Communication skills needed for patient-centered care include eliciting the patient's agenda with open-ended questions, especially early on; not interrupting the patient; and engaging in focused active listening. Understanding the patient's perspective of the illness and expressing empathy are key features of patient-centered communication. Understanding the patient's perspective entails exploring the patient's feelings, ideas, concerns, and experience regarding the impact of the illness, as well as what the patient expects from the physician. Empathy can be expressed by naming the feeling; communicating understanding, respect, and support; and exploring the patient's illness experience and emotions. Before revealing a new diagnosis, the patient's prior knowledge and preferences for the depth of information desired should be assessed. After disclosing a diagnosis, physicians should explore the patient's emotional response. Shared decision making empowers patients by inviting them to consider the pros and cons of different treatment options, including no treatment. Instead of overwhelming the patient with medical information, small chunks of data should be provided using repeated cycles of the “ask-tell-ask” approach. Training programs on patient-centered communication for health care professionals can improve communication skills.
The Institute of Medicine identified patient-centered care as one of six elements of high-quality health care.1 A patient-centered approach to care is based on three goals1–3: eliciting the patient's perspective on the illness, understanding the patient's psychosocial context, and reaching shared treatment goals based on the patient's values. Patient-centered care builds on discussions and decisions that involve shared information, compassionate and empowering care provision, sensitivity to patient needs, and relationship building.3 In contrast to a disease-focused biomedical approach, patient-centered care considers patient preferences, needs, and values, ensuring that they guide all medical decisions in tandem with scientific evidence.1 Although most patients (about 70%) prefer patient-centered communication, it is difficult to predict preferences for an interviewing style (patient-centered vs. disease-focused) based on the patient's age, sex, or ethnicity.4 This article provides an overview of patient-centered communication techniques for physicians. Table 1 outlines a sequence for medical interviewing that incorporates patient-centered elements.
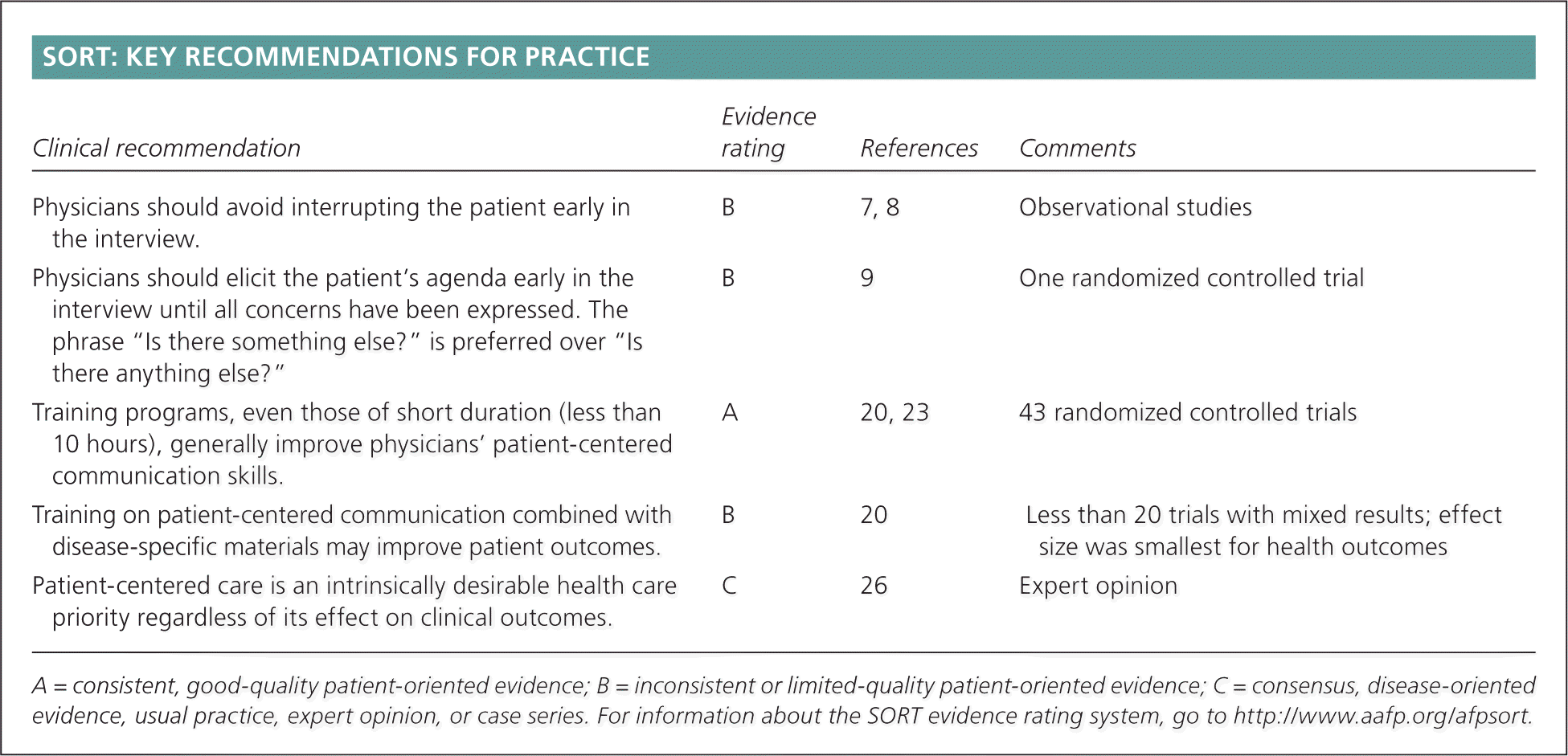
