Borderline personality disorder is a psychological disorder characterized by a pervasive pattern of instability in affect regulation, impulse control, interpersonal relationships, and self-image. Borderline personality disorder may be present in up to 6.4% of adult primary care visits, which is fourfold higher than in the general population. Borderline personality disorder is underdiagnosed and most patients who have it also have additional psychiatric conditions. Individuals with borderline personality disorder have an underlying vulnerability to emotional hyperarousal states and social and interpersonal stressors. Clinically these patients may have high health care utilization, health-sabotaging behaviors, chronic or vague somatic concerns, aggressive outbursts, high-risk sexual behaviors, and substance use. Obesity and binge-eating disorders are common comorbidities in those diagnosed with borderline personality disorder. There is an established correlation between borderline personality disorder and increased suicide risk. Structured interview assessments that are designed specifically for borderline personality disorder include the Revised Diagnostic Interview for Borderlines and the Structured Clinical Interview for the DSM-5 Alternative Model for Personality Disorders. As general guidelines for practice, family physicians should avoid excessive familiarity, schedule regular visits, set appropriate limits, and maintain awareness of personal feelings. Use of effective communication strategies such as motivational interviewing and problem-solving techniques can help navigate addressing problematic behaviors in patients who have borderline personality disorder. Multiple behavior treatments are useful, the most effective of which are dialectical behavior therapy and mentalization-based therapy. No medications have been approved by the U.S. Food and Drug Administration specifically for the treatment of borderline personality disorder.
Borderline personality disorder is a psychological disorder with a characteristic pervasive pattern of instability in affect regulation, impulse control, interpersonal relationships, and self-image.1 Patients with borderline personality disorder are often characterized as difficult because of aggressive outbursts, health-sabotaging behaviors (i.e., exercising on an injury), and high health care utilization.2,3
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | Comments |
|---|---|---|
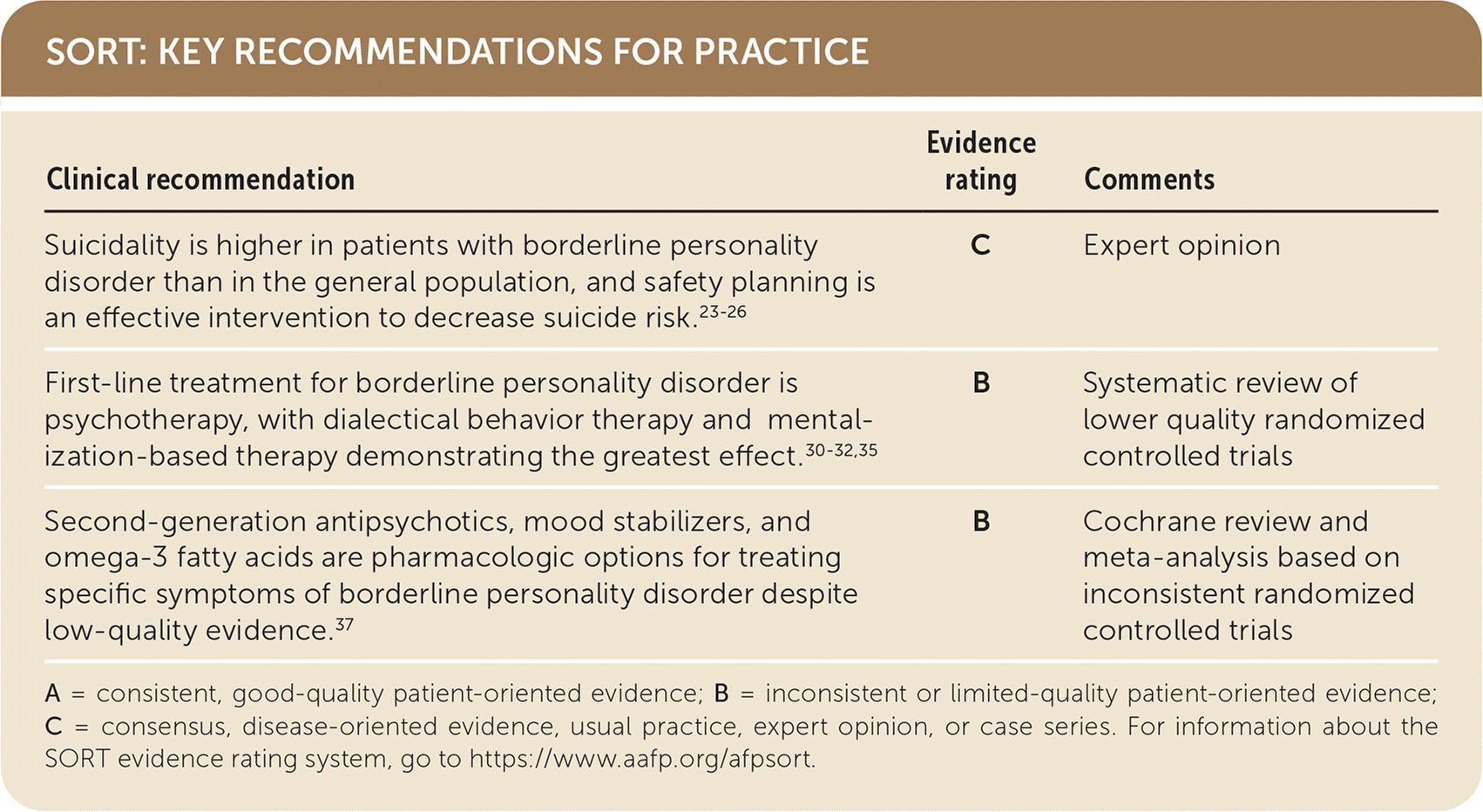
| Suicidality is higher in patients with borderline personality disorder than in the general population, and safety planning is an effective intervention to decrease suicide risk.23–26 | C | Expert opinion |
| First-line treatment for borderline personality disorder is psychotherapy, with dialectical behavior therapy and mentalization-based therapy demonstrating the greatest effect.30–32,35 | B | Systematic review of lower quality randomized controlled trials |
| Second-generation antipsychotics, mood stabilizers, and omega-3 fatty acids are pharmacologic options for treating specific symptoms of borderline personality disorder despite low-quality evidence.37 | B | Cochrane review and meta-analysis based on inconsistent randomized controlled trials |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Borderline personality disorder has a prevalence of 1.6% in the general population.4 In one study, it was found to be present in 6.4% of adult primary care visits, about fourfold higher than what has been noted in general community studies.4–6 Psychiatric diagnostic comorbidities are common. According to one epidemiologic survey, 85% of patients with borderline personality disorder had at least one comorbid psychiatric disorder.7 There is an established correlation between increased suicide risk and a diagnosis of borderline personality disorder.8
Etiology and Pathogenesis
Borderline personality disorder is thought to be caused by a combination of genetic, neurobiologic, and psychosocial factors, with moderate evidence for genetic transmission and heritability, combined with environmental factors such as trauma.1 Trauma and neglect may exacerbate biologic predisposition and behavioral tendencies already present in those with borderline personality disorder.9 Nearly one-third of patients with borderline personality disorder have been raped or sexually assaulted during adulthood.8
