Clinical Question
Which treatments for basal cell carcinoma (BCC) have the lowest recurrence rates and most favorable cosmetic outcomes?
Evidence-Based Answer
The recurrence rate after surgical management of BCC by standard surgical excision or Mohs micrographic surgery is very low (recurrence at five years = 5.2% vs. 3.2%, respectively; 95% CI, 0.9% to 10.7%). Recurrence after management with imiquimod (Aldara) is also low (recurrence at five years = 17.5%) and may result in more favorable cosmetic outcomes. (Strength of Recommendation [SOR]: B, based on moderate-quality patient-oriented evidence.) Other nonsurgical options may have acceptably low rates of recurrence but also have low certainty of evidence.1 (SOR: B, based on inconsistent or limited-quality patient-oriented evidence.)
SUMMARY TABLE
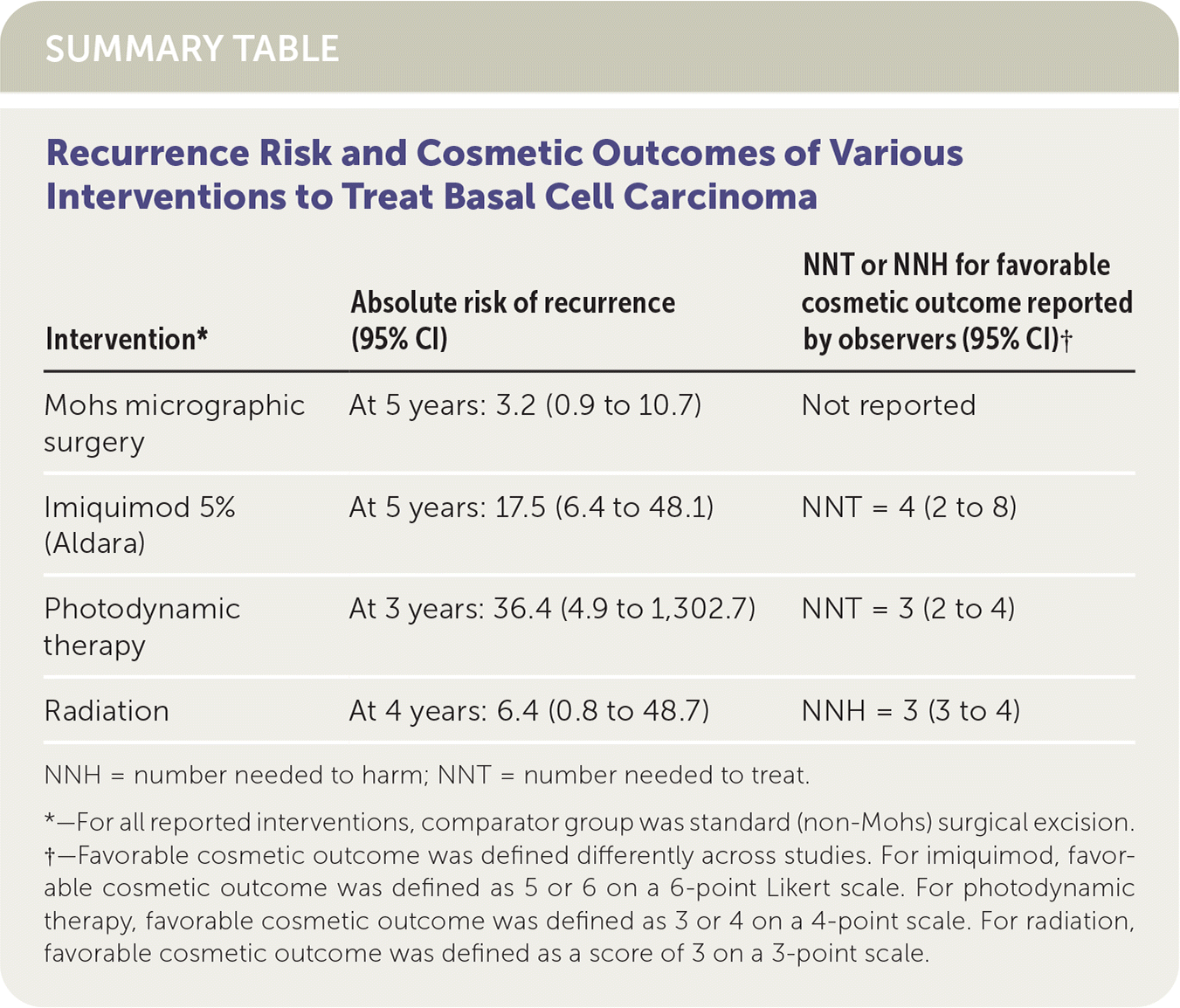
| Intervention* | Absolute risk of recurrence (95% CI) | NNT or NNH for favorable cosmetic outcome reported by observers (95% CI)† |
|---|---|---|
| Mohs micrographic surgery | At 5 years: 3.2 (0.9 to 10.7) | Not reported |
| Imiquimod 5% (Aldara) | At 5 years: 17.5 (6.4 to 48.1) | NNT = 4 (2 to 8) |
| Photodynamic therapy | At 3 years: 36.4 (4.9 to 1,302.7) | NNT = 3 (2 to 4) |
| Radiation | At 4 years: 6.4 (0.8 to 48.7) | NNH = 3 (3 to 4) |
NNH = number needed to harm; NNT = number needed to treat.