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| Physicians should avoid interrupting the patient early in the interview. | B | 7, 8 | Observational studies |
| Physicians should elicit the patient's agenda early in the interview until all concerns have been expressed. The phrase “Is there something else?” is preferred over “Is there anything else?” | B | 9 | One randomized controlled trial |
| Training programs, even those of short duration (less than 10 hours), generally improve physicians' patient-centered communication skills. | A | 20, 23 | 43 randomized controlled trials |
| Training on patient-centered communication combined with disease-specific materials may improve patient outcomes. | B | 20 | Less than 20 trials with mixed results; effect size was smallest for health outcomes |
| Patient-centered care is an intrinsically desirable health care priority regardless of its effect on clinical outcomes. | C | 26 | Expert opinion |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
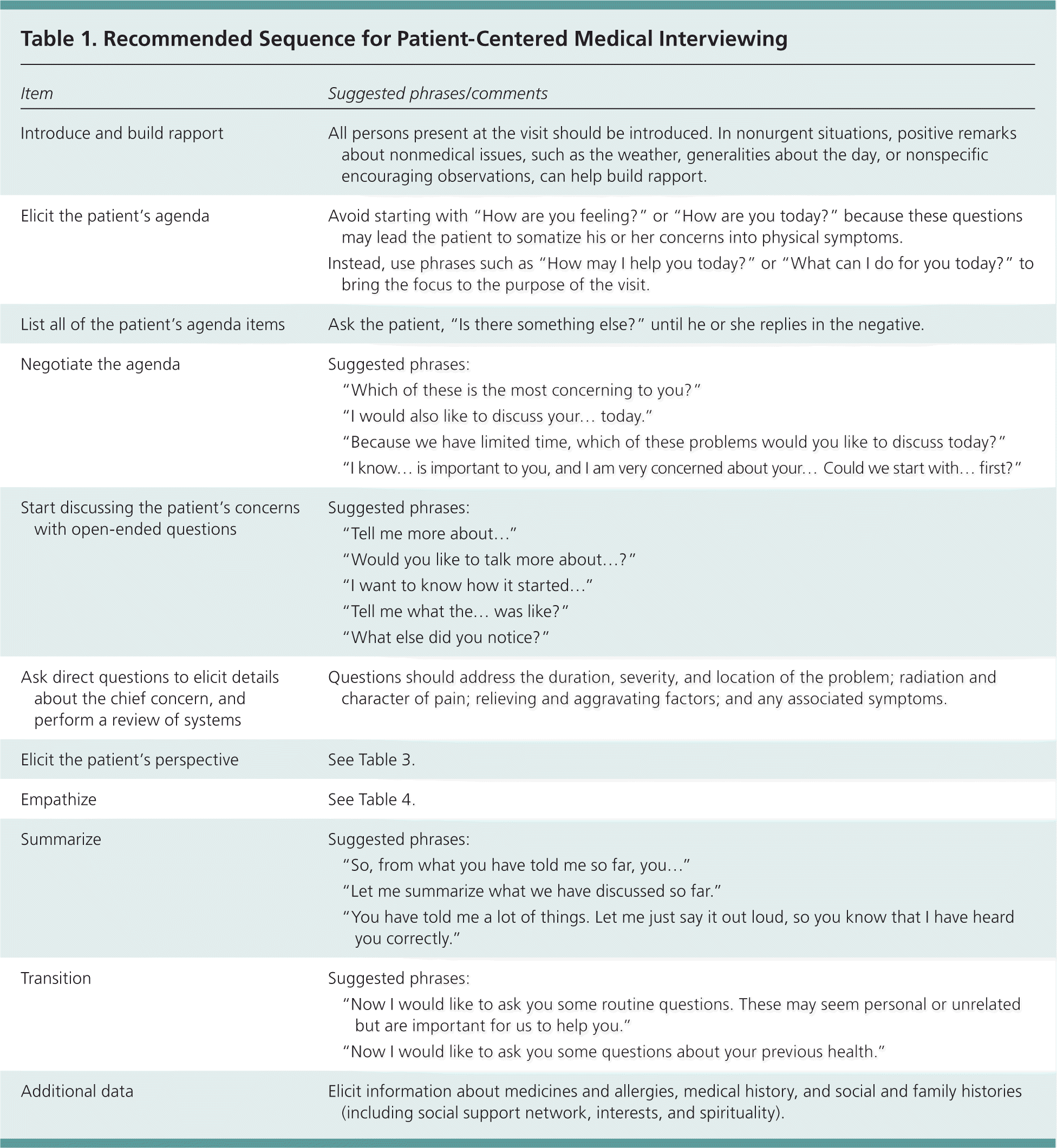
Table 1. Recommended Sequence for Patient-Centered Medical Interviewing
| Item | Suggested phrases/comments | |
|---|---|---|
| Introduce and build rapport | All persons present at the visit should be introduced. In nonurgent situations, positive remarks about nonmedical issues, such as the weather, generalities about the day, or nonspecific encouraging observations, can help build rapport. | |
| Elicit the patient's agenda | Avoid starting with “How are you feeling?” or “How are you today?” because these questions may lead the patient to somatize his or her concerns into physical symptoms. | |
| Instead, use phrases such as “How may I help you today?” or “What can I do for you today?” to bring the focus to the purpose of the visit. | ||
| List all of the patient's agenda items | Ask the patient, “Is there something else?” until he or she replies in the negative. | |
| Negotiate the agenda | Suggested phrases: | |
| “Which of these is the most concerning to you?” | ||
| “I would also like to discuss your… today.” | ||
| “Because we have limited time, which of these problems would you like to discuss today?” | ||
| “I know… is important to you, and I am very concerned about your… Could we start with… first?” | ||
| Start discussing the patient's concerns with open-ended questions | Suggested phrases: | |
| “Tell me more about…” | ||
| “Would you like to talk more about…?” | ||
| “I want to know how it started…” | ||
| “Tell me what the… was like?” | ||
| “What else did you notice?” | ||
| Ask direct questions to elicit details about the chief concern, and perform a review of systems | Questions should address the duration, severity, and location of the problem; radiation and character of pain; relieving and aggravating factors; and any associated symptoms. | |
