An acute uncomplicated urinary tract infection (UTI) is a bacterial infection of the lower urinary tract with no sign of systemic illness or pyelonephritis in a noncatheterized, nonpregnant adult with no urologic abnormalities or immunocompromise. In women, a self-diagnosis of a UTI with the presence of typical symptoms (e.g., frequency, urgency, dysuria/burning sensation, nocturia, suprapubic pain), without vaginal discharge, is accurate enough to diagnose an uncomplicated UTI without further testing. Urine culture and susceptibility testing should be reserved for women with recurrent infection, treatment failure, history of resistant isolates, or atypical presentation to make a definitive diagnosis and guide antibiotic selection. First-line antibiotics include nitrofurantoin for five days, fosfomycin in a single dose, trimethoprim for three days, or trimethoprim/sulfamethoxazole for three days. Symptomatic treatment with nonsteroidal anti-inflammatory drugs and delayed antibiotics may be considered because the risk of complications is low. Increased fluids, intake of cranberry products, and methenamine hippurate can prevent recurrent infections. Antibiotic prophylaxis is also effective in preventing recurrence but has a risk of adverse effects and antimicrobial resistance. Men with lower UTI symptoms should always receive antibiotics, with urine culture and susceptibility results guiding the antibiotic choice. Clinicians should also consider the possibility of urethritis and prostatitis in men with UTI symptoms. First-line antibiotics for men with uncomplicated UTI include trimethoprim, trimethoprim/sulfamethoxazole, and nitrofurantoin for seven days. Uncomplicated UTIs in nonfrail women and men 65 years and older with no relevant comorbidities also necessitate a urine culture with susceptibility testing to adjust the antibiotic choice after initial empiric treatment; first-line antibiotics and treatment durations do not differ from those recommended for younger adults.
This article provides a rapid evidence review of the best available patient-oriented evidence for acute uncomplicated urinary tract infection (UTI) in adults. An uncomplicated UTI is a bacterial infection of the lower urinary tract in a noncatheterized, nonpregnant adult without urologic abnormalities, immunocompromise, or signs of systemic illness or pyelonephritis. More than 80% of UTIs occur in women; therefore, unless specified, the recommendations in this article are for adult women younger than 65 years. Recommendations for uncomplicated UTIs in other populations, such as men and women and men 65 years or older, are reviewed briefly. Nonbinary and transgender people should be evaluated and treated according to their current urogenital anatomy.
WHAT'S NEW ON THIS TOPIC

| In U.S. outpatients, the resistance of common uropathogens to beta-lactam antibiotics, trimethoprim/sulfamethoxazole, and fluoroquinolones is greater than 55%, 22%, and 21%, respectively. |
| Recent European and UK guidelines do not recommend trimethoprim/sulfamethoxazole due to concerns about adverse effects (rare but severe skin and neurologic manifestations), allergy, and increasing resistance in many communities. |
| Relapse within two weeks or recurrent urinary tract infections are equally likely in women initially treated with or without antibiotics. |
SORT: KEY RECOMMENDATIONS FOR PRACTICE
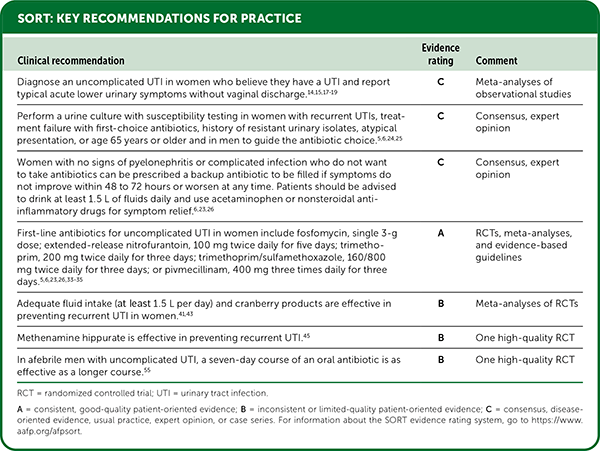
RCT = randomized controlled trial; UTI = urinary tract infection.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN INFECTIOUS DISEASE

| Recommendation | Sponsoring organization |
|---|---|
| Avoid using a fluoroquinolone antibiotic for the first-line treatment of uncomplicated UTIs in women. | American Urogynecologic Society |
| Avoid presumptive antibiotic treatment of recurrent UTIs in women without first obtaining a urinalysis (culture and sensitivity). | American Urogynecologic Society |
| Do not order urine cultures unless patients have symptoms consistent with a UTI. | American Society for Microbiology |
Note: For Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/pubs/afp/collections/choosing-wisely.html.
UTI = urinary tract infection.
