The aging demographic presents a significant challenge and opportunity for health care systems worldwide.1 The number of people in the United States 65 years and older is projected to reach approximately 95 million by 2060.2 Current health care models often operate in silos, lacking continuity and integration.3 This is particularly problematic for the growing older population with multimorbidity.4,5
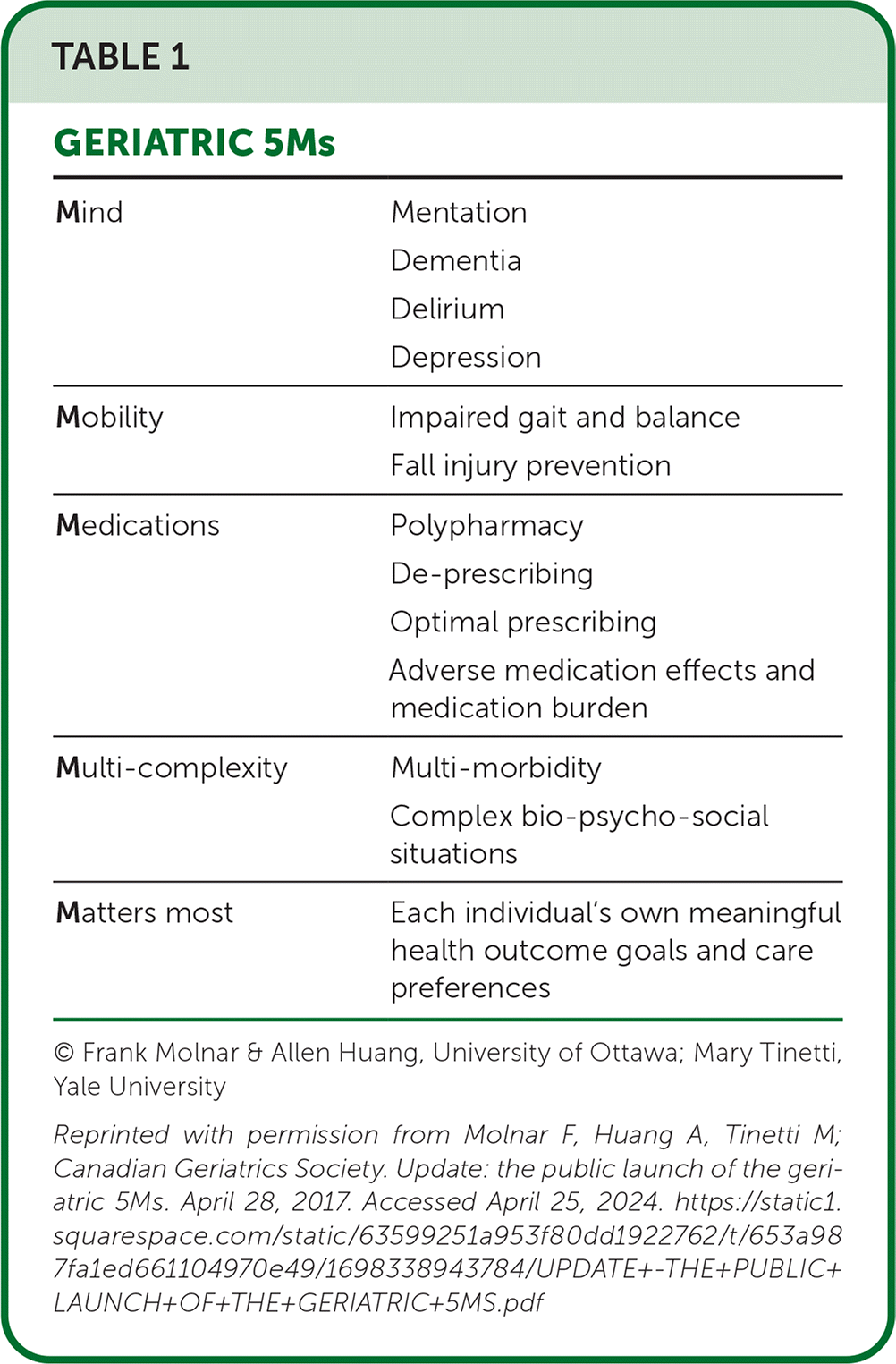
The Geriatric 5Ms framework includes five areas of focus: mind/mentation, mobility, medications, multicomplexity, and what matters most (Table 1).6 It offers a comprehensive approach to the care of older adults and emphasizes patient-centered strategies and interdisciplinary coordination.4,5 The framework has been shown to improve outcomes for older adults, reduce low-quality services, and increase the use of cost-effective services.7
TABLE 1. GERIATRIC 5Ms
| Mind | Mentation |
| Dementia | |
| Delirium | |
| Depression | |
| Mobility | Impaired gait and balance |
| Fall injury prevention | |
| Medications | Polypharmacy |
| De-prescribing | |
| Optimal prescribing | |
| Adverse medication effects and medication burden | |
| Multi-complexity | Multi-morbidity |
| Complex bio-psycho-social situations | |
| Matters most | Each individual's own meaningful health outcome goals and care preferences |
© Frank Molnar & Allen Huang, University of Ottawa; Mary Tinetti, Yale University
Reprinted with permission from Molnar F, Huang A, Tinetti M; Canadian Geriatrics Society. Update: the public launch of the geriatric 5Ms. April 28, 2017. Accessed April 25, 2024. https://static1.squarespace.com/static/63599251a953f80dd1922762/t/653a987fa1ed661104970e49/1698338943784/UPDATE+-THE+PUBLIC+LAUNCH+OF+THE+GERIATRIC+5MS.pdf
Case Presentation
An 80-year-old artist with hypertension, type 2 diabetes mellitus, hyperlipidemia, major depressive disorder, mild cognitive impairment, and urinary incontinence resides independently and recently experienced a fall while visiting her daughter. This incident has heightened her fear of future falls and has affected her cherished daily walks and psychological well-being. The recent loss of her husband has compounded her mental health issues. This narrative underscores the importance of an integrated approach to the care of older adults that should address the physical, emotional, and social aspects of health.
Mind: Cognitive and Emotional Well-Being
The loss of her husband, coupled with her fall, may have exacerbated the patient's depression and cognitive decline. Dementia, delirium, and depression are often interlinked8,9; therefore, the evaluation and management of these conditions are a pivotal aspect of her care. Older adults with depression are twice as likely to develop cognitive impairment.10 Various factors associated with aging, such as sensory limitations, social isolation, and losses, can contribute to depressive symptoms.11 Positive findings on an assessment may prompt a referral for counseling and/or management with pharmacologic and/or nonpharmacologic therapies.12 Modifying a patient's medications and addressing mobility issues can help treat depression and reduce the risk of developing cognitive impairment.13 Using physical activity and tailored interventions (e.g., social engagement) as nonpharmacologic therapy is an integral part of this strategy.14
