Generalized anxiety disorder (GAD) and panic disorder (PD) are common mental health conditions in adults that are often seen in primary care. Although there is insufficient evidence to support universal screening for PD and GAD, evaluation should be considered in patients who express recurrent, pervasive worry or present with somatic symptoms not attributed to underlying medical conditions. The GAD-7 and Patient Health Questionnaire for PD are validated screening tools that can aid in diagnosis and assessment. Anxiety disorders often present with substance use disorders, which should be treated concurrently. Effective therapies for PD and GAD include cognitive behavior therapy and anti-depressants, including selective serotonin reuptake inhibitors and serotonin-norepinephrine reuptake inhibitors. Benzodiazepines are not recommended for first-line therapy or long-term use because of adverse reactions, risk of dependence, and higher mortality. No consistent evidence currently supports a specific prevention strategy for PD or GAD, but exercise may be beneficial.
Anxiety disorders are some of the most common mental health conditions seen in primary care, with generalized anxiety disorder (GAD) and panic disorder (PD) being the most common anxiety disorders in adults.1 Patients with anxiety disorders are more likely than those unaffected to also have other chronic medical problems and are twice as likely to present with somatic symptoms.2 Integrating mental health services with primary care decreases treatment costs and increases access to care.3 This article summarizes the diagnosis and management of GAD and PD in the general adult population.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
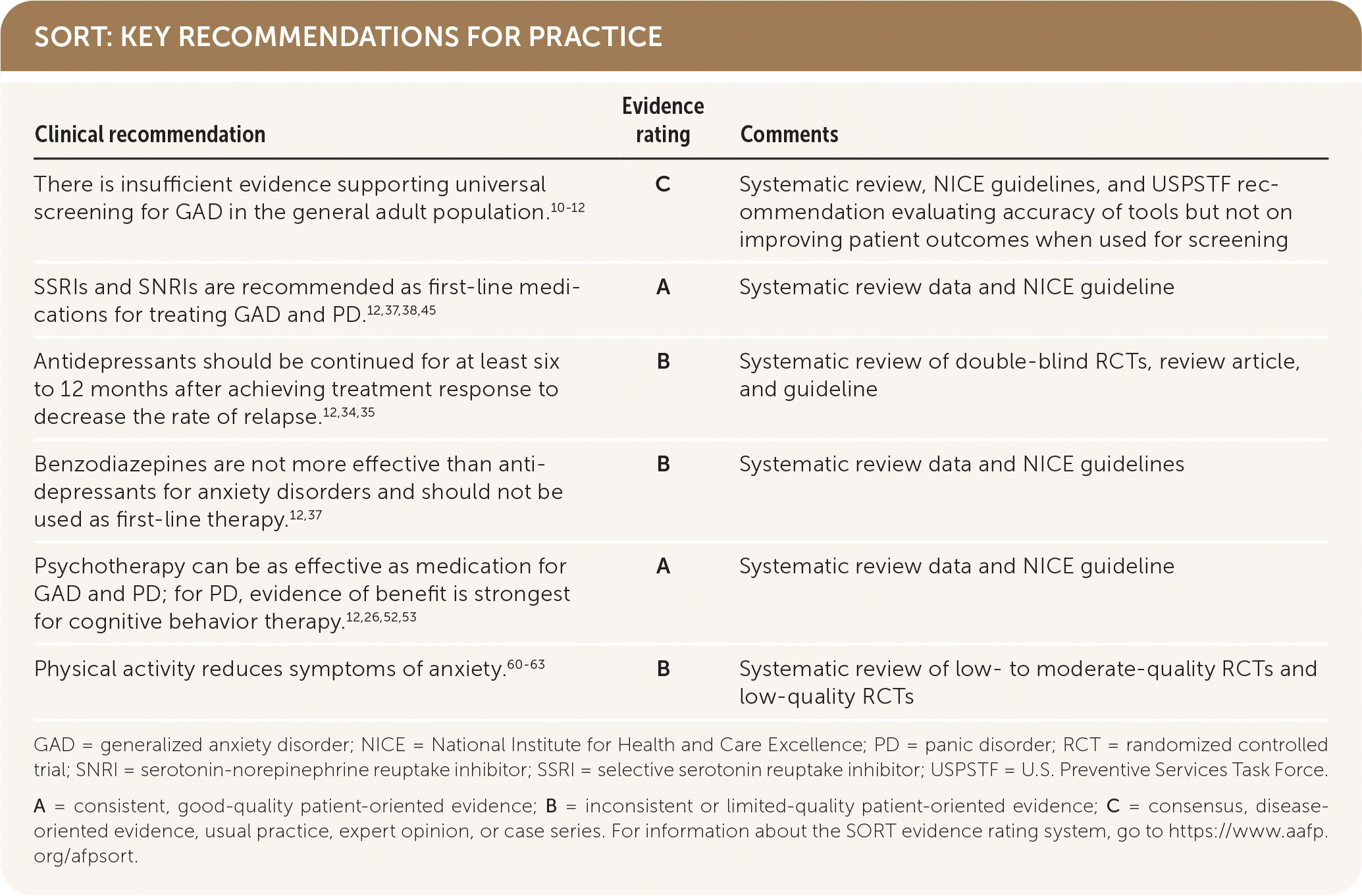