Epidemiology and Microbiology
- The self-reported annual incidence of UTI is 11% in women and 3% in men.1,2 UTIs are most common in women between 18 and 29 years of age.3
- UTIs are uncommon in men younger than 60 years; by 80 years of age, women and men have similar incidence rates.2,3
- Most UTIs are uncomplicated. Complicating factors are listed in Table 1.4–7
- Uropathogenic Escherichia coli causes 75% to 90% of UTIs; the remaining infections are caused by organisms such as Enterobacteriaceae, Enterococcus species, Staphylococcus saprophyticus, and Pseudomonas aeruginosa (Table 2).8,9
- In U.S. outpatients, the resistance of common uropathogens to beta-lactam antibiotics, trimethoprim/sulfamethoxazole, and fluoroquinolones is 55.8%, 22.4%, and 21.6%, respectively.10
- Multidrug-resistant uropathogens are increasingly prevalent. The primary risk factors for bacterial resistance include recent antibiotic use and hospitalization in the past three months.11,12
TABLE 1. Signs and Underlying Conditions Related to Complicated Urinary Tract Infections
TABLE 2. Prevalence of the Most Common Organisms That Cause Acute Uncomplicated Urinary Tract Infections
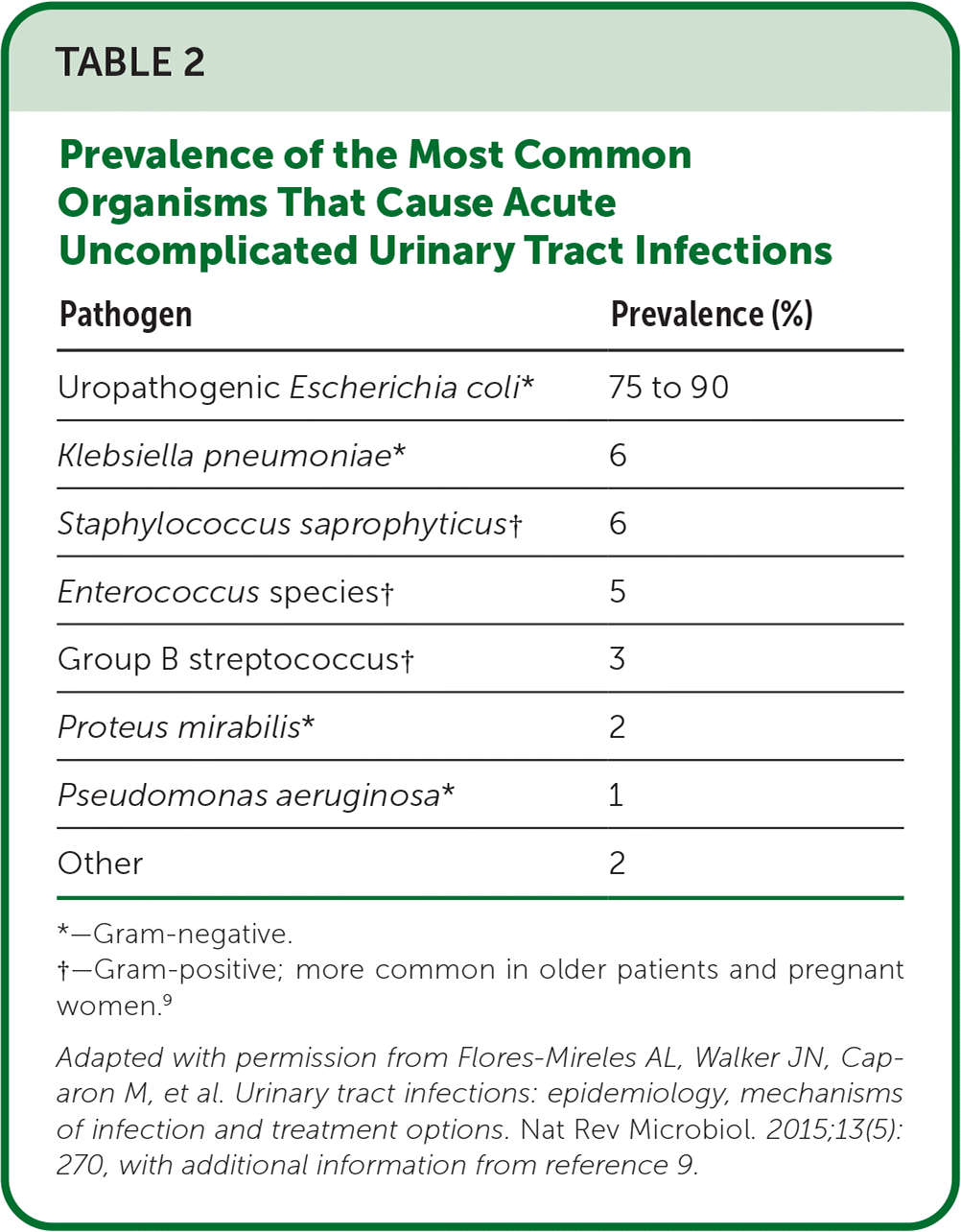
| Pathogen | Prevalence (%) |
|---|---|
| Uropathogenic Escherichia coli* | 75 to 90 |
| Klebsiella pneumoniae* | 6 |
| Staphylococcus saprophyticus† | 6 |
| Enterococcus species† | 5 |
| Group B streptococcus† | 3 |
| Proteus mirabilis* | 2 |
| Pseudomonas aeruginosa* | 1 |
| Other | 2 |
*—Gram-negative.
