A five-month-old girl presented with a rash that had been worsening over the previous week. The rash appeared six weeks earlier on her face and then spread to the diaper area, extremities, and chest. The rash persisted despite treatment with herbs, talcum, and what the mother described as “antibiotic ointment.” The rash did not seem pruritic, although the patient had been irritable. There were no other known symptoms, including fever, eye changes, cough, difficulty breathing, vomiting, diarrhea, change in appetite, or hair or nail changes.
The infant was born by vaginal delivery at home and had no medical care prior to this presentation. She was unimmunized and had no known food or drug allergies. There were no sick contacts at home, and her parents were not aware of any familial skin conditions such as eczema. The infant was initially breastfed exclusively; however, she stopped breastfeeding entirely two weeks before presentation. Her mother was unsure of the composition of the formula she was using. An older sibling had used the same formula without difficulty. According to the mother, the baby was growing and developing appropriately.
On examination, the child was nontoxic and appropriately interactive for age. She was afebrile with normal vital signs. Her weight was in the 10th percentile. Extensive skin lesions were noted on the face, perineum, and extremities (Figure 1 and Figure 2). The physical examination showed no other significant findings.
FIGURE 1
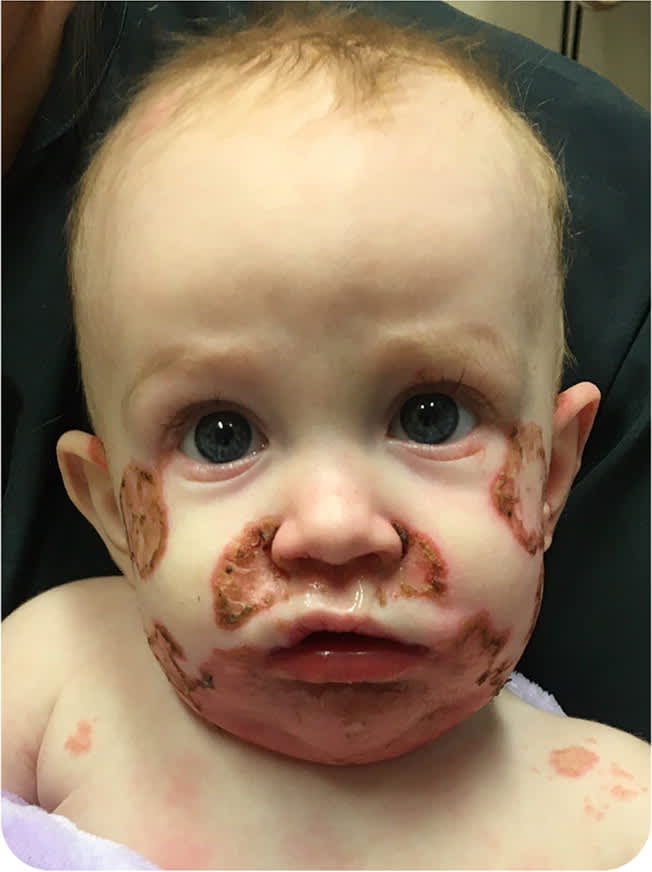
FIGURE 2
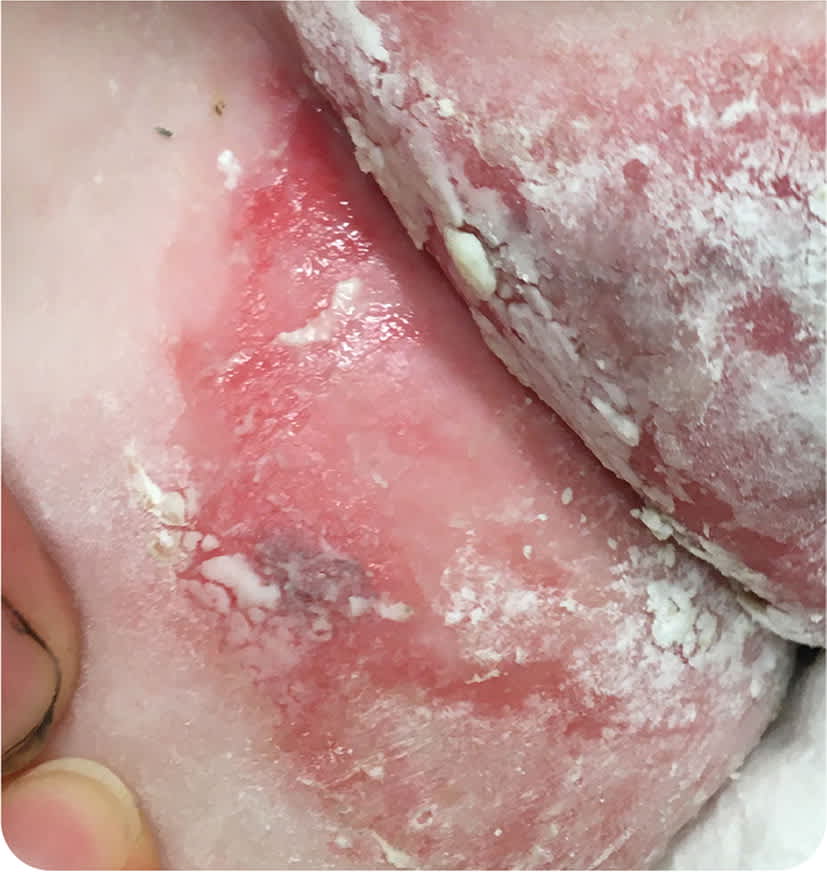
Question
Based on the patient’s history and physical examination findings, which one of the following is the most likely diagnosis?
