Pleuritic chest pain is characterized by sudden and intense sharp, stabbing, or burning pain in the chest when inhaling and exhaling. Pulmonary embolism is the most common serious cause, found in 5% to 21% of patients who present to an emergency department with pleuritic chest pain. A validated clinical decision rule for pulmonary embolism should be employed to guide the use of additional tests such as d-dimer assays, ventilation-perfusion scans, or computed tomography angiography. Myocardial infarction, pericarditis, aortic dissection, pneumonia, and pneumothorax are other serious causes that should be ruled out using history and physical examination, electrocardiography, troponin assays, and chest radiography before another diagnosis is made. Validated clinical decision rules are available to help exclude coronary artery disease. Viruses are common causative agents of pleuritic chest pain. Coxsackieviruses, respiratory syncytial virus, influenza, parainfluenza, mumps, adenovirus, cytomegalovirus, and Epstein-Barr virus are likely pathogens. Treatment is guided by the underlying diagnosis. Nonsteroidal anti-inflammatory drugs are appropriate for pain management in those with virally triggered or nonspecific pleuritic chest pain. In patients with persistent symptoms, persons who smoke, and those older than 50 years with pneumonia, it is important to document radiographic resolution with repeat chest radiography six weeks after initial treatment.
Pleuritic chest pain is characterized by sudden and intense sharp, stabbing, or burning pain in the chest when inhaling and exhaling. It is exacerbated by deep breathing, coughing, sneezing, or laughing. When pleuritic inflammation occurs near the diaphragm, pain can be referred to the neck or shoulder. Pleuritic chest pain is caused by inflammation of the parietal pleura and can be triggered by a variety of causes.
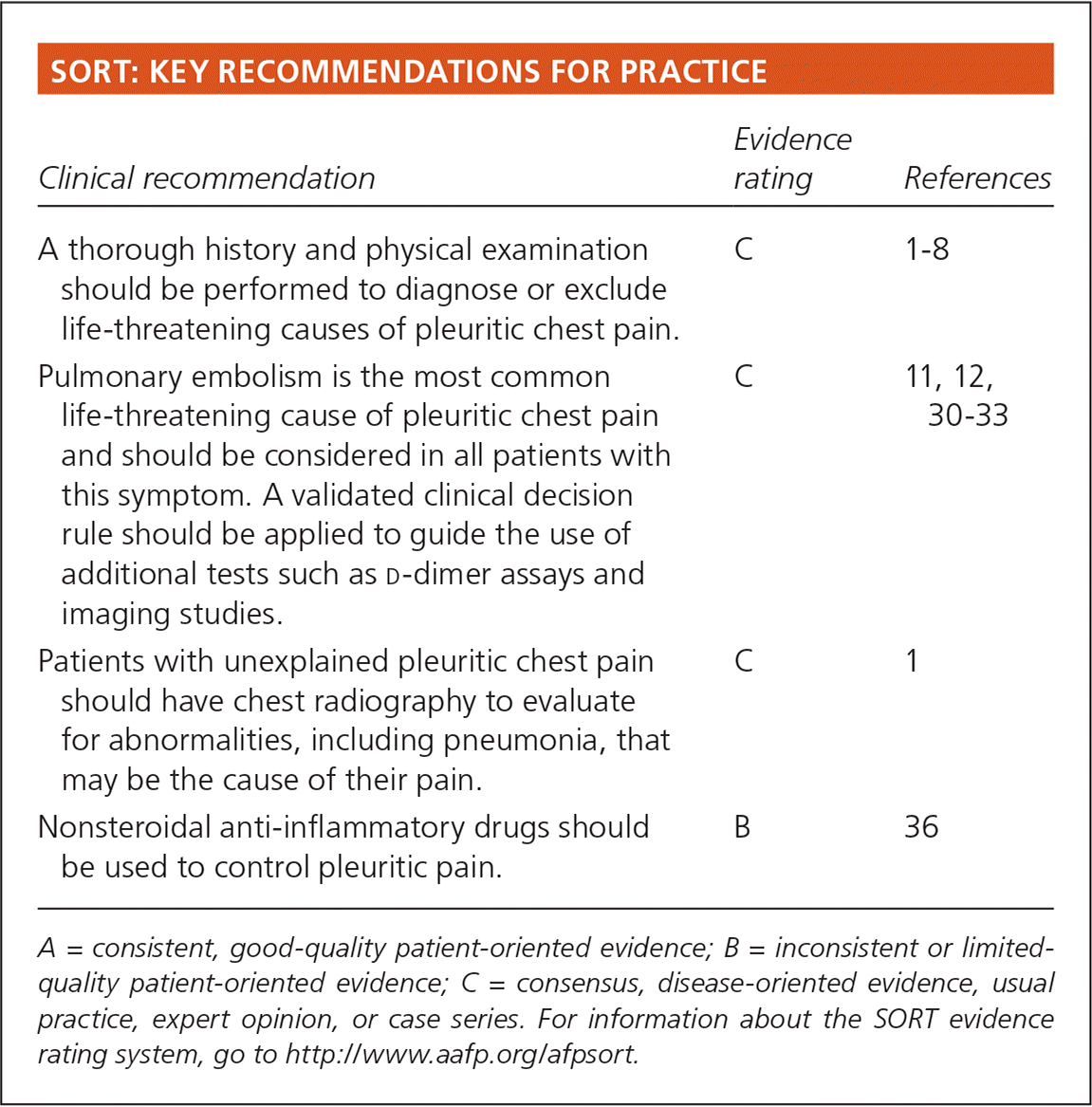
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| A thorough history and physical examination should be performed to diagnose or exclude life-threatening causes of pleuritic chest pain. | C | 1–8 |
