Frailty, which is a geriatric syndrome that affects 5% to 17% of older adults, is a state of increased vulnerability across multiple health domains that leads to adverse health outcomes. Frail older adults are at increased risk of falls, disability, hospitalizations, and death. Frailty may initially be overlooked or incorrectly identified as part of the normal aging process because of the variable nature of the presentation and diagnosis. Symptoms include generalized weakness, exhaustion, slow gait, poor balance, decreased physical activity, cognitive impairment, and weight loss. There is no current recommendation for routine screening. A comprehensive geriatric assessment can identify risk factors and symptoms that suggest frailty. Several validated frailty assessment tools can evaluate a patient for frailty. Patients are diagnosed as not-frail, prefrail, or frail. Patients with a larger number of frail attributes are at higher risk of poor outcomes. The management of frail patients must be individualized and tailored to each patient's goals of care and life expectancy. Physical activity and balance exercises may be suitable for patients who are less frail. Palliative care and symptom control may be appropriate for those who are more frail.
Frailty is a syndrome of growing importance among the geriatric population, occurring in 5% to 17% of older adults.1,2 Clinicians need to recognize the signs and symptoms of frailty as the average life expectancy of the population continues to increase. Several studies have demonstrated that frail adults are at increased risk of adverse health outcomes.3–5 However, there is no unifying definition for frailty. It is a syndrome recognized primarily in older adults that affects health, energy, and physical abilities by increasing a patient's vulnerability to stressors (e.g., falls, infection) and risk of further decline.1,6,7 Recognizing frailty and understanding its progression will help physicians develop treatment plans and better discuss prognosis with patients and their families.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