GAD = generalized anxiety disorder; NICE = National Institute for Health and Care Excellence; PD = panic disorder; RCT = randomized controlled trial; SNRI = serotonin-norepinephrine reuptake inhibitor; SSRI = selective serotonin reuptake inhibitor; USPSTF = U.S. Preventive Services Task Force.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Typical Presentation and Diagnostic Criteria
GENERALIZED ANXIETY DISORDER
GAD is defined by the Diagnostic and Statistical Manual of Mental Disorders, 5th ed. (DSM-5) as excessive worry that occurs on most days for at least six months and causes significant distress or impairment (Table 1).4 Clinically, GAD most commonly presents as excessive worry about minor issues, often manifesting with somatic symptoms and pathologic behavioral changes.5 Most studies suggest a peak onset of GAD during late adolescence or early adulthood, but it can also present later in life.6
TABLE 1. Generalized Anxiety Disorder Diagnostic Criteria 300.02 (F41.1)

|
Reprinted with permission from the Diagnostic and Statistical Manual of Mental Disorders. 5th ed. American Psychiatric Association; 2014:222.
PANIC DISORDER
PD is defined by the DSM-5 as recurrent panic attacks that include characteristic symptoms and lack an obvious trigger (Table 2).4 PD includes at least one month of persistent concern for panic attack recurrence and may include mal-adaptive behavioral changes. Although other symptoms such as headache, tinnitus, and uncontrollable crying are common, they do not help define panic attacks. The most common symptom of a panic attack is heart palpitations.7 Panic attacks that are nocturnal or lack fear require a more extensive workup; however, these features are not uncommon in PD.4
TABLE 2. Panic Disorder Diagnostic Criteria 300.01 (F41.0)

|
Reprinted with permission from the Diagnostic and Statistical Manual of Mental Disorders. 5th ed. American Psychiatric Association; 2014:208–209.