| Elicit the patient's perspective | See Table 3. | |
| Empathize | See Table 4. | |
| Summarize | Suggested phrases: | |
| “So, from what you have told me so far, you…” | ||
| “Let me summarize what we have discussed so far.” | ||
| “You have told me a lot of things. Let me just say it out loud, so you know that I have heard you correctly.” | ||
| Transition | Suggested phrases: | |
| “Now I would like to ask you some routine questions. These may seem personal or unrelated but are important for us to help you.” | ||
| “Now I would like to ask you some questions about your previous health.” | ||
| Additional data | Elicit information about medicines and allergies, medical history, and social and family histories (including social support network, interests, and spirituality). | |
Eliciting the Patient's Agenda
Patient-centered medical interviewing should begin with the introduction of all persons present at the visit. This includes the physician and the patient, and anyone else in the room, specifying their relationship to the patient. In nonurgent situations, positive remarks about nonmedical issues such as the weather, generalities about the day, or non-specific encouraging observations can help build rapport. New patients should be welcomed to the clinic. Avoid opening the interview with “How are you feeling?” or “How are you today?” because these questions may lead the patient to somatize their concerns into physical symptoms.5 Instead, the open-ended question “How can I help you today?” brings focus to the purpose of the visit, enabling patients to discuss anything relevant to their health, and emphasizes the physician's role as a helper. It is the preferred initial statement for initial and follow-up visits.6
On average, physicians tend to interrupt a patient within 16 seconds of asking an opening question.7 Allowing patients to speak uninterrupted may take an average of just six seconds longer than redirecting them.8 More significantly, allowing patients to speak reduces late-arising concerns. Because patients often present with more than one concern (on average, 1.7 concerns per visit; range, one to four),9 physicians should continue to ask “Is there something else?” until the patient replies in the negative. Using the term “something” is more effective than “anything” in eliciting concerns without increasing the duration of the visit.9
