Providing perinatal care for diverse populations may involve additional clinical considerations. This editorial highlights the additional risks to and health care recommendations for transgender and adolescent pregnant patients and pregnant patients with opioid use disorder (OUD). These populations are often less likely to seek care and have worse parental and neonatal outcomes than the general population. Table 1 provides a summary of key perinatal care recommendations.
TABLE 1. Key Recommendations for Perinatal Care of Transgender Patients, Adolescent Patients, or Patients With Opioid Use Disorder
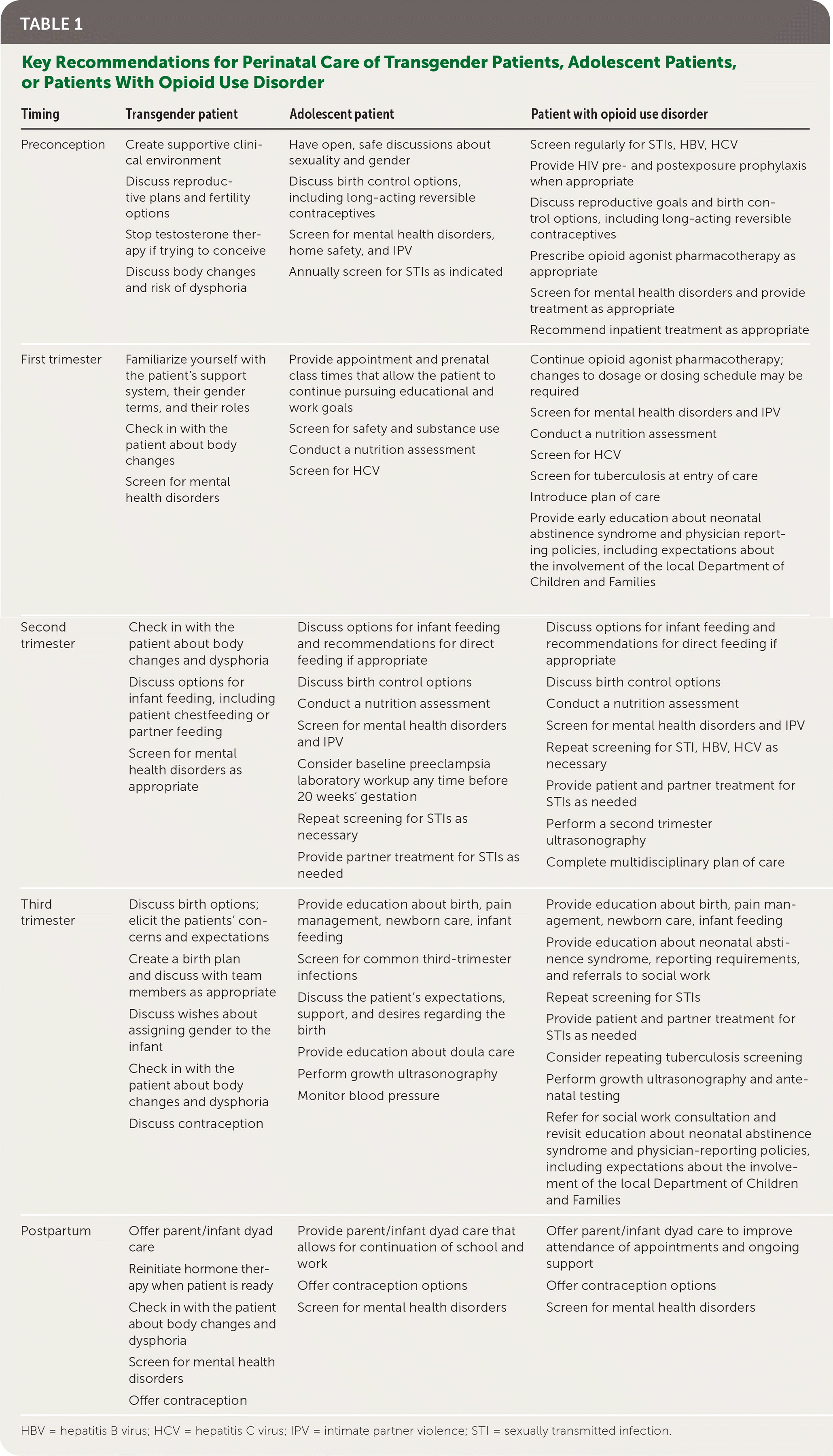
| Timing | Transgender patient | Adolescent patient | Patient with opioid use disorder |
|---|---|---|---|
| Preconception | Create supportive clinical environment Discuss reproductive plans and fertility options Stop testosterone therapy if trying to conceive Discuss body changes and risk of dysphoria | Have open, safe discussions about sexuality and gender Discuss birth control options, including long-acting reversible contraceptives Screen for mental health disorders, home safety, and IPV Annually screen for STIs as indicated | Screen regularly for STIs, HBV, HCV Provide HIV pre- and postexposure prophylaxis when appropriate Discuss reproductive goals and birth control options, including long-acting reversible contraceptives Prescribe opioid agonist pharmacotherapy as appropriate Screen for mental health disorders and provide treatment as appropriate Recommend inpatient treatment as appropriate |
| First trimester | Familiarize yourself with the patient’s support system, their gender terms, and their roles Check in with the patient about body changes Screen for mental health disorders | Provide appointment and prenatal class times that allow the patient to continue pursuing educational and work goals Screen for safety and substance use Conduct a nutrition assessment Screen for HCV | Continue opioid agonist pharmacotherapy; changes to dosage or dosing schedule may be required Screen for mental health disorders and IPV Conduct a nutrition assessment Screen for HCV Screen for tuberculosis at entry of care Introduce plan of care Provide early education about neonatal abstinence syndrome and physician reporting policies, including expectations about the involvement of the local Department of Children and Families |
| Second trimester | Check in with the patient about body changes and dysphoria Discuss options for infant feeding, including patient chestfeeding or partner feeding Screen for mental health disorders as appropriate | Discuss options for infant feeding and recommendations for direct feeding if appropriate Discuss birth control options Conduct a nutrition assessment Screen for mental health disorders and IPV Consider baseline preeclampsia laboratory workup any time before 20 weeks’ gestation Repeat screening for STIs as necessary Provide partner treatment for STIs as needed | Discuss options for infant feeding and recommendations for direct feeding if appropriate Discuss birth control options Conduct a nutrition assessment Screen for mental health disorders and IPV Repeat screening for STI, HBV, HCV as necessary Provide patient and partner treatment for STIs as needed Perform a second trimester ultrasonography Complete multidisciplinary plan of care |