| Pulmonary embolism is the most common life-threatening cause of pleuritic chest pain and should be considered in all patients with this symptom. A validated clinical decision rule should be applied to guide the use of additional tests such as | C | 11, 12, 30–33 |
| Patients with unexplained pleuritic chest pain should have chest radiography to evaluate for abnormalities, including pneumonia, that may be the cause of their pain. | C | 1 |
| Nonsteroidal anti-inflammatory drugs should be used to control pleuritic pain. | B | 36 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Pathophysiology
The visceral pleura does not contain pain receptors, whereas the parietal pleura is innervated by somatic nerves that sense pain due to trauma or inflammation. Inflammatory mediators released into the pleural space trigger local pain receptors. Parietal pleurae at the periphery of the rib cage and lateral hemidiaphragm are innervated by intercostal nerves. Trauma or inflammation in these regions results in pain localized in the cutaneous distribution of those nerves. In contrast, the phrenic nerve innervates the central diaphragm and can refer pain to the ipsilateral neck or shoulder.
Differential Diagnosis
Pleuritic chest pain has many etiologies. It is helpful to use a clinical approach that aids physicians in immediately distinguishing between six life-threatening causes of pleuritic chest pain and other more common indolent causes.1–8 Pulmonary embolism, myocardial infarction, pericarditis, aortic dissection, pneumonia, and pneumothorax are the six serious conditions that must be initially considered. The differential diagnosis is presented in Table 1.9,10
Table 1. Differential Diagnosis of Pleuritic Chest Pain

| Category | Etiology | |
|---|---|---|
| Cardiac | Acute coronary syndrome, congestive heart failure, pericarditis, postcardiac injury syndrome, postmyocardial infarction syndrome, postpericardiotomy syndrome | |
| Gastrointestinal | Inflammatory bowel disease, pancreatitis, spontaneous bacterial pleuritis | |
| Hematologic/Oncologic | Malignancy, malignant pleural effusion, sickle cell crisis | |
