A 64-year-old woman presented with an enlarging lesion on the back of her right calf. She initially noted a small, raised, white area 2 to 3 months earlier that progressively enlarged. The lesion was not painful or pruritic. The patient had no other skin lesions or history of trauma to the area. Treatment had not been attempted, including nonprescription medications. She had a history of hypertension.
Physical examination revealed a dome-shaped lesion that was 1 cm in diameter and had central hyperkeratosis (Figure 1).
FIGURE 1
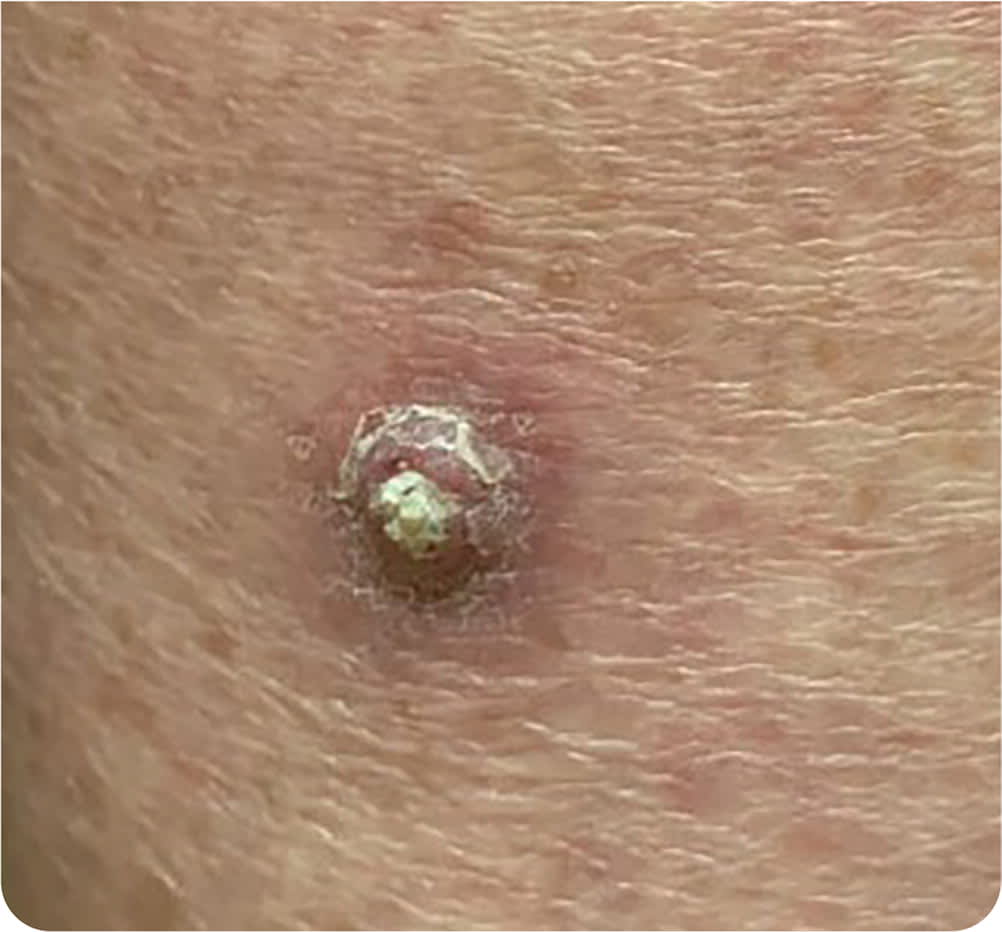
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
- A. Amelanotic melanoma.
- B. Keratoacanthoma.
- C. Nodular basal cell carcinoma.
- D. Prurigo nodularis.
Discussion
The answer is B: keratoacanthoma. This is an unpredictable skin tumor that may behave similarly to a squamous cell carcinoma. Keratoacanthomas typically present as a solitary, rapidly growing nodular lesion, often with central hyperkeratosis, on sun-exposed areas in older adults. The mean age at diagnosis is 64 years. Keratoacanthomas often evolve in the three stages of proliferation, maturation, and spontaneous resolution, typically over 4 to 6 months.1 Risk factors for development of keratoacanthomas include ultraviolet light exposure and skin trauma.2
There is some disagreement about the prognosis and treatment of keratoacanthomas. Some lesions behave as a cancer, similar to squamous cell carcinoma, whereas others progress like benign skin lesions.3 Treatment typically includes excision or Mohs surgery, depending on the size and location of the lesion. Alternative treatments including topical fluorouracil or imiquimod and intralesional fluorouracil have been proposed.4
Amelanotic melanoma is a rare subtype of melanoma characterized by absence of pigment, making its diagnosis more challenging. These lesions typically occur on sun-exposed areas and can display rapid growth. The condition has been reported in all melanoma subtypes, including superficial spreading, nodular, acral-lentiginous, and lentigo melanoma.5 Due to its nonspecific appearance, which can be the same color as the surrounding skin or erythematous, a low threshold for biopsy is recommended for any skin lesion that does not resolve following 1 month of appropriate treatment. The addition of EFG (elevated, firm, growing) to the classic ABCDE (asymmetry, border, color, diameter, evolving) criteria for melanoma may enhance detection.6
Basal cell carcinoma is the most common form of cancer and typically develops on sun-exposed areas. The nodular form typically presents as a well-defined, pearly papule with rolled borders and telangiectasia.7 Treatment is based on patient and lesion characteristics and may include excision, electrodesiccation and curettage, topical fluorouracil, or radiation therapy.8
Prurigo nodularis is a chronic skin condition that typically presents with intensely pruritic nodules, often located on the extremities and trunk. Lesions vary in size from a few millimeters to 2 cm in diameter. Lesions are commonly associated with excoriation and crusting.9 Diagnosis is clinical, although biopsy is often performed for confirmation. Treatment focuses on minimizing pruritus to stop scratching and allow for nodule resolution and healing.10
SUMMARY TABLE

| Condition | Characteristics |
|---|---|
| Amelanotic melanoma | Lesions that are erythematous or the same color as surrounding skin, with variable appearance and rapid growth; occurs in sun-exposed areas |
| Keratoacanthoma | Solitary, rapidly growing nodule with central hyperkeratosis on sun-exposed areas in older adults; often the period of rapid growth is followed by spontaneous resolution |
| Nodular basal cell carcinoma | Well-defined, pearly papule occurring on sun-exposed areas in older adults; nodule has rolled borders and telangiectasias |
| Prurigo nodularis | Intensely pruritic nodules, often located on the extremities and trunk; associated with excoriation and crusting |