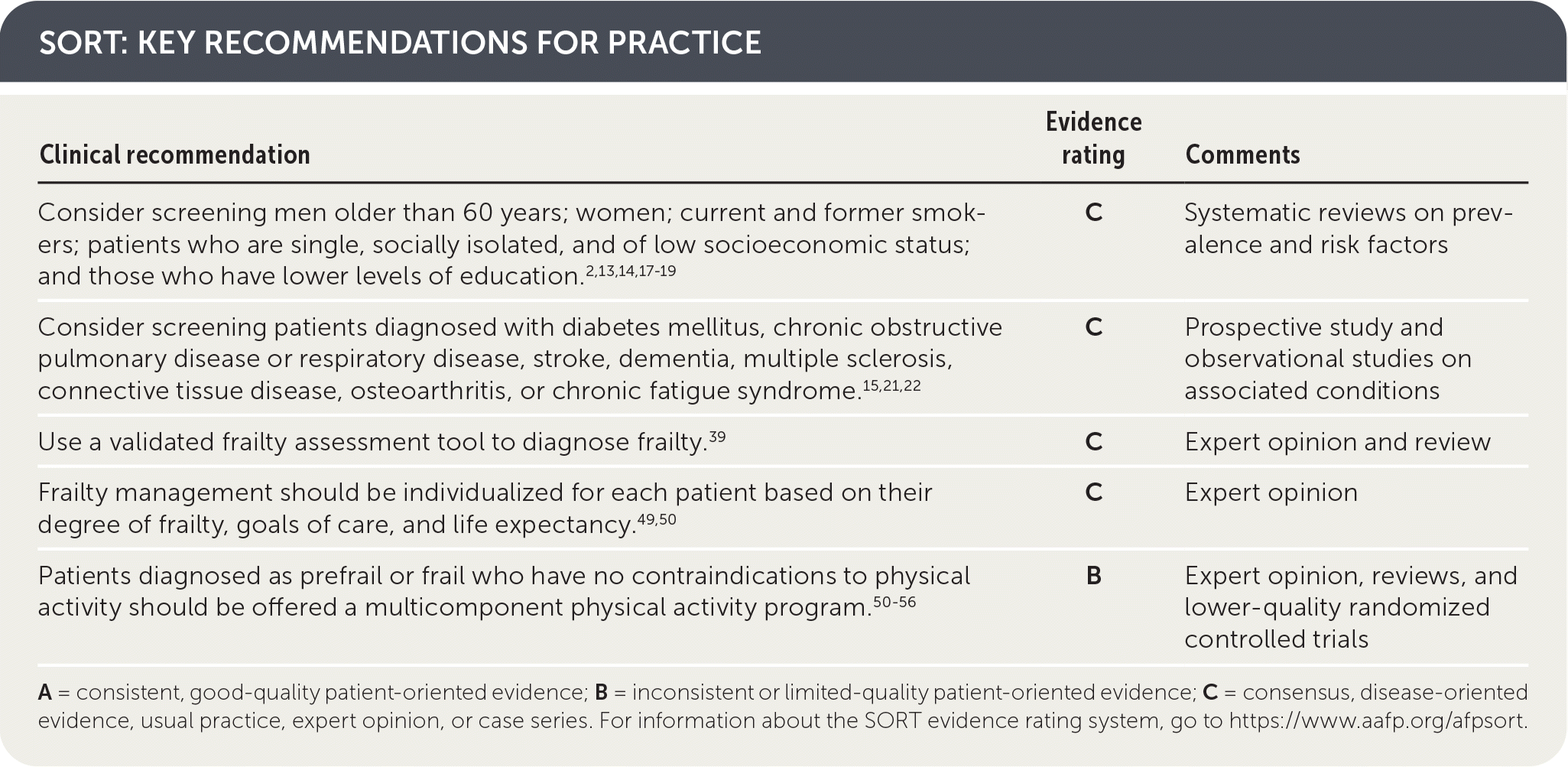
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN GERIATRIC MEDICINE

| Recommendation | Sponsoring organization |
|---|---|
| Do not recommend aggressive or hospital-level care for a frail older person without a clear understanding of the patient's goals of care and the possible benefits and harms. | Society for Post-Acute and Long-Term Care Medicine |
Source: For more information on the Choosing Wisely Campaign, see https://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
Pathophysiology
The normal aging process is a cumulative result of molecular and cellular damage that leads to a loss of physiologic reserve. A patient's physiologic reserve provides the ability to compensate for disease-related changes and maintain a homeostatic balance in the natural aging process. There is no one specific organ system that causes frailty but rather an aggregate loss across multiple systems.8–11 On the cellular level, altered processes in mitochondria and protein processing, increased free radical concentrations, and amplified sensitivity to apoptosis contribute to systemic changes.12 Key age-related changes include hormonal dysregulation (e.g., increased cortisol levels), sarcopenia (i.e., loss of skeletal and muscle mass), and increased immune system activation and proinflammatory cytokines.10,11 These changes cause a loss of homeostasis and a significantly decreased physiologic reserve, making patients who are frail more vulnerable to functional decline. As a result, these patients do not adapt to the stress of systemic disease as well as patients who are not frail.
