MyProstateScore (MPS; also referred to as Michigan Prostate Score) combines serum prostate-specific antigen (PSA) levels with the urinary biomarkers prostate cancer antigen 3 (PCA3) and TMPRSS2: ERG gene fusion to estimate the risk of prostate cancer. MPS is marketed as a tool for determining the likelihood of detecting clinically significant prostate cancer on biopsy.1–3 It may help patients and physicians decide whether to proceed with a prostate biopsy.
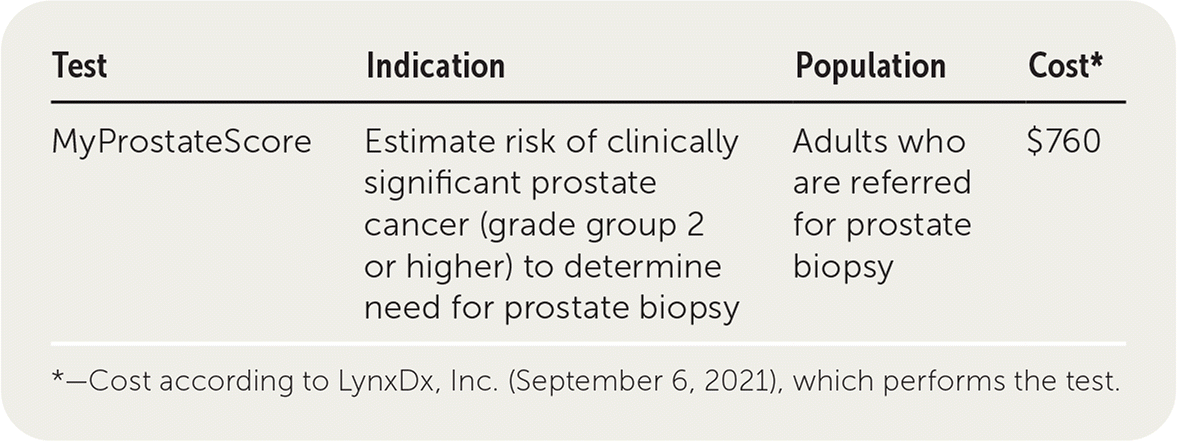
| Test | Indication | Population | Cost* |
|---|---|---|---|
| MyProstateScore | Estimate risk of clinically significant prostate cancer (grade group 2 or higher) to determine need for prostate biopsy | Adults who are referred for prostate biopsy | $760 |
*—Cost according to LynxDx, Inc. (September 6, 2021), which performs the test.
Accuracy
The biomarkers PCA3 and TMPRSS2: ERG have each been studied independently to determine their clinical utility. In a 2020 systematic review and meta-analysis of 54 studies (N = 17,575) that included 4,043 patients with a prostate cancer diagnosis, a PCA3 score of 35 was 71% sensitive (95% CI, 67% to 74%) and 68% specific (95% CI, 63% to 74%) for diagnosing prostate cancer, with a positive likelihood ratio of 2.25 (95% CI, 1.93 to 2.61) and negative likelihood ratio of 0.43 (95% CI, 0.38 to 0.47).4 Although the review was limited by marked heterogeneity of sample sizes and analysis methods, the authors concluded that PCA3 has moderate diagnostic accuracy.4
In a 2018 meta-analysis (N = 1,057), the presence of urinary TMPRSS2: ERG was associated with a histologic diagnosis of prostate cancer (odds ratio = 2.79; 95% CI, 1.12 to 6.98; eight studies); however, there was marked heterogeneity that the authors could not adequately explain.5 In addition, validity was limited because the included studies were a mix of randomized controlled trials and cohort, case-control, and cross-sectional studies of patients undergoing prostate biopsy or resection, for which the indications were not clearly described.5
In a prospective cohort of 1,225 individuals presenting for a prostate biopsy, the area under the curve (AUC) was used to compare PSA with MPS. The AUC for MPS was greater than for PSA alone in the detection of prostate cancer (0.751 vs. 0.585, P < .001).2 An AUC of 0.5 is considered to be of limited diagnostic utility. An AUC of 0.7 to 0.8 is generally considered good diagnostic accuracy, 0.8 to 0.9 is excellent, and greater than 0.9 is outstanding.6
MPS may be useful for identifying high-grade prostate cancer (i.e., grade group 2 or higher 7,8) in those presenting for prostate biopsy.1,3 In a large validation study that combined two external cohorts of 1,525 total patients referred for their first prostate biopsy (338 of the patients [22%] had confirmed grade group 2 or higher cancer), an MPS threshold score of 10 was 97% sensitive for detecting high-grade cancer, with a negative predictive value of 97.5%.1 Using an MPS threshold score of less than 10 would have avoided 387 unnecessary biopsies for the 1,187 patients (32.6%) whose biopsies were normal or grade group 1 and would have missed only 10 high-grade cancers (3%).1 Limitations of the study include the use of prostate biopsy as a reference standard because it is known to miss clinically significant cancers and detect those that are clinically insignificant. Furthermore, the study did not incorporate other diagnostic testing capabilities such as magnetic resonance imaging, which is increasingly used in the diagnosis of prostate cancer.1
Benefit
MPS may reduce biopsies in the evaluation of suspected prostate cancer.1,2 The initial derivation study applied mathematical models that suggest the use of MPS would avoid 35% to 47% of biopsies.2 This finding is similar to that of a prospective cohort study, which found that 33% of prostate biopsies could have been avoided in patients with an MPS of less than 10.1 It should be noted that these predictive models have not been studied outside of patients presenting for prostate biopsy.1,2
Harms
The MPS test includes a blood draw for PSA, and a urine sample for PCA3 and TMPRSS2: ERG should be collected within one hour after a digital rectal examination that includes a prostate massage.3,9 In the two prospective cohort studies from which the clinical decision tool was derived, the missed diagnosis rate was 1% to 3.7% for grade group 2 or higher cancers.1,2
The harms of PSA-based prostate cancer screening have been established. Although current screening standards may offer some mortality benefit (preventing 1.3 deaths from prostate cancer over 13 years per 1,000 individuals screened), harms of screening include overdiagnosis, false-positives, and the harms associated with biopsy or treatment.10,11
The U.S. Preventive Services Task Force recommends an individualized approach to PSA-based prostate cancer screening for men 55 to 69 years of age that incorporates a discussion of potential harms and benefits and recommends against PSA-based screening for men 70 years and older.10 There is insufficient evidence for the U.S. Preventive Services Task Force to provide recommendations for expanded screening tools such as MPS.10 The American Urological Association states that additional modalities such as MPS or imaging can be considered for determining the need for prostate biopsy in individuals with elevated PSA levels, although evidence of benefit is lacking.12
Cost
MPS costs $760, according to a representative from LynxDx, Inc. (September 6, 2021), which performs the test. MPS is not covered by Medicare or Medicaid but may be covered by commercial insurance.13 A draft proposal currently under consideration would authorize Medicare and Medicaid coverage for prostate biomarker diagnostic tests before biopsy for individuals meeting strict medical necessity criteria if ordered by physicians who specialize in the management of prostate cancer, such as urologists and oncologists.14
Bottom Line
MPS is a promising tool for the detection of clinically significant prostate cancer and has been validated for determining the necessity of a prostate biopsy in select individuals.1,2 It has not been studied as a prostate cancer screening tool. Given the potential harms of standard prostate cancer screening methods, further study is needed to determine the effects of MPS on prostate cancer–related morbidity and mortality before it can be recommended in the primary care setting.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Air Force, Department of Defense, or U.S. government.