Physicians may prioritize concerns based on patient preferences and medical urgency. Low-priority concerns can be deferred to a future visit. The primary concern should initially be explored using open-ended phrases: “Tell me more about…” This should be followed by a silent pause and, if needed, nonverbal facilitation. Patients can thus express themselves in an atmosphere of nonjudgmental acceptance, often providing valuable diagnostic information that they may not provide with closed-ended questions. Focused active listening by the physician is critical at this stage, and distracting activities (e.g., reviewing the patient's medical record) should be avoided while the patient is talking. Later in the interview, after the patient appears to have expressed his or her concerns, physicians can interleave the conversation with brief reviews of the medical record. Documentation should be completed after the patient has left the room. Table 2 includes examples of verbal and nonverbal methods for facilitating patient-centered communication.
Table 2. Verbal and Nonverbal Methods for Facilitating Patient-Centered Communication

| Method | Examples |
|---|---|
| Verbal | |
| Continuers | “Go on,” “I hear you,” “Hmmm,” “Aha” |
| Legitimation | “That makes sense.” |
| Open-ended questions | “Tell me more about...” |
| Understanding | “It seems like …” |
| Exploration | “I wonder if you …” |
| Rephrasing | “Let me summarize what you have told me so far…” |
| Checking the patient's understanding | “Could you summarize what we have discussed so far?” |
| Nonverbal | |
| Attention | Judicious eye contact |
| Responsiveness | Facial expressions such as grinning, lip biting, concerned frowning |
| Attentiveness | Holding of chin, keeping index finger on temple |
| Openness | Palms exposed, avoiding crossed arms or legs |
| Interest | Leaning forward |
| Active listening | Head nodding |
| Focus | Purposefully turning away from the computer or medical file |
| Tactful silent pauses | |
| Avoiding interrupting or completing sentences | |
Direct questions can elicit specifics about the patient's chief concern, including the duration, severity, and location of the problem; radiation and character of pain; relieving and aggravating factors; and any associated symptoms. This part of the medical interview is often biomedical in focus and assists in determining a working diagnosis. Additional questions are guided by hypothesis-driven clinical reasoning as the patient's story unfolds and the differential diagnosis is narrowed. Although the review of systems has traditionally been the last item in the medical interview, it should be obtained after the history of presenting illness because it can support diagnostic reasoning.