Risk Factors
The estimated prevalence of frailty in the community setting is inconsistent in the literature, and incidence is likely underreported.2,13,14 Prevalence is hard to estimate because frailty is multifactorial, with older age, female sex, unhealthy lifestyle, and lower economic status identified as potential risk factors.2,13–16 Social factors such as marital status, smoking history, social isolation, and lower levels of education also put people at risk.17–20 Research suggests that frailty increases with the number of health deficits and presence of multiple comorbidities.2 Patients diagnosed with diabetes mellitus, respiratory disease, stroke, dementia, multiple sclerosis, connective tissue disease, osteoarthritis, and chronic fatigue syndrome have higher documented frailty rates.15,21,22
The relationship between medication use and frailty is not well defined. Some studies demonstrated that polypharmacy (taking five or more medications) was associated with frailty; however, potentially inappropriate medication use as defined by the Beers Criteria for Potentially Inappropriate Medication Use in Older Adults was not associated.23–26 One study indicated that frailty can be a risk factor for polypharmacy.27
Presentation
Frailty is a dynamic state of well-being involving multiple health domains that are influenced by a range of variables.28 Patients who are frail share many common physical traits, but there is no hallmark sign or symptom that is pathognomonic to confirm the diagnosis. Early frailty symptoms often involve generalized weakness and exhaustion.7,29 Other symptoms include slow gait, poor balance, decreased physical activity, decreased strength, and cognitive impairment. Weight loss is typically a sign of late-stage frailty.7,29
Assessing Frailty
SCREENING
There are currently no recommendations to routinely screen for frailty. However, to optimize care and communicate appropriately with families, clinicians may need to identify patients at risk and those who may already be frail. One of the most effective screening approaches for frailty is a comprehensive geriatric assessment, a systematic, multidimensional assessment conducted by an interprofessional team of geriatric health professionals, including primary care physicians familiar with the components of a geriatric assessment.25,30 This assessment addresses social, environmental, and medical determinants of health rather than focusing on individual disease states. Clinicians assess a patient's medical comorbidities, polypharmacy, functional abilities (activities of daily living), fall risk, hearing, vision, mental health, and cognition.25,30,31 Impairment in any one of these areas can be a risk factor for frailty and requires further evaluation.
There is a growing interest among specialists—including cardiologists, surgeons, and oncologists—about screening for frailty as a predictor for health care outcomes.32–35 During the coronavirus disease 2019 (COVID-19) pandemic, some critical care physicians have screened for frailty to assist in medical decision-making for patients hospitalized with COVID-19.36–38 Primary care physicians and specialists may wish to collaborate with a geriatrician if a diagnosis is uncertain or if time limitations are a barrier.25 Specific aspects of the assessment can span multiple visits, making it more feasible to implement into a busy family medicine practice. Medicare Annual Wellness Visits also provide opportunities to introduce some of the screening tools into a patient's visit3 (https://www.aafp.org/fpm/2019/0300/p25.html).
EVALUATION
Frailty is not defined by a single patient-reported symptom or physical examination finding, and no laboratory tests or imaging studies can diagnose frailty. Rather, frailty is assessed through a comprehensive history and physical examination, focusing on several key elements. A patient thought to be frail should be evaluated using validated frailty assessment tools.39 Two of the most common assessment tools are the Fried frailty phenotype and the Rockwood frailty index.40 Both tools use the history and physical examination components to assess a patient's degree of frailty based on predetermined variables that have been studied and used in research and clinical practice.1,6
The Fried frailty phenotype uses five predefined variables to assess patients assumed to be frail. Patients are evaluated for unintentional weight loss, weakness, slowness, poor endurance, and low physical activity.1 Table 1 includes the minimum values and further definitions and resources needed to score each variable.1 [corrected]
TABLE 1. Fried Frailty Phenotype Criteria

| Frailty phenotype variables | Diagnostic criteria |
|---|---|
| Weight loss (in the past 12 months) | Self-reported loss of 10 lb (4.5 kg) Documented weight loss of ≥ 5% of total body weight |
| Gait speed (walking 15 feet) | Men (height in inches): ≤ 68: ≤ 7 seconds > 68: ≤ 6 seconds Women (height in inches): ≤ 62.5: ≤ 7 seconds > 62.5: ≤ 6 seconds |
| Grip strength (measured with a dynamometer) | Men (body mass index [kg per m2]; grip strength): ≤ 24: ≥ 64 lb (29 kg) 24.1 to 26: ≥ 66 lb (30 kg) 26.1 to 28: ≥ 66 lb > 28: ≥ 70.5 lb (32 kg) Women (body mass index [kg per m2]; grip strength): ≤ 23: ≥ 37.5 lb (17 kg) 23.1 to 26: ≥ 38 lb (17.3 kg) 26.1 to 29: ≥ 39.5 lb (18 kg) > 29: ≥ 46 lb (21 kg) |
| Physical exhaustion (Center for Epidemiological Studies Depression Scale) | Patients respond to the following questions: I felt that everything I did was an effort in the past week. I could not get going in the past week. Score 0 to 3 (0 = rarely or none of the time; 1 = some or a little of the time; 2 = a moderate amount of the time; 3 = most or all of the time) Scoring 2 or 3 on either question meets the criteria for frailty. |
| Low energy expenditure (per the Minnesota Leisure Time Physical Activity Questionnaire) | Men: < 383 kcals per week Women: < 270 kcals per week |
Note: Each criteria is one point. A score of 0 is considered “not-frail,” and a score of 1 or 2 is considered “prefrail” or at risk of frailty. A score of 3 or more meets the diagnosis of frail.