| Third trimester | Discuss birth options; elicit the patients’ concerns and expectations Create a birth plan and discuss with team members as appropriate Discuss wishes about assigning gender to the infant Check in with the patient about body changes and dysphoria Discuss contraception | Provide education about birth, pain management, newborn care, infant feeding Screen for common third-trimester infections Discuss the patient’s expectations, support, and desires regarding the birth Provide education about doula care Perform growth ultrasonography Monitor blood pressure | Provide education about birth, pain management, newborn care, infant feeding Provide education about neonatal abstinence syndrome, reporting requirements, and referrals to social work Repeat screening for STIs Provide patient and partner treatment for STIs as needed Consider repeating tuberculosis screening Perform growth ultrasonography and antenatal testing Refer for social work consultation and revisit education about neonatal abstinence syndrome and physician-reporting policies, including expectations about the involvement of the local Department of Children and Families |
| Postpartum | Offer parent/infant dyad care Reinitiate hormone therapy when patient is ready Check in with the patient about body changes and dysphoria Screen for mental health disorders Offer contraception | Provide parent/infant dyad care that allows for continuation of school and work Offer contraception options Screen for mental health disorders | Offer parent/infant dyad care to improve attendance of appointments and ongoing support Offer contraception options Screen for mental health disorders |
HBV = hepatitis B virus; HCV = hepatitis C virus; IPV = intimate partner violence; STI = sexually transmitted infection.
Perinatal Care of the Transgender Patient
The transgender population includes transgender men, transgender women, and people with other identities such as agender or nonbinary.1,2 Prenatal care should focus on understanding the goals of each patient because the trans-gender community is very diverse. Physical changes and the social constructs of pregnancy and infant feeding may create feelings of dysphoria. Many prenatal care concerns cited by transgender patients and physicians involve broader social issues of being a transgender person who is pregnant and increased contact with medical professionals who do not have cultural competency in transgender care.3,4
The following actions should be prioritized in the perinatal care of transgender individuals:
- Create an affirming environment by providing gender-neutral bathrooms in the office, having nondiscrimination policies visible, and using forms that allow for a variety of identities and the distinction between sex, gender, and sexuality.
- Ensure that the staff receives training related to trans-gender identities, including appropriate pronouns, parenting language, terms used to discuss body parts, and the differences between legal and preferred names.
- Become familiar with the patient’s family and support system, their gender terms, and the roles they will play in the pregnancy, in the postpartum period, and for the child.
- Discuss infant names and patient preferences about assigning gender to the infant.
