Fibromyalgia is a chronic, centralized pain syndrome characterized by disordered processing of painful stimuli. Fibromyalgia is diagnosed more frequently in women and occurs globally, affecting 2% of people in the United States. Patients with fibromyalgia have diffuse chronic pain, poor sleep, fatigue, cognitive dysfunction, and mood disturbances. Comorbid conditions, such as functional somatic syndromes, psychiatric diagnoses, and rheumatologic conditions may be present. The Fibromyalgia Rapid Screening Tool is a helpful screening method for patients with diffuse chronic pain. The American College of Rheumatology criteria or the Analgesic, Anesthetic, and Addiction Clinical Trial Translations Innovations Opportunities and Networks–American Pain Society Pain Taxonomy diagnostic criteria can diagnose fibromyalgia. Establishing the diagnosis and providing education can reassure patients and decrease unnecessary testing. A multidisciplinary approach that incorporates nonpharmacologic therapies and medications to address problematic symptoms is most effective. Patient education, exercise, and cognitive behavior therapy can improve pain and function. Duloxetine, milnacipran, pregabalin, and amitriptyline are potentially effective medications for fibromyalgia. Nonsteroidal anti-inflammatory drugs and opioids have not demonstrated benefits for fibromyalgia and have significant limitations.
Fibromyalgia is characterized by diffuse musculoskeletal pain, fatigue, poor sleep, and other somatic symptoms.1 Chronic diffuse pain affects 10% to 15% of adults in the general population worldwide, many of whom have fibromyalgia.2,3 Approximately 2% of people in the United States have fibromyalgia, although the prevalence varies across populations and with the diagnostic criteria used.3 Fibromyalgia can occur in children and adults and is found worldwide and across cultures. Women are diagnosed more frequently than men; a Scottish survey found that women are diagnosed between two and 14 times as often as men depending on the criteria used.3,4 Changes in the diagnostic criteria over the past decade, including the elimination of specific tender points, have resulted in more patients with chronic pain meeting the criteria for fibromyalgia.3–5
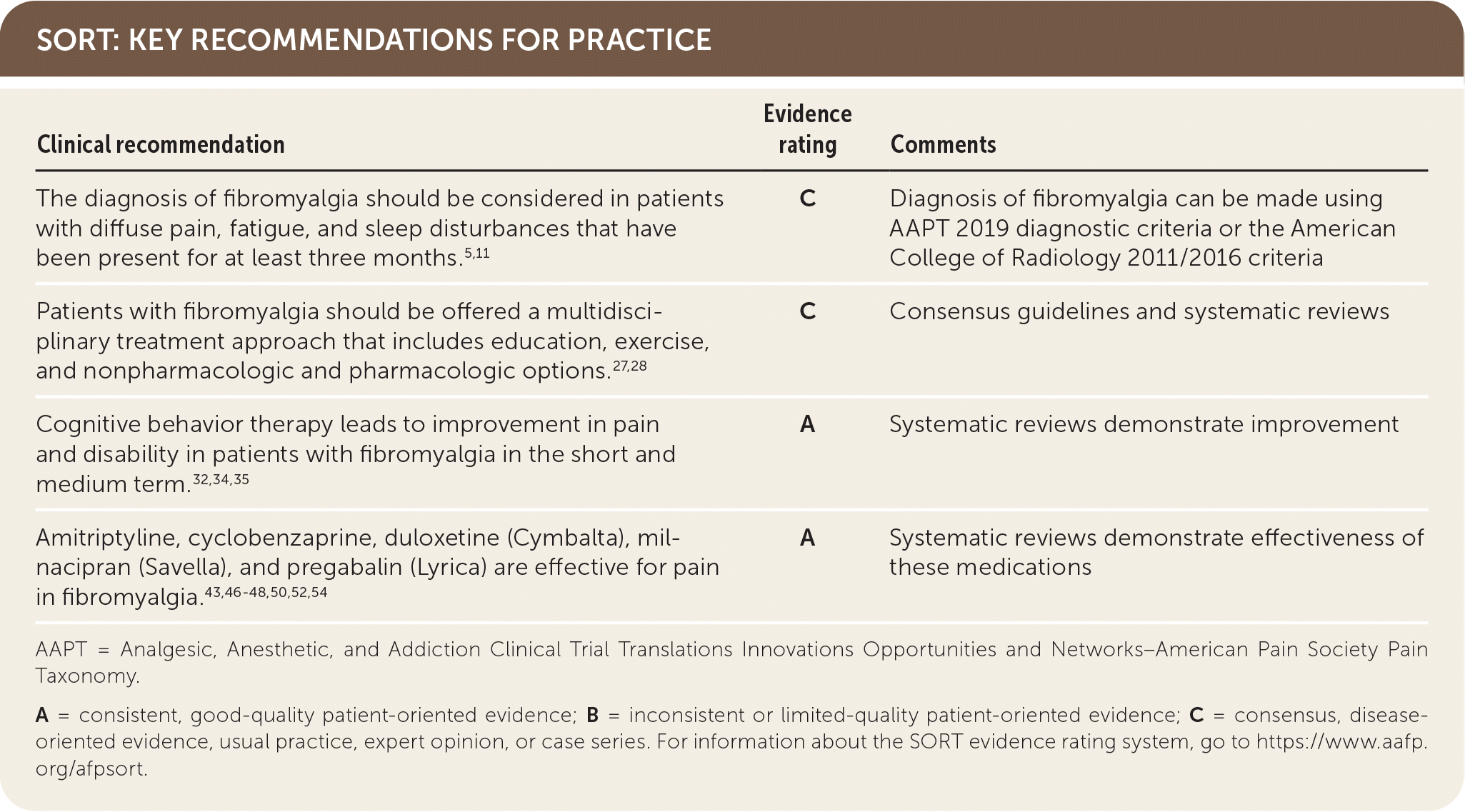
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | Comments |
|---|---|---|
| The diagnosis of fibromyalgia should be considered in patients with diffuse pain, fatigue, and sleep disturbances that have been present for at least three months.5,11 | C | Diagnosis of fibromyalgia can be made using AAPT 2019 diagnostic criteria or the American College of Radiology 2011/2016 criteria |
