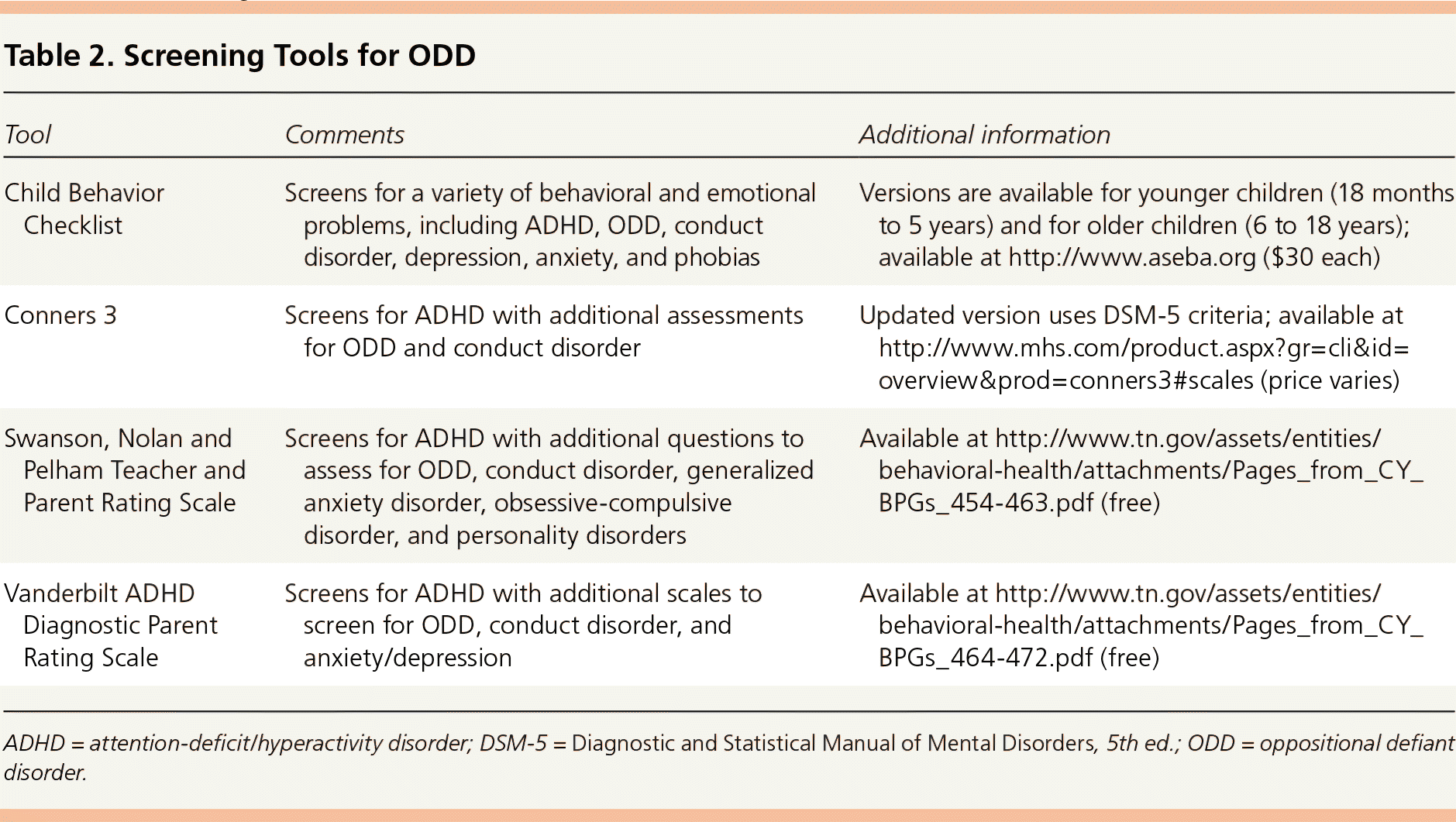
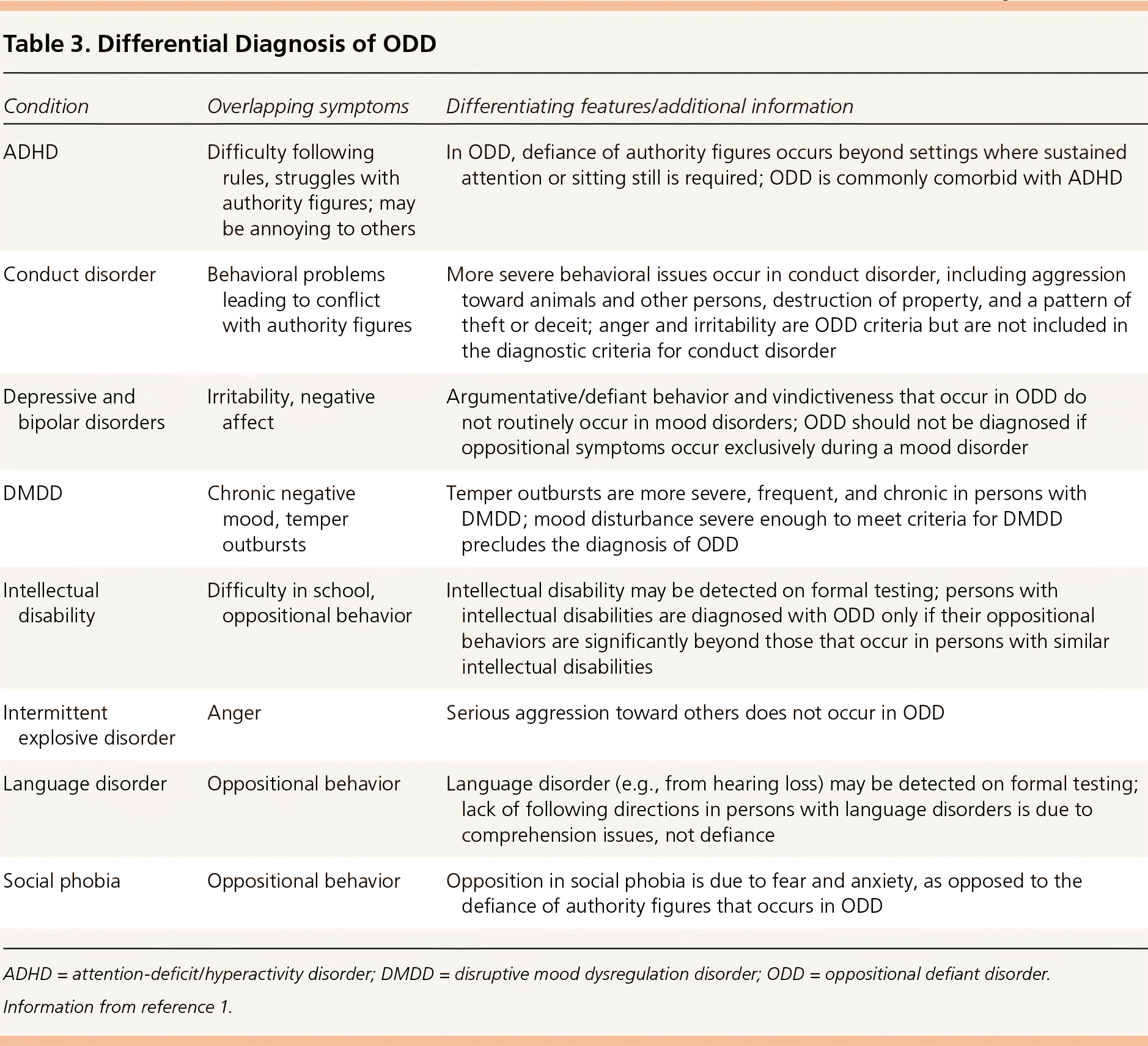
Diagnostic tools for ADHD, such as the Vanderbilt ADHD Diagnostic Parent Rating Scale and the Conners 3 scales, have comorbidity screening scales that can help identify ODD.6,13 One study of the Vanderbilt scale found that affirmative answers (“often” or “very often”) to the items “Actively disobeys or refuses to follow adults' requests or rules” and “Is angry or bitter” had good sensitivity (55% to 88%) and specificity (85% to 94%) for diagnosing ODD.13 Table 2 provides information on these and other tools for identifying behavior disorders; Table 3 lists the differential diagnosis of ODD.1
Table 2. Screening Tools for ODD
| Tool | Comments | Additional information |
|---|---|---|
| Child Behavior Checklist | Screens for a variety of behavioral and emotional problems, including ADHD, ODD, conduct disorder, depression, anxiety, and phobias | Versions are available for younger children (18 months to 5 years) and for older children (6 to 18 years); available at http://www.aseba.org ($30 each) |
| Conners 3 | Screens for ADHD with additional assessments for ODD and conduct disorder | Updated version uses DSM-5 criteria; available at http://www.mhs.com/product.aspx?gr=cli&id=overview&prod=conners3#scales (price varies) |
| Swanson, Nolan and Pelham Teacher and Parent Rating Scale | Screens for ADHD with additional questions to assess for ODD, conduct disorder, generalized anxiety disorder, obsessive-compulsive disorder, and personality disorders | Available at http://www.tn.gov/assets/entities/behavioral-health/attachments/Pages_from_CY_BPGs_454-463.pdf (free) |
| Vanderbilt ADHD Diagnostic Parent Rating Scale | Screens for ADHD with additional scales to screen for ODD, conduct disorder, and anxiety/depression | Available at http://www.tn.gov/assets/entities/behavioral-health/attachments/Pages_from_CY_BPGs_464-472.pdf (free) |
ADHD = attention-deficit/hyperactivity disorder; DSM-5 = Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; ODD = oppositional defiant disorder.
