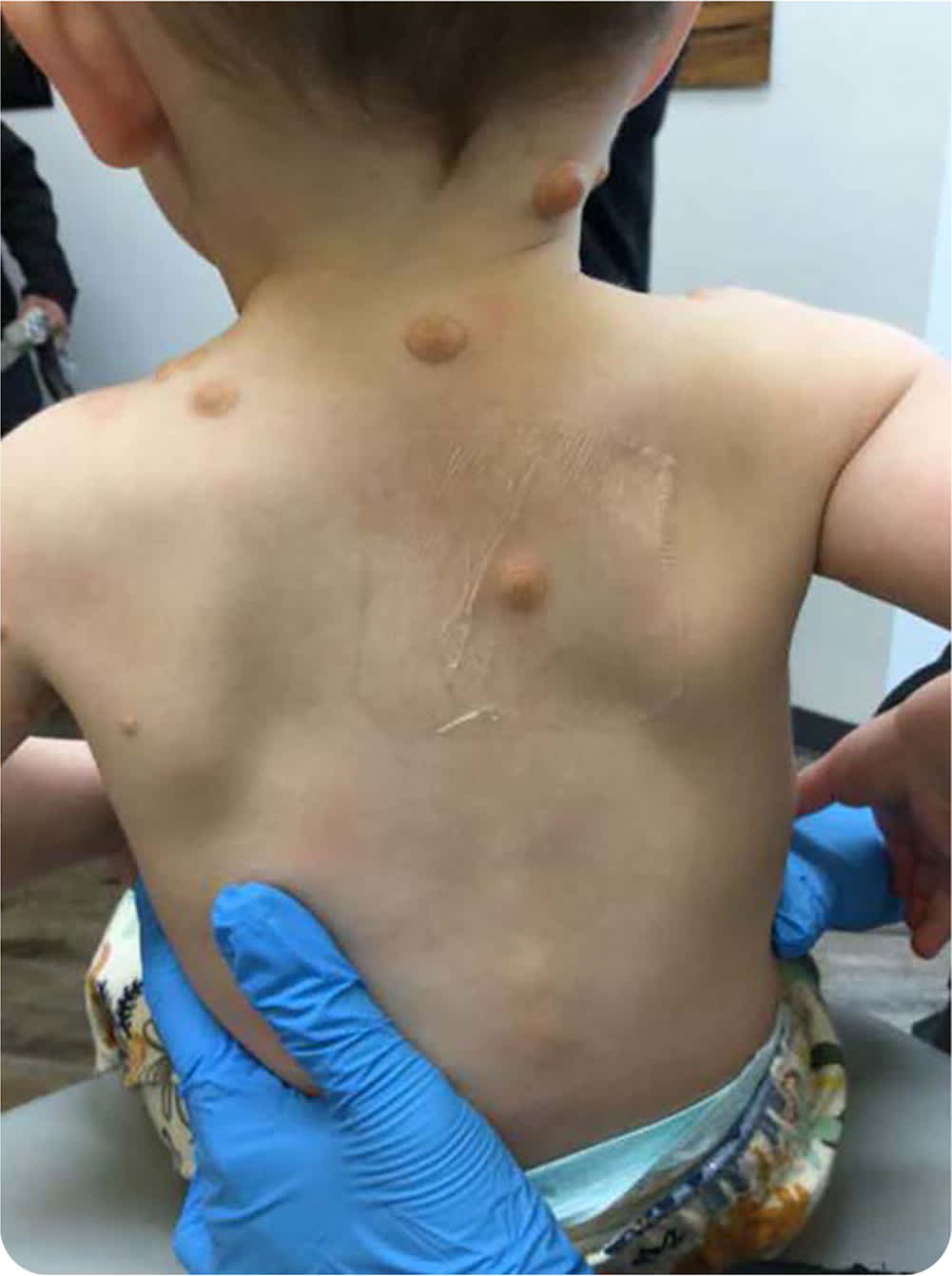
A 15-month-old infant presented with yellowish papules and nodules scattered on his trunk, back, scalp, and eyelids (Figure 1). The asymptomatic lesions first appeared at three months of age. Since then, they have enlarged and changed from dark red to yellowish-orange. Histological examination of a punch biopsy specimen from the center of a plaque revealed aggregates of histiocytes, Touton giant cells, and lymphocytes in the dermis.