| Iatrogenic/Exposure | Asbestosis, cardiothoracic surgery, medications, pericardiocentesis | |
| Infection | Abscess | |
| Liver, pulmonary, splenic | ||
| Bacterial | ||
| Empyema | ||
| Legionnaires' disease | ||
| Mediterranean spotted fever (caused by a rickettsial organism [Rickettsia conorii] endemic to the Mediterranean region of Europe that triggers a syndrome similar to Rocky Mountain spotted fever in the United States), parapneumonic pleuritic pneumonia, tuberculosis | ||
| Myocarditis | ||
| Parasitic | ||
| Amebiasis, paragonimiasis | ||
| Viral | ||
| Adenovirus, coxsackieviruses, cytomegalovirus, Epstein-Barr virus, herpes zoster, influenza, mumps, parainfluenza, respiratory syncytial virus | ||
| Inflammatory/autoimmune/Genetic | Ankylosing spondylitis, collagen vascular diseases, familial Mediterranean fever, fibromyalgia, reactive eosinophilic pleuritis, rheumatoid arthritis, systemic lupus erythematosus | |
| Pulmonary | Chronic obstructive pulmonary disease, hemothorax, pleural adhesions, pneumothorax, pulmonary embolism | |
| Renal | Chronic renal failure, renal capsular hematoma | |
| Rheumatologic | Lupus pleuritis, rheumatoid pleuritis, Sjögren syndrome | |
Studies of pleuritic chest pain have shown that pulmonary embolism is the most common life-threatening cause and the source of the pain 5% to 21% of the time.11,12 A recent prospective trial of 7,940 patients evaluated for pulmonary embolism revealed that pleuritic-type chest pain was significantly associated with confirmed pulmonary embolism (adjusted odds ratio of 1.53).13 The most commonly occurring symptoms of pulmonary embolism were dyspnea and pleuritic chest pain in 73% and 66% of patients, respectively.11 Physicians should use validated clinical decision rules (e.g., Wells, PERC [pulmonary embolism rule-out criteria], Geneva) to evaluate for pulmonary embolism, as discussed in a previous article in American Family Physician.14
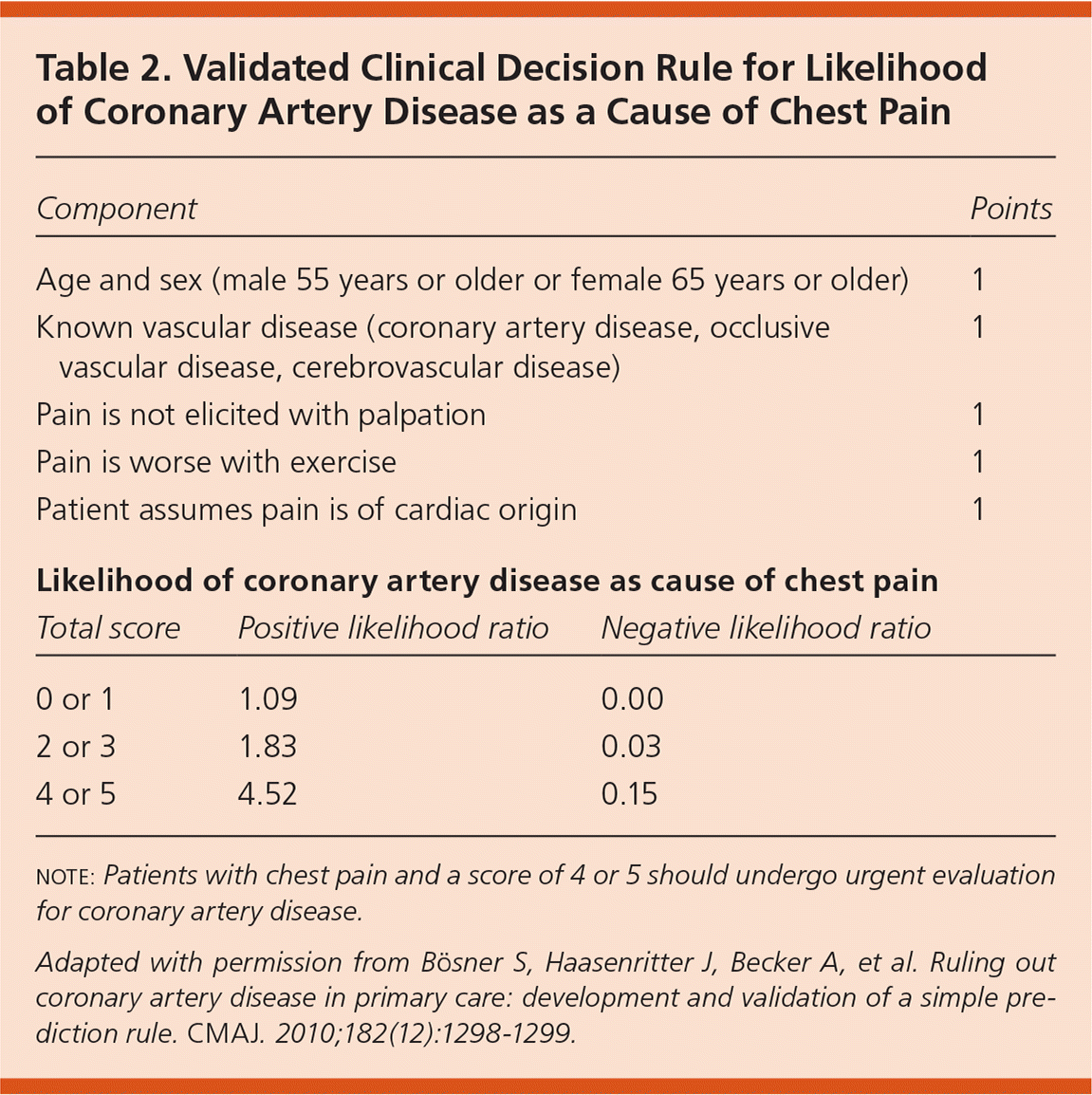
