Vocal cord dysfunction (i.e., vocal cords closing when they should be opening, particularly during inspiration) should be suspected in patients presenting with inspiratory stridor or wheezing; sudden, severe dyspnea (without hypoxia, tachypnea, or increased work of breathing); throat or chest tightness; and anxiety, particularly in females. Common triggers include exercise, asthma, gastroesophageal reflux disease, postnasal drip, upper or lower respiratory tract infection, and irritants. Nasolaryngoscopy and pulmonary function testing, with provocative exercise and methacholine, can help diagnose vocal cord dysfunction and are helpful to evaluate for other etiologies. Conditions that can trigger vocal cord dysfunction should be optimally treated, particularly asthma, gastroesophageal reflux disease, and postnasal drip, while avoiding potential irritants. Therapeutic breathing maneuvers and vocal cord relaxation techniques are first-line therapy for dyspnea that occurs with vocal cord dysfunction. A subset of vocal cord dysfunction leads to dysphonia, as opposed to dyspnea, secondary to abnormal laryngeal muscle spasms (vocal cord closure is less severe). OnabotulinumtoxinA injections may be helpful for spasmodic dysphonia and for treating dyspnea in certain cases, although evidence is limited.
Vocal cord dysfunction is a condition in which the vocal cords close when they should be opening, particularly during inspiration. This can be more severe and impair breathing or, more commonly, less severe and impact the patient's voice. This article is a brief summary and review of the best available evidence for the presentation, diagnosis, and management of vocal cord dysfunction.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