Diagnosis, Comorbidity, and Screening
The symptoms of GAD and PD can suggest medical diagnoses, including hyperthyroidism, arrhythmias, asthma, chronic obstructive pulmonary disease, certain medication use or withdrawal (e.g., albuterol, levothyroxine, decongestants, antidepressants, antianxiety medications), and substance use or withdrawal (e.g., caffeine, alcohol, cocaine, amphetamines, cannabinoids).4
GAD and PD commonly occur with other psychiatric conditions, including major depressive episodes, manic-hypomanic episodes, dysthymia, and substance use disorder.4,8 GAD and PD are also associated with suicidal ideation and suicide attempts.4,8 Because patients with more severe symptoms more often seek treatment, evaluating for suicidality is important.9
There is insufficient evidence to support universal screening for GAD or PD in adults at this time; however, the U.S. Preventive Services Task Force is updating guidelines regarding screening for anxiety, suicidality, and depression.10,11 Evaluation for GAD should be considered for patients who express anxiety, pervasive worry, or recurrent somatic symptoms not related to an underlying physical condition.12 The GAD-2 and GAD-7 are two-item and seven-item validated screening tools for GAD 11 (Table 313,14 ). The Patient Health Questionnaire for PD is the most accurate screening tool for PD in patients expressing sudden episodes of anxiety or fear 15,16 (Table 417,18 ). The Women's Preventive Services Initiative recommends screening for anxiety disorders in women and adolescent girls older than 13 years; however, the systematic review did not find studies that directly evaluated the overall effectiveness or harms of screening for anxiety in this population.19
TABLE 4. PHQ-PD Screening Tool for Panic Disorder
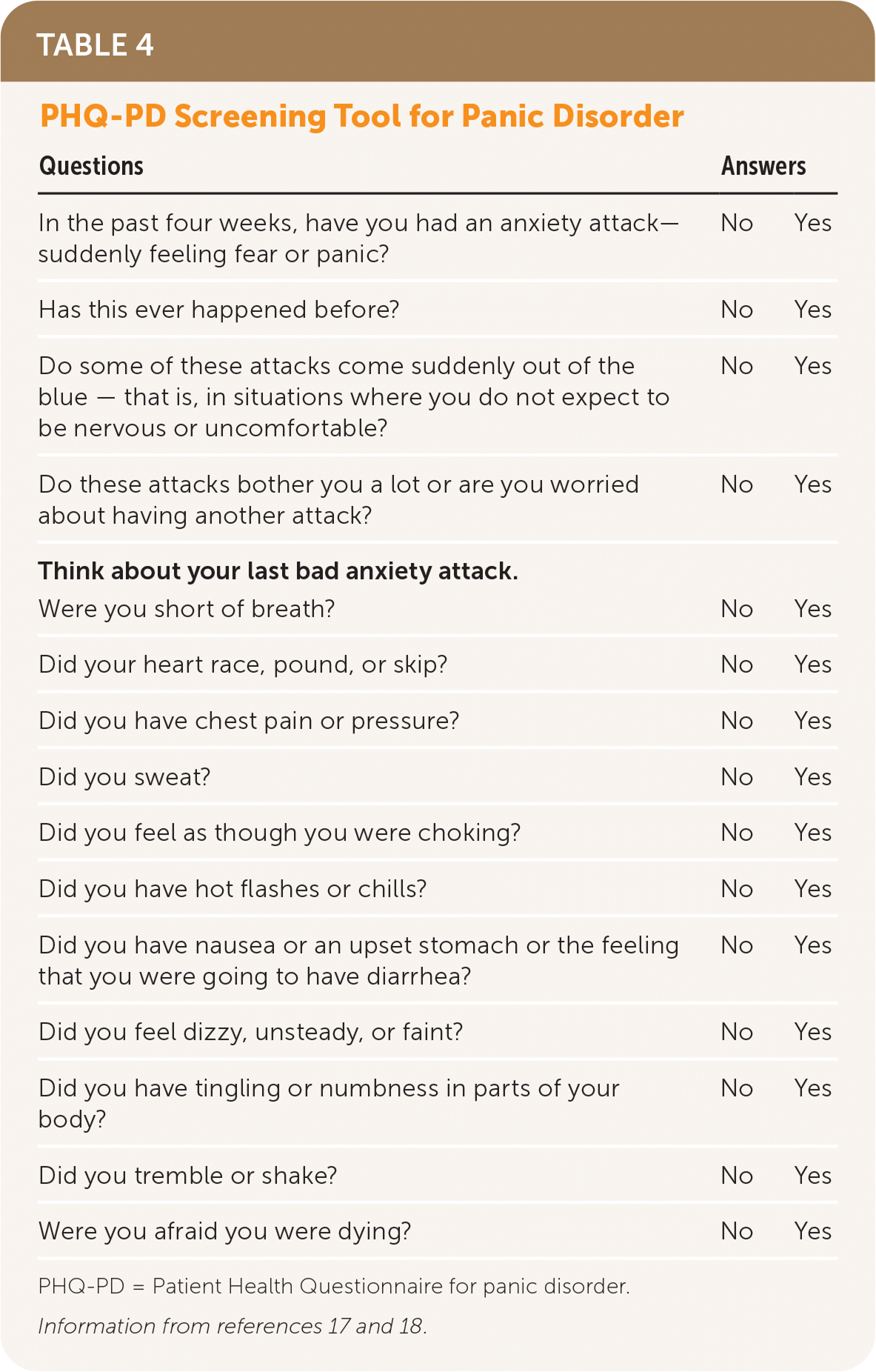
| Questions | Answers | |
|---|---|---|
| In the past four weeks, have you had an anxiety attack—suddenly feeling fear or panic? | No | Yes |
| Has this ever happened before? | No | Yes |
| Do some of these attacks come suddenly out of the blue — that is, in situations where you do not expect to be nervous or uncomfortable? | No | Yes |
| Do these attacks bother you a lot or are you worried about having another attack? | No | Yes |
| Think about your last bad anxiety attack. | ||
| Were you short of breath? | No | Yes |
| Did your heart race, pound, or skip? | No | Yes |
| Did you have chest pain or pressure? | No | Yes |
| Did you sweat? | No | Yes |
| Did you feel as though you were choking? | No | Yes |
| Did you have hot flashes or chills? | No | Yes |
| Did you have nausea or an upset stomach or the feeling that you were going to have diarrhea? | No | Yes |
| Did you feel dizzy, unsteady, or faint? | No | Yes |