Physicians can evaluate patients for myocardial infarction and coronary artery disease using electrocardiography and troponin levels. Applying a five-point validated clinical decision rule helps improve diagnostic accuracy for coronary artery disease15,16 (Table 215 ). The presence of zero or one of the five scored items predicted only a 1% likelihood of coronary artery disease, whereas 63% of patients with four or five of these factors had coronary artery disease.16 Additionally, high-sensitivity cardiac troponin levels can help improve diagnostic accuracy for myocardial infarction.17,18
Table 2. Validated Clinical Decision Rule for Likelihood of Coronary Artery Disease as a Cause of Chest Pain
| Component | Points | ||
|---|---|---|---|
| Age and sex (male 55 years or older or female 65 years or older) | 1 | ||
| Known vascular disease (coronary artery disease, occlusive vascular disease, cerebrovascular disease) | 1 | ||
| Pain is not elicited with palpation | 1 | ||
| Pain is worse with exercise | 1 | ||
| Patient assumes pain is of cardiac origin | 1 | ||
| Likelihood of coronary artery disease as cause of chest pain | |||
| Total score | Positive likelihood ratio | Negative likelihood ratio | |
| 0 or 1 | 1.09 | 0.00 | |
| 2 or 3 | 1.83 | 0.03 | |
| 4 or 5 | 4.52 | 0.15 | |
note: Patients with chest pain and a score of 4 or 5 should undergo urgent evaluation for coronary artery disease.
Adapted with permission from Bösner S, Haasenritter J, Becker A, et al. Ruling out coronary artery disease in primary care: development and validation of a simple prediction rule. CMAJ 2010;182(12):1298–1299.
Pericarditis can be excluded by review of an electrocardiogram and, if required, echocardiogram findings. Pneumonia and pneumothorax can be evaluated with chest radiography.1 Aortic dissection can be excluded with chest radiography in very low-risk patients; otherwise, computed tomography angiography should be performed.19
Viruses are common causative agents of pleuritic chest pain. Coxsackieviruses, respiratory syncytial virus, influenza, parainfluenza, mumps, adenovirus, cytomegalovirus, and Epstein-Barr virus are likely pathogens.2,20,21 A recommended approach to the diagnosis of patients with pleuritic chest pain is provided in Figure 1.3
Figure 1. Outpatient Diagnosis of Pleuritic Chest Pain.