| Patients with fibromyalgia should be offered a multidisciplinary treatment approach that includes education, exercise, and nonpharmacologic and pharmacologic options.27,28 | C | Consensus guidelines and systematic reviews |
| Cognitive behavior therapy leads to improvement in pain and disability in patients with fibromyalgia in the short and medium term.32,34,35 | A | Systematic reviews demonstrate improvement |
| Amitriptyline, cyclobenzaprine, duloxetine (Cymbalta), milnacipran (Savella), and pregabalin (Lyrica) are effective for pain in fibromyalgia.43,46–48,50,52,54 | A | Systematic reviews demonstrate effectiveness of these medications |
AAPT = Analgesic, Anesthetic, and Addiction Clinical Trial Translations Innovations Opportunities and Networks–American Pain Society Pain Taxonomy.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Pathophysiology
Fibromyalgia is likely caused by disordered central nociceptive signal processing that leads to sensitization expressed as hyperalgesia and allodynia, which is similar to chronic pain conditions such as irritable bowel syndrome, interstitial cystitis, chronic pelvic pain, and chronic low back pain.6,7 Functional brain imaging suggests that this aberrant processing may be attributed to an imbalance between excitatory and inhibitory neurotransmitters, particularly within the insula.8 Suggested etiologies include dysfunction of the hypothalamic-pituitary-adrenal axis and the autonomic nervous system, diffuse inflammation, glial cell activation, small fiber neuropathy, and infections such as the Epstein-Barr virus, Lyme disease, and viral hepatitis.9 Twin studies suggest a genetic component may also be a factor.10
Clinical Presentation
Chronic diffuse pain is the predominant symptom in most patients with fibromyalgia. Patients may also experience muscle stiffness and tenderness. The physical examination in patients with fibromyalgia generally finds diffuse tenderness without other unusual findings. If joint swelling, inflammation, or deformities are present, an alternative or additional diagnosis should be investigated.5 Fatigue and sleep disturbances are also common.5,11 Sleep disturbances include difficulty falling and staying asleep, frequent awakenings, or feeling unrefreshed after sleeping. Comorbid mental health diagnoses are common, as are cognitive symptoms such as poor concentration, forgetfulness, or altered thinking.5,6,12 This cognitive dysfunction has been termed “fibrofog” and is described by patients as a mental slowing that adversely affects daily activities.13
The presence of another painful disorder does not exclude the diagnosis of fibromyalgia. The Fibromyalgia Rapid Screening Tool can screen patients with diffuse chronic pain to help distinguish between fibromyalgia and other conditions (Table 1).14 The tool may also be used to detect coexisting fibromyalgia in patients with confirmed rheumatologic conditions.15