Table 3. Differential Diagnosis of ODD
| Condition | Overlapping symptoms | Differentiating features/additional information |
|---|---|---|
| ADHD | Difficulty following rules, struggles with authority figures; may be annoying to others | In ODD, defiance of authority figures occurs beyond settings where sustained attention or sitting still is required; ODD is commonly comorbid with ADHD |
| Conduct disorder | Behavioral problems leading to conflict with authority figures | More severe behavioral issues occur in conduct disorder, including aggression toward animals and other persons, destruction of property, and a pattern of theft or deceit; anger and irritability are ODD criteria but are not included in the diagnostic criteria for conduct disorder |
| Depressive and bipolar disorders | Irritability, negative affect | Argumentative/defiant behavior and vindictiveness that occur in ODD do not routinely occur in mood disorders; ODD should not be diagnosed if oppositional symptoms occur exclusively during a mood disorder |
| DMDD | Chronic negative mood, temper outbursts | Temper outbursts are more severe, frequent, and chronic in persons with DMDD; mood disturbance severe enough to meet criteria for DMDD precludes the diagnosis of ODD |
| Intellectual disability | Difficulty in school, oppositional behavior | Intellectual disability may be detected on formal testing; persons with intellectual disabilities are diagnosed with ODD only if their oppositional behaviors are significantly beyond those that occur in persons with similar intellectual disabilities |
| Intermittent explosive disorder | Anger | Serious aggression toward others does not occur in ODD |
| Language disorder | Oppositional behavior | Language disorder (e.g., from hearing loss) may be detected on formal testing; lack of following directions in persons with language disorders is due to comprehension issues, not defiance |
| Social phobia | Oppositional behavior | Opposition in social phobia is due to fear and anxiety, as opposed to the defiance of authority figures that occurs in ODD |
ADHD = attention-deficit/hyperactivity disorder; DMDD = disruptive mood dysregulation disorder; ODD = oppositional defiant disorder.
Information from reference 1.
What Are Common Comorbidities with ODD?
ODD is often comorbid with other mental health conditions. The most common are ADHD and conduct disorder, although mood disorders are also common. Substance use and other behavioral problems may also coexist with ODD.
EVIDENCE SUMMARY
ADHD is one of the most common comorbid conditions with ODD, occurring in 14% to 40% of children with the disorder.14,15 Symptoms of ADHD may precede those of ODD. Children with more predominant defiant and headstrong symptoms of ODD are more likely to have comorbid ADHD.2,16 Older studies suggested that conduct disorder may be a more severe, age-related progression of ODD, although more recent evidence suggests that they are distinct disorders.2,12,14 Retrospective studies estimate that conduct disorder is comorbid in up to 42% of persons with ODD.4,14 Those with comorbid ADHD and ODD or conduct disorder and ODD tend to have more severe and persistent behavioral problems and are more likely to have additional comorbid mood disorders.6,17 They are also at higher risk of substance use and abuse.17
Anxiety and depression are commonly associated with ODD, developing as early as preschool age.2,5,14 One study found that up to 14% of persons with ODD also have anxiety, and 9% have a depressive disorder.15 A more recent study found even higher rates; at least 50% of participants with ODD had comorbid anxiety or depression.14 Those with angry and irritable symptoms of ODD are at higher risk of comorbid mood disorders, whereas those with argumentative, defiant, and vindictive symptoms are at higher risk of conduct disorder.16
Which Behavioral Treatments Are Effective?
Individualized treatment plans by mental health professionals for both the child and family are the most effective. Behavioral parenting interventions are first-line therapy in younger children. In adolescence, individual therapy takes a more prominent role, but outcomes are better when parents are involved. Early intervention may help prevent other disorders, such as conduct disorder, substance abuse, and delinquency.