In a study of Hispanic patients in primary care, childhood and adulthood interpersonally traumatic events were strongly associated with borderline personality disorder.10 Increased awareness of the prevalence of the disorder among underrepresented ethnic minorities receiving primary care, in addition to the high rates of trauma exposure in this population, may enhance physicians' ability to detect borderline personality disorder in these patients and provide appropriate referrals.10
Clinical Presentation
HALLMARK SYMPTOMS
The core features of borderline personality disorder are instability of interpersonal relationships, negative self-image, and marked impulsivity, especially in expressing emotions, controlling moods, and exhibiting chronic suicidal tendencies.1,11 Borderline personality disorder can also present as multiple vague somatic complaints, high-risk sexual behaviors, binge eating, or chronic pain.5 Patients commonly engage in splitting, which is when relationships are rapidly devalued or over-valued (e.g., in one moment the patient can highly appreciate a clinician and then reverse this opinion when an appointment needs to be rescheduled or another perceived rejection occurs).6 A useful model organizes the disorder into three dimensions that are outlined in Table 1.11,12
TABLE 1. Clinical Features of Various Dimensions of Borderline Personality Disorder

| Dimension | Clinical features |
|---|---|
| Emotion dysregulation | Intense moods, sudden mood shifts, outbursts of anger, self-harm, increased risk of suicide |
| Interpersonal problems | Chronic loneliness and emptiness, recklessness and impulsivity, fear of being abandoned, persistent efforts to avoid feeling unaccepted and/or unloved |
| Self-identity disturbance | Aggressive impulses, lack of an integrated sense of self, persistent unstable self-image, transient paranoia, and/or severe dissociative symptoms |
Although longstanding beliefs suggest borderline personality disorder has a chronic unchanging course over a patient's lifespan, most patients will experience remission.6,13 Predictors of good outcomes include factors related to self-efficacy and a favorable psychosocial history, whereas predictors of poor outcomes include greater severity and chronicity of illness, higher degrees of comorbidity, and a history of childhood adversity.13 Despite high rates of remission over time, global functioning may not improve, with up to 75% of patients who have borderline personality disorder lacking full-time employment, even during remission.6,11
DIAGNOSTIC CRITERIA
Table 2 lists the diagnostic criteria for borderline personality disorder as outlined in the Diagnostic and Statistical Manual of Mental Disorders, 5th ed. (DSM-5).14 The clinical diagnosis is based on a comprehensive psychiatric assessment that gathers information from multiple sources, including a self-reported clinical history, clinician observations, review of the patient's medical record, and information from the patient's friends and family. The McLean Screening Instrument for Borderline Personality Disorder is a self-report measure that screens patients for the disorder, but it is not intended to make a diagnosis.15 Borderline personality disorder is chronically underdiagnosed in clinical populations, and use of structured interviews is encouraged to improve assessment.16 Interview assessments that are designed specifically for borderline personality disorder include the Revised Diagnostic Interview for Borderlines and the Structured Clinical Interview for the DSM-5 Alternative Model for Personality Disorders.17,18
TABLE 2. DSM-5 Diagnostic Criteria for Borderline Personality Disorder

A pervasive pattern of instability of interpersonal relationships, self-image, and affects, and marked impulsivity, beginning by early adulthood and present in a variety of contexts, as indicated by five (or more) of the following:
|
Reprinted with permission from the Diagnostic and Statistical Manual of Mental Disorders. 5th ed. American Psychiatric Association; 2013:663.
DIFFERENTIAL DIAGNOSIS