Diagnosis
Fibromyalgia should be considered in patients with chronic pain without a history of tissue injury or inflammation that has been present for more than three months and who also have fatigue, mood issues, and sleep disturbances.
Multiple diagnostic criteria for fibromyalgia have been developed, many of which are in use today. The initial American College of Rheumatology (ACR) classification criteria included widespread pain and multiple specific muscular tender points.16 When these criteria were updated in 2010 and 2011, the physical examination of tender points was eliminated, and a symptom severity scale and self-reported widespread pain index were added.11 The 2011 changes were updated in 2016 to require generalized pain in at least four of five regions for at least three months.11 The 2016 criteria also require minimum scores on the widespread pain index and the symptom severity scale, which rates the degree of fatigue, waking unrefreshed, and cognitive symptoms.
The AAPT (Analgesic, Anesthetic, and Addiction Clinical Trial Translations Innovations Opportunities and Networks–American Pain Society Pain Taxonomy) diagnostic criteria are an alternate framework created in 2019 (Table 2).5 The criteria require at least three months of pain in at least six of nine anatomic regions and moderate to severe sleep problems or fatigue.
The 2011 ACR criteria, the 2016 ACR criteria (Table 311 ), and the 2019 AAPT criteria are acceptable for diagnosis. A single study that compared criteria to rheumatologist diagnosis demonstrated similar sensitivity and specificity for all three. The 74% sensitivity of the 2019 AAPT criteria was less than the 78% to 80% sensitivity of the 2011 and 2016 ACR criteria.17
Comorbidities
Fibromyalgia and other chronic pain conditions may represent a single disorder that manifests as pain in different body regions at different times over the life span. These functional somatic conditions represent a spectrum of chronic pain.6 The coexistence of these conditions is termed chronic overlapping pain.18 Other painful conditions that may coexist with fibromyalgia include temporomandibular pain, irritable bowel syndrome, vulvodynia, myalgic encephalomyelitis (i.e., chronic fatigue syndrome), interstitial cystitis, endometriosis, chronic tension headaches, migraine headaches, and chronic low back pain.18
Restless legs syndrome may occur with fibromyalgia, exacerbating sleep disturbances.19,20 Psychiatric comorbidities are common in patients with fibromyalgia. More than one-half of patients with fibromyalgia also experience depression.21,22 Other mental health conditions often coexist with fibromyalgia, including bipolar disorder, generalized anxiety, and substance use disorder.22,23
