AFP uses the Strength-of-Recommendation Taxonomy (SORT),1 to label key recommendations in clinical review articles. In general, only key recommendations are given a Strength-of-Recommendation grade. Grades are assigned on the basis of the quality and consistency of available evidence. Table 1 shows the three grades recognized.
As the table indicates, the strength-of-recommendation grade depends on the quality and consistency of the evidence for the recommendation. Quality and consistency of evidence are determined as indicated in Table 2 and Table 3.
An alternative way to understand the significance of a strength-of-recommendation grade is through the algorithm generally followed by authors and editors in assigning grades based on a body of evidence (Figure 1). While this algorithm provides a general guideline, authors and editors may adjust the strength of recommendation based on the benefits, harms, and costs of the intervention being recommended.
TABLE 1. Strength-of-Recommendation Grades

| Strength of recommendation | Basis for recommendation |
|---|---|
| A | Consistent, good-quality patient-oriented evidence* |
| B | Inconsistent or limited-quality patient-oriented evidence* |
| C | Consensus, disease-oriented evidence,** usual practice, expert opinion, or case series for studies of diagnosis, treatment, prevention, or screening |
*—Patient-oriented evidence measures outcomes that matter to patients: morbidity, mortality, symptom improvement, cost reduction, and quality of life.
**—Disease-oriented evidence measures intermediate, physiologic, or surrogate end points that may or may not reflect improvements in patient outcomes (e.g., blood pressure, blood chemistry, physiologic function, pathologic findings).
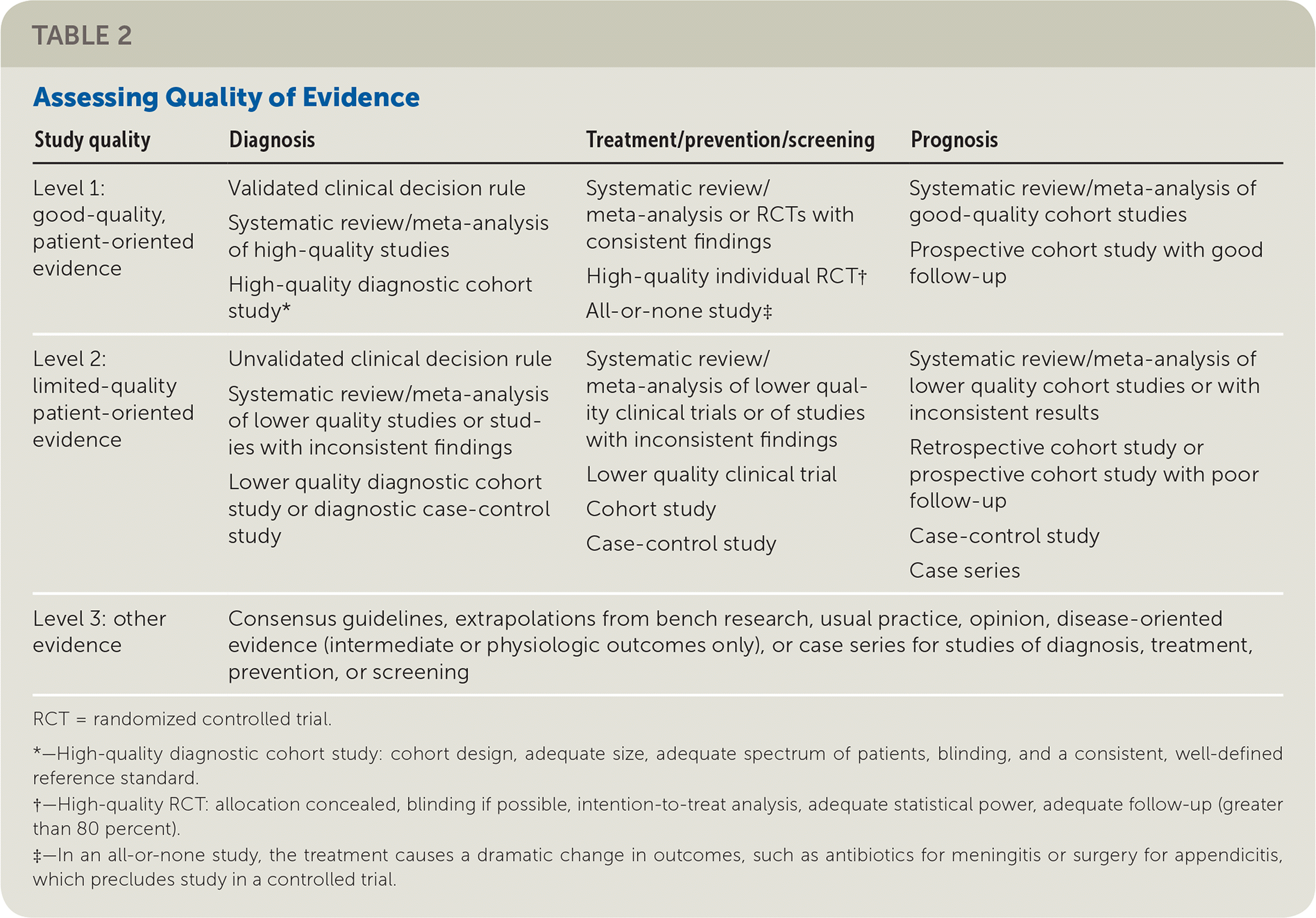
TABLE 2. Assessing Quality of Evidence
| Study quality | Diagnosis | Treatment/prevention/screening | Prognosis |
|---|---|---|---|
| Level 1: good-quality, patient-oriented evidence | Validated clinical decision rule Systematic review/meta-analysis of high-quality studies High-quality diagnostic cohort study* | Systematic review/meta-analysis or RCTs with consistent findings High-quality individual RCT† All-or-none study‡ | Systematic review/meta-analysis of good-quality cohort studies Prospective cohort study with good follow-up |
| Level 2: limited-quality patient-oriented evidence | Unvalidated clinical decision rule Systematic review/meta-analysis of lower quality studies or studies with inconsistent findings Lower quality diagnostic cohort study or diagnostic case-control study | Systematic review/meta-analysis of lower quality clinical trials or of studies with inconsistent findings Lower quality clinical trial Cohort study Case-control study | Systematic review/meta-analysis of lower quality cohort studies or with inconsistent results Retrospective cohort study or prospective cohort study with poor follow-up Case-control study Case series |
| Level 3: other evidence | Consensus guidelines, extrapolations from bench research, usual practice, opinion, disease-oriented evidence (intermediate or physiologic outcomes only), or case series for studies of diagnosis, treatment, prevention, or screening | ||
RCT = randomized controlled trial.
*—High-quality diagnostic cohort study: cohort design, adequate size, adequate spectrum of patients, blinding, and a consistent, well-defined reference standard.
†—High-quality RCT: allocation concealed, blinding if possible, intention-to-treat analysis, adequate statistical power, adequate follow-up (greater than 80 percent).
‡—In an all-or-none study, the treatment causes a dramatic change in outcomes, such as antibiotics for meningitis or surgery for appendicitis, which precludes study in a controlled trial.
TABLE 3. Assessing Consistency of Evidence Across Studies

| Consistent | Most studies found similar or at least coherent conclusions (coherence means that differences are explainable). or If high-quality and up-to-date systematic reviews or meta-analyses exist, they support the recommendation. |
| Inconsistent | Considerable variation among study findings and lack of coherence or If high-quality and up-to-date systematic reviews or meta-analyses exist, they do not find consistent evidence in favor of the recommendation. |