Adapted with permission from Fried LP, Tangen CM, Walston J, et al.; Cardiovascular Health Study Collaborative Research Group. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56(3):M156.
Grip strength is often evaluated by using a dynamometer.1 This device is held in the dominant hand with the arm flexed to 90 degrees, the elbow at the side of the body, and the handle adjusted so the distal interphalangeal joint wraps around the device. The patient squeezes the dynamometer with a maximum isometric grip for five seconds, followed by a 15-second relaxation period. The best of the three measurements is compared with minimum grip strength values based on sex and body mass index. A value below the minimum cutoff meets the criteria for frailty. A dynamometer is not commonly found in outpatient offices but may be available in some geriatric assessment clinics. Most physical therapy or occupational hand therapy departments will have dynamometers.
Slowness is measured by the time it takes a patient to walk 15 ft (4.5 m). Maximum time allotments are defined by sex and height (Table 1).1 Time values slower than expected meet the criteria for frailty.
The questions “I felt that everything I did was an effort in the past week” and “I could not get going in the past week” from the Center for Epidemiological Studies Depression Scale are used to measure endurance.41
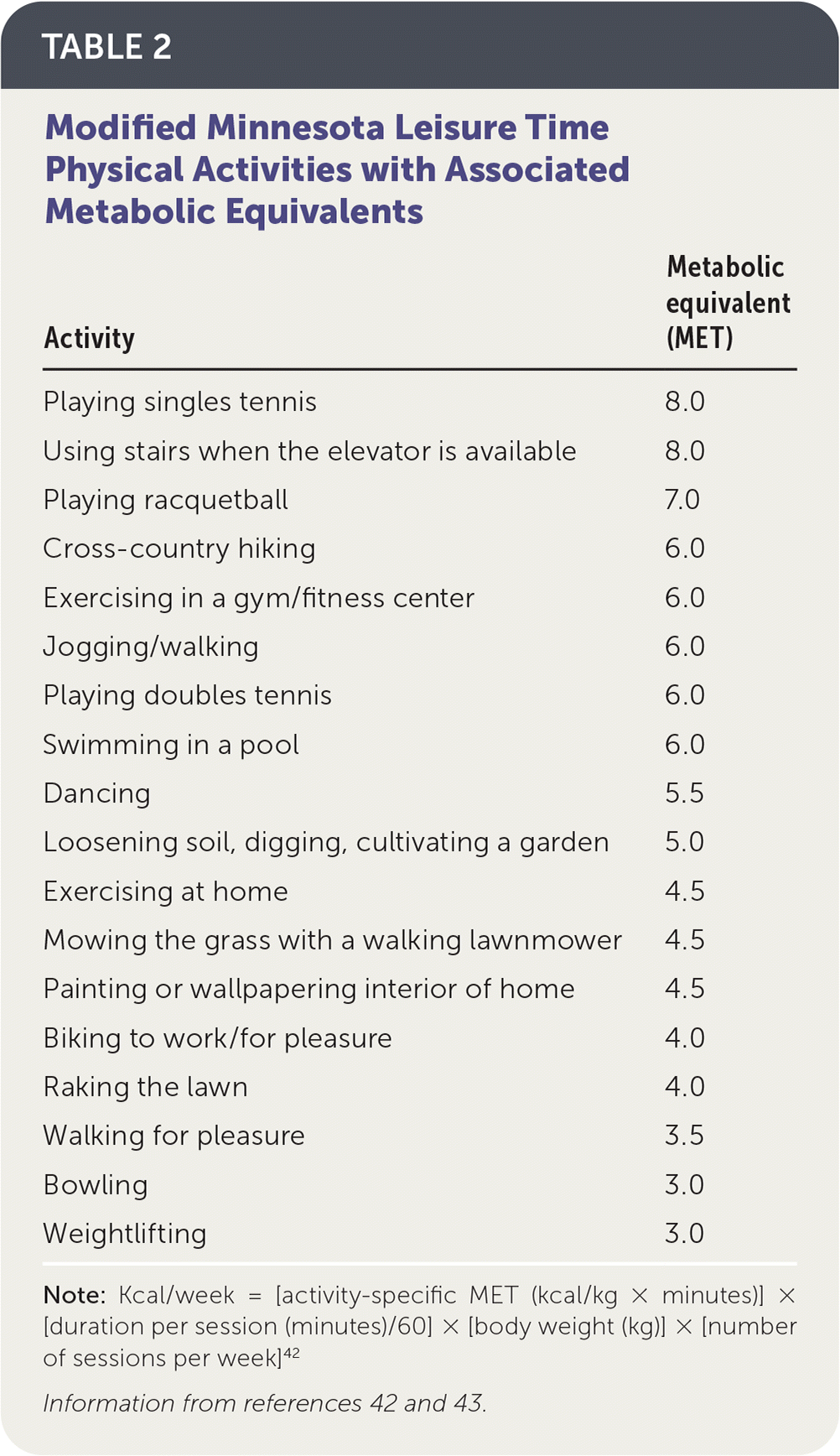
A modified version of the Minnesota Leisure Time Physical Activity Questionnaire is used to determine physical activity by calculating kilocalorie expenditure per week based on a patient's sex. Energy expenditure below the predefined minimum values meets the criteria for frailty. Table 2 lists the Minnesota leisure activities, associated metabolic equivalents, and kcal expenditure formula.42,43
TABLE 2. Modified Minnesota Leisure Time Physical Activities with Associated Metabolic Equivalents
| Activity | Metabolic equivalent (MET) |