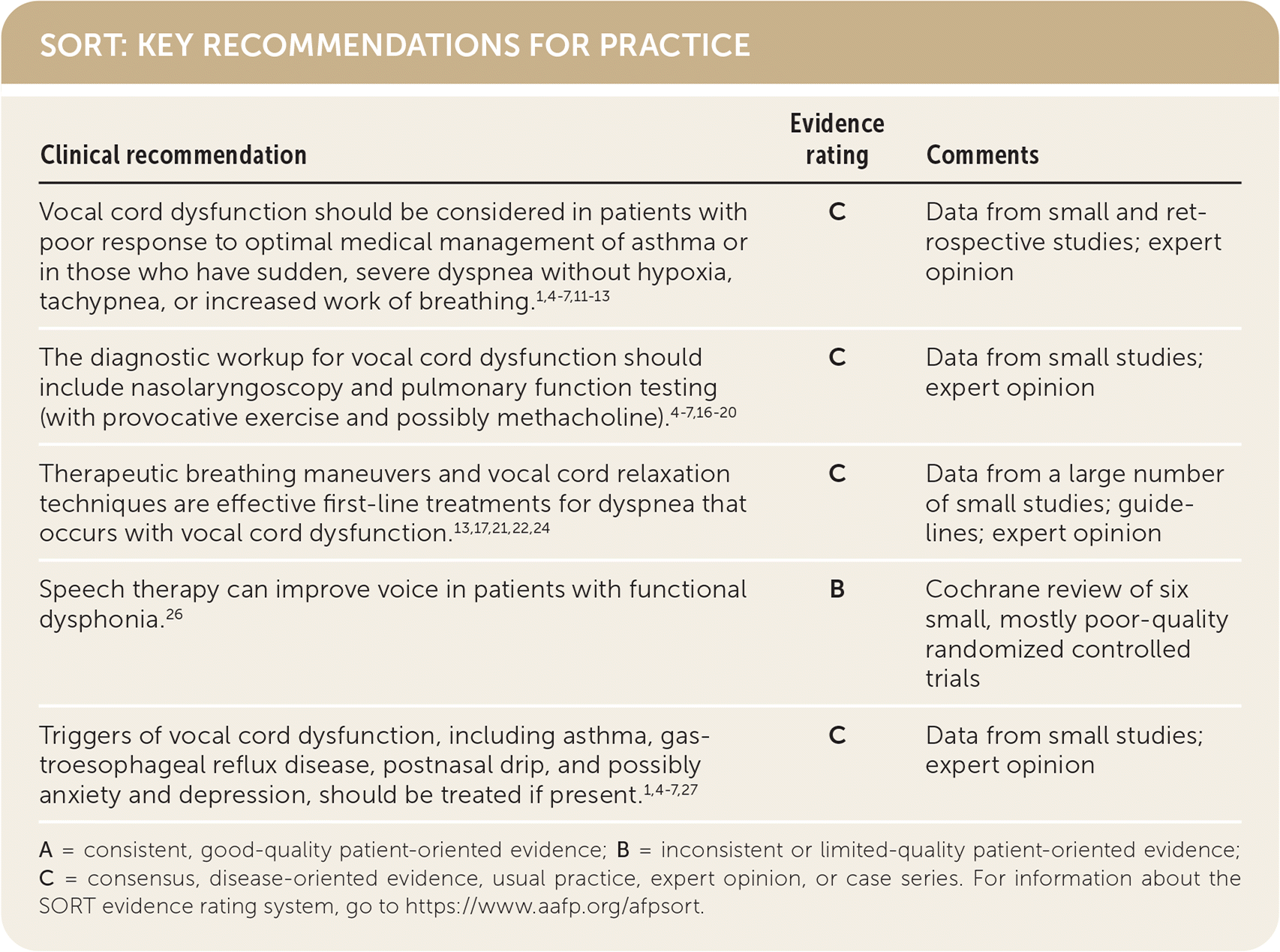
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Epidemiology
- Vocal cord dysfunction predominantly occurs in females (prevalence is two to three times greater in females than in males).1,2
- It occurs at any age but is more commonly diagnosed in patients 30 to 40 years of age.1
- It may coexist with asthma (25% to 30%),3,4 gastroesophageal reflux disease, or anxiety disorders.1,4–7
- Vocal cord dysfunction is categorized as inducible laryngeal obstruction and is known by many other names,2,8–10 which are listed in Table 1.8
TABLE 1. Other Terms Used to Describe Vocal Cord Dysfunction

| Emotional laryngeal asthma |
| Episodic laryngeal dyskinesia |
| Exercise-induced dyspnea |
| Factitious asthma |
| Functional dysphonia |
| Inducible laryngeal obstruction |
| Irritable larynx syndrome |
| Laryngospasm |
| Munchausen stridor |
| Paradoxical vocal cord dysfunction |
| Paradoxical vocal fold motion |
| Psychosomatic stridor |
| Spasmodic dysphonia |
Information from reference 8.
Diagnosis
- Vocal cord dysfunction should be considered in patients with poor response to optimal medical management of asthma or in those who have sudden, severe dyspnea without hypoxia, tachypnea, or increased work of breathing.1,4–7,11–13
- The differential diagnosis includes poorly controlled asthma, anatomic defects, laryngeal edema, nerve injury, and neurologic disorders11 (Table 2).