EVIDENCE SUMMARY
Child-based therapy often focuses on problem-solving skills, whereas parent training (parent management therapy) focuses on how to respond to the child's behavior. Parent management therapy aims to help parents manage disruptive behavior by decreasing unintentional positive reinforcement of disruptive behaviors, to help them understand appropriate consequences and punishments for disruptive behaviors, and to help them make their response timely, predictable, and appropriate. Overall, the goal is for parents to be more positive and less harsh.6 A 2012 Cochrane review found that group parenting interventions based on behavioral therapy and cognitive behavior therapy (CBT) are effective and cost-effective for improving child conduct problems, parental mental health, and parenting skills in the short term.18 Group CBT for children has also been found to decrease aggressive behaviors.19
Collaborative problem solving, in which parents and children work together, is another effective technique for treating ODD.20 A 2015 trial found collaborative problem solving to be as effective as parent management therapy.21 In both treatment arms, 50% of children no longer met criteria for ODD after six months.
Can Pharmacologic Treatment Help?
Medications are not recommended as first-line treatment for ODD, but they may be helpful in some situations when used in conjunction with behavioral interventions. Treatment of comorbid conditions often improves symptoms of ODD. 6Mood stabilizers and atypical antipsychotics may be helpful for aggressive behaviors, but have limited data for ODD.
EVIDENCE SUMMARY
Stimulants can help improve oppositional symptoms in persons with comorbid ADHD, whereas atomoxetine (Strattera) has mixed evidence for reduction of ODD symptoms.22,23 Clonidine has also proved effective in managing concomitant ADHD and ODD.24
Antidepressant therapy in persons with concomitant depression and ODD can help both disorders. One study found that fluoxetine (Prozac), with or without CBT, improves comorbid ODD.25 Fluoxetine plus CBT was superior to CBT alone, but ODD symptoms improved in all treated groups.
The broader literature on conduct disorder suggests that mood stabilizers and atypical antipsychotics may be helpful for managing aggressive behavior. A 2012 Cochrane review found limited evidence that atypical antipsychotics help with aggression and conduct problems in children five to 18 years of age.26 The evidence was strongest for risperidone (Risperdal), and there was no evidence to support the use of quetiapine (Seroquel) in this population.
What Is the Natural History of ODD?
ODD does not have a consistent course. Symptoms often resolve by early adulthood, although other mental health problems, such as mood disorders and social impairment, may persist or develop.
EVIDENCE SUMMARY
The normal course of ODD is not well defined. One study showed that 70% of persons with ODD had symptom resolution by 18 years of age.14 However, ODD can persist into adulthood, and earlier onset of symptoms and male sex predict more severe psychopathology.6,14
Environmental factors such as family instability, low may increase the risk of conduct disorder in persons with ODD.2,4 Because antisocial personality disorder is considered a more severe adult form of conduct disorder, children with ODD and comorbid conduct disorder are at risk of developing antisocial personality disorder.6
Adults and adolescents with a history of ODD have a greater than 90% chance of being diagnosed with another mental illness in their lifetime.14 They are at high risk of social and emotional problems as adults, including suicide. They also have a higher risk of mood disorders, such as anxiety, depression, and bipolar disorder, and high rates of substance use disorders.2,17,27,28 Early intervention is aimed at preventing the development of conduct disorder, substance abuse, and delinquency that can cause lifelong social, occupational, and academic impairments.
Can ODD Be Prevented?
Programs that improve social skills, conflict resolution, and anger management in preschool-aged children to adolescents can reduce the risk of ODD. These programs are often embedded in existing community programs that serve high-risk youth, such as Head Start, or in elementary or secondary school curricula.
EVIDENCE SUMMARY
Integrating behavioral programs for preventing conduct problems into existing programs such as Head Start has had a positive impact. One example, the Incredible Years program (http://www.incredibleyears.com), has been found to improve social competence and emotional self-regulation and decrease conduct issues. This program has content for parents, children, educators, and clinicians.29,30 Other programs for adolescents concentrate on CBT-based interventions, skills training, vocational training, and academic preparation. A comprehensive list of programs and resources is available on the American Academy of Child and Adolescent Psychiatry's website (https://www.aacap.org/aacap/Families_and_Youth/Resource_Centers/Oppositional_Defiant_Disorder_Resource_Center/Home.aspx).6,31
Data Sources: A PubMed search was completed in Clinical Queries using the key term oppositional defiant disorder. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. A search was also performed using Essential Evidence Plus. Search dates: January 2015 through December 2015.