*—For all reported interventions, comparator group was standard (non-Mohs) surgical excision.
†—Favorable cosmetic outcome was defined differently across studies. For imiquimod, favorable cosmetic outcome was defined as 5 or 6 on a 6-point Likert scale. For photodynamic therapy, favorable cosmetic outcome was defined as 3 or 4 on a 4-point scale. For radiation, favorable cosmetic outcome was defined as a score of 3 on a 3-point scale.
Practice Pointers
According to one estimate, about one-half of the 5.4 million nonmelanoma skin cancers diagnosed in 2012 were BCC.2 Numerous surgical and nonsurgical treatment options exist. This Cochrane review summarizes evidence for 15 treatments of BCC from 52 randomized controlled trials (RCTs) involving 6,690 participants.1
Most of the studies (48 of 52) included only low-risk superficial or nodular BCC, as defined by the National Comprehensive Cancer Network.3 Although not further defined in the review, low-risk lesions were generally smaller, slower growing, and outside of cosmetically challenging areas such as the face or genitals. The review identified four treatments: Mohs micrographic surgery, imiquimod, photodynamic therapy, and radiation. Primary outcomes were recurrence at three to five years after diagnosis and favorable cosmetic result.
For low-risk BCC, radiation resulted in a higher recurrence rate than standard surgical excision at four years (relative risk [RR] = 11.06; 95% CI, 1.44 to 84.77). There were mixed results regarding the benefits of cryotherapy. Compared with patients treated with radiation, those treated with cryotherapy had significantly more recurrences at one year, yet compared with photodynamic therapy, cryotherapy was not shown to result in any statistically significant difference in recurrence rate. The difference between five-year recurrence rates after standard surgical excision (5.2%) and Mohs micrographic surgery (3.2%) was not statistically significant based on one small low-quality RCT, indicating similar effectiveness.
Although surgical management of BCC appeared to be most effective at preventing recurrence, conservative measures have reasonably low recurrence rates and may have more favorable cosmetic outcomes. Imiquimod 5% cream applied daily for six weeks (superficial BCC) or 12 weeks (nodular BCC) resulted in more patients achieving favorable observer-rated cosmetic results on a Likert scale compared with standard surgical excision three years after the treatments were administered (number needed to treat [NNT] for one additional patient to achieve good or excellent observer-rated cosmetic result = 4; 95% CI, 2 to 8). Study quality was considered low because the data came from a single study (n = 344), and there was a high risk of bias due to difficulty in blinding and the subjective nature of the cosmetic outcome. Within the same study group, recurrence at five years with imiquimod was 17.5% vs. 2.3% with standard surgical excision (RR for recurrence with imiquimod = 7.73; 95% CI, 2.81 to 21.30; n = 383).
Treatment with photodynamic therapy also yielded favorable cosmetic outcomes. Compared with patients undergoing standard surgical excision, those who had photodynamic therapy with two sessions separated by one week were more likely to have a favorable observer-rated cosmetic outcome (NNT for one additional patient to achieve a good or excellent observer-rated cosmetic result = 3; 95% CI, 2 to 4). Recurrence was only reported at three years and favored standard surgical excision over photodynamic therapy (RR for recurrence with photodynamic therapy = 26.47; 95% CI, 1.63 to 429.92). One RCT (n = 347) demonstrated that radiation therapy was inferior at achieving favorable cosmetic outcomes (rated by observers and participants) compared with surgery.
Limitations of this review include the heterogeneity of treatments and their outcomes. In addition, most of the studies of imiquimod were industry-funded and unblinded. The reported cosmetic outcomes were subjective, and in several of the included studies, observers performed the rating rather than participants, which may be considered a less patient-centered result. Finally, data on race-specific outcomes were not included because most of the studies either did not report or did not define race.
The American Academy of Dermatology recommends surgical excision for low-risk BCC but states that nonsurgical options are reasonable alternatives.3 The Choosing Wisely Initiative recommends deferring Mohs micrographic surgery referral in patients with uncomplicated, nonmelanoma skin cancer less than 1 cm in size on the trunk or extremities.4
The practice recommendations in this activity are available at http://www.cochrane.org/CD003412.
Editor's Note: The NNTs, NNH, and their corresponding CIs reported in this Cochrane for Clinicians were calculated by the authors based on raw data provided in the original Cochrane review.