|---|---|
| Playing singles tennis | 8.0 |
| Using stairs when the elevator is available | 8.0 |
| Playing racquetball | 7.0 |
| Cross-country hiking | 6.0 |
| Exercising in a gym/fitness center | 6.0 |
| Jogging/walking | 6.0 |
| Playing doubles tennis | 6.0 |
| Swimming in a pool | 6.0 |
| Dancing | 5.5 |
| Loosening soil, digging, cultivating a garden | 5.0 |
| Exercising at home | 4.5 |
| Mowing the grass with a walking lawnmower | 4.5 |
| Painting or wallpapering interior of home | 4.5 |
| Biking to work/for pleasure | 4.0 |
| Raking the lawn | 4.0 |
| Walking for pleasure | 3.5 |
| Bowling | 3.0 |
| Weightlifting | 3.0 |
Note: Kcal/week = [activity-specific MET (kcal/kg × minutes)] × [duration per session (minutes)/60] × [body weight (kg)] × [number of sessions per week]42
The Rockwood frailty index is an assessment tool that includes a larger number of health indices in patients suspected to be frail. This frailty index uses predefined variables to assess a patient's level of independence, evaluate health history, review physical examination findings, assess cognitive function, and review abnormal laboratory results.6 Each item is scored based on the variable being present or absent. The total number of deficits present are divided by the total number of variables, generating a frailty score between 0 and 1, with a value of 0.25 or greater suggesting frailty.39
The Fried frailty phenotype and the Rockwood frailty index have advanced the field of frailty research. However, their use may prove cumbersome and impractical in certain clinical settings. Several other validated frailty assessment tools, which include elements similar to those used in the frailty phenotype and the frailty index, may be easier to apply in practice. No frailty tool has been proven superior to another.39 Physicians must choose a frailty assessment tool that is appropriate for their patient demographic and practice setting.