| Did you have tingling or numbness in parts of your body? | No | Yes |
| Did you tremble or shake? | No | Yes |
| Were you afraid you were dying? | No | Yes |
PHQ-PD = Patient Health Questionnaire for panic disorder.
Epidemiology, Etiology, and Pathophysiology
In the United States, lifetime prevalence is 8% and 5% for GAD and PD, respectively.20,21 Females are two to three times more likely to experience GAD and PD,22,23 although the gender discrepancy is less apparent later in life.
The etiology of anxiety disorders is multifactorial. Psychological, biological, environmental, and genetic theories can help explain the cause of anxiety disorders. Psychological theories suggest that patients with anxiety perceive higher risk or fear in lower-risk situations. Biologically, people with anxiety disorders are theorized to have overstimulation of specific circuits in the brain that are activated with fearful or noxious stimuli.24 These circuits can be inhibited by increasing serotonin neurotransmission. Environmental theories suggest that patients who have experienced greater adversity are more likely to develop an anxiety disorder. Studies of twin patients have found heritability of approximately 32% for GAD and 48% for PD.25
Treatment
The two main categories of treatment for GAD and PD are pharmacotherapy and psychotherapy, with cognitive behavior therapy (CBT) being the most effective and well-studied form of psychotherapy for PD.26 First-line medications are selective serotonin reuptake inhibitors (SSRIs) and serotonin-norepinephrine reuptake inhibitors (SNRIs). Concomitant substance use disorders, including tobacco use, should be treated at the same time to improve anxiety symptoms and treatment success.12,27 Smoking cessation decreases short- and long-term symptoms of anxiety.28,29 The Panic Disorder Severity Scale is a tool that can be used to monitor symptoms of PD and response to treatment.30–32
PHARMACOTHERAPY
Antidepressants, SSRIs and SNRIs in particular, are considered first-line therapies for GAD and PD because they are effective and generally well tolerated.12 Continuing to take antidepressants for at least six to 12 months is recommended to minimize relapse.12,33–35 Although approximately 16% of patients relapse despite continued use of antidepressants, discontinuing antidepressants before one year leads to symptom relapse in up to 50% of patients being treated with an SSRI or SNRI.35,36 Benzodiazepines are not more effective than antidepressants for treating anxiety disorders and should not be used as first-line therapy.13,37
