A 65-year-old man presented with three days of pain and pressure in his right eye, accompanied by blurred vision and photosensitivity. He did not have pain with eye movement. He had a fever and chills. He had a history of poorly controlled diabetes mellitus and a urinary tract infection a week earlier that was treated with ciprofloxacin.
Physical examination revealed a mildly dilated right pupil, with incomplete constriction to light, compared with the left pupil. A small collection of white fluid was observed in the anterior chamber of the right eye (Figure 1).
FIGURE 1
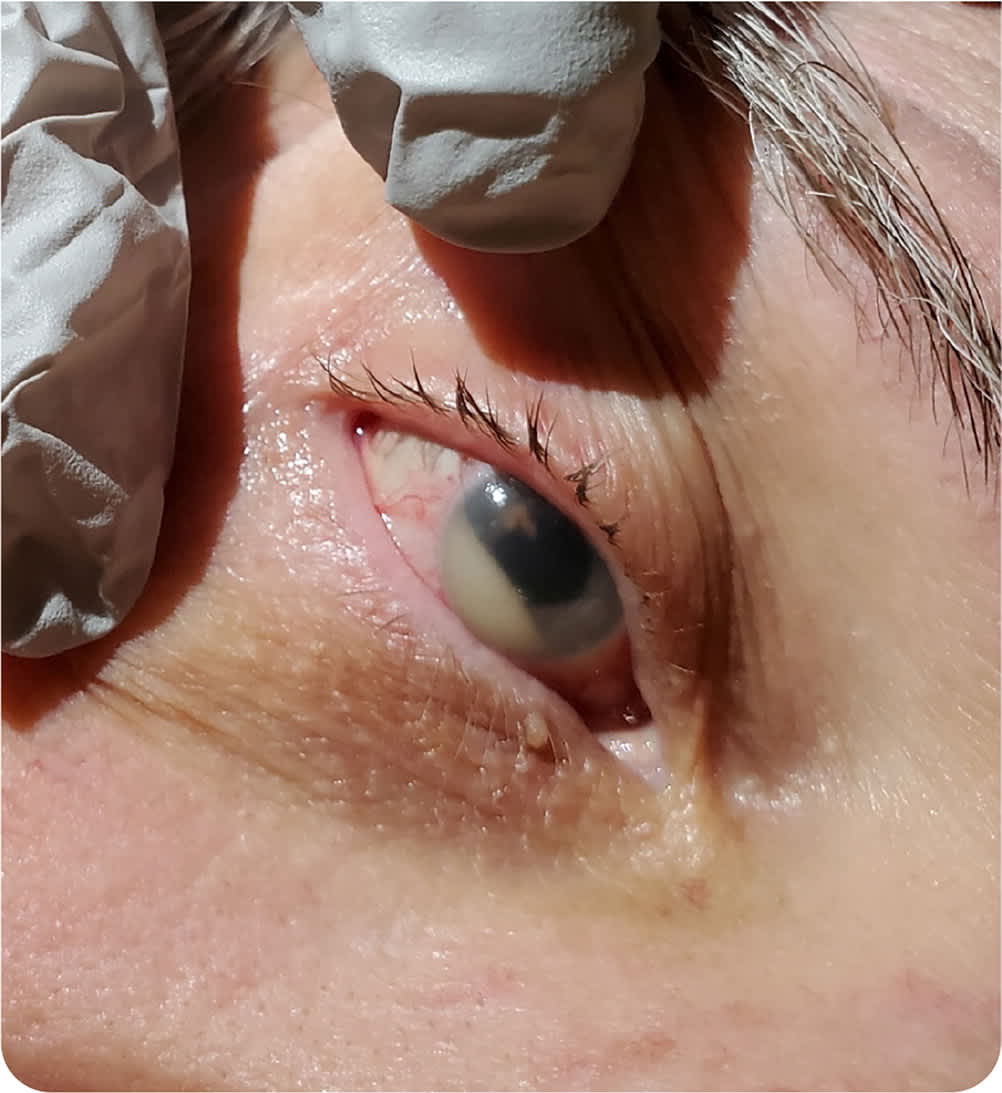
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
- A. Acute glaucoma.