Understanding the Patient's Perspective
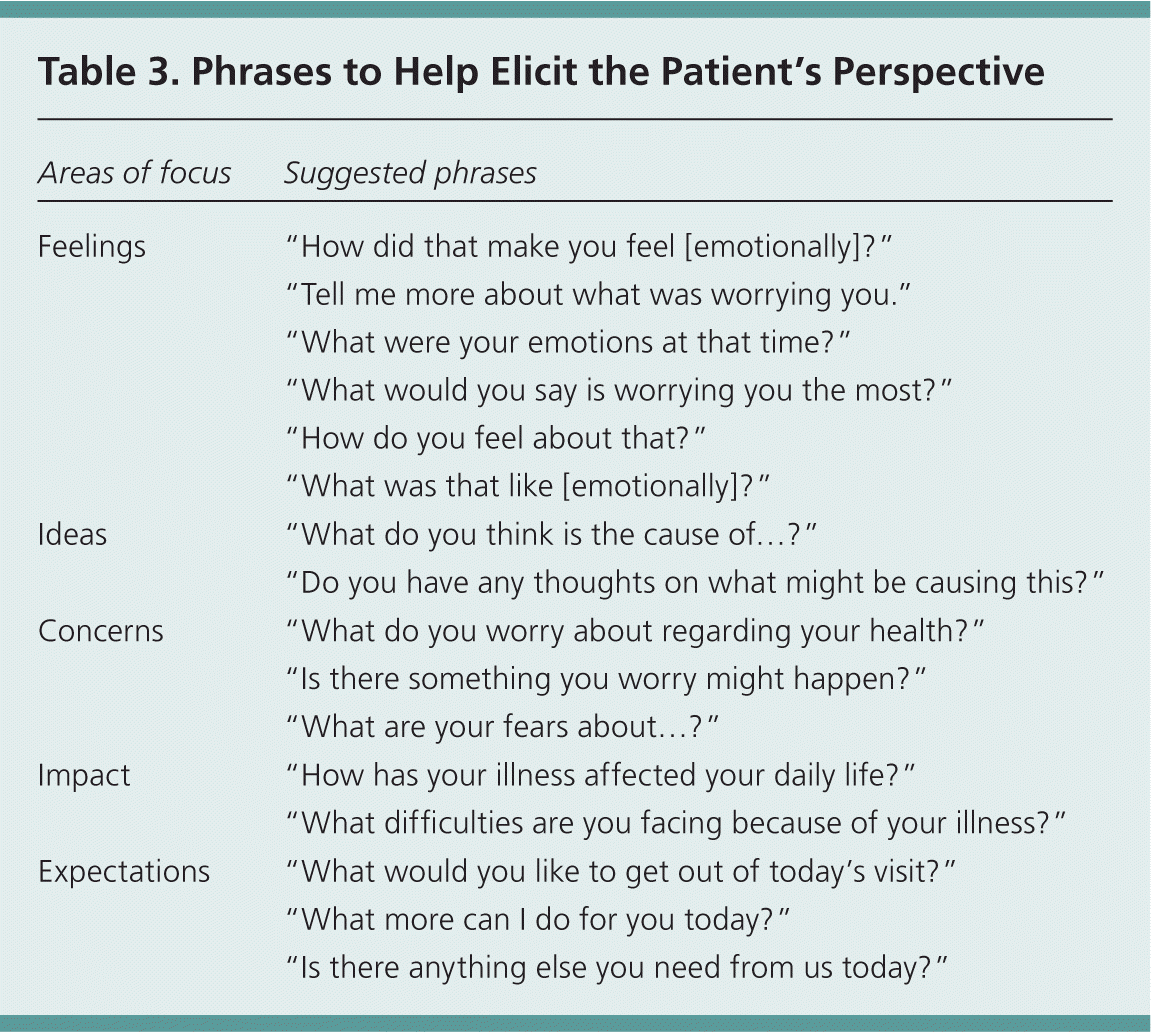
The patient's views of his or her illness are a primary focus of patient-centered care. The patient's perspective includes feelings, ideas, concerns, impact, and expectations. Asking the patient about his or her understanding of the cause of the illness may provide additional diagnostic clues. Understanding the patient's beliefs allows the physician to appreciate the cultural context of the illness. Thus, physicians can avoid recommending interventions that go against the patient's views. Table 3 includes phrases that can be used to help in understanding the patient's perspective.