Generalized Anxiety Disorder. SSRIs and SNRIs are the mainstay of pharmacotherapy for GAD.12 A recent meta-analysis found that escitalopram (Lexapro), duloxetine (Cymbalta), venlafaxine, and pregabalin (Lyrica) appear to be most effective and well tolerated.38 Antidepressants should be tried before pregabalin,12 which appears effective but may cause weight gain and sedation.39 Limited evidence suggests that antipsychotics have poor effectiveness and cause several adverse effects.12,40 Benzodiazepines have the benefit of quick onset and are effective in treating symptoms of anxiety; however, they are associated with withdrawal, rebound anxiety, and dependence and are not recommended for long-term use.5,12,34,41
Adding additional medications to antidepressants does not appear to improve outcomes. Benzodiazepines are those most often prescribed, but initiating a benzodiazepine with SSRIs in adolescents and young adults does not shorten the duration of SSRI treatment.42 There is no evidence of overall benefit to augmentation of antidepressant therapy with benzodiazepines, atypical antipsychotics, or buspirone (Buspar) in treatment-resistant anxiety disorders.43 Limited evidence suggests hydroxyzine may be as effective as benzodiazepines.44
Panic Disorder. Antidepressants are effective for treating PD, with an estimated number needed to treat of 10 for remission after two to six months of treatment.45 SSRIs and SNRIs are preferred over tricyclic antidepressants or monotherapy with benzodiazepines because of a higher risk of adverse effects with tricyclic antidepressants and benzodiazepines, although all have comparable effectiveness.41,46 Benzodiazepines improve symptoms in PD compared with placebo but not compared with antidepressants.37,47 Treatment with benzodiazepines increases the risk of tolerance, withdrawal, and mortality.48 Escitalopram, sertraline (Zoloft), citalopram (Celexa), paroxetine (Paxil), and venlafaxine are effective for the treatment of PD.12 Despite limited data with no evidence of benefit, beta blockers are often used to treat the acute symptoms of panic attack in PD.49 The effectiveness of buspirone in treating PD remains uncertain.50 Antipsychotics or sedating antihistamines are not recommended for PD because of overall limited evidence of effectiveness and adverse effects that lessen tolerability.12,40,41
PSYCHOTHERAPY AND RELAXATION TECHNIQUES
Psychotherapy for GAD and PD can include relaxation techniques; cognitive restructuring, including CBT; and exposure therapy.51 Psychotherapy is as effective as pharmacotherapy for treating PD and GAD and can be used alone or combined with pharmacotherapy for anxiety disorders, with combination treatment likely to be more effective than either treatment alone.12,52,53 Of the psychotherapy techniques that have been studied for GAD and PD, CBT appears to be the most effective.26,53,54 Limited evidence suggests that therapist-supported internet CBT, which can expand access to therapy, is effective, but comparisons with alternative therapies are limited.55 CBT can be as effective for PD as pharmacotherapy, but evidence is limited and lacks data on adverse effects.52,56