- A suggested approach to the diagnosis of vocal cord dysfunction includes obtaining a clinical history focusing on triggers (Table 3) and symptoms, physical examination focusing on location and timing of stridor or wheezing, pulmonary function testing, and direct nasolaryngoscopy performed during an episode.1,4–7
TABLE 2. Differential Diagnosis of Vocal Cord Dysfunction
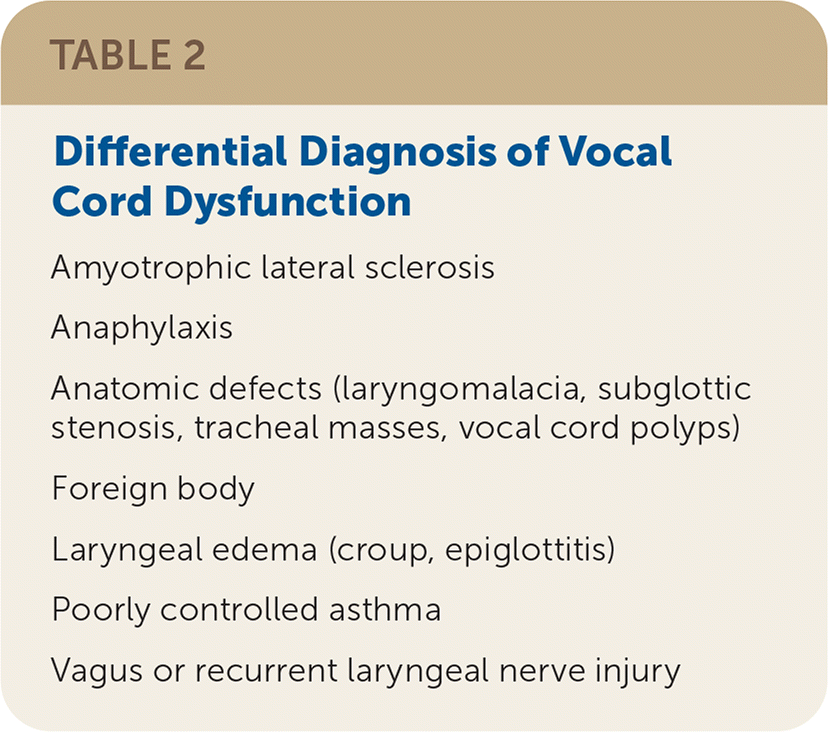
| Amyotrophic lateral sclerosis |
| Anaphylaxis |
| Anatomic defects (laryngomalacia, subglottic stenosis, tracheal masses, vocal cord polyps) |
| Foreign body |
| Laryngeal edema (croup, epiglottitis) |
| Poorly controlled asthma |
| Vagus or recurrent laryngeal nerve injury |
TABLE 3. Reported Triggers for Episodes of Vocal Cord Dysfunction

| Exercise |
| Inflammatory states |
| Asthma |
| Episodic croup |
| Gastroesophageal reflux disease |
| Postnasal drip |
| Recent upper or lower respiratory tract infection |
| Irritants |
| Dry, cold air |
| Toxin inhalation |
| Workplace chemicals |
| Postoperative injury (with vocal cord paresis) |
| Psychiatric conditions |
| Generalized anxiety disorder |
| Major depression |
| Obsessive-compulsive disorder |
| Performance stress/anxiety |
SIGNS AND SYMPTOMS
- Many symptoms are a result of difficulty with breathing in air due to inappropriate closure of the vocal cords during inspiration. These symptoms include: Inspiratory stridor11
Wheezing, predominantly over the upper airway11
Severe, sudden dyspnea without oxygen desaturation, tachypnea, or increased work of breathing; often associated with anxiety11–13
Chest or throat tightness12
Chronic cough may be an associated condition, although it typically does not occur during symptoms related to vocal cord dysfunction14
Onset with exposure to known triggers (Table 3)
- When the vocal cord closure is less severe (from abnormal laryngeal muscle spasm), it impacts the voice, but not breathing, causing dysphonia or aphonia.15
DIAGNOSTIC TESTING
- The diagnostic standard is direct visualization of vocal cord adduction during inspiration using nasolaryngoscopy.7 Diagnostic yield of nasolaryngoscopy is improved when the patient is experiencing symptoms and with provocation, such as exercise or use of methacholine.3–5,11–15 Based on expert opinion, nasolaryngoscopy should be performed when signs and symptoms suggest vocal cord dysfunction.
- In patients with vocal cord dysfunction, pulmonary function testing may show a flattened inspiratory flow loop or FEF50/FIF50 (ratio of expiratory flow to inspiratory flow at 50% of forced vital capacity) of 1 or greater.6,7,11 Yield is higher when the patient is experiencing symptoms.6 Use of methacholine during pulmonary function testing helps evaluate for asthma as an alternative diagnosis.7,16–20
- Pulmonary function testing should be performed when signs and symptoms suggest vocal cord dysfunction or when asthma is considered as a possible etiology.