The differential diagnosis of borderline personality disorder involves distinguishing it from other psychiatric disorders such as bipolar disorder, major depressive disorder, posttraumatic stress disorder, and other personality disorders. Other comorbidities include persistent depressive disorder, panic disorder with agoraphobia, social anxiety disorder, specific phobia, generalized anxiety disorder, alcohol use disorder, and nicotine use disorder.9,19 Patients with borderline personality disorder are more likely to experience pain and to rate their pain as more severe than patients with other personality disorders.20 Consistent with all personality disorders, patients with borderline personality disorder are more likely to be obese.21 Recognition and appropriate treatment of medical and psychiatric comorbidities may improve long-term functioning of people with borderline personality disorder.20
SUICIDE AND SELF-HARM
Compared with the general population, a large percentage of people with borderline personality disorder attempt suicide, with an average of four attempts, and have a history of psychiatric hospitalizations and evidence of self-harm.8,22 The literature is somewhat limited in offering more than partial knowledge on helping to identify the patients with borderline personality disorder who are most at risk of death by suicide.23 Therefore, it is important to complete careful evaluation of risk and protective factors, thoughts, plans, means, intent, and current levels of impulsivity. Safety planning is a brief, effective intervention to help individuals survive suicidal crises by teaching them a set of steps they can take to reduce the likelihood of engaging in suicidal behavior.24 Tools such as the Suicide Safety Plan can be helpful in identifying warning signs, coping strategies, distractions, and support systems (e.g., family, clinicians, emergency services); restricting means to commit suicide (e.g., removing extra prescriptions from a medicine cabinet); and establishing reasons to live.25,26
Treatment
GENERAL CONSIDERATIONS: STRATEGIES FOR PRIMARY CARE
Difficult patient-physician relationships may signal the presence of borderline personality disorder and complicate medical treatment.4 Individuals with symptoms of borderline personality disorder tend to consult a greater number of primary care physicians and specialists, and experience greater turnover in primary care physicians. A multifaceted management approach for physicians who encounter these patients includes avoiding familiarity; scheduling regular visits; providing clear explanations of diagnosis, testing, and clinical management; tolerating angry outbursts while still setting limits; maintaining awareness of personal feelings; and enlisting the help of a psychiatrist when needed.27
Clinicians can avoid excessive familiarity by setting clear boundaries at the first visit and not responding to a patient's attempts to interact outside of established clinical encounters.6 By ensuring that appointments are routinely scheduled to address patient concerns, judicious medical and clinical boundaries are maintained.6,11 Physicians should set firm limits on manipulative behaviors without judgment or anger.6 When communicating with the patient, the physician should actively interrupt the patient discourse to focus on current scenarios rather than past experiences.11 Acute emotional self-awareness during interactions can help the physician respond to provocative behaviors more easily in a clear-headed, calm manner. Problematic behaviors can be mitigated by using effective communication strategies, such as motivational interviewing and problem-solving techniques, and clear language to address medical concerns.28,29 Importantly, the physician should acknowledge and respond to any patient-communicated threats of harm to self or others, acting on the need to ensure safety while discouraging excessive emergency department visits.11
PSYCHOLOGICAL THERAPIES