Interoceptive exposure, a technique in which patients induce the somatic symptoms of a panic attack to decouple their association with fear, is the most beneficial component of CBT for treating PD, whereas muscle relaxation and virtual reality exposure may be less effective.51 CBT has positive short- and long-term outcomes for most anxiety disorders, although it may not have as much long-term benefit for PD.56
COMPLEMENTARY AND ALTERNATIVE THERAPIES
A variety of complementary and alternative therapies are available for management of GAD and PD, although most have limited evidence.57–59 Exercise reduces symptoms of anxiety; however, randomized controlled trial data are lacking regarding how much or what type of exercise is most beneficial.60–63 Yoga and mindfulness meditation can improve anxiety symptoms, but high-quality trials comparing alternative therapies to first-line therapies are lacking.64,65 Supplements that may be beneficial in treating anxiety are listed in Table 5.58,66–76 The American Psychiatric Association highlights the absence of scientific evidence supporting cannabis in the treatment of psychiatric disorders and its strong association with the onset of psychiatric disorders and calls for more research in a 2019 position statement against the use of medicinal cannabis.77 There is inconclusive evidence for the use of marijuana in treating GAD and PD, and its use has been associated with increased anxiety, withdrawal syndromes, and cannabinoid hyperemesis syndrome (cyclic vomiting syndrome associated with cannabis use).78,79 Cannabidiol may be effective for GAD and appears to be well tolerated; however, studies are limited, and the dosing in randomized controlled trials is highly variable.80
TABLE 5. Botanicals and Supplements Commonly Used for Anxiety Disorders
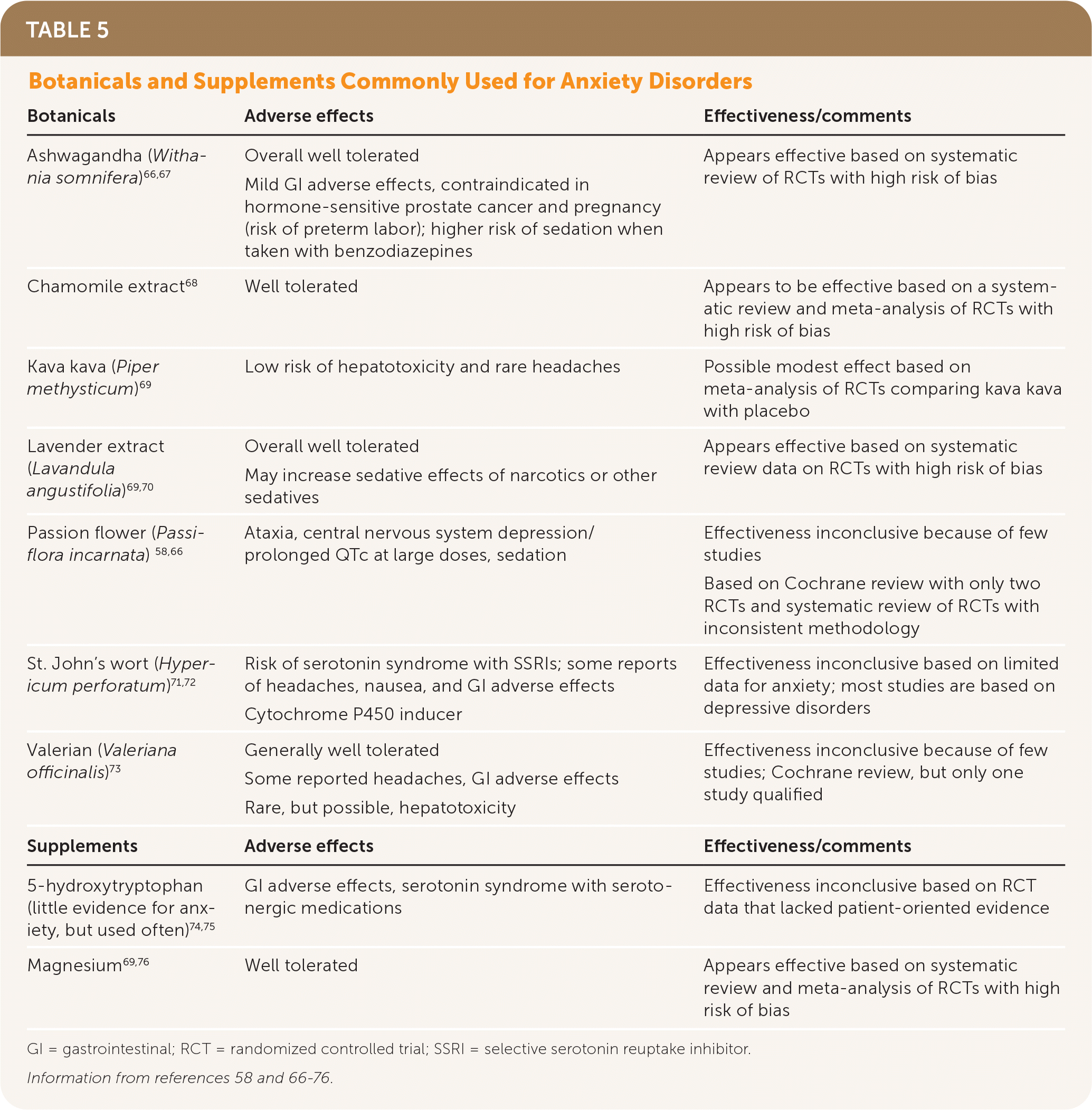
| Botanicals | Adverse effects | Effectiveness/comments |
|---|---|---|
| Ashwagandha (Withania somnifera)66,67 | Overall well tolerated Mild GI adverse effects, contraindicated in hormone-sensitive prostate cancer and pregnancy (risk of preterm labor); higher risk of sedation when taken with benzodiazepines | Appears effective based on systematic review of RCTs with high risk of bias |
| Chamomile extract68 | Well tolerated | Appears to be effective based on a systematic review and meta-analysis of RCTs with high risk of bias |