Table 3. Phrases to Help Elicit the Patient's Perspective
| Areas of focus | Suggested phrases |
|---|---|
| Feelings | “How did that make you feel [emotionally]?” |
| “Tell me more about what was worrying you.” | |
| “What were your emotions at that time?” | |
| “What would you say is worrying you the most?” | |
| “How do you feel about that?” | |
| “What was that like [emotionally]?” | |
| Ideas | “What do you think is the cause of…?” |
| “Do you have any thoughts on what might be causing this?” | |
| Concerns | “What do you worry about regarding your health?” |
| “Is there something you worry might happen?” | |
| “What are your fears about…?” | |
| Impact | “How has your illness affected your daily life?” |
| “What difficulties are you facing because of your illness?” | |
| Expectations | “What would you like to get out of today's visit?” |
| “What more can I do for you today?” | |
| “Is there anything else you need from us today?” |
Exploring the patient's feelings is important in assessing the emotional burden and psychological impact of the illness. Unexpressed emotions may impede the patient's trust and confidence in medical care. Physicians should not judge the patient's emotions as being appropriate or inappropriate and resist offering premature reassurance early in the medical encounter.10 Similarly, normalizing (“Many of my patients experience this” or “This is a fairly common reaction”) without first adequately exploring the concern may be perceived as blocking the patient's feelings.
Patients often have concerns about future complications and disability from their medical problems. Some of these fears may be unfounded or unlikely, requiring gentle exploration and eventual reassurance. Other fears are realistic and require a thorough understanding of the patient's values and resources. The patient's fears may help the physician understand the patient's priorities in managing the disease. Physicians can thus ensure that the treatment plan addresses these concerns. An illness can impact a patient's life in ways that the physician may not anticipate. Discussion should explore the effects of the illness on personal activities and social responsibilities (e.g., the inability to care for oneself, loss of employment).
Physicians often do not accurately perceive patients' expectations during visits.11 The patient's expectations may be medical (e.g., diagnosis; physical examination; medications, such as analgesics or antibiotics) or may include nonmedical requests, such as a note for sick leave. Some patients may state that they need reassurance (after careful evaluation) more than medical treatment. In such cases, prescribing an unwanted treatment will most likely be ineffective. Patient-centered care respects the patient's expectations without disregarding clinical evidence. Some requests need to be explored with open-ended questions to find out the patient's underlying concerns. Examples include requests for unnecessary prescriptions or testing, such as antibiotics for viral respiratory infections or brain imaging for tension headaches. Exploratory statements include “I am interested in knowing why…” or “Tell me more about why you would like…”
Expressing Empathy
Empathy is the capacity to understand and relate to the patient's illness experience and emotions. Physicians can express empathy verbally or through nonverbal gestures, such as respectful silence, touching a patient's hand or knee (when culturally appropriate), or sighing. In some situations, such as when a patient is tearful, offering a box of tissues is perhaps more appropriate than verbal expression. Table 4 includes techniques for expressing empathy to patients.10
Table 4. Techniques for Expressing Empathy to Patients

| Technique | Examples (may overlap) |
|---|---|
| Naming | “It seems like you are feeling…” |
| “I wonder if you are feeling…” | |
| “Some people would feel… in this situation.” | |
| “I can see that this makes you feel…” | |
| Understanding | “I can understand how that might upset you.” |
| “I can understand why you would be… given what you are going through.” | |
| “I can imagine what that would feel like.” | |
| “I can't imagine what that would feel like!” | |
| “I know someone who had a similar experience. It is not easy.” | |
| “This has been a hard time for you.” | |
| “That makes sense to me.” | |
| Respecting | “It must be a lot of stress to deal with…” |
| “I respect your courage to keep a positive attitude in spite of your difficulties.” | |
| “You are a brave person.” | |
| “I am impressed by how well you handled this.” | |
| “It sounds like a lot to deal with.” | |
| “You have been through a lot.” | |
| “You did the right thing by coming in.” | |
| Supporting | “I want to help in any way I can.” |
| “Please let me know if there is anything I can do to help.” | |
| “I am here to help you in any way I can.” | |
| “I will be with you in this difficult time.” | |
| “I will be with you all the way.” | |
| Exploring | “Tell me more about what you were feeling when you were sick.” |
| “How are you coping with this?” | |
| “What has happened since we last met?” |
Information from reference 10.