†—Gram-positive; more common in older patients and pregnant women.9
Adapted with permission from Flores-Mireles AL, Walker JN, Caparon M, et al. Urinary tract infections: epidemiology, mechanisms of infection and treatment options. Nat Rev Microbiol. 2015;13(5):270, with additional information from reference 9.
Diagnosis
- The typical presentation includes frequency, urgency, dysuria/burning sensation, nocturia, and suprapubic pain or tenderness. Physical examination findings are usually normal.4,5,13
- The prevalence of culture-confirmed UTI among women with urinary tract symptoms is 45% to 65%.14 Combinations of signs and symptoms suggesting other diagnoses are presented in Table 3.4,5,15,16
TABLE 3. Differential Diagnosis of Urinary Tract Infection in Women
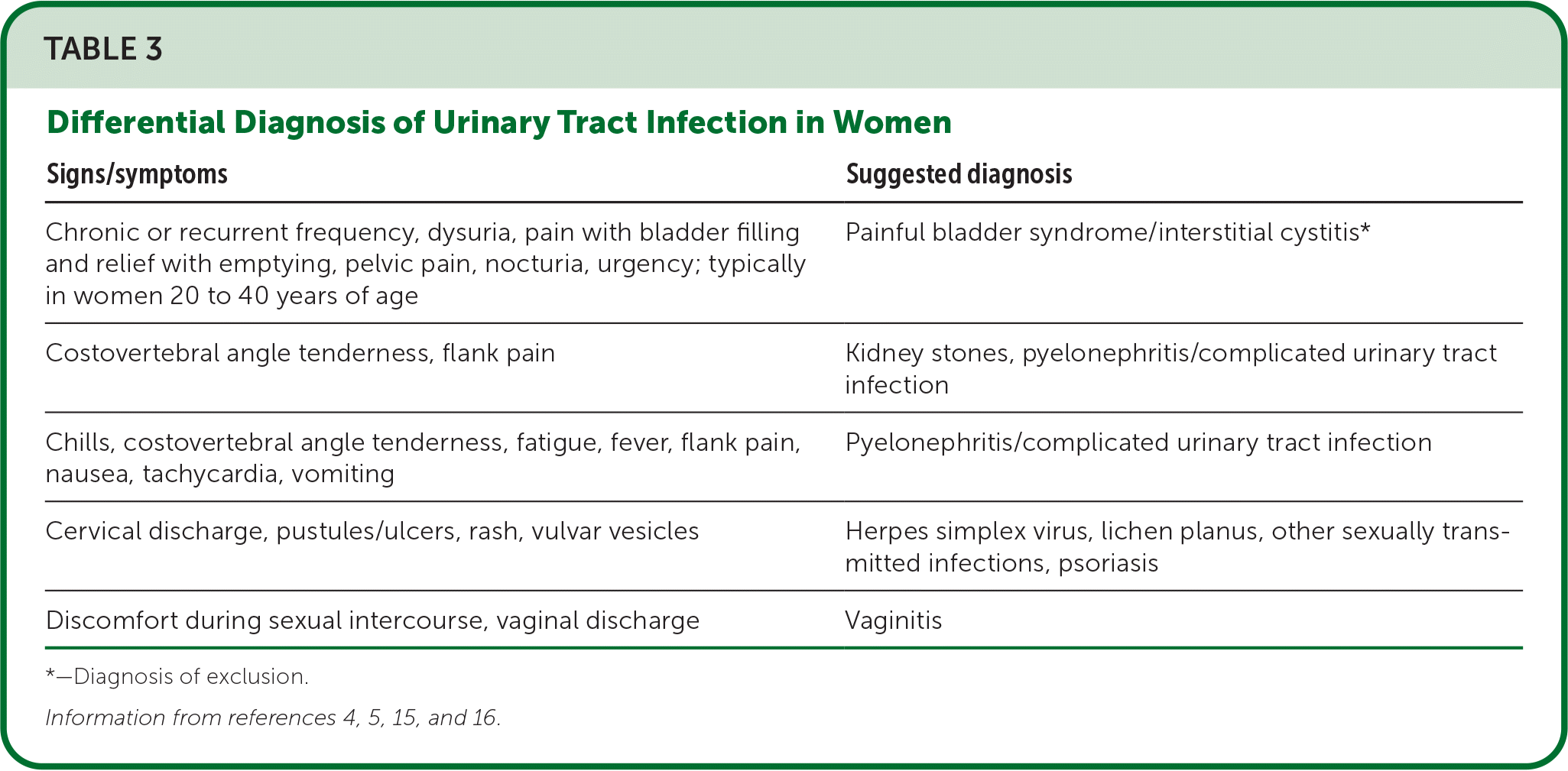
| Signs/symptoms | Suggested diagnosis |
|---|---|
| Chronic or recurrent frequency, dysuria, pain with bladder filling and relief with emptying, pelvic pain, nocturia, urgency; typically in women 20 to 40 years of age | Painful bladder syndrome/interstitial cystitis* |
| Costovertebral angle tenderness, flank pain | Kidney stones, pyelonephritis/complicated urinary tract infection |
| Chills, costovertebral angle tenderness, fatigue, fever, flank pain, nausea, tachycardia, vomiting | Pyelonephritis/complicated urinary tract infection |
| Cervical discharge, pustules/ulcers, rash, vulvar vesicles | Herpes simplex virus, lichen planus, other sexually transmitted infections, psoriasis |
| Discomfort during sexual intercourse, vaginal discharge | Vaginitis |
*—Diagnosis of exclusion.