Mobility: Falls
The patient's fall reflects how common falls are among older adults.11,15 Falling increases the risk of recurrent falls and hip fractures and causes significant financial burden.16–18 Assessing mobility is vital across health care settings. Although the patient did not sustain injuries, the psychological aftermath of the fall has led to a fear of falling again, which may reduce her mobility and worsen her mentation. This case highlights the need for assessing the risk of falls in older adults and incorporating strategies (e.g., physical therapy) to mitigate these fears. Mobility and physical activity are linked to prevention of depression, which further demonstrates the interconnectedness of mentation and mobility.19
Medications: Managing Polypharmacy
The prevalence of polypharmacy in older adults is a growing concern.20 Polypharmacy leads to adverse drug events, drug-drug interactions, nonadherence, functional decline, geriatric syndromes, and higher costs.14,21
For this patient, a comprehensive medication review is essential to identify any drugs that might contribute to her fall risk, cognitive issues, or urinary incontinence, underscoring the critical role of medication reconciliation in the care of older patients.22
This case exemplifies the multicomplexity in the care of older adults.4 Using multiple treatment guidelines increases the risk of polypharmacy, drug-drug interactions, a high treatment burden, and a failure to align care with the patient's priorities and values.23
The patient has several chronic conditions that necessitate a nuanced approach that balances disease management with her personal health care values.4,24 This approach should focus on modifiable aspects of care, addressing social determinants of health, and adapting patient education to her health literacy.25
What Matters Most: Person-Centered Care
Understanding and aligning care with what matters most to the patient is central to the age-friendly care model.3 This is especially essential in older adults with multiple chronic conditions who experience fragmented care and use of unnecessary health care that does not align with their goals and preferences.26 A collaborative approach that focuses on goals leads to improvements in health outcomes.27,28 Effective communication and facilitation of advance care planning and shared decision-making that is aligned with an individual's preferences ensure a person-centric approach that can significantly enhance quality of life.29 For this patient, that involves respecting her desire for independence and her passion for art while addressing her mental health needs. Strategies addressing symptom management and the trajectory of disease and goals of care can positively affect care for older adults with impaired cognition.26,30
Conclusion
This patient's case illustrates the complexities inherent in providing holistic care to older adults. The Geriatric 5Ms framework offers a comprehensive lens through which to view and address these complexities. By focusing on the mind, mobility, medications, multicomplexity, and what matters most, physicians can enhance the quality of life for older adults and ensure a more integrated and effective approach to geriatric care.