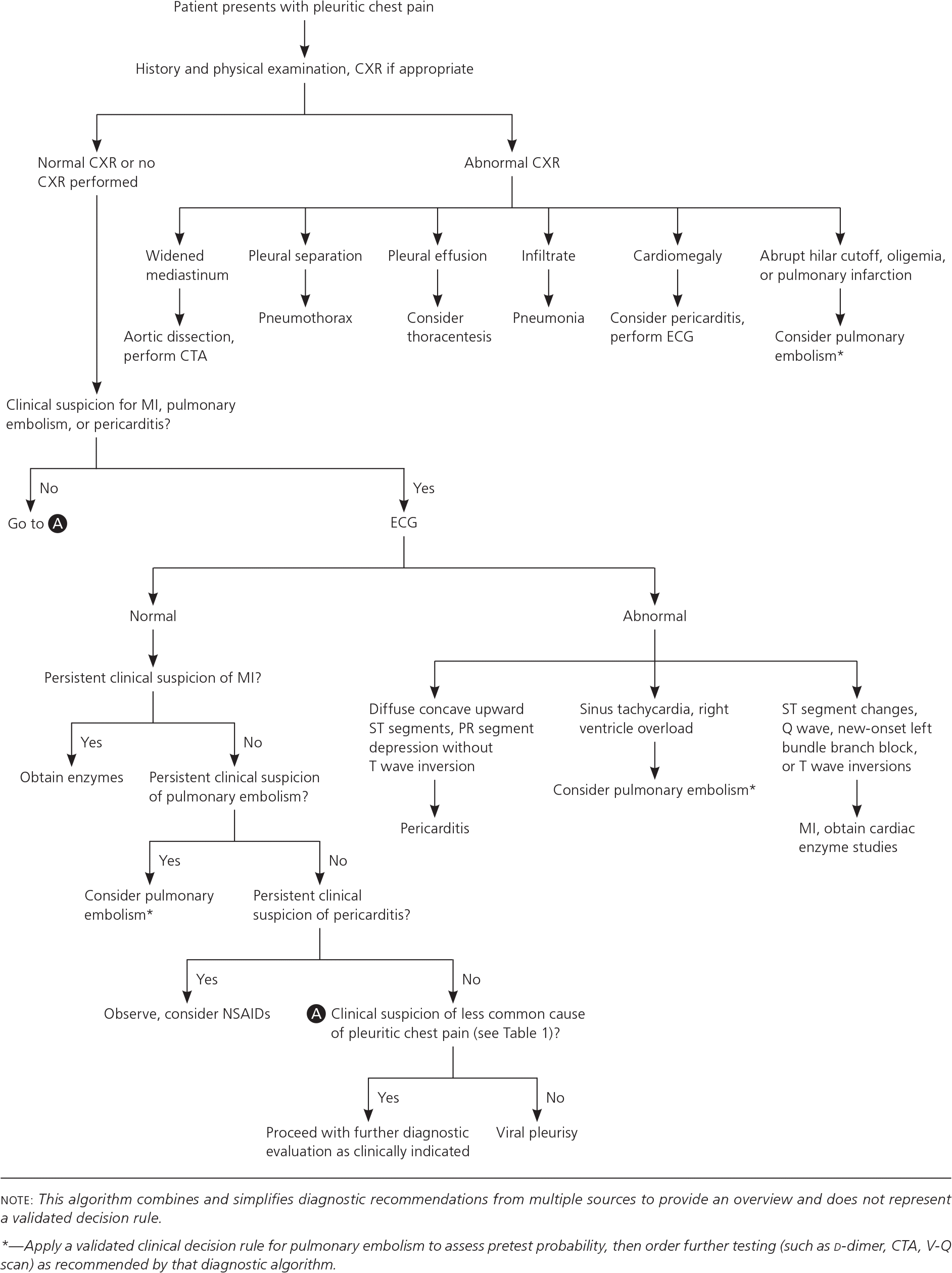
Algorithm for the outpatient diagnosis of pleuritic chest pain. (CTA = computed tomography angiography; CXR = chest radiography; ECG = electrocardiography; MI = myocardial infarction; NSAID = nonsteroidal anti-inflammatory drug; V-Q = ventilation-perfusion.)
Adapted with permission from Kass SM, Williams PM, Reamy BV. Pleurisy. Am Fam Physician. 2007;75(9):1359.