SIGNS, SYMPTOMS, AND URINALYSIS
- According to a systematic review using a positive urine culture result as the reference standard, dysuria, frequency, urgency, nocturia, and hematuria increase the likelihood of UTI, with hematuria showing the highest predictive value, especially if combined with a dipstick test positive for nitrites.17
- Another systematic review found that dysuria, urgency, nocturia, and sexual activity with simultaneous presence of urgency and dysuria are weak diagnostic indicators of UTI, whereas vaginal discharge is a weak predictor of the absence of UTI.18
- Self-diagnosis of UTI is a stronger predictor of UTI, or no UTI, than individual symptoms or signs.15,19
- Based on two meta-analyses, dipstick testing positive for nitrites is helpful in diagnosing a UTI (positive likelihood ratio = 5.3 to 6.5), whereas dipstick testing negative for both leukocytes and nitrites can exclude a UTI (negative likelihood ratio = 0.25).18,20
- Posttest probabilities and likelihood ratios for positive or negative clinical findings and dipstick test results are presented in Table 4.15,17,18
TABLE 4. Probability of a UTI in Women Based on Symptoms and Dipstick Test Results
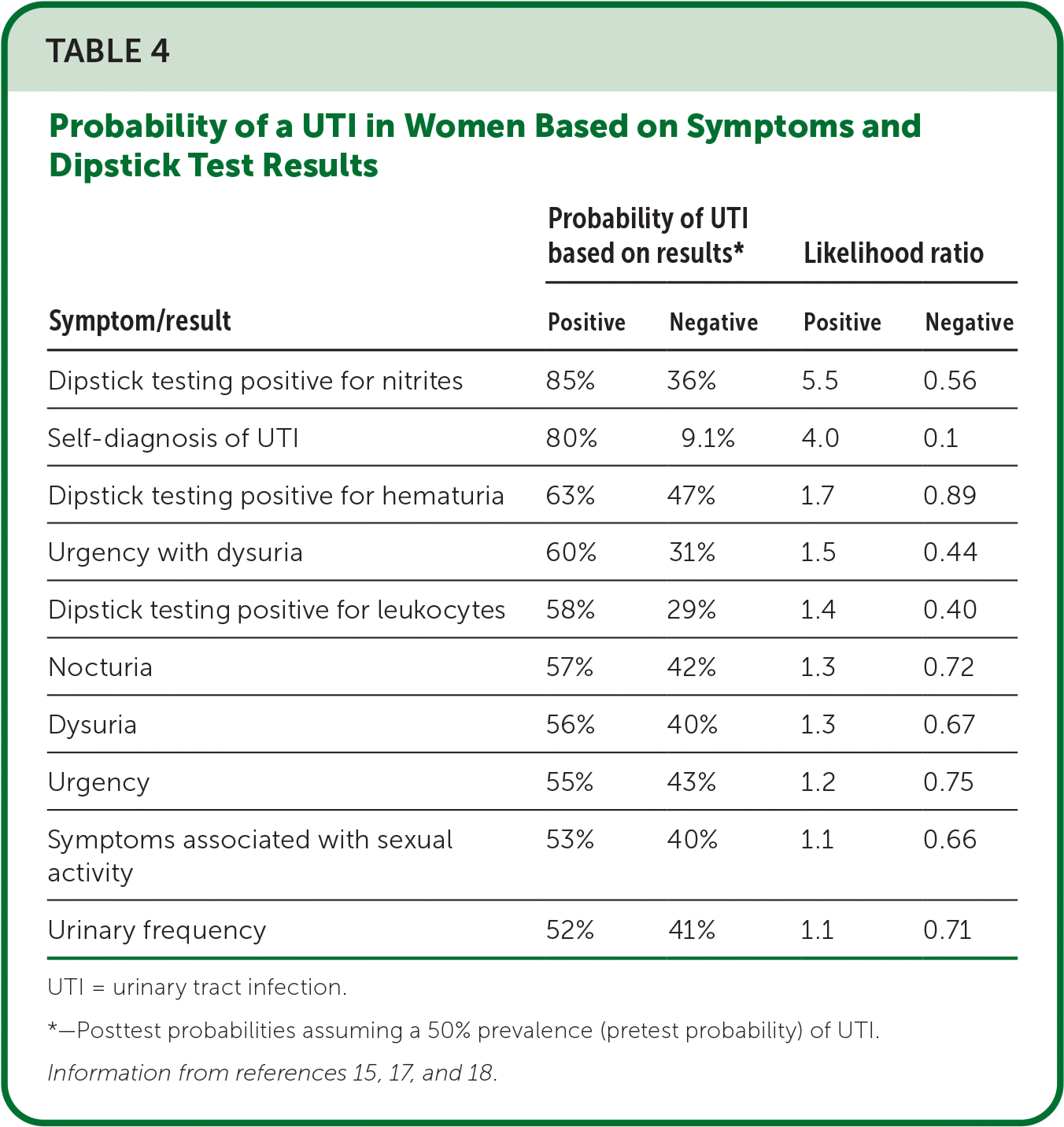
| Symptom/result | Probability of UTI based on results* | Likelihood ratio | ||
|---|---|---|---|---|
| Positive | Negative | Positive | Negative | |
| Dipstick testing positive for nitrites | 85% | 36% | 5.5 | 0.56 |
| Self-diagnosis of UTI | 80% | 9.1% | 4.0 | 0.1 |
| Dipstick testing positive for hematuria | 63% | 47% | 1.7 | 0.89 |
| Urgency with dysuria | 60% | 31% | 1.5 | 0.44 |
| Dipstick testing positive for leukocytes | 58% | 29% | 1.4 | 0.40 |
| Nocturia | 57% | 42% | 1.3 | 0.72 |
| Dysuria | 56% | 40% | 1.3 | 0.67 |
| Urgency | 55% | 43% | 1.2 | 0.75 |
| Symptoms associated with sexual activity | 53% | 40% | 1.1 | 0.66 |
| Urinary frequency | 52% | 41% | 1.1 | 0.71 |
UTI = urinary tract infection.
*—Posttest probabilities assuming a 50% prevalence (pretest probability) of UTI.
APPROACH TO THE PATIENT
- No single clinical feature is accurate enough to diagnose or exclude a UTI.14,15,17,18,20