Management
Older adults who are frail have a higher likelihood of poor health outcomes that include falls, hospitalizations, institutionalization, disability, and death.1,3–6,44 Compared with nonfrail adults, being diagnosed as prefrail or frail is predictive of a 1.3- to 2.6-fold worsening mobility, decreased activities of daily living, and an overall increased rate of falls, disability, hospitalization, and death.1,45,46 Women are more often diagnosed as frail, but men diagnosed with frailty have a higher mortality rate.45
Several studies have evaluated the dynamic nature of frailty. Over time, transitioning between frailty stages (not-frail, prefrail, frail) can occur, with patients worsening, improving, or maintaining their current degree of frailty.3,22 Research shows that women and patients living in better socioeconomic conditions have a higher likelihood of improving their frailty status.21,45 One study suggested that older adults who are prefrail have a better chance than their frail cohorts to improve their frailty diagnosis.47 However, dementia and cancer limit the chances of improving frailty status.46
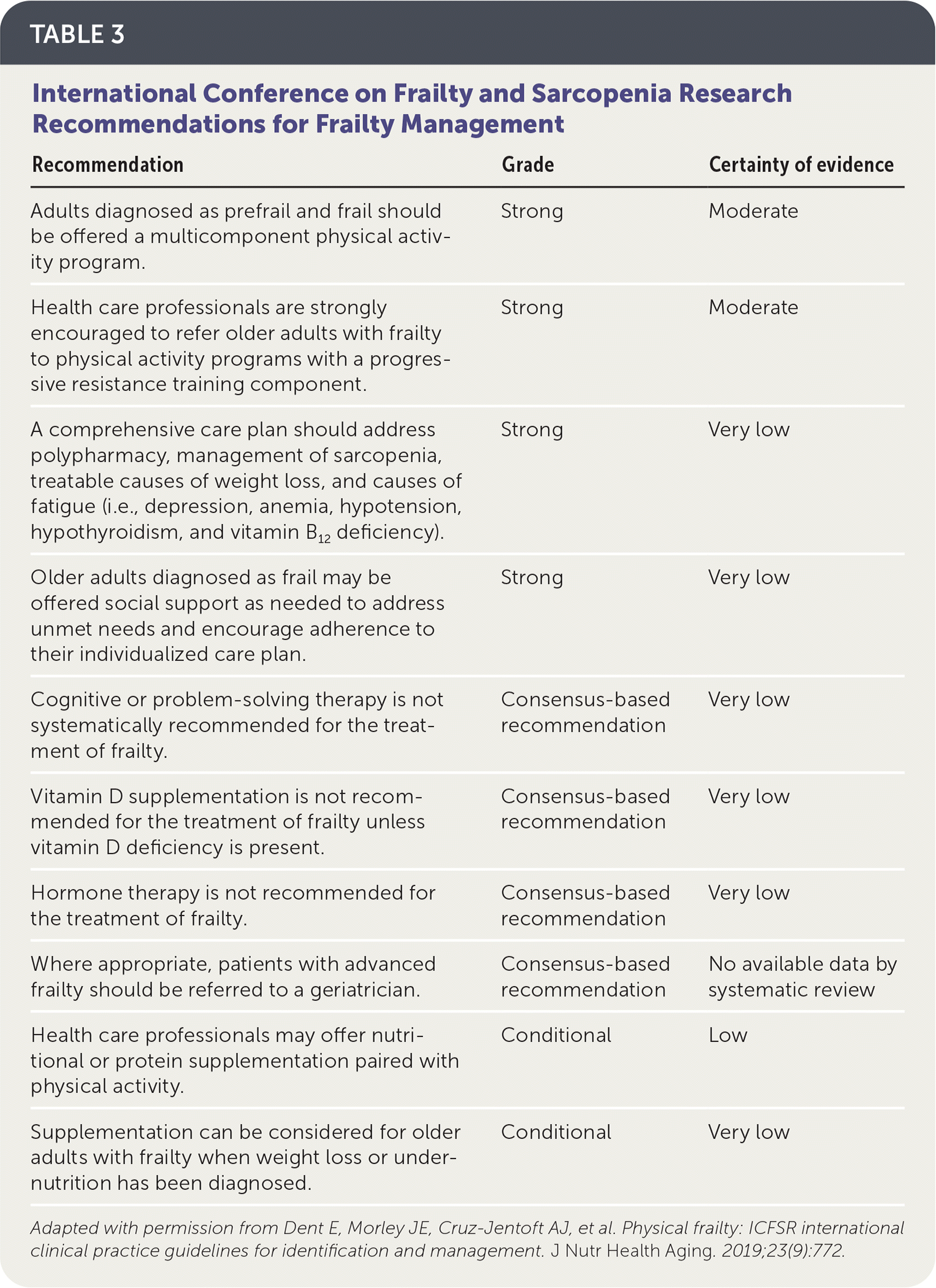
When considering management options, it is important to recognize that patients diagnosed with frailty vary in their presentation and treatment needs. Evidence for an effective, comprehensive care plan is emerging, but there is a lack of quality evidence-based literature to support any specific frailty treatment plan fully. In 2019, the task force of the International Conference on Frailty and Sarcopenia Research (ICFSR) developed clinical practice guidelines for the identification and management of frailty.48 Table 3 outlines the ICFSR frailty management recommendations, based on moderate to very low quality of evidence.48 Clinical judgment is critical when choosing a treatment option. Some older adults may not be capable of initiating or completing certain treatments, and in certain situations, the risk of treatment may outweigh the benefit. In later stages of frailty, palliative care options may be appropriate to discuss.