Medical History
The time course of the onset of symptoms is the most useful historical information for narrowing the differential diagnosis. Most potentially lethal causes of pleuritic chest pain (i.e., pulmonary embolism, myocardial infarction, aortic dissection, and pneumothorax) typically have an acute onset over minutes. In contrast, less immediately lethal causes of pleuritic chest pain (e.g., infection, malignancy, inflammatory processes) progress over hours to days or weeks.4 Pain that worsens when the patient is supine and lessens when the patient is upright and leaning forward should prompt consideration for pericarditis.4–6 True dyspnea should also increase suspicion for a pulmonary embolus, pneumothorax, or pneumonia.1,7,8 It is clinically useful to distinguish true dyspnea from patient-perceived dyspnea caused by a desire to suppress respirations to avoid pain.22,23
Cardiac symptoms such as diaphoresis, nausea, and palpitations should be elucidated. Pain that is described as sharp and stabbing is typical of noncardiac chest pain.22 Radiation of pain to the shoulders or arms has a positive likelihood ratio of 4.07 (95% confidence interval, 2.53 to 6.54) for acute myocardial infarction.22 In contrast, pain that radiates to the back and is maximal in intensity at onset is more commonly associated with aortic dissection than cardiac ischemia.22
Cough, fever, and sputum production should prompt evaluation for community-acquired pneumonia. Symptoms such as weight loss, malaise, night sweats, or arthralgias indicate chronic inflammatory causes of pleuritic chest pain, such as tuberculosis infection, rheumatoid arthritis, or malignancy. A family history of similar symptoms increases the likelihood of rare diagnoses such as familial Mediterranean fever. A medication history that includes the use of drugs with a high risk of adverse pulmonary effects should raise concerns for a pharmacologic reaction. A sickle cell crisis must be considered in any patient with known sickle cell disease (Table 19,10 ).
Physical Examination
Tachycardia or tachypnea may be present with any of the serious causes of pleuritic chest pain but should raise suspicion for pulmonary embolism, pneumothorax, or myocardial infarction. Patients may demonstrate shallower breaths as they attempt to avoid deep breathing that triggers pain.23 Likewise, hypotension and a markedly widened pulse pressure should raise concerns for aortic dissection or severe myocardial infarction. Fever increases the likelihood of infection.
Pleural inflammation, or pleurisy, causes roughening of the smooth surfaces of the parietal and visceral pleurae. As these surfaces rub against each other with normal inspiration and expiration, a scratching sound or friction rub may be heard. This may also occur in 4% of patients with pneumonia or pulmonary embolism.24 Pneumonia with lung consolidation may also lead to decreased breath sounds, rales, and egophony. In contrast, pneumothorax could lead to hyperresonance on lung examination.
In new-onset heart failure due to large myocardial infarction, cardiac examination may show an extra heart sound (third or fourth heart sound). A friction rub may be heard over the heart in severe cases of pericarditis. Patients may present with an initial normal examination even when serious conditions are present. The absence of a clear diagnosis warrants additional diagnostic testing.
Diagnostic Tests