Patients with rheumatologic conditions, including rheumatoid arthritis, ankylosing spondylitis, and psoriatic arthritis, may also have fibromyalgia, although the symptom overlap makes a diagnosis challenging.24 The presence of erythematous, swollen, or painful joints suggests a rheumatologic source, whereas diffuse soft tissue tender points may indicate fibromyalgia. Patients with fibromyalgia and inflammatory conditions tend to have higher self-rated disease activity scores than the degree of inflammation, which can lead to overtreatment of the inflammatory condition.24
Differential Diagnosis
The differential diagnosis includes rheumatologic conditions, such as rheumatoid arthritis, systemic lupus erythematosus, systemic sclerosis, spondyloarthropathies, polymyalgia rheumatica, and myopathies.5 Fibromyalgia should be considered in patients with other rheumatologic diagnoses who do not respond well to treatment of their primary condition. Based on the history and examination findings, other diagnoses to consider include Lyme disease, hepatitis, hyperthyroidism, hypothyroidism, hyperparathyroidism, and neurologic conditions such as multiple sclerosis and other disorders that cause neuropathic pain. The Choosing Wisely initiative recommends against testing for Lyme disease as a cause of musculoskeletal symptoms without an exposure history and relevant examination findings.25 Medication adverse effects can rarely cause diffuse pain, including from statins, opioids, bisphosphonates, and aromatase inhibitors.5
Testing
Fibromyalgia is a clinical diagnosis, and laboratory testing is not routinely needed. Because fatigue can be from many causes, clinicians can consider a complete blood count to exclude anemia, a comprehensive metabolic panel, and a thyroid-stimulating hormone test.12 Tests for rheumatoid factor or antinuclear antibody levels are not recommended in patients without features concerning for a rheumatologic condition because of their high false-positive rates.5,12
A cytokine array–based blood test, known as the FM/a Test, has the potential to help confirm the diagnosis of fibromyalgia.26 Patients with fibromyalgia demonstrate higher cytokine production in stimulated immune cells than in the general population. The FM/a Test demonstrated 93% sensitivity and 89% specificity in 160 patients with fibromyalgia compared with patients in the control group.26 Compared with people who have rheumatoid arthritis or systemic lupus erythematosus without fibromyalgia, the specificity of the FM/a Test was 70%; however, the test had a positive likelihood ratio of 3.1 and a negative likelihood ratio of 0.1.26 This test is not commonly used and is expensive, but could be beneficial to help differentiate fibromyalgia from other conditions.
