Many communities in the United States have few or no clinicians providing maternity care services, contributing to a national maternal and infant mortality rate that is much higher than that in comparable developed countries.1 The March of Dimes defines maternity care deserts (MCDs) as counties that have no hospitals providing obstetric care and no practicing obstetrician-gynecologists (OB-GYNs) or certified nurse midwives (CNMs).2 However, this definition excludes the thousands of family physicians who provide maternity care, particularly in rural areas.3,4 We sought to determine the extent to which family physicians provide obstetric care within MCDs throughout the United States.
Using 2011 to 2019 data from the Family Medicine Certification Examination Application Practice Demographic Questionnaire provided by the American Board of Family Medicine, the office addresses of family physicians who reported performing deliveries were geocoded and mapped at the county level.5 These data represent roughly 90% of family physicians over nine years by capturing the 10% of family physicians continuing certification each year. County-level data from the Health Resources and Services Administration Area Health Resource File, 2020–2021, were then used to map OB-GYNs and CNMs.6 Finally, geographic information systems were used to create county-level maps displaying the distribution of family physicians delivering babies in relation to MCDs.
Figure 1 displays the location of all obstetric care clinicians relative to MCDs. More than one-third (35.8%) of counties in the United States have been identified as an MCD, with more than eight in 10 (81.3%) of these counties located in nonmetropolitan areas. Family physicians deliver babies in more than four in 10 (40.7%) of all U.S. counties, and more than five in 10 (52.4%) of these counties are located in nonmetropolitan areas. Family physicians are the sole maternity care clinicians delivering babies in 181 MCDs (about one in six [16.2%] of all MCDs), serving more than 400,000 women (18 to 44 years of age). Decreasing numbers of family physicians delivering babies, combined with the movement of these physicians away from nonmetropolitan areas, may cause fluctuations in the true count of family physicians delivering babies in MCDs at a given time.7–10
FIGURE 1.
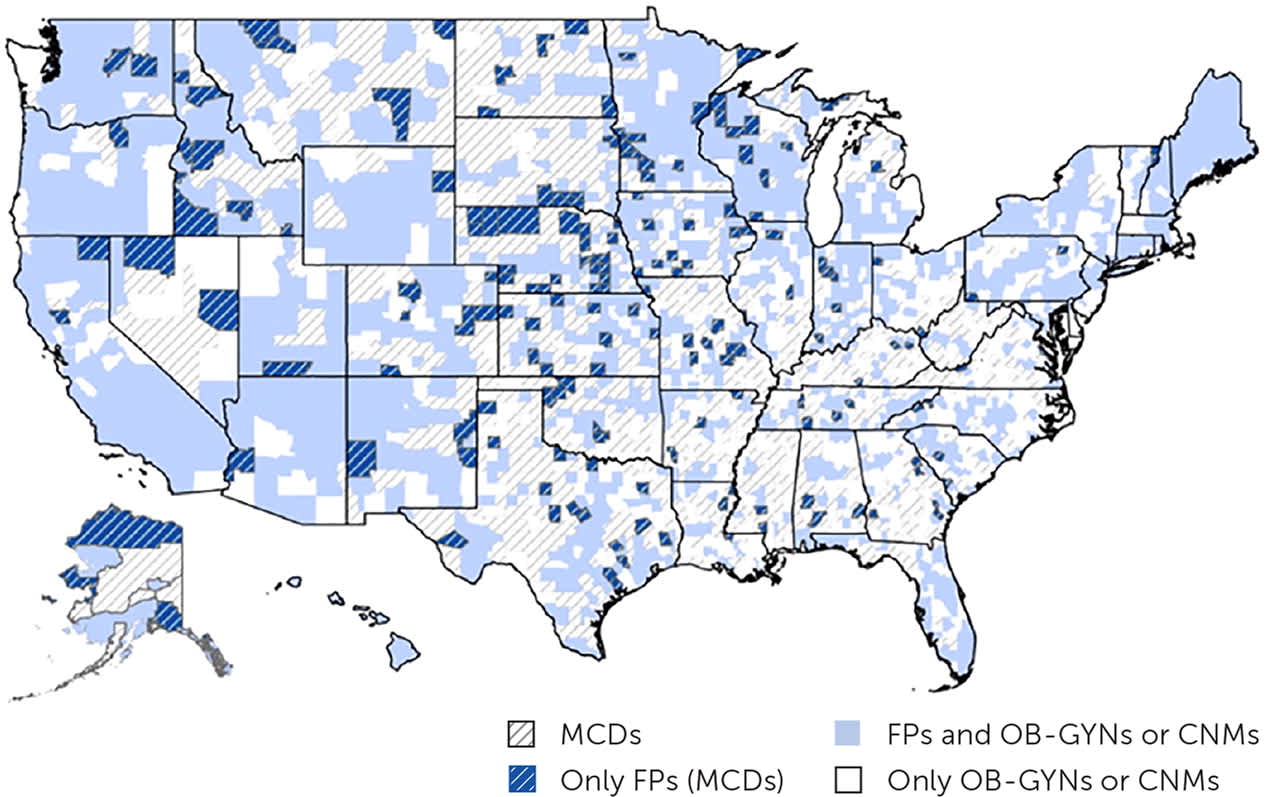
Map of MCDs and of obstetric care clinicians by specialty in the United States.
CNMs = certified nurse midwives; FPs = family physicians; MCDs = maternity care deserts; OB-GYNs = obstetrician-gynecologists.
Sources: American Board of Family Medicine, 2011–2019; Area Health Resource File, 2021
The data demonstrate the significant role family physicians play in MCDs and nationwide. Despite their important contribution, family physicians are excluded from the Health Resources and Services Administration's definition of maternity care health professional target areas (MCTAs), which help to distribute maternity care clinicians to shortage areas.11 MCTAs receive a score partially based on the ratio of OB-GYNs and CNMs to women 15 to 44 years of age; however, the score does not include family physicians also providing care in that area.11 Overlooking family physicians providing care in MCTAs may result in the faulty allocation of maternity care clinicians away from the highest need areas.12 To ensure equitable distribution of clinicians who perform obstetrics, the contribution of family physicians to maternity care must be recognized and supported. Residency programs should continue to offer robust training opportunities and advanced fellowship opportunities.13–16 The discipline, credentialing bodies, and health systems must also support family physicians who perform deliveries, particularly in nonmetropolitan areas, by simplifying credentialing, building interdisciplinary relationships, and ensuring adequate numbers of deliveries to maintain obstetric skills.9,14,17