- If a woman believes she has a UTI and reports typical symptoms without vaginal discharge, there is a high likelihood of UTI.14,17,18 In the absence of signs and symptoms of pyelonephritis or systemic illness (e.g., fever, chills, fatigue, nausea, vomiting, flank pain, costovertebral angle tenderness), the diagnosis can be made without an in-person examination or urinalysis.13,14,16–19,21
- In women with a less clear presentation, the diagnosis should be made during an in-person examination aided by a dipstick urinalysis.13,14,16–19,21
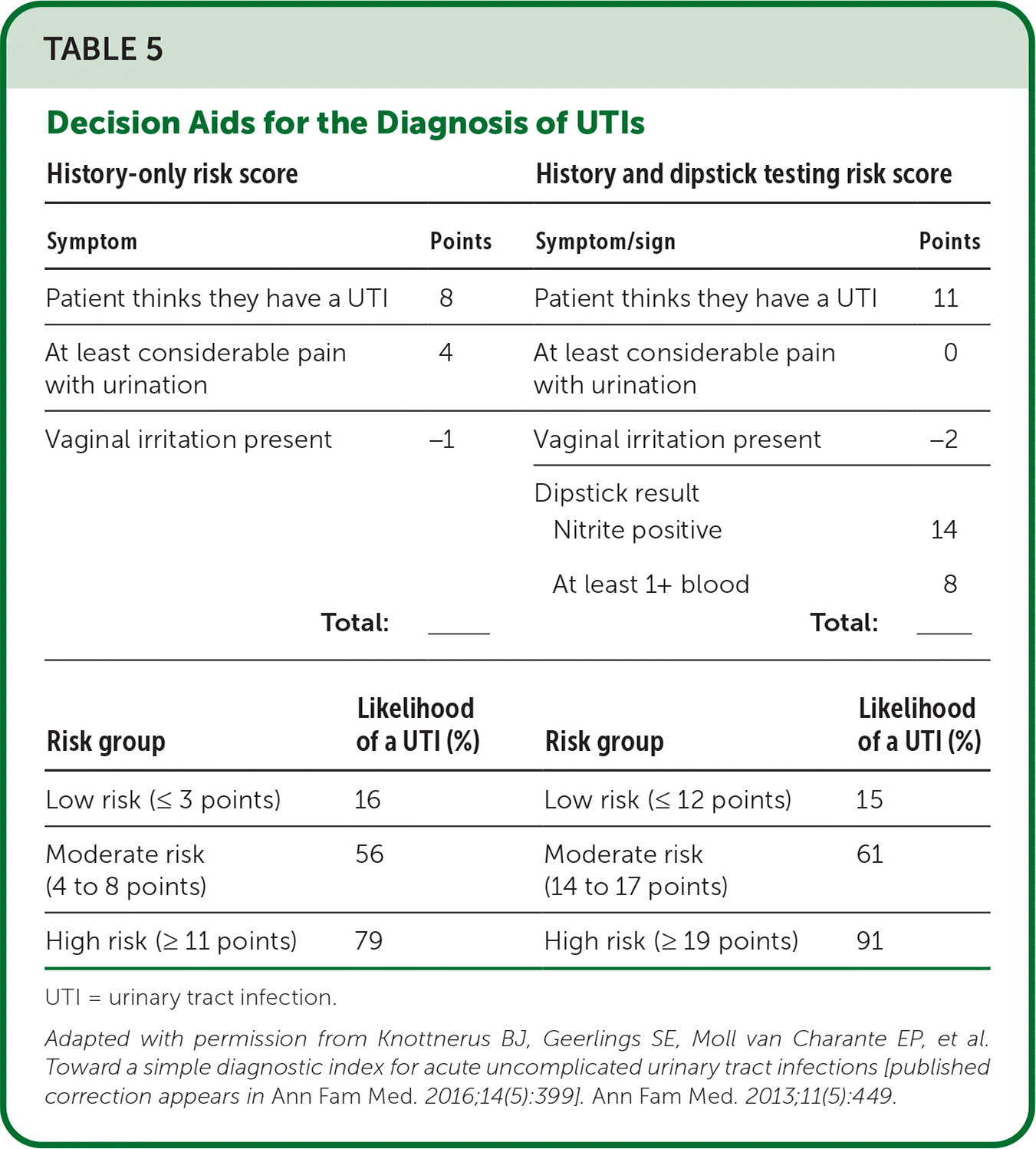
- Clinical decision aids that integrate clinical findings with urine findings can help guide management19,22 (Table 519 ).
- Most guidelines recommend urine culture with susceptibility testing only in women younger than 65 years of age with recurrent UTIs (i.e., two or more UTIs in the past six months or three or more UTIs in the past year), treatment failure with first-choice antibiotics, history of resistant urinary isolates, or atypical presentation.5–7,23–25
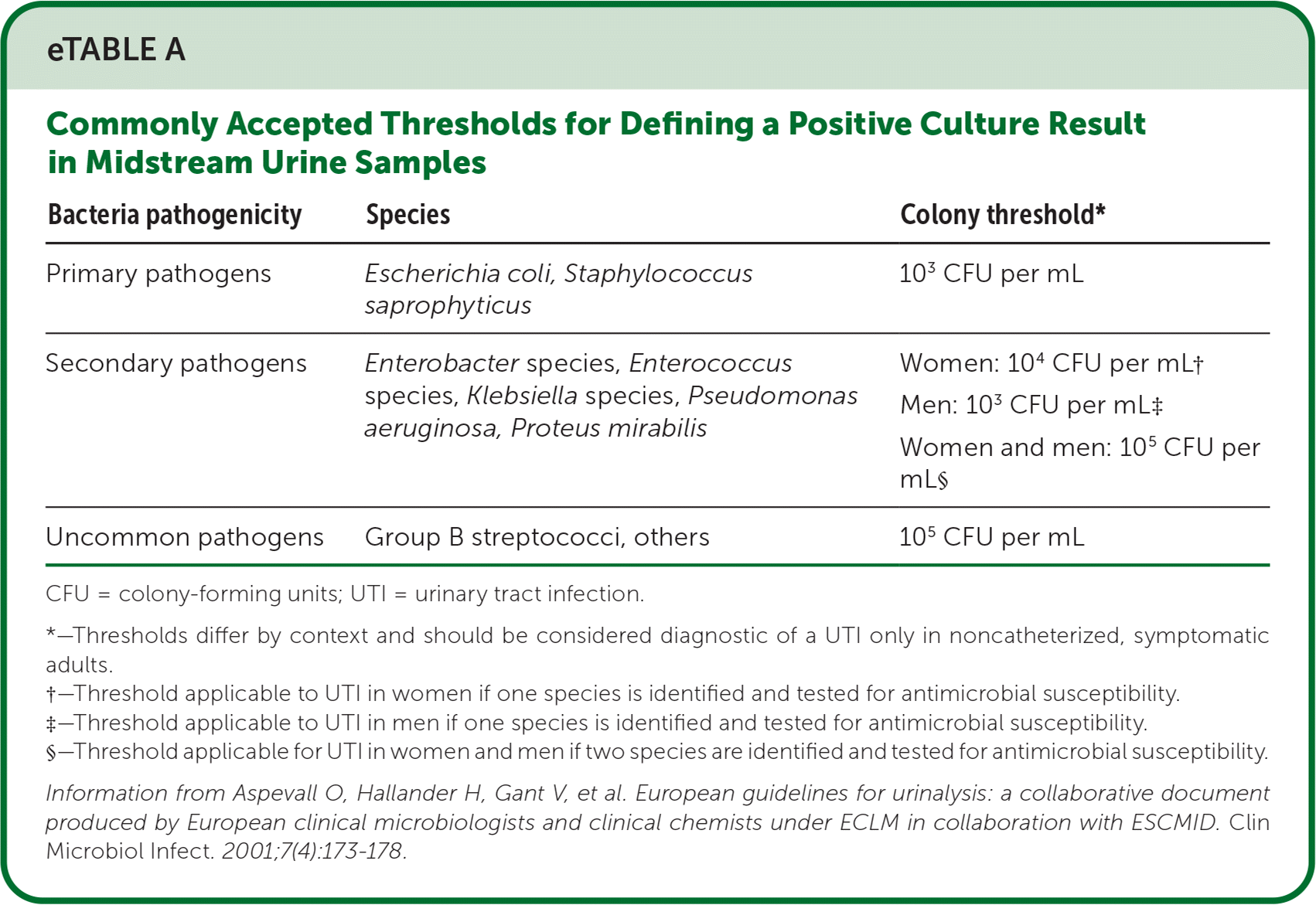
- Thresholds for positive urine culture results are listed in eTable A.