Most patients presenting with pleuritic chest pain will require imaging with chest radiography to fully define their diagnosis.1 If pleural fluid is seen on a chest radiograph, the fluid can be aspirated and examined for additional clues about the source of the pleuritic chest pain.25,26 Lung ultrasonography can guide thoracentesis, as well as localize a small pneumothorax and identify other pulmonary conditions.27,28
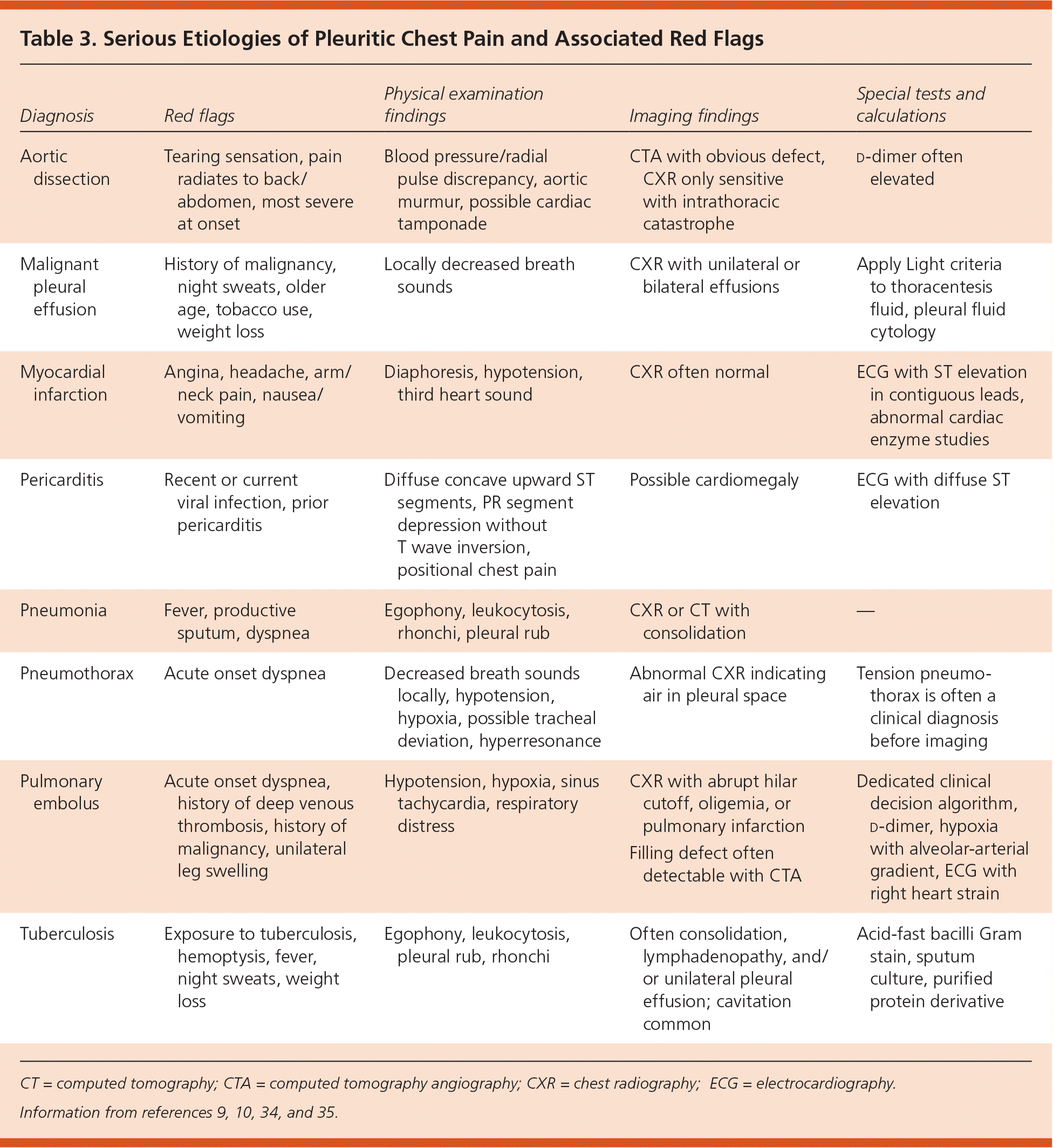
When a cardiac or vascular source is considered, electrocardiography, cardiac enzyme studies, and echocardiography are useful tests. Widespread ST segment elevation is a typical electrocardiographic finding in pericarditis.19,29 In the case of infection, a complete blood count, serology, and cultures of blood, sputum, or pleural fluid may be indicated. A validated clinical decision rule for pulmonary embolism should be employed to guide the use of additional tests such as d-dimer assays, ventilation-perfusion scans, or computed tomography angiography.30–33 Table 3 integrates red flag symptoms of serious causes of pleuritic chest pain, physical examination, and diagnostic findings to aid in the evaluation of pleuritic chest pain.9,10,34,35
Table 3. Serious Etiologies of Pleuritic Chest Pain and Associated Red Flags
| Diagnosis | Red flags | Physical examination findings | Imaging findings | Special tests and calculations |
|---|---|---|---|---|
| Aortic dissection | Tearing sensation, pain radiates to back/abdomen, most severe at onset | Blood pressure/radial pulse discrepancy, aortic murmur, possible cardiac tamponade | CTA with obvious defect, CXR only sensitive with intrathoracic catastrophe | |
| Malignant pleural effusion | History of malignancy, night sweats, older age, tobacco use, weight loss | Locally decreased breath sounds | CXR with unilateral or bilateral effusions | Apply Light criteria to thoracentesis fluid, pleural fluid cytology |
| Myocardial infarction | Angina, headache, arm/neck pain, nausea/vomiting | Diaphoresis, hypotension, third heart sound | CXR often normal | ECG with ST elevation in contiguous leads, abnormal cardiac enzyme studies |
| Pericarditis | Recent or current viral infection, prior pericarditis | Diffuse concave upward ST segments, PR segment depression without T wave inversion, positional chest pain | Possible cardiomegaly | ECG with diffuse ST elevation |
| Pneumonia | Fever, productive sputum, dyspnea | Egophony, leukocytosis, rhonchi, pleural rub | CXR or CT with consolidation | — |
| Pneumothorax | Acute onset dyspnea | Decreased breath sounds locally, hypotension, hypoxia, possible tracheal deviation, hyperresonance | Abnormal CXR indicating air in pleural space | Tension pneumothorax is often a clinical diagnosis before imaging |
| Pulmonary embolus | Acute onset dyspnea, history of deep venous thrombosis, history of malignancy, unilateral leg swelling | Hypotension, hypoxia, sinus tachycardia, respiratory distress | CXR with abrupt hilar cutoff, oligemia, or pulmonary infarction Filling defect often detectable with CTA | Dedicated clinical decision algorithm, |
| Tuberculosis | Exposure to tuberculosis, hemoptysis, fever, night sweats, weight loss | Egophony, leukocytosis, pleural rub, rhonchi | Often consolidation, lymphadenopathy, and/or unilateral pleural effusion; cavitation common | Acid-fast bacilli Gram stain, sputum culture, purified protein derivative |
CT = computed tomography; CTA = computed tomography angiography; CXR = chest radiography; ECG = electrocardiography.
Treatment