First-line treatment for borderline personality disorder is psychotherapy.30 Dialectical behavior therapy and mentalization-based therapy were found to be most effective.31 Dialectical behavior therapy is a form of cognitive behavior therapy that integrates group and individual sessions to help patients manage their emotional lability and impulsive behavior.2 Dialectical behavior therapy has shown positive treatment effects for borderline personality disorder severity, self-harm, and psychosocial functioning. It has effectively reduced suicide attempts and psychiatric hospitalizations in those with borderline personality disorder.32 In a randomized controlled trial comparing fluoxetine (Prozac) therapy with dialectical behavior therapy, the medication-only group was observed to have significantly higher rates of suicide attempts.33 A streamlined version of dialectical behavior therapy has been found to be effective within a few months.34
Mentalization-based therapy aims to increase an individual's understanding of how actions are influenced by mental states, thereby decreasing impulsiveness and emotional lability. Studies have demonstrated reduced self-harm and suicidality by the end of mentalization-based therapy; however, these results were based on low-quality evidence.31,32,35 Although often used for anxiety, depression, and polysubstance abuse, standard cognitive behavior therapy also has evidence to support its use in patients with borderline personality disorder.34
Individuals with borderline personality disorder may have difficulty remaining in psychotherapy and have dropout rates between 22.3% and 29.9%.36 Most dropouts occur in the first half of treatment. Reasons for leaving therapy include dissatisfaction with treatment, expulsion from treatment, lack of motivation, and life events or a change in life situation.36
MEDICATIONS
Pharmacologic treatments for patients with borderline personality disorder remain controversial with limited evidence, despite the common practice of prescribing selective serotonin reuptake inhibitors and quetiapine (Seroquel).37 There are no medications approved by the U.S. Food and Drug Administration for the treatment of borderline personality disorder. Cochrane reviews showed minimal promise for second-generation antipsychotics, mood stabilizers, and omega-3 fatty acids for treating specific symptoms of borderline personality disorder.37 The results were often based on single trials with limited evaluation of adverse events.37 Although some small studies have suggested a therapeutic role for mood stabilizers, a large randomized controlled trial lasting 12 months showed no benefit for lamotrigine (Lamictal) in any dimension of borderline personality disorder.38 Modest beneficial effects of valproate (Depacon) and omega-3 fatty acids in improving depressive symptoms have not been confirmed outside of limited-quality trials.37 Medications such as buprenorphine and naltrexone (Revia) have been used to decrease suicidality and self-injurious behaviors; however, the evidence of benefit is of low quality.39
Given the similarities between affect instability in borderline personality disorder and rapid mood shifting in bipolar disorder, similar medications such as atypical antipsychotics have been used to treat both conditions. However, the evidence for using these medications for borderline personality disorder is limited. 40,41 Clinicians should prioritize medication safety by avoiding polypharmacy and limiting the use of controlled substances when treating borderline personality disorder.6 If medications are prescribed, treatment should be augmented by psychological therapy.11
Data Sources: A PubMed search (including meta-analyses, randomized controlled trials, clinical trials, and reviews) was completed in Clinical Queries using the key terms borderline personality disorder (BPD), BPD diagnosis, BPD and medication, BPD and pharmacotherapy, BPD and quetiapine, BPD and buprenorphine, BPD and suicide risk, BPD and suicide, BPD and safety contract, and BPD and evidence-based treatment. We utilized the summary from Essential Evidence Plus: including potentially relevant POEMs, Cochrane reviews, clinical decision rules, and a targeted PubMed search from Dr. Mark Ebell. We also searched the Agency for Healthcare Research and Quality evidence reports, Clinical Evidence, the Cochrane database, and the Diagnostic and Statistical Manual of Mental Disorders, 5th ed. Search dates: November 2020, December 2020, January 2021, and September 2021.