Physicians should recognize that their work has an element of “emotional labor.” Regardless of their own emotional state, physicians need to show concern and interest verbally and through facial expressions.12 This can manifest as deep actions (with empathic understanding) or surface actions (displaying empathic expressions without full cognitive engagement). In contrast, physicians who listen with an unresponsive, blank expression are in effect blocking the patient's emotions.
Revealing a Diagnosis
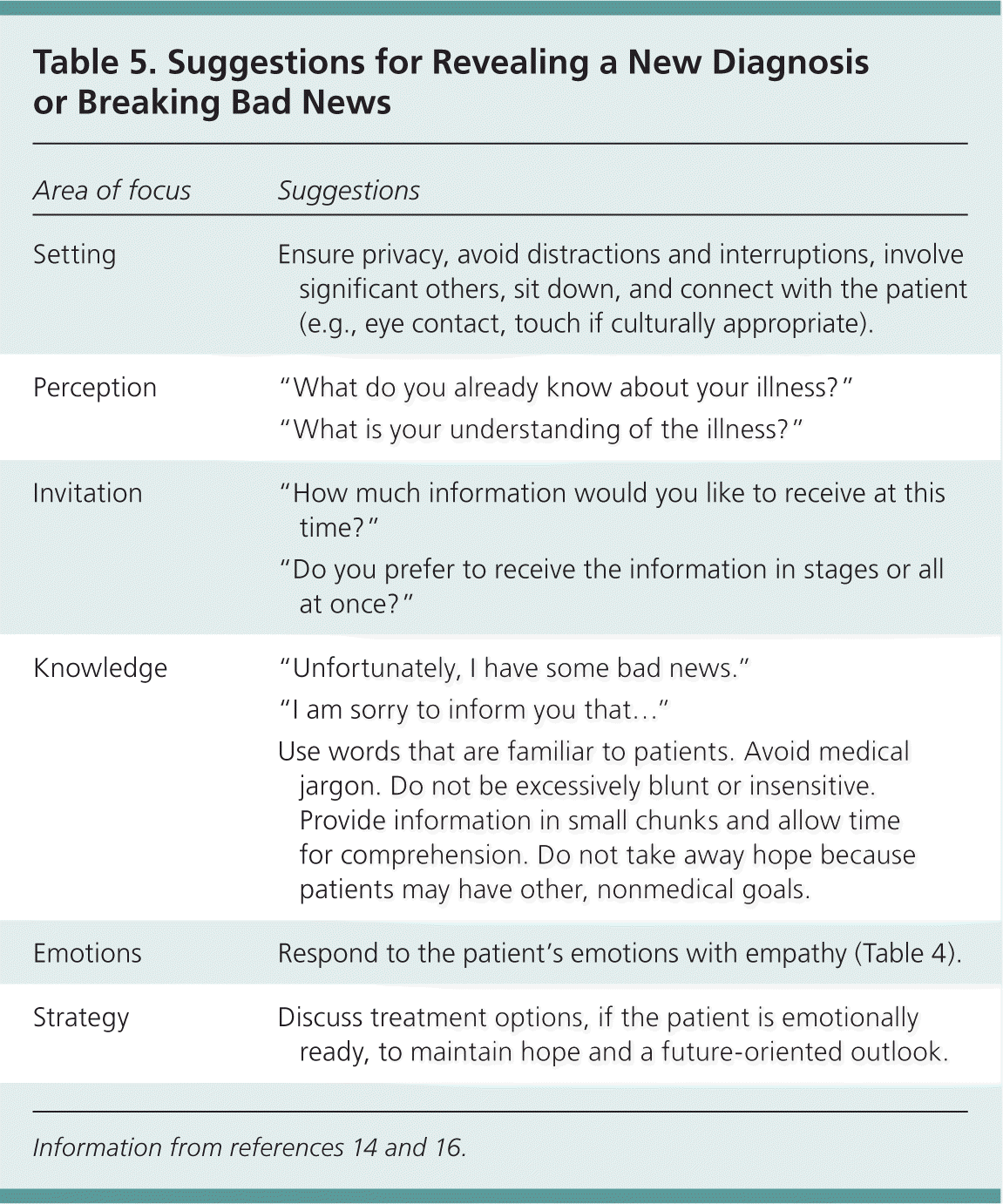
Family physicians routinely have to inform patients about a new diagnosis, such as diabetes mellitus, herpes infection, or cancer. Inappropriate communication, such as an abrupt or harsh disclosure, can be psychologically devastating to the patient. Yet, there is limited empirical evidence on communication techniques for breaking bad news.13 Patients prefer that physicians be seated when breaking bad news.14 Detailed information is requested more often by patients who are younger, female, and more educated.15 Recommendations for breaking bad news include first assessing the patient's prior knowledge and understanding of the illness, and the patient's preference for an overview vs. detailed information. Important points to consider are included in Table 5.14,16 Patients should be given time to absorb the news. Physicians should empathize with the patient's emotions while limiting further information in this initial stage.