After excluding the six serious causes of pleuritic chest pain that require emergent evaluation, there are two primary management considerations: controlling the pain and treating the etiology of the underlying condition. Initial pain control is best achieved with nonsteroidal anti-inflammatory drugs.36 These drugs do not have the analgesic potency of narcotics, but they also do not suppress the respiratory drive and do not change the patient's sensorium during early evaluation. Although a class effect is assumed, studies on the treatment of pleuritic chest pain in humans have focused on the use of indomethacin at dosages of 50 to 100 mg orally up to three times per day. These studies have shown improvements in pain and mechanical lung function.36 Corticosteroids should be reserved for patients who are intolerant of nonsteroidal anti-inflammatory drugs. They are also used in the treatment of tuberculous pleurisy and have been shown to result in some reduction in effusions and symptoms, but they have not demonstrated improvements in mortality.37
Once pain is adequately controlled and serious underlying conditions are excluded, other conditions should be treated. Antimicrobial or antiparasitic agents should be started based on the presumed organism in pneumonia. Colchicine (1.2 to 2.0 mg orally once per day or divided twice per day) is the standard treatment for familial Mediterranean fever.38 Biologic agents such as anti-interleukin-1, interleukin-6 inhibitor, and tocilizumab may have utility in refractory cases of familial Mediterranean fever.39,40 Pleural effusions that rapidly reaccumulate after initial thoracentesis may require pleurodesis. This is more likely to occur when the effusion is due to malignancy, renal failure, or rheumatoid pleurisy.41
In most cases of pleuritic chest pain from viral infection, pain and symptoms will resolve within two to four weeks. In cases of persistent or recurrent pain, or when significant pathology is discovered, patient care should continue as required based on the etiology.
In patients diagnosed with pneumonia who smoke tobacco, have persistent symptoms, or are older than 50 years, it is important to document resolution of the abnormality with repeat chest radiography performed six weeks after initial treatment.42 These patients are at increased risk of developing pneumonia secondary to an obstructing lesion such as lung cancer. One study showed that of 236 adults presenting to their primary care physician with community-acquired pneumonia, 10 were found to have an underlying lung cancer.42 The percentage of those with lung cancer rose to 17% in smokers older than 60 years.42 Studies have shown resolution of radiographic abnormalities in 60% to 73% of patients by six weeks after diagnosis.42 Further evaluation should be considered in patients with persisting symptoms or radiographic abnormalities.
Data Sources: The three authors performed independent literature searches using PubMed, the Cochrane Library, POEMs research summaries, and Essential Evidence Plus. Searches were conducted from February 2016 to June 2016. A total of 243 citations were identified using the key words pleurisy and pleuritic chest pain, and the search was limited to human studies. These citations were reviewed independently by the authors and then collaboratively at a series of conference calls to identify the key references to be included in the article.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the Uniformed Services University of the Health Sciences, the U.S. Air Force, or the Department of Defense.