TABLE 3. International Conference on Frailty and Sarcopenia Research Recommendations for Frailty Management
| Recommendation | Grade | Certainty of evidence |
|---|---|---|
| Adults diagnosed as prefrail and frail should be offered a multicomponent physical activity program. | Strong | Moderate |
| Health care professionals are strongly encouraged to refer older adults with frailty to physical activity programs with a progressive resistance training component. | Strong | Moderate |
| A comprehensive care plan should address polypharmacy, management of sarcopenia, treatable causes of weight loss, and causes of fatigue (i.e., depression, anemia, hypotension, hypothyroidism, and vitamin B12 deficiency). | Strong | Very low |
| Older adults diagnosed as frail may be offered social support as needed to address unmet needs and encourage adherence to their individualized care plan. | Strong | Very low |
| Cognitive or problem-solving therapy is not systematically recommended for the treatment of frailty. | Consensus-based recommendation | Very low |
| Vitamin D supplementation is not recommended for the treatment of frailty unless vitamin D deficiency is present. | Consensus-based recommendation | Very low |
| Hormone therapy is not recommended for the treatment of frailty. | Consensus-based recommendation | Very low |
| Where appropriate, patients with advanced frailty should be referred to a geriatrician. | Consensus-based recommendation | No available data by systematic review |
| Health care professionals may offer nutritional or protein supplementation paired with physical activity. | Conditional | Low |
| Supplementation can be considered for older adults with frailty when weight loss or under-nutrition has been diagnosed. | Conditional | Very low |
Adapted with permission from Dent E, Morley JE, Cruz-Jentoft AJ, et al. Physical frailty: ICFSR international clinical practice guidelines for identification and management. J Nutr Health Aging. 2019;23(9):772.