- B. Behçet syndrome.
- C. Corneal ulcer.
- D. Endogenous bacterial endophthalmitis.
- E. Pseudohypopyon.
Discussion
The answer is D: endogenous bacterial endophthalmitis, an intraocular infection caused by hematogenous spread of organisms from an extraocular location.1 Findings include decreased vision, eyelid edema, pupillary abnormalities, hypopyon, and conjunctival injection. Diagnosis is based on physical examination and blood culture findings. Intraocular fluid culture from the anterior chamber and vitreous may be needed to confirm the diagnosis if blood culture results are negative.1 This patient was found to have group B streptococcus bacteremia, confirmed with vitreous culture.
Treatment of endogenous bacterial endophthalmitis includes intravenous antibiotics to manage the systemic infection. The ocular infection may be managed with pars plana vitrectomy, intravitreal antibiotics, and steroids, and the intraocular infection managed with topical steroids, antibiotics, and cycloplegics.2 The prognosis for visual improvement is poor despite treatment. Patients with a history of alcoholism, cardiovascular disease, and diabetes mellitus are at increased risk of endogenous bacterial endophthalmitis.3 Patients with endogenous bacterial endophthalmitis should be evaluated for endocarditis. The hypopyon in this patient indicates leukocytes within the anterior chamber of the eye, which warrants emergent evaluation by an ophthalmologist.4
Acute glaucoma is an ocular emergency. It presents with a mid-dilated fixed pupil with severe eye pain and a prominent ciliary flush. Patients also report nausea, vomiting, cloudy vision, seeing rings around lights, and headache. Acute glaucoma is caused by anterior chamber angle closure in the affected eye, leading to an increased intraocular pressure of more than 40 mm Hg. Hypopyon is not seen in patients with glaucoma. Patients should be emergently referred to an ophthalmologist. Patients should not receive topical steroids or antibiotics because these treatments may lead to infection or corneal ulceration.5