Management
The initial benefit of establishing the diagnosis of fibromyalgia is to reassure patients and prevent further unnecessary testing and anxiety. The goal of fibromyalgia treatment is to manage symptoms such as pain, fatigue, poor sleep, and cognitive issues. A multidisciplinary individualized treatment regimen that includes pharmacologic and nonpharmacologic elements is recommended. An industry-funded initiative called the FibroCollaborative convened a panel of fibromyalgia experts to make clinical recommendations. It emphasizes a multimodal approach that includes patient education, treatment of comorbid conditions, lifestyle modification, pharmacologic therapy, cognitive behavior therapy (CBT), and self-management support.27
NONPHARMACOLOGIC TREATMENT
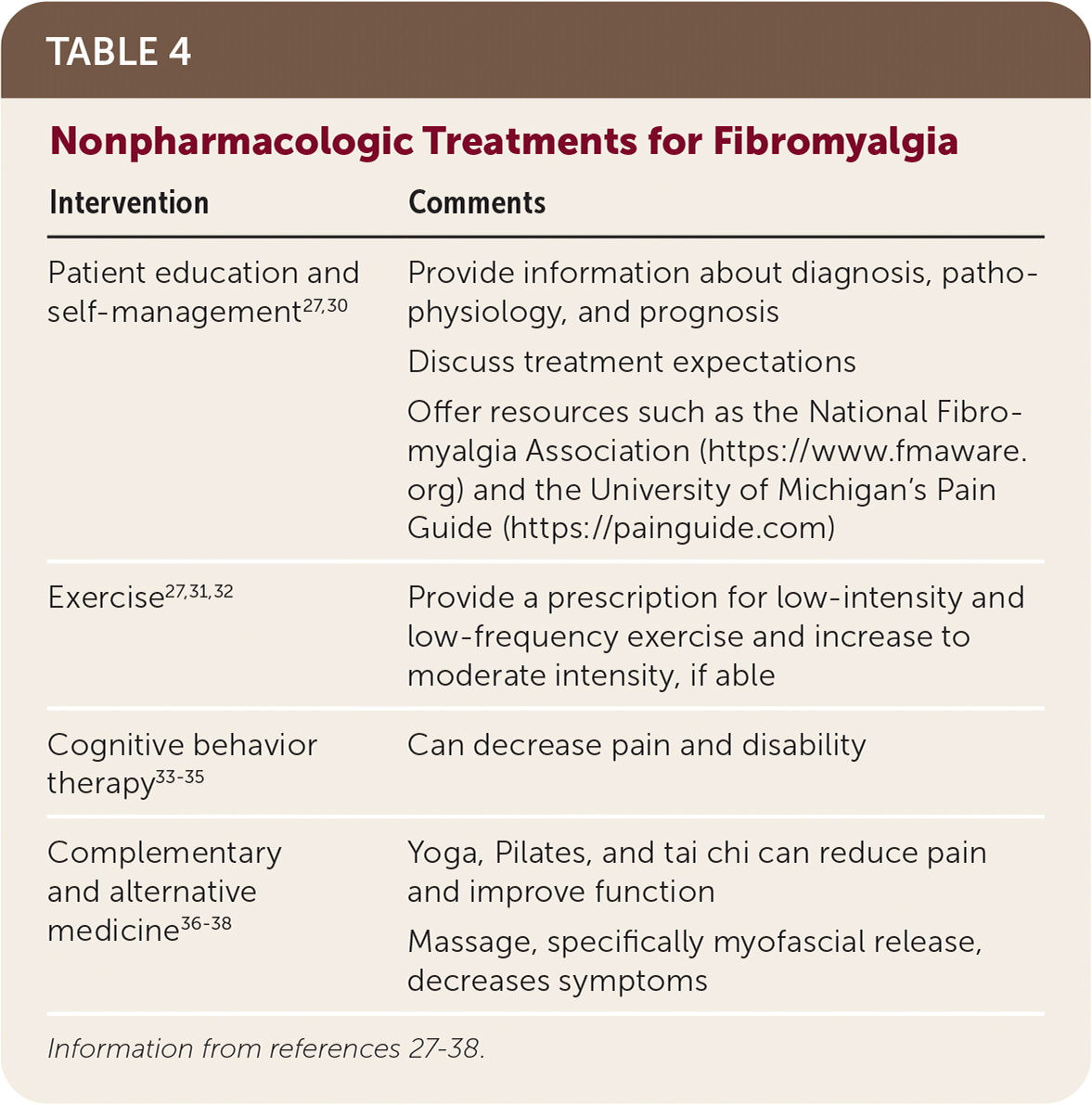
Patient education is important for patients with fibromyalgia and improves outcomes.27,28 Educating patients about the diagnosis, pathophysiology, and clinical manifestations can reassure patients, improve patient satisfaction, decrease symptoms, and reduce health care utilization.6,12,27 Clinicians can refer patients to websites such as the University of Michigan's Pain Guide and the National Fibromyalgia Association.29,30 Combining self-management strategies with exercise is beneficial.31 Table 4 lists nonpharmacologic treatment options for fibromyalgia.27–38
TABLE 4. Nonpharmacologic Treatments for Fibromyalgia
| Intervention | Comments |
|---|---|
| Patient education and self-management27,30 | Provide information about diagnosis, pathophysiology, and prognosis Discuss treatment expectations Offer resources such as the National Fibromyalgia Association (https://www.fmaware.org) and the University of Michigan's Pain Guide (https://painguide.com) |
| Exercise27,31,32 | Provide a prescription for low-intensity and low-frequency exercise and increase to moderate intensity, if able |
| Cognitive behavior therapy33–35 | Can decrease pain and disability |
| Complementary and alternative medicine36–38 | Yoga, Pilates, and tai chi can reduce pain and improve function Massage, specifically myofascial release, decreases symptoms |
There is moderate-quality evidence that exercise (i.e., aerobic, resistance, stretching, or a combination) produces small improvements in quality of life, pain, and physical function in patients with fibromyalgia.33,39 The strongest evidence exists for aerobic exercise of moderate intensity. In addition to improvements in pain and function, exercise can decrease fatigue and improve sleep quality.32 Exercise prescriptions should start at a low intensity and low frequency and gradually increase in intensity and frequency.