Physicians are encouraged to develop a patient-specific treatment plan based on shared decision-making. Management should align with each patient's goals of care and life expectancy. Goals of care should be reviewed periodically, especially when there is a change in frailty status, to ensure that the physician, patient, and patient's family have a clear understanding of management options based on life expectancy. The Palliative and Therapeutic Harmonization model is a standardized system for frail patients to help with health care management. The model focuses on obtaining a comprehensive history, ensuring that the patient and family comprehend the patient's vulnerability and potentially shortened life span, assisting with health care decisions that consider frailty, and improving the ability of the team's emergency response system to prepare for appropriate support in the setting of sudden deterioration while paralleling goals of care.49,50
Research focused on early interventions to prevent or reduce the level of frailty in community-dwelling older adults identified physical activity, nutritional support, and psychosocial engagement as possible areas of benefit.51–57 Studies have evaluated these variables independently and in combination as part of an interdisciplinary approach.51,52 Physical activity aims to improve strength and balance based on the American College of Sports Medicine guidelines for older adults.56 Table 4 and Table 5 outline strength training and balance training prescriptions for patients who are frail.55–57 Several European studies demonstrated a reduction in frailty and prevention of frailty progression when nutritional education was added to a physical activity routine.58–60 However, one study involving intensive, multidisciplinary care demonstrated no improvement in overall frailty measures or functional decline.61 Although there is no approved medication to treat any aspect of frailty, addressing polypharmacy may reduce the risk of becoming frail.23,24 Ongoing research is necessary to help better identify optimal treatment strategies.
TABLE 4. Frailty Strength Training Prescription

| Two to three nonconsecutive days per week | |
| Moderate intensity (5 to 6 on a 10-point scale) | |
| Target the major muscle groups with eight to 10 exercises per session | |
| Eight to 15 repetitions per exercise; at least one set of repetitions per exercise* | |
| Gradually increase weight and repetitions based on tolerability† | |
| Strength training exercises: | |
| Sit to stand | |
| Heel lifts | |
| Toe lifts | |
| Lunges | |
| Front arm raises | |
| Side arm raises | |
| Wall push-ups | |
*—Weights may be added to maximize strength.
†—Taking extended time at less-than-moderate intensity may be appropriate for older adults or those diagnosed as frail, in comparison to robust (not-frail) or prefrail adults.
TABLE 5. Frailty Balance Training Prescription

| Two or more hours per week, initially under close supervision to reduce fall risk | |
| Begin with less challenging positions | |
| Maintain each exercise for a minimum of five to 10 seconds, with at least one repetition per exercise | |
| Start on flat surfaces and gradually advance the level of difficulty* | |
| Flat surface exercises: | |
| Side-by-side stance | |
| Semi-tandem stance | |
| Tandem stance | |
| Single limb stance | |
| Heel stance | |
| Toe stance | |
| Uneven surface exercises: | |
| Step up, step down without hand support | |
| Forward and backward walking | |
| Sideways walking | |
| Change directions while walking | |
| Complex task exercises: | |
| Navigate obstacles while walking | |
| Pick up objects from the floor while walking | |
| Carry objects of variable weight and size while walking | |
| Incorporate head turns while reaching in different directions | |
| Carry on conversation while walking | |
| Conduct simple mathematical calculations while walking | |
*—Remove arm support, followed by base support, and then add complex tasks.
Data Sources: PubMed and Google Scholar were searched using the key terms (alone and in combination) geriatric, frailty, syndrome, older adult, elderly, frailty index, frailty phenotype, classification, criteria, comprehensive geriatric assessment, fitness, management, and polypharmacy. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Cochrane database, Essential Evidence Plus, the Institute for Clinical Systems Improvement, and DynaMed. Search dates: January 15 to 27, 2020, and November 2, 2020.