| Kava kava (Piper methysticum)69 | Low risk of hepatotoxicity and rare headaches | Possible modest effect based on meta-analysis of RCTs comparing kava kava with placebo |
| Lavender extract (Lavandula angustifolia)69,70 | Overall well tolerated May increase sedative effects of narcotics or other sedatives | Appears effective based on systematic review data on RCTs with high risk of bias |
| Passion flower (Passiflora incarnata) 58,66 | Ataxia, central nervous system depression/prolonged QTc at large doses, sedation | Effectiveness inconclusive because of few studies Based on Cochrane review with only two RCTs and systematic review of RCTs with inconsistent methodology |
| St. John's wort (Hypericum perforatum)71,72 | Risk of serotonin syndrome with SSRIs; some reports of headaches, nausea, and GI adverse effects Cytochrome P450 inducer | Effectiveness inconclusive based on limited data for anxiety; most studies are based on depressive disorders |
| Valerian (Valeriana officinalis)73 | Generally well tolerated Some reported headaches, GI adverse effects Rare, but possible, hepatotoxicity | Effectiveness inconclusive because of few studies; Cochrane review, but only one study qualified |
| Supplements | Adverse effects | Effectiveness/comments |
| 5-hydroxytryptophan (little evidence for anxiety, but used often)74,75 | GI adverse effects, serotonin syndrome with serotonergic medications | Effectiveness inconclusive based on RCT data that lacked patient-oriented evidence |
| Magnesium69,76 | Well tolerated | Appears effective based on systematic review and meta-analysis of RCTs with high risk of bias |
GI = gastrointestinal; RCT = randomized controlled trial; SSRI = selective serotonin reuptake inhibitor.
Prevention of Anxiety Disorders
Anxiety prevention programs, including exercise programs, have shown limited benefits in the prevention of anxiety.81,82 Educational programs that teach coping techniques and methods of cognitive restructuring have shown some success in preventing anxiety disorders.83
Referral
Referral to a psychiatrist may be considered for patients with complex mental or physical health comorbidities, safety concerns, or poor response to multiple treatments.12 Patients with concomitant substance use disorder may benefit from referral to specialized dual-treatment programs.27
This article updates a previous article on this topic by Locke, et al.14
Data Sources: A search of PubMed, Ovid, Medline, Essential Evidence Plus, and DynaMed was completed using the key words anxiety disorders, generalized anxiety, generalized anxiety disorder, mixed anxiety-depressive disorder, panic disorder, and panic-associated dizziness. This search included InfoPOEMs, Cochrane reviews, and practice guidelines. Search dates: July 3, 2020, to September 9, 2021.