Behçet syndrome is a multisystem inflammatory disorder. The classic presentation is painful mucocutaneous sores in the mouth, anterior uveitis, genital sores, and pathergy (skin rashes resistant to healing). The cause is unknown but may be genetic. Diagnosis is based on the presence of recurrent oral ulcers and at least two of the other classic findings. Hypopyon may occur in 10% to 30% of patients who have Behçet syndrome with anterior uveitis. Behçet syndrome is treated with immunomodulatory therapy and systemic corticosteroids if the patient reports vision changes.6
Most corneal ulcers are caused by direct minor trauma to the eye, such as from contact lenses. The area may become infected with bacteria, viruses, or fungi, usually secondary to the breakdown of the protective epithelial barrier of the eye. Patients with corneal ulcers present with decreased visual acuity, photophobia, and conjunctival injection. Patients should be referred to an ophthalmologist. If consultation or referral is not available within hours, it is reasonable to obtain cultures and start ophthalmic antibiotics immediately.7
Pseudohypopyon is the accumulation of neoplastic cells in the anterior chamber of the eye that usually occurs in patients with lymphoma, leukemia, or retinoblastoma. It may be the only presenting feature of recurrent lymphoma, even in the setting of negative imaging and cerebrospinal fluid findings. Diagnosis can be confirmed with flow cytometry of an anterior chamber aspirate. Patients with bilateral pseudohypopyon have a poor prognosis.8
SUMMARY TABLE
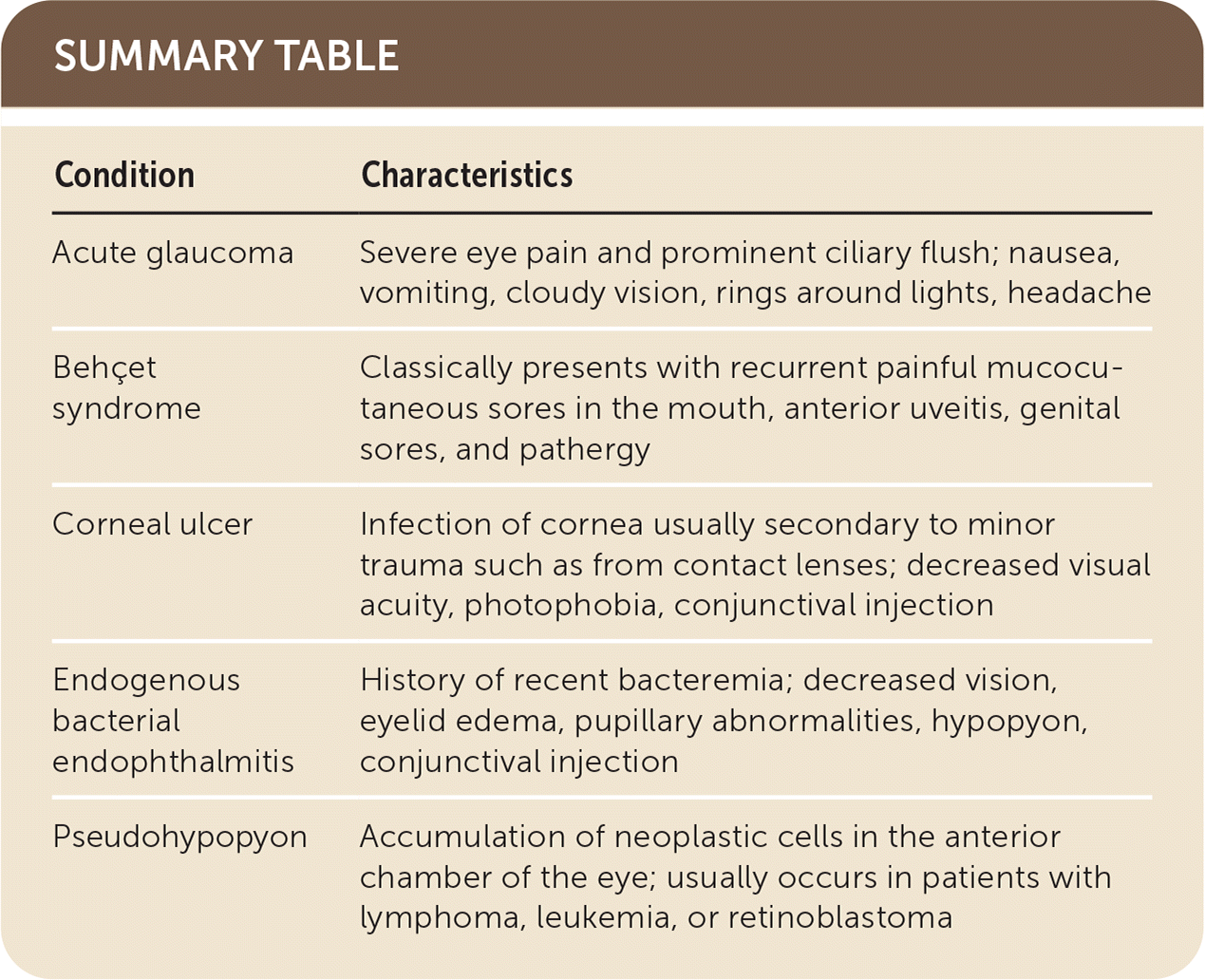
| Condition | Characteristics |
|---|---|
| Acute glaucoma | Severe eye pain and prominent ciliary flush; nausea, vomiting, cloudy vision, rings around lights, headache |
| Behçet syndrome | Classically presents with recurrent painful mucocutaneous sores in the mouth, anterior uveitis, genital sores, and pathergy |
| Corneal ulcer | Infection of cornea usually secondary to minor trauma such as from contact lenses; decreased visual acuity, photophobia, conjunctival injection |
| Endogenous bacterial endophthalmitis | History of recent bacteremia; decreased vision, eyelid edema, pupillary abnormalities, hypopyon, conjunctival injection |
| Pseudohypopyon | Accumulation of neoplastic cells in the anterior chamber of the eye; usually occurs in patients with lymphoma, leukemia, or retinoblastoma |
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Air Force Medical Department or the U.S. Air Force at large.