Table 5. Suggestions for Revealing a New Diagnosis or Breaking Bad News
| Area of focus | Suggestions |
|---|---|
| Setting | Ensure privacy, avoid distractions and interruptions, involve significant others, sit down, and connect with the patient (e.g., eye contact, touch if culturally appropriate). |
| Perception | “What do you already know about your illness?” |
| “What is your understanding of the illness?” | |
| Invitation | “How much information would you like to receive at this time?” |
| “Do you prefer to receive the information in stages or all at once?” | |
| Knowledge | “Unfortunately, I have some bad news.” |
| “I am sorry to inform you that…” | |
| Use words that are familiar to patients. Avoid medical jargon. Do not be excessively blunt or insensitive. Provide information in small chunks and allow time for comprehension. Do not take away hope because patients may have other, nonmedical goals. | |
| Emotions | Respond to the patient's emotions with empathy (Table 4). |
| Strategy | Discuss treatment options, if the patient is emotionally ready, to maintain hope and a future-oriented outlook. |
By discussing treatment options, physicians can help patients make more informed choices. The pros and cons of each option should be outlined, including benefits, risks (potential immediate and long-term adverse effects or complications), and costs (direct and indirect).17 The option of no active treatment with follow-up (watchful waiting) may be discussed. Providing options reaffirms the patient's need to be actively involved in his or her medical care.18
However, the patient should not be overburdened with extensive information. A balanced approach involves asking about the patient's previous knowledge of the illness, then providing small chunks of information and checking for understanding after each chunk (ask-tell-ask technique).10 The patient's values and goals should be explored if the patient is unable to make decisions based on medical information alone. The patient's clinical condition, health literacy, and emotional state, and the complexity of the medical decision may necessitate multiple sessions with the physician. Shared decision making can be supported by printed aids that visually depict clinical risks using pictographs.19
Final Comment
Exploring and understanding the patient's illness experience and respecting the patient's beliefs and expectations are at the core of patient-centered communication. Patient-centered communication should extend to medical documentation by respecting patients as persons. Terms such as “a case of” and “chief complaint” should be replaced with “a patient with” and “chief concern.” Training programs, even those of short duration (less than 10 hours), have been shown to generally improve physicians' communication skills.20–22 However, patient-centered communication alone does not appear to improve patients' health status or behaviors.23 There is some evidence that adding disease management skills to training programs on patient-centered communication may improve patient outcomes.20 Observational studies indicate an association between patient-centered communication and patients' trust in physicians,24 as well as reduced diagnostic testing.25 Patient-centered care is an intrinsically desirable health care priority, regardless of its effect on clinical outcomes.26 The following YouTube videos provide assistance with patient-centered communication: https://www.youtube.com/playlist?list=PLNfCyzdWB9X6myvivDIeSofzZE0gosTN7, https://youtu.be/ekrnhvqmm-o, and https://youtu.be/36Cuuzw1p8w.
Data Sources: A PubMed search was conducted using the term patient-centered communication. The search was refined using the Sort by Relevance and Related Articles features. The results were not limited by type of article, language, or date of publication. Additional sources searched included the Cochrane database, EMBASE, ScienceDirect, EBSCO Academic Search Complete, and Web of Science. Search dates: September 13, 2015, through September 26, 2016.

