To the Editor: A healthy 18-year-old patient presented with three years of bilateral great toe-nail thickening, with no preceding trauma, tight footwear, or family history of skin or nail disease. Empiric treatment with topical antifungals had been ineffective.
The examination found subtle valgus deformities at the interphalangeal joints of both great toes, with hyperkeratosis, yellowing, horizontal ridging, and lateral nail plate deviation (Figure 1). The right nail plate showed early trapezoidal change at the distal edge (Figure 2). The patient's skin and other nails were unaffected.
FIGURE 1.
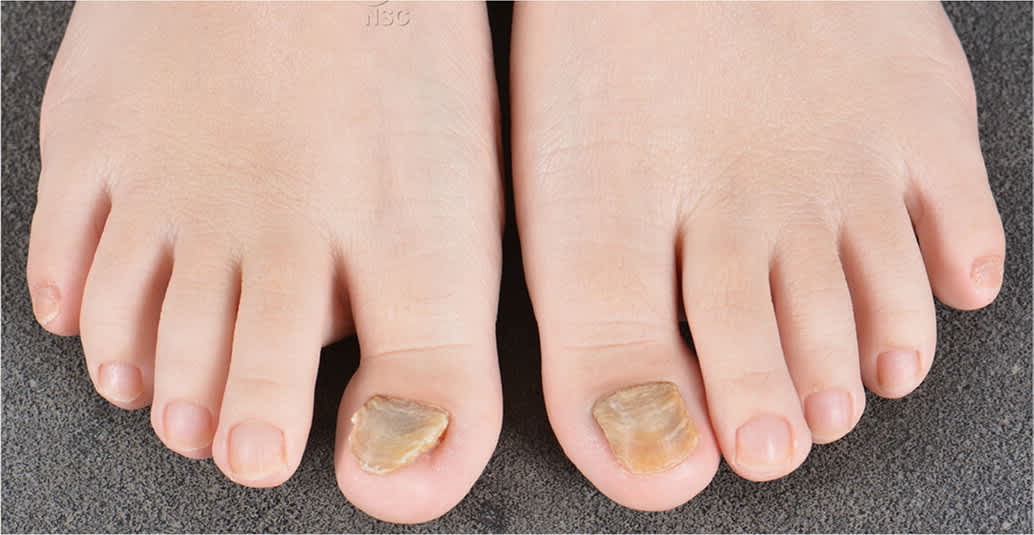
Subtle valgus deformities at the interphalangeal joints with hyperkeratosis, yellowing, horizontal ridging, and lateral nail plate deviation.
Reprinted with permission from the National Skin Centre, Singapore.
FIGURE 2. Close-up of the right great toenail showing lateral nail plate deviation and early trapezoidal change at the distal edge.
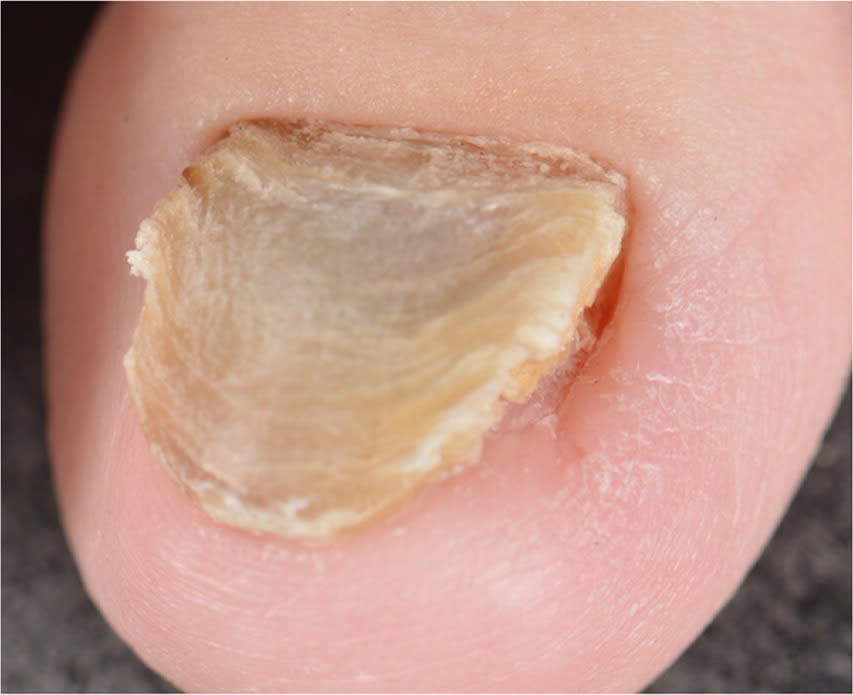
Reprinted with permission from the National Skin Centre, Singapore.
Histology of the nail bed and matrix found no cytologic atypia or inflammation. Two negative fungal cultures of the nail plate excluded onychomycosis. Onychodystrophy from late-onset congenital malalignment of the great toenails was diagnosed.
Congenital malalignment of the great toenail is the lateral deviation of the nail plate on its longitudinal axis and is usually bilateral and present at birth.1 Theories about its pathogenesis include nail matrix deviation because of increased traction by the extensor hallucis tendons and dyssynchronous growth of the nail apparatus and the distal phalanx.1,2 Mechanical instability of the nail plate with poor contact between the nail plate and bed, combined with secondary trauma, hemorrhage, or bacterial infection, results in nail plate thickening, opacity, ridging, and tapering toward the distal edge.2
Congenital malalignment usually presents in early childhood, with a slight female predilection.2 However, chronic microtrauma and recurrent mechanical stresses in a patient with an existing mild, initially clinically inapparent congenital malalignment may lead to the emergence of nail plate deviation later in life.3
Spontaneous resolution has been reported in one-half of childhood cases of congenital malalignment, but data on late-onset malalignment are limited.4 Clinicians should evaluate and treat secondary infections. Therapeutic considerations are the degree of nail plate deviation and patient preference. Well-fitting footwear, nail trimming, and a podiatry review would be reasonable recommendations for this patient because of their mild lateral deviation and preference for conservative treatment. Partial or total matricectomy may be considered when the deviation is notable or causes ingrown nails and pain. Surgical realignment of the nail apparatus has been described in children two years and younger.4
Recognizing nail plate malalignment in patients presenting with great toenail onychodystrophy helps to minimize unnecessary procedures and ineffective treatment and manage expectations about the trajectory of recovery.