- Discuss contraceptive options for the postpartum period; testosterone is not a contraceptive.2
- Increase discussion with the patient about the necessity of examination of the genitals and the reproductive system, which can be a highly sensitive topic for trans-gender patients.5
- Recognize the signs of increased gender dysphoria due to body changes during pregnancy and postpartum. ○ Discuss breastfeeding or chestfeeding (a term used to refer to breastfeeding for those who identify as transgender or nonbinary) and the potential for chest tissue to grow, even in those who have had chest masculinization surgery.6
○ Discuss how pregnancy hormones may affect the body, including loss of facial and other body hair, loss of muscle mass, chest changes, and other factors that might increase gender dysphoria.6,7
- Refer patients to specialists, social workers, case managers, and mental health experts with experience and expertise in transgender care to help alleviate gender dysphoria and loneliness.8
Perinatal Care of the Adolescent Patient
Risks associated with pregnancy in adolescent patients include late initiation of prenatal care, hypertensive disorders, anemia, poor maternal weight gain, sexually transmitted infections, substance use, operative deliveries, and intimate partner violence.9 Neonatal and fetal morbidities may include preterm delivery, low birth weight, and childhood behavior disorders.10 As of 2016, up to 17% of teen pregnancies were repeat births.11 Although even one pregnancy during adolescence has a significant effect on the patient’s level of education achieved, financial independence, and prenatal outcomes, a repeat birth significantly increases the risks of infant mortality, low birth weight, lack of educational achievement, and need for government support.11 Although adolescent pregnancy rates have been falling, they may increase again because of the 2022 Supreme Court ruling in the Dobbs vs. Jackson Women’s Health Organization case 12 and are still higher than in any other comparable country.13
The following actions should be prioritized in the perinatal care of adolescents:
- Provide easy access to perinatal care and counseling about pregnancy options (e.g., abortion, adoption, parenting).10
- Provide appointment and prenatal class times that allow patients to continue pursuing education and work goals; drop-in availability and telemedicine can increase engagement with adolescent patients, and dual appointments in the postpartum period for the adolescent parent and infant can streamline care.11
- Screen for alcohol and substance use; pregnancy and early parenting are powerful motivators for seeking sobriety.
- Refer patients to social workers, case managers, and nutritionists as appropriate.
- Conduct a nutrition assessment, screen for anemia, and prescribe prenatal vitamins and iron supplementation.
- Provide sexually transmitted infection screening, treatment, and expedited partner therapy (if possible).
- Have early and repeated shared decision-making conversations about postpartum birth control options, including long-acting reversible contraceptives.
- Provide blood pressure screening and monitoring, including remote home surveillance as needed; consider prescribing aspirin, 81 mg daily, as appropriate for preeclampsia prevention.14
- Screen for intimate partner violence and mood disorders throughout the pregnancy and postpartum periods, with timely intervention and referral to behavioral support when needed.
- Encourage breastfeeding by providing free breast pumps and breastfeeding support and by recommending appropriate tools and resources, including mobile apps.15
- Promote the use of doulas to improve experience and outcomes.16,17
Perinatal Care of the Patient With OUD
Chronic, untreated addiction during pregnancy is associated with lack of health care; increased risk of fetal growth restriction, placental abruption, fetal death, and preterm labor; and-high-risk behavior such as prostitution or trading sex for drugs. Pregnant patients with OUD often have coexisting mental health disorders, poor nutrition, and disrupted social support systems.18
Among women who have OUD, up to 80% of pregnancies are unintended.19 Priorities in treatment should include offering pharmacologic therapy for OUD, such as opioid agonists; screening and providing treatment for mood disorders; screening for intimate partner violence; discussing postpregnancy contraceptive options, including long-acting reversible contraceptives and emergency contraception; screening for HIV and other sexually transmitted infections, including hepatitis B and C; screening for tuberculosis; and considering preexposure prophylaxis for HIV.19,20
The following actions should be prioritized during the perinatal care of patients with OUD:
- Screen all pregnant patients for substance use disorders.19
- Screen for sexually transmitted infections, including hepatitis C, and for tuberculosis at the start of care with consideration to repeat screening in the third trimester.
- Screen and provide treatment for mental health disorders.
- Perform dating ultrasonography, second trimester ultrasonography, and third trimester growth ultrasonography.
- Provide early referral to social services and case management; offer residential treatment options if appropriate.
- Consider completing a plan of care document that outlines pregnancy support, plans for delivery, and postpartum care for the parent(s) and child.21,22
- Continue prescribing current opioid agonists, and adjust dosing schedules and dosages as needed during pregnancy 23; all available opioid agonists are acceptable to continue throughout pregnancy (e.g., methadone, buprenorphine, buprenorphine/naloxone, buprenorphine extended-release injection).
- Offer opioid agonist pharmacotherapy in patients who are not already taking it; this improves outcomes compared with medically supervised withdrawal.19
- Provide counseling about neonatal abstinence syndrome and the possibility of a prolonged hospital stay for neonatal monitoring; discuss the benefits of skin-to-skin contact and early breastfeeding for reducing the duration and severity of neonatal abstinence syndrome.24
- Familiarize yourself with reporting requirements in your state, and educate the patient about these policies and what the involvement of government agencies may look like intra- and postpartum.25
- Create a multidisciplinary plan for labor and delivery, including preplanning with anesthesiology, neonatology, and obstetrics (including maternal-fetal medicine) as needed.
- In patients with OUD, 25% to 35% do not attend postpartum visits; parent/infant dyad care improves attendance at postpartum visits and may play an important role in increasing sobriety and safety for the dyad.26