- A. Candidal dermatitis.
- B. Impetigo.
- C. Plaque psoriasis.
- D. Seborrheic dermatitis.
- E. Zinc deficiency.
Discussion
The correct answer is E: zinc deficiency. Zinc deficiency classically presents with a perioral facial rash in a U-shaped pattern, with cheeks to chin involvement and sparing of the upper lip. There is sharp demarcation between the affected area and normal skin. A symmetrical rash with excoriation can also be prominent in the perineal, gluteal, and perianal areas. The condition is often associated with alopecia, diarrhea, and nails that tend to be soft with bridging, dystrophy, and paronychia. Other symptoms may include conjunctivitis and sensitivity to light, loss of appetite, irritability, and impeded growth.1
Zinc plays an important role in a variety of cellular processes, including protein synthesis, wound healing, and immune function.2 Dietary sources include human breast milk, meat, shellfish, chickpeas, cashews, and pumpkin seeds. Absorption of zinc occurs in the jejunum of the small intestine.3 Zinc deficiency can be nutritional or a result of an inherited zinc transporter defect. Acquired zinc deficiency is typically caused by inadequate intake, increased demand, malabsorption, or excessive losses. Acrodermatitis enteropathica is an autosomal recessive disorder caused by a mutation that reduces the uptake and transport of zinc, particularly across the small intestinal mucosa. Human milk usually contains enough zinc to maintain adequate levels despite transporter defects; thus, the condition tends to present when weaning from breast milk.4
The treatment for zinc deficiency is supplementation with elemental zinc (0.5 to 1 mg per kg per day) until the symptoms resolve.5 Treatment for acrodermatitis enteropathica is lifelong supplementation with elemental zinc (3 mg per kg per day); a higher dosage is needed to overcome the zinc transporter defect.1 The only known adverse effect of zinc supplementation is copper deficiency. High zinc levels inhibit copper absorption by competitively inhibiting a common cationic transporter; therefore, copper levels should be monitored during treatment of zinc deficiency.
Candidal dermatitis is typically located in areas of moisture (e.g., neck folds, inguinal folds, diaper area, axillae) and classically presents with beefy red plaques, superficial pustules, and satellite papules that leave a collarette of scale after rupturing. Although this patient presented with several clinical signs of candidal superinfection, the rash was not limited to areas of moisture.
Impetigo presents with bullae, honey-colored crusts, erythema, edema, and exudate on the face or extremities. It most commonly occurs in children two to five years of age.
Plaque psoriasis is characterized by round, brightly erythematous plaques covered with silvery-white scale on extensor surfaces and the scalp.
Seborrheic dermatitis presents with yellowish, greasy scales on the scalp, eyebrows, umbilicus, and diaper area in infants.
