Study Population: Adults with distal deep venous thrombosis (DVT) diagnosed using venography or ultrasonography
Efficacy End Points: Incidence of recurrent venous thromboembolism (DVT or pulmonary embolism) and mortality
Harm End Points: Incidence of major bleeding and incidence of clinically relevant nonmajor bleeding
TREATMENT OF DISTAL DVT
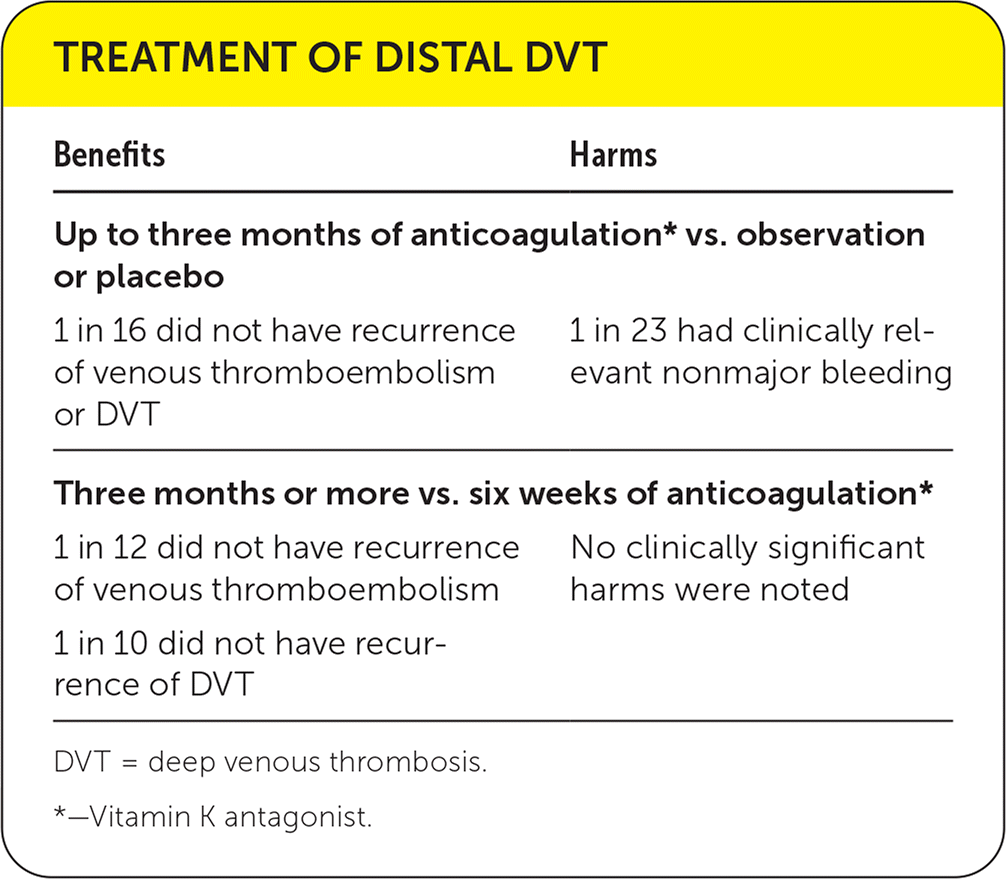
| Benefits | Harms |
|---|---|
| Up to three months of anticoagulation* vs. observation or placebo | |
| 1 in 16 did not have recurrence of venous thromboembolism or DVT | 1 in 23 had clinically relevant nonmajor bleeding |
| Three months or more vs. six weeks of anticoagulation* | |
| 1 in 12 did not have recurrence of venous thromboembolism 1 in 10 did not have recurrence of DVT | No clinically significant harms were noted |
DVT = deep venous thrombosis.
*—Vitamin K antagonist.
Narrative: Distal (below the knee) DVT includes thrombosis of the tibial, peroneal, soleal, and gastrocnemius veins.1 Worldwide, the incidence of distal DVT in adults is estimated to be 0.1% per year, and distal DVT encompasses about one-third to one-half of all lower extremity DVTs.2,3 The standard treatments for distal DVT include anticoagulation or close observation with repeat evaluations to monitor for potential progression of the thrombosis, most significantly extension above the knee.3 Observation is a viable option because many distal DVTs will spontaneously resolve, although the exact percentage is unclear.4
The American College of Chest Physicians (CHEST) recommends anticoagulation if risk factors for DVT extension are present (weak recommendation with low-quality evidence).5 Risk factors include a positive d-dimer test result, extensive thrombosis (greater than 5 cm in length, involves multiple veins, greater than 7 mm in maximum diameter, close to proximal veins), no reversible provoking factor for DVT, active cancer, history of venous thromboembolism, or inpatient status. If no risk factors are present, CHEST recommends observation (weak recommendation with low-quality evidence). In patients at high risk of bleeding, observation is preferred.5
This Cochrane review evaluated the best treatments for distal DVT and included eight randomized controlled trials and 1,239 adult participants.6 Primary outcomes included recurrence of venous thromboembolism and major bleeding episodes. Secondary outcomes included clinically relevant nonmajor bleeding and overall mortality. Five studies compared anticoagulation with vitamin K antagonists for up to three months vs. observation or placebo. The number needed to treat (NNT) to prevent one recurrence of venous thromboembolism was 16 (risk ratio [RR] = 0.34; 95% CI, 0.15 to 0.77). The NNT to prevent one recurrence of DVT was 16 (RR = 0.25; 95% CI, 0.10 to 0.67). The number needed to harm (NNH) to cause clinically relevant nonmajor bleeding was 23 (RR = 3.34; 95% CI, 1.07 to 10.46), with no clinically significant effect on major bleeding or overall mortality. Three studies compared anticoagulation with vitamin K antagonists for three months or more vs. six weeks. Anticoagulation for three months or more was superior, with an NNT of 12 for recurrence of venous thromboembolism (RR = 0.42; 95% CI, 0.26 to 0.68) and an NNT of 10 for recurrence of DVT (RR = 0.32; 95% CI, 0.16 to 0.64). No clinically significant change in occurrence of pulmonary embolism or in overall mortality was noted.6
Caveats: Regarding the comparison of anticoagulation vs. observation or placebo, the Cochrane review authors rated the quality of evidence as high for recurrence of venous thromboembolism and clinically relevant nonmajor bleeding. The quality of evidence was rated as low for pulmonary embolism and major bleeding. Regarding the comparison of anticoagulation for three months or more vs. only six weeks, the quality of the evidence was high for recurrence of DVT and low for pulmonary embolism, major bleeding, and clinically relevant nonmajor bleeding.
The quality of the evidence was downgraded by the authors because of imprecision of the results and the small number of patients. There was significant bias because only one study was double blind; the other seven were open label.6
Conclusion: The Cochrane review demonstrated that anticoagulation was effective and superior to observation; however, given the limited number of patients, potential biases, and conflicting recommendations from CHEST, we give this treatment a yellow rating (unclear benefits). Further studies, specifically larger randomized controlled trials, are needed to confirm the best treatment for distal DVT.