CBT teaches patients how to change negative thoughts and behaviors, and helps promote skills to improve chronic pain, fatigue, and poor sleep. Options include traditional CBT, acceptance-based cognitive therapies, and operant therapy. Three systematic reviews demonstrated moderate-quality evidence that patients with fibromyalgia treated with CBT experience modest improvements in pain and disability in the short and medium term.32,34,35
As part of a multidisciplinary treatment approach, patients with fibromyalgia may pursue complementary and alternative medicine options such as acupuncture, massage, meditation, nutritional supplements, and herbs.27,28 Most complementary and alternative medicine options have not been extensively studied, and there is no consistently high-quality evidence to support them.40 A systematic review found that yoga, Pilates, and tai chi improved function and reduced pain.36 One randomized trial found that performing tai chi for one hour twice per week for 12 to 24 weeks led to moderate symptomatic improvement in pain and function.37 Meditation and mindfulness techniques are also promising options.40 A Cochrane review concluded that acupuncture could improve short-term pain and stiffness compared with usual care, but it is not consistently better than sham acupuncture.41 Manual therapy, specifically myofascial release, may decrease symptoms and improve the quality of life in patients with fibromyalgia.38 Manual therapy acts on the ascending nociceptive pathways involved in the process of central sensitization.38 A small trial suggested that patient self-myofascial release improves pain and quality of life.42
There are limited studies showing uncertain benefits of cannabinoids for the treatment of fibromyalgia, although use is becoming more common.40 Other possible treatments that have not been well studied in patients with fibromyalgia include transcutaneous electrical nerve stimulation units, thermal therapies, hyperbaric oxygen, laser and phototherapy, transdermal magnesium, and vibroacoustic and rhythmic sensory stimulation.13,40
PHARMACOLOGIC TREATMENT
Because nonpharmacologic measures often do not provide adequate symptom relief, medications are also used to treat the most problematic symptoms. Potentially useful medication classes include tricyclic antidepressants, serotonin-norepinephrine reuptake inhibitors, and gabapentinoids.28 A single medication should be started at a low dosage, slowly increased to the recommended dosage, and then continued for at least three months to ensure an adequate trial, unless adverse effects are intolerable. If a satisfactory clinical response is achieved, treatment should be continued for at least 12 months. In patients who do not respond to an adequate trial of medication, clinicians should assess medication adherence, confirm that nonpharmacologic management has been maximized, and exclude other conditions that may need additional intervention.43 Few studies compare monotherapy with combination pharmacotherapy for fibromyalgia; however, combinations are sometimes needed.44,45 Duloxetine (Cymbalta), milnacipran (Savella), and pregabalin (Lyrica) are approved by the U.S. Food and Drug Administration for the treatment of fibromyalgia in the United States; however, several other medications are beneficial46 (Table 527,28,47–52 ).