- If asthma is being considered, initial pulmonary function testing should be ordered before flexible nasolaryngoscopy. However, if asthma is unlikely, flexible nasolaryngoscopy should be used for the initial evaluation based on expert opinion.
- Chest radiography may be considered to evaluate for other etiologies, such as a compressive mass, although vocal cord dysfunction tends to cause more intermittent symptoms.
- Reviewing a patient-generated video of an acute, symptomatic episode can be helpful to assess signs and symptoms.
Treatment
ACUTE ATTACKS
- Therapeutic breathing maneuvers and vocal cord relaxation techniques (see examples at https://www.youtube.com/watch?v=cKHd935oRBg) are recommended based on expert opinion, in the absence of clinical trials.13,17,21,22
- Coexisting asthma should be treated with usual asthma care.
- Heliox (a mixture of helium and oxygen) has been described as a potential treatment, but evidence is lacking.23
CHRONIC MANAGEMENT
- There are no randomized trials to guide selection of therapy, which is largely based on expert opinion and pathophysiologic reasoning.
- Therapeutic breathing maneuvers and vocal cord relaxation techniques are first-line therapy for dyspnea that occurs with vocal cord dysfunction.13,17,21,22,24 A single case study suggests that using aerodynamic feedback (real-time display of air flow and pressure changes during exhalation and phonation) can be helpful in learning breathing maneuvers.25 Speech therapy teaches these techniques.
- A systematic review of six small, mostly poor-quality randomized controlled trials with 163 participants showed that speech therapy, including direct voice therapy and indirect voice therapy (education and counseling), improved voice in the treatment of functional dysphonia.26
- Coexisting asthma, gastroesophageal reflux disease, and postnasal drip should be treated. Treating comorbid psychiatric conditions may be helpful for vocal cord dysfunction, but data are conflicting and limited.1,4–7,27
- Based on guidelines from the American Academy of Otolaryngology–Head and Neck Surgery, onabotulinumtoxinA (Botox) injections into the laryngeal muscles may be used for the treatment of spasmodic dysphonia.28 These injections may be helpful in vocal cord dysfunction with dyspnea or concomitant asthma that is resistant to optimized asthma treatment, but evidence is limited.14,26,28–30
- Patients should avoid triggers, including irritants (Table 3).
- Behavioral counseling should be considered for patients with comorbid anxiety and depression.27
REFERRAL
- Referral to an ears, nose, and throat specialist should be considered for further evaluation (with nasolaryngoscopy) and management.
- Referral to a speech therapist should be considered for therapeutic breathing maneuvers, vocal cord relaxation techniques, and speech therapy (initial management).
Prognosis
- A small cohort study found that a multidisciplinary treatment approach for vocal cord dysfunction was associated with 57% fewer emergency department visits and/or hospital admissions and 52% fewer ambulatory clinic visits.31
- Other small case series have reported that appropriate diagnosis and treatment result in symptom improvement and decreased use of asthma medications, although there were no comparison groups.32–34
This article updates a previous article on this topic by Deckert and Deckert.35
Data Sources: A PubMed search was conducted using the terms vocal cord dysfunction, laryngospasm, paradoxical vocal fold motion, paradoxical vocal cord dysfunction, spasmodic dysphonia, episodic laryngeal dyskinesia, exercise induced dyspnea, inducible laryngeal obstruction, irritable larynx syndrome, emotional laryngeal asthma, factitious asthma, functional dysphonia, Munchausen stridor, and psychomotor stridor combined with the terms diagnosis, management, and treatment. These terms were also used to search the Agency for Healthcare Research and Quality, Essential Evidence Plus, and the Cochrane Database of Systematic Reviews. Search dates: October 15 to 17, 2020.