SUMMARY TABLE
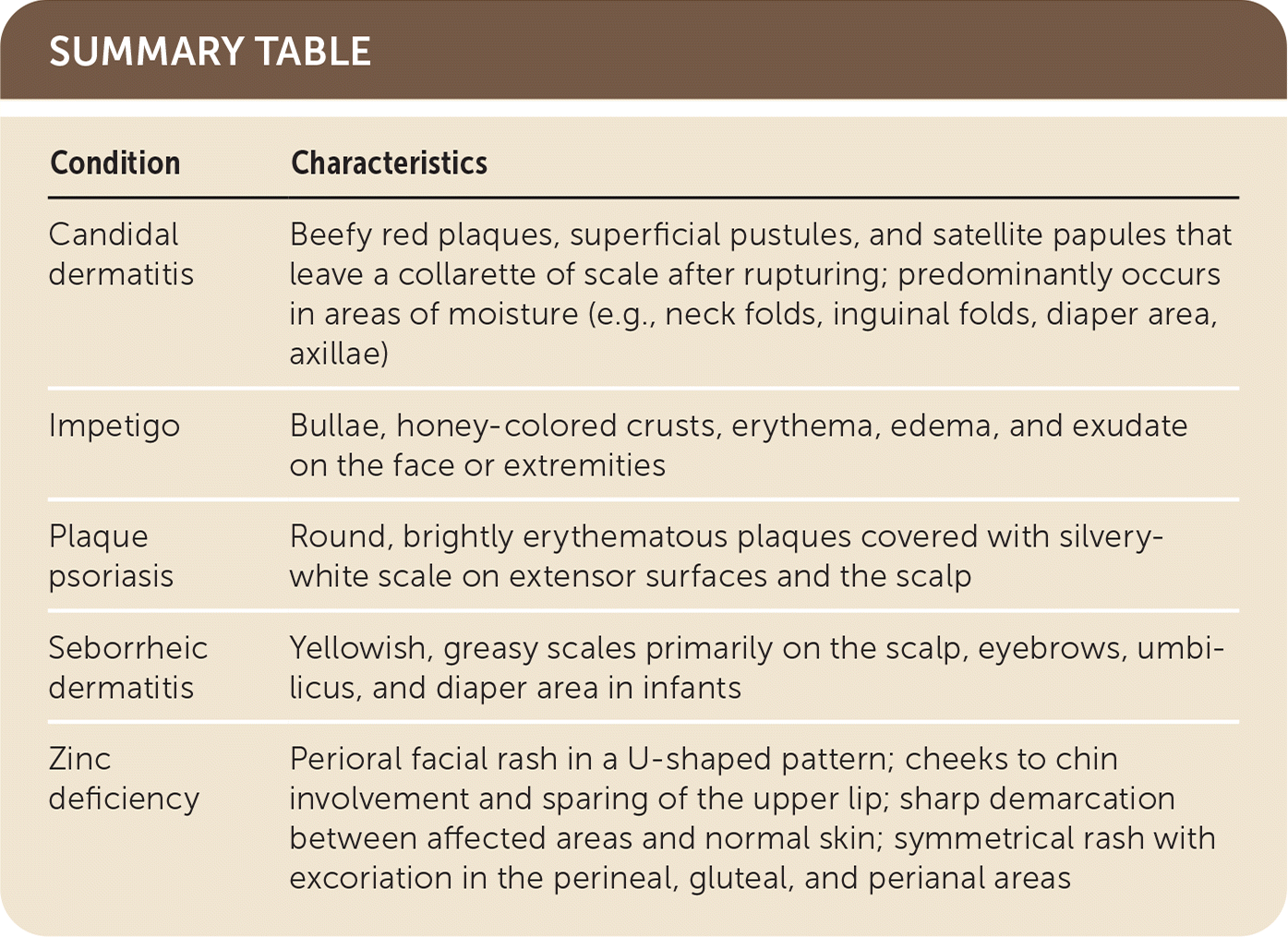
| Condition | Characteristics |
|---|---|
| Candidal dermatitis | Beefy red plaques, superficial pustules, and satellite papules that leave a collarette of scale after rupturing; predominantly occurs in areas of moisture (e.g., neck folds, inguinal folds, diaper area, axillae) |
| Impetigo | Bullae, honey-colored crusts, erythema, edema, and exudate on the face or extremities |
| Plaque psoriasis | Round, brightly erythematous plaques covered with silvery-white scale on extensor surfaces and the scalp |
| Seborrheic dermatitis | Yellowish, greasy scales primarily on the scalp, eyebrows, umbilicus, and diaper area in infants |
| Zinc deficiency | Perioral facial rash in a U-shaped pattern; cheeks to chin involvement and sparing of the upper lip; sharp demarcation between affected areas and normal skin; symmetrical rash with excoriation in the perineal, gluteal, and perianal areas |