FIGURE 1
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
- A. Cutaneous mastocytosis.
- B. Eruptive xanthomas.
- C. Juvenile xanthogranulomas.
- D. Molluscum contagiosum.
Discussion
The answer is C: juvenile xanthogranulomas. This non-Langerhans cell histiocytosis is associated with asymptomatic, yellowish papules. Lesions appear in infancy or early childhood and often regress by early adolescence. They are usually solitary, but multiple lesions can occur. The most common locations are the head, neck, upper torso, and extremities.
Dermoscopy characteristically finds a “setting sun” appearance, an orange-yellow background with yellow globules, shiny white streaks, and irregular vascular structures. Histopathology is characterized by dermal aggregates of histiocytes with scattered eosinophils, lymphocytes, and foam cells. Touton giant cells, which are multinucleated and comprise fused epithelioid macrophages surrounded by foamy cytoplasm commonly found in lipid-laden areas, are also characteristic.1,2
In the case of an asymptomatic solitary juvenile xanthogranuloma, a full-body skin examination is recommended, followed by monitoring to confirm spontaneous involution of the lesion. In patients with multiple xanthogranulomas, further workup is indicated, including abdominal ultrasonography to rule out hepatic xanthogranulomas (especially if the patient has hepatomegaly or jaundice) and ophthalmic examination to rule out ocular involvement.3
Cutaneous mastocytosis presents as yellow to brown macules, papules, or both, located on the trunk and extremities. Lesions most commonly appear during the first two years of life. Rubbing or scratching of lesions can result in the pathognomonic swollen or flushed skin, known as Darier sign. The three subtypes of cutaneous mastocytosis are diffuse cutaneous mastocytosis, solitary mastocytoma, and maculopapular (urticaria pigmentosa), which is the most common subtype.4,5
Eruptive xanthomas present as acute development of small, grouped, red or yellow papules. Lesions are commonly found on the extensor surfaces of extremities, trunk, and buttocks. Early lesions may have a surrounding erythematous ring and associated pruritus and tenderness. Risk factors for this condition include hypertriglyceridemia, hypercholesterolemia, diabetes mellitus, excessive alcohol intake, obesity, and familial lipoprotein lipase deficiency.6
Molluscum contagiosum is an infection caused by a pox-virus that most commonly affects infants and children. It appears two to six weeks after skin contact with an infected individual. It presents as a singular or multiple dome-shaped papules with a central umbilication. The papules are the same color as the surrounding skin and can occur on any part of the body except the palms and soles.7 Dermoscopy identifies multilobulated, ovoid areas that are white to yellow in the center and surrounded by a crown of blood vessels. Histology is not usually indicated for diagnosis.8 History of day care, school, or sports team outbreaks may be helpful in diagnosis.