TABLE 5. Medications for Fibromyalgia
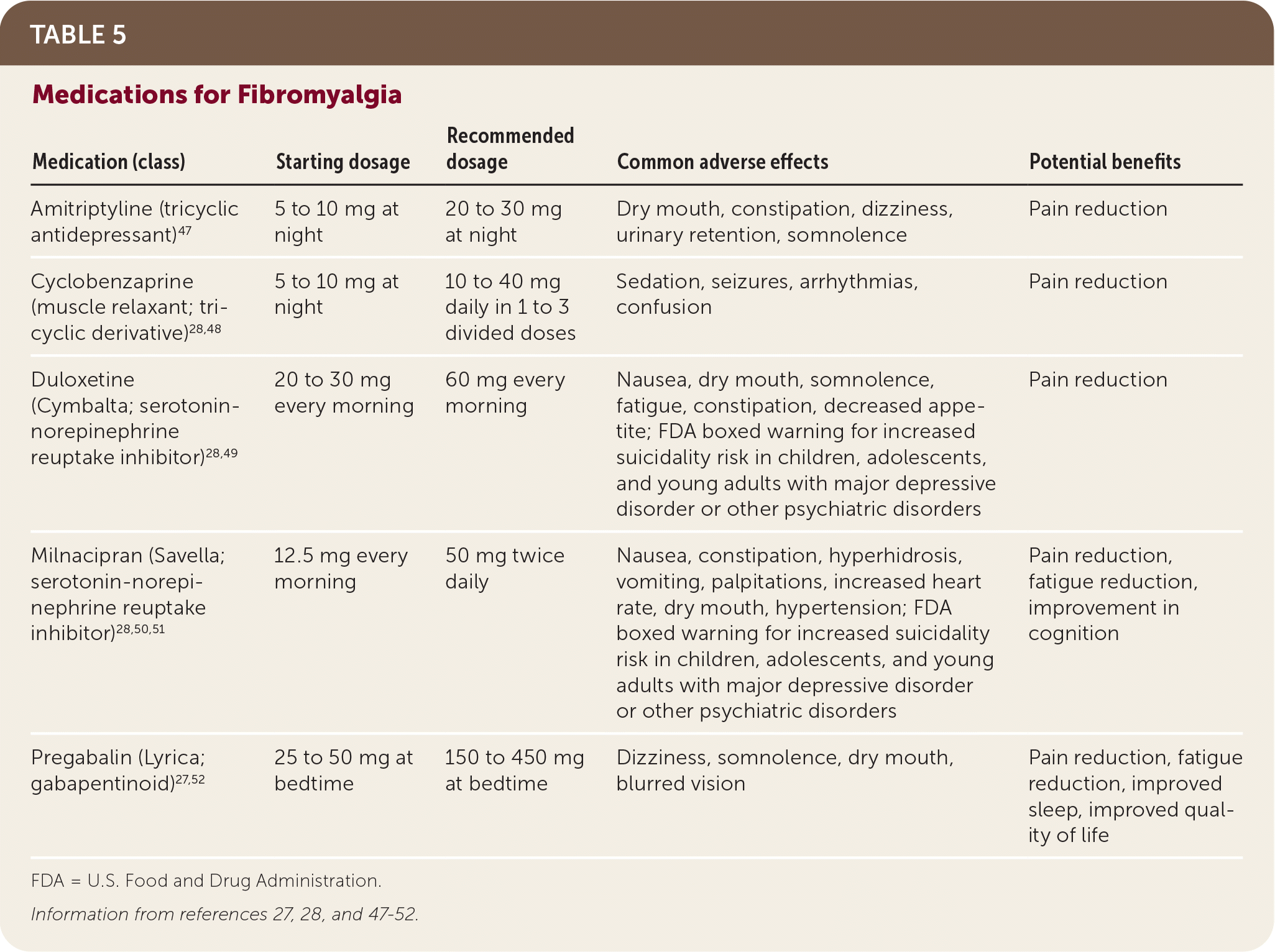
| Medication (class) | Starting dosage | Recommended dosage | Common adverse effects | Potential benefits |
|---|---|---|---|---|
| Amitriptyline (tricyclic antidepressant)47 | 5 to 10 mg at night | 20 to 30 mg at night | Dry mouth, constipation, dizziness, urinary retention, somnolence | Pain reduction |
| Cyclobenzaprine (muscle relaxant; tricyclic derivative)28,48 | 5 to 10 mg at night | 10 to 40 mg daily in 1 to 3 divided doses | Sedation, seizures, arrhythmias, confusion | Pain reduction |
| Duloxetine (Cymbalta; serotonin-norepinephrine reuptake inhibitor)28,49 | 20 to 30 mg every morning | 60 mg every morning | Nausea, dry mouth, somnolence, fatigue, constipation, decreased appetite; FDA boxed warning for increased suicidality risk in children, adolescents, and young adults with major depressive disorder or other psychiatric disorders | Pain reduction |
| Milnacipran(Savella; serotonin-norepinephrine reuptake inhibitor)28,50,51 | 12.5 mg every morning | 50 mg twice daily | Nausea, constipation, hyperhidrosis, vomiting, palpitations, increased heart rate, dry mouth, hypertension; FDA boxed warning for increased suicidality risk in children, adolescents, and young adults with major depressive disorder or other psychiatric disorders | Pain reduction, fatigue reduction, improvement in cognition |
| Pregabalin (Lyrica; gabapentinoid)27,52 | 25 to 50 mg at bedtime | 150 to 450 mg at bedtime | Dizziness, somnolence, dry mouth, blurred vision | Pain reduction, fatigue reduction, improved sleep, improved quality of life |
FDA = U.S. Food and Drug Administration.
Tricyclic antidepressant medications improve several symptoms of fibromyalgia. A systematic review of amitriptyline demonstrated reduced pain, improved sleep, and improved patient satisfaction after six to eight weeks.47 Other tricyclic agents such as nortriptyline have fewer adverse effects and may be better tolerated; however, there are few studies evaluating their use in fibromyalgia.53 For patients unable to tolerate amitriptyline, cyclobenzaprine, a muscle relaxant that is a tricyclic derivative, can be a reasonable option. A meta-analysis of five randomized trials found that cyclobenzaprine produced modest pain reduction without affecting fatigue or sleep.48 There is insufficient evidence for other muscle relaxants in the treatment of fibromyalgia.