TABLE 5. Decision Aids for the Diagnosis of UTIs
| History-only risk score | History and dipstick testing risk score | ||
|---|---|---|---|
| Symptom | Points | Symptom/sign | Points |
| Patient thinks they have a UTI | 8 | Patient thinks they have a UTI | 11 |
| At least considerable pain with urination | 4 | At least considerable pain with urination | 0 |
| Vaginal irritation present | −1 | Vaginal irritation present | −2 |
| Dipstick result | |||
| Nitrite positive | 14 | ||
| At least 1+ blood | 8 | ||
| Total: ______ | Total: ______ | ||
| Risk group | Likelihood of a UTI (%) | Risk group | Likelihood of a UTI (%) |
| Low risk (≤ 3 points) | 16 | Low risk (≤ 12 points) | 15 |
| Moderate risk (4 to 8 points) | 56 | Moderate risk (14 to 17 points) | 61 |
| High risk (≥ 11 points) | 79 | High risk (≥ 19 points) | 91 |
UTI = urinary tract infection.
Adapted with permission from Knottnerus BJ, Geerlings SE, Moll van Charante EP, et al. Toward a simple diagnostic index for acute uncomplicated urinary tract infections [published correction appears in Ann Fam Med. 2016;14(5):399]. Ann Fam Med. 2013;11(5):449.
eTABLE A Commonly Accepted Thresholds for Defining a Positive Culture Result in Midstream Urine Samples
| Bacteria pathogenicity | Species | Colony threshold* |
|---|---|---|
| Primary pathogens | Escherichia coli, Staphylococcus saprophyticus | 103 CFU per mL |
| Secondary pathogens | Enterobacter species, Enterococcus species, Klebsiella species, Pseudomonas aeruginosa, Proteus mirabilis | Women: 104 CFU per mL† Men: 103 CFU per mL‡ Women and men: 105 CFU per mL§ |
| Uncommon pathogens | Group B streptococci, others | 105 CFU per mL |
CFU = colony-forming units; UTI = urinary tract infection.
*—Thresholds differ by context and should be considered diagnostic of a UTI only in noncatheterized, symptomatic adults.
†—Threshold applicable to UTI in women if one species is identified and tested for antimicrobial susceptibility.
‡—Threshold applicable to UTI in men if one species is identified and tested for antimicrobial susceptibility.
§—Threshold applicable for UTI in women and men if two species are identified and tested for antimicrobial susceptibility.
Information from Aspevall O, Hallander H, Gant V, et al. European guidelines for urinalysis: a collaborative document produced by European clinical microbiologists and clinical chemists under ECLM in collaboration with ESCMID. Clin Microbiol Infect. 2001;7(4):173–178.
Treatment
NONANTIBIOTICS
- Treatment failures are increasing due to rising rates of antimicrobial resistance; therefore, alternatives to immediate antibiotics may be considered using patient-centered decision-making.10
- Women with no signs of pyelonephritis or complicated infection who do not want to take antibiotics can be prescribed a backup antibiotic to be filled if symptoms do not improve within 48 to 72 hours or worsen at any time.23,26–28
- Women should be advised to drink at least 1.5 L of fluids daily and use acetaminophen or nonsteroidal anti-inflammatory drugs for symptomatic relief.5,6,23,26
- Without antibiotics, women have a higher risk of pyelonephritis, although its overall incidence is low (1.43% without and 0.46% with antibiotics; number needed to treat to avoid one pyelonephritis over 30 days = 105).29 [corrected]
- Relapse within two weeks or recurrent infections are equally likely in women treated initially with or without antibiotics.30
ANTIBIOTICS
- Immediate antibiotics should be considered in women who perceive a high burden of symptoms, have a longer symptom duration at presentation, and have risk factors for complications.5,6,23,26,31
- First-line antibiotics are presented in Table 6.5,6,23,26,31–35 The antibiotic choice should be guided by local resistance data and previous susceptibility results, where available.5,6,16, 23,26,32,36
- A 2010 guideline from the Infectious Diseases Society of America and the European Society for Microbiology and Infectious Diseases recommends extended-release nitrofurantoin for five days, fosfomycin in a single dose, and trimethoprim or trimethoprim/sulfamethoxazole for three days as first-line options. However, trimethoprim/sulfamethoxazole is recommended only if community resistance is less than 20%.32
- European and UK guidelines do not recommend trimethoprim/sulfamethoxazole due to concerns about adverse effects (rare but severe skin and neurologic manifestations), allergy, and increasing resistance in many communities. European and UK guidelines also include pivmecillinam as a first-line antibiotic for uncomplicated UTIs.5,6,23,26,33,34
- Fluoroquinolones are effective in treating uncomplicated UTIs but should be avoided as first-line therapy because of the risk of serious adverse effects and increasing bacterial resistance.5,6,23,26,32–34,37,38
- If no susceptibility results are available, beta-lactam antibiotics should also be avoided because they are a less effective empiric treatment.35
TABLE 6. First-Line Antibiotics for Uncomplicated Urinary Tract Infections in Women
| Antibiotic | Dosage | Cost (generic)* |
|---|---|---|
| Trimethoprim/sulfamethoxazole† | 160/800 mg twice daily for three days | $5 |
| Nitrofurantoin (extended release)‡ | 100 mg twice daily for five days | $15 |
| Trimethoprim† | 200 mg twice daily for three days | $15 |
| Fosfomycin | Single 3-g dose | $30 |
| Pivmecillinam | 400 mg three times daily for three days | — |
*—Estimated lowest GoodRx price for a treatment course. Actual cost will vary with insurance and by region. Information obtained at https://www.goodrx.com (accessed October 25, 2023; zip code: 66211).