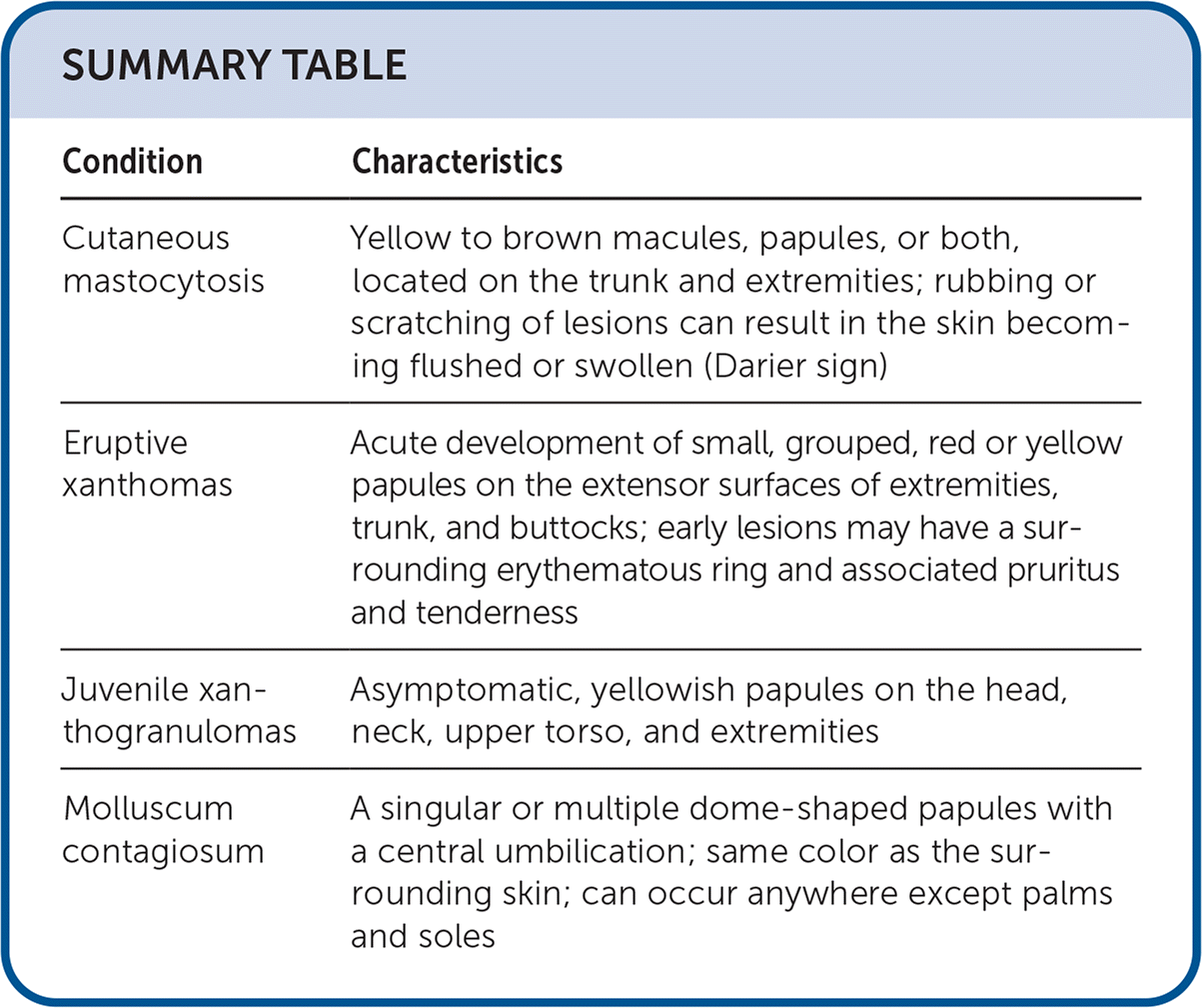
SUMMARY TABLE
| Condition | Characteristics |
|---|---|
| Cutaneous mastocytosis | Yellow to brown macules, papules, or both, located on the trunk and extremities; rubbing or scratching of lesions can result in the skin becoming flushed or swollen (Darier sign) |
| Eruptive xanthomas | Acute development of small, grouped, red or yellow papules on the extensor surfaces of extremities, trunk, and buttocks; early lesions may have a surrounding erythematous ring and associated pruritus and tenderness |
| Juvenile xanthogranulomas | Asymptomatic, yellowish papules on the head, neck, upper torso, and extremities |
| Molluscum contagiosum | A singular or multiple dome-shaped papules with a central umbilication; same color as the surrounding skin; can occur anywhere except palms and soles |

