A 28-year-old man presented with several days of fever, diarrhea, body aches, and vomiting. His urine output was low and turbid. The symptoms began one week after he returned home from a family trip to Puerto Rico. His wife had similar symptoms that resolved. During his trip, he received a few mosquito bites, went swimming in a local river, and ate local food.
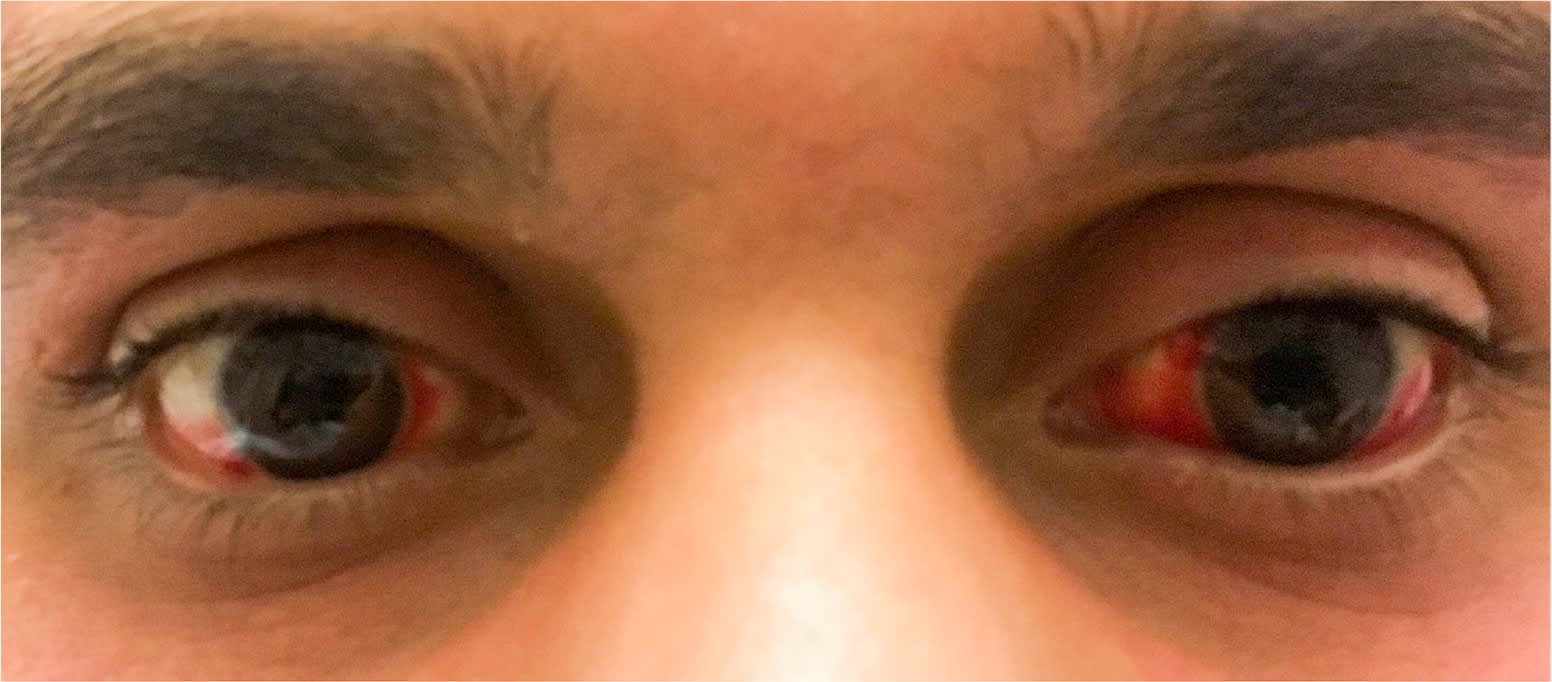
Physical examination showed mild jaundice and conjunctival suffusion (Figure 1). There was a petechial rash on his forehead and swelling in all extremities that was especially pronounced along the thenar eminence of the right hand.
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Dengue.
B. Leptospirosis.
C. Malaria.
D. Shigellosis.
Discussion
The answer is B: leptospirosis. Leptospirosis is an infection caused by Leptospira bacteria. Humans can become infected through contact with water, soil, or food that is contaminated with urine from infected animals, such as rodents (most common), deer, raccoons, and domestic dogs. As many as 10 million persons worldwide are infected with Leptospira annually, mostly in tropical areas. Symptoms appear seven to 10 days after exposure, although some persons experience minimal to no symptoms.1
When present, symptoms of leptospirosis arise in two phases. The first phase includes fever, chills, headache, myalgia, red eyes, vomiting, or diarrhea. Conjunctival suffusion is a classic sign that can be overlooked.2 The second phase is more severe and can result in meningitis and kidney and liver failure.1 At its most severe, the infection can cause Weil syndrome, which presents as jaundice and kidney failure. Treatment with antibiotics, such as penicillin or doxycycline, is usually effective. Intravenous administration may be necessary for severe infections.1
Dengue is transmitted by infected mosquitos. Symptoms of dengue are high fever, severe headache, pain behind the eyes, myalgia, arthralgia, rash, and mild bleeding (epistaxis or gingival bleeding). Infected patients are at risk of hemorrhagic fever, characterized by high fever, damage to lymph nodes and blood vessels, bleeding from the nose and gums, enlarged liver, and circulatory failure.3
Malaria is caused by Plasmodium infection and should be suspected in a patient who develops a fever after traveling to an endemic area. Other symptoms include headache, malaise, myalgia, and arthralgia. Counseling for travelers to malaria-endemic areas should include prevention of mosquito bites. Chemoprophylaxis should be recommended when appropriate.4
Shigellosis is a diarrheal illness caused by Shigella bacteria. Symptoms include fever, abdominal pain with bloody or nonbloody diarrhea, and the painful sensation of needing to pass stool despite an empty bowel (tenesmus). Symptoms generally last five to seven days, but it may take months before bowel habits return to normal. Complications may include postinfectious arthritis, bacteremia, seizures, or hemolytic uremic syndrome.4
Summary Table
| Condition | Transmission | Characteristics |
|---|---|---|
| Dengue | Bite from infected mosquito | High fever, severe headache, pain behind the eyes, myalgia, arthralgia, rash, mild bleeding (epistaxis or gingival bleeding) |
| Leptospirosis | Contact with contaminated water, soil, or food | Self-limited fever, chills, headache, myalgia, red eyes, vomiting, diarrhea; may become more severe, resulting in meningitis and liver and kidney failure (e.g., Weil syndrome) |
| Malaria | Bite from infected mosquito in an endemic area | Fever, headache, malaise, myalgia, arthralgia |
| Shigellosis | Fecal-oral transmission | Fever, abdominal pain with bloody or nonbloody diarrhea, the painful sensation of needing to pass stool despite an empty bowel (tenesmus) |