A Cochrane review found low-quality evidence that duloxetine and milnacipran improved pain relief.50 A systematic review showed that duloxetine produced greater pain relief compared with placebo and other antidepressants such as sertraline, paroxetine, fluoxetine, and bupropion.49 Milnacipran improves pain, fatigue, and cognition compared with placebo over three months.28,51,54 Other serotonin-norepinephrine reuptake inhibitors, such as venlafaxine, have not been examined as extensively. A Cochrane review did not find evidence that selective serotonin reuptake inhibitors helped treat pain, fatigue, or sleep problems in fibromyalgia, although they can effectively treat depression.55
Gabapentinoids may be helpful in fibromyalgia with severe sleep disturbances. Pregabalin reduces pain by up to 50% with a number needed to treat of 10, and improves sleep, fatigue, and quality of life.52,56 The evidence is insufficient to determine if gabapentin is effective for fibromyalgia.57
There is also insufficient evidence to recommend the routine use of opioids in fibromyalgia. Opioids are not recommended for fibromyalgia because they do not target the processes involved in centralized sensitization, and their use may cause additional harm because of the risk of dependence, misuse, worsening of hyperalgesia, and other significant adverse effects.28,58 A Cochrane review concluded that nonsteroidal anti-inflammatory medications are not superior to placebo for pain in fibromyalgia and can have significant adverse effects.59 The data are insufficient to determine the benefit of acetaminophen for pain in fibromyalgia.28
This article updates previous articles on this topic by Kodner,12 Chakrabarty and Zoorob,1 and Millea and Holloway.60
Data Sources: A PubMed search was completed in Clinical Queries, the Cochrane database, and Essential Evidence Plus using the key terms fibromyalgia, diagnosis, and treatment. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. The initial search was limited to the years 2010 to 2021. Search dates: August 17, 2021, October 27, 2021, and January 5, 2023.