†—Do not prescribe in the first trimester of pregnancy. Avoid if the local or regional resistance rates are greater than 20%.
‡—Avoid in the first and third trimesters of pregnancy.
Screening and Prevention
- Screening for asymptomatic bacteriuria should be avoided except in pregnant women.39,40
- Adequate fluid intake (at least 1.5 L per day), cranberry products, and methenamine hippurate are effective in reducing the risk of recurrent UTIs, whereas probiotics and D-mannose are not.41–47
- A systematic review of four randomized trials concluded that topical application of vaginal estrogens may reduce the risk of recurrent UTI in postmenopausal women.48
- Postcoital or long-term antibiotic prophylaxis effectively prevents recurrent UTIs (number needed to treat < 2); however, initiation and duration should be considered carefully because prophylaxis has an increased risk of adverse effects and antimicrobial resistance.49
- An evidence-based guideline recommends the following regimens for long-term prophylaxis: fosfomycin, 3 g every 10 days; nitrofurantoin, 50 mg or 100 mg once daily; or trimethoprim, 100 mg once daily, for three to six months or after sexual intercourse.24,25
Other Populations
MEN
- Uncomplicated UTI in men (or people with male anatomy) should be suspected in otherwise healthy men with typical symptoms (e.g., acute dysuria, frequency, urgency, nocturia) and no signs of systemic illness.50
- Rectal, pelvic, or suprapubic pain and a tender prostate on digital rectal examination suggest acute prostatitis, whereas purulent urethral discharge or multiple or new sex partners suggest acute urethritis.51–53
- The evidence for the optimal diagnostic workup and the type and duration of antibiotic treatment in men with suspected uncomplicated UTI is limited and primarily based on expert opinion.54
- A urine culture with susceptibility testing should always be performed in men to confirm the diagnosis and adjust the choice of antibiotic once results become available.5,52
- First-line antibiotics for uncomplicated UTI in men include trimethoprim, 200 mg; trimethoprim/sulfamethoxazole, 160/800 mg; and extended-release nitrofurantoin, 100 mg, twice daily.6,26,52
- A randomized trial concluded that a seven-day course of an oral antibiotic is as effective as a longer course in afebrile men with an uncomplicated UTI.55
- The diagnostic approach and treatment options for men with suspected urethritis, prostatitis, or pyelonephritis differ from those for men with suspected uncomplicated UTIs. Those topics are covered in previous American Family Physician articles.56–58
OLDER PEOPLE
- In nonfrail women and men 65 years and older who have no relevant comorbidities and present with typical clinical features of an uncomplicated UTI, the diagnostic workup does not differ significantly from that used for younger patients.23,59,60
- A urine culture with susceptibility testing should always be performed in older adults to confirm the diagnosis and adjust the choice of antibiotic once the results become available.52,59,60 First-line empiric antibiotics are the same as the medications that are recommended for younger people.52,59,60
- Short courses of antibiotics (three to six days in women and seven days in men) are likely as effective as longer courses in older adults.55,61
This article updates previous articles on this topic by Colgan and Williams4; Mehnert-Kay62; and Orenstein and Wong.63
Data Sources: This article is based on literature searches in Essential Evidence Plus, the Cochrane database, and PubMed using the Clinical Queries database for the term urinary tract infection. Studies that used gender as patient categories did not define explicitly how these categories were assigned, but they were judged to be essential and, therefore, included in this review. Search dates: August 14, 2023, and November 28, 2023.
Editor's Note: Dr. Ebell is deputy editor for evidence-based medicine for AFP.


