A psychodermatologic disorder is a condition that involves an interaction between the mind and the skin. Psychodermatologic disorders fall into three categories: psychophysiologic disorders, primary psychiatric disorders and secondary psychiatric disorders. Psychophysiologic disorders (e.g., psoriasis and eczema) are associated with skin problems that are not directly connected to the mind but that react to emotional states, such as stress. Primary psychiatric disorders involve psychiatric conditions that result in self-induced cutaneous manifestations, such as trichotillomania and delusions of parasitosis. Secondary psychiatric disorders are associated with disfiguring skin disorders. The disfigurement results in psychologic problems, such as decreased self-esteem, depression or social phobia. Most psychodermatologic disorders can be treated with anxiety-decreasing techniques or, in extreme cases, psychotropic medications.
Psychodermatology, or psychocutaneous medicine, focuses on the boundary between psychiatry and dermatology. Understanding the psychosocial and occupational context of skin diseases is critical to the optimal management of psychodermatologic disorders.
The management of psychodermatologic disorders requires evaluation of the skin manifestation and the social, familial and occupational issues underlying the problem. Once the disorder has been diagnosed, management requires a dual approach, addressing both dermatologic and psychologic aspects. Even with self-induced skin problems, supportive dermatologic care is needed to avoid secondary complications, such as infection, and to ensure that the patient feels supported. Patients with psychodermatologic disorders frequently resist referral to mental health professionals. Acceptance of psychiatric treatment or consultation may be enhanced through support from the family physician.
Management options include psychotropic medication, stress management courses and referral to a psychiatrist. Family physicians are well positioned to help patients with psychodermatologic disorders; these patients may be concerned about the stigma associated with psychiatrists, and family physicians are familiar with the use of psychotropic medications.
Classification
Psychodermatologic disorders can be broadly classified into three categories: psychophysiologic disorders, primary psychiatric disorders and secondary psychiatric disorders.1 The term “psychophysiologic disorder” refers to a skin disorder, such as eczema or psoriasis, that is worsened by emotional stress (Figure 1). “Primary psychiatric disorder” refers to a skin disorder such as trichotillomania, in which the primary problem is psychologic; the skin manifestations are self-induced. “Secondary psychiatric disorders” affect patients with significant psychologic problems that have a profoundly negative impact on their self-esteem and body image. Depression, humiliation, frustration and social phobia may develop as a consequence of a disfiguring skin disorder.2 Table 1 lists common diagnoses associated with the different categories of psychodermatologic disorders.
FIGURE 1.
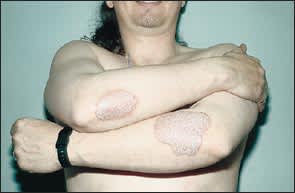
Psoriasis, like atopic dermatitis or other forms of eczema, is exacerbated by emotional stress in at least one half of patients.
Psychophysiologic Disorders
Psychophysiologic disorders are conditions that are frequently precipitated or exacerbated by emotional stress. Each of these conditions has “stress responders”and “non-stress responders,” depending on whether a patient's skin disease is or is not frequently and predictably exacerbated by stress. The proportion of stress responders depends on the dermatologic diagnosis involved, as illustrated in Table 2.3
TABLE 1 Diagnoses Associated with Psychodermatologic Disorders
| Major categories | Examples |
|---|---|
| Psychophysiologic disorders | Acne |
| Alopecia areata | |
| Atopic dermatitis | |
| Psoriasis | |
| Psychogenic purpura | |
| Rosacea | |
| Seborrheic dermatitis | |
| Urticaria (hives) | |
| Primary psychiatric disorders | Bromosiderophobia |
| Delusions of parasitosis | |
| Dysmorphophobia | |
| Factitial dermatitis | |
| Neurotic excoriations | |
| Trichotillomania | |
| Secondary psychiatric disorders | Alopecia areata |
| Cystic acne | |
| Hemangiomas | |
| Ichthyosis | |
| Kaposi's sarcoma | |
| Psoriasis | |
| Vitiligo |
In patients with treatment-responsive skin conditions such as eczema, psoriasis and acne, the issue of stress may not be important.4 However, when physicians are faced with disease recalcitrant to treatment, patients should be asked whether psychologic, social or occupational stress might be contributing to the skin disorder.
Emotional stress may exacerbate many chronic dermatoses and can initiate a vicious cycle referred to as the “itch-scratch cycle”; therefore, treatment of recalcitrant patients with chronic dermatoses may be difficult without addressing stress as an exacerbating factor.5 Patients often are embarrassed about discussing psychologic issues, especially if they feel hurried. Stress management classes, relaxation techniques, music or exercise may benefit these patients. If a specific psychosocial or occupational issue exists, therapy or counseling can help.
When the patient's stress or tension is intense enough to warrant consideration of an anti-anxiety medication, two general types are available. Benzodiazepines, which can be used on an as-needed basis, provide relatively quick relief from anxiety, stress and tension.6 For treatment of chronic anxiety, selective serotonin reuptake inhibitors (SSRIs) are safe and effective.
Other options for the treatment of chronic stress include nonsedating and nonaddictive anti-anxiety agents such as buspirone (Buspar). If a patient's anxiety disorder warrants psychiatric referral, the referral should be discussed with the patient in a supportive and diplomatic way so that the patient is able to accept the referral as an adjunct to continuing dermatologic therapy.
Primary Psychiatric Disorders
Primary psychiatric disorders are encountered less often than psychophysiologic disorders.
DELUSIONS OF PARASITOSIS
Delusions of parasitosis belongs to a group of disorders called “monosymptomatic hypochondriacal psychosis.” Patients with the latter disorder present with isolated delusions regarding a skin complaint.6 Because the nature of the delusional disorder is truly isolated, these disorders are quite different from schizophrenia, which involves multiple functional deficits, including auditory hallucinations, lack of social skills and flat affect, in addition to delusional ideation.7
The most common form of monosymptomatic hypochondriacal psychosis encountered among patients with skin problems is called delusions of parasitosis.8 Patients with delusions of parasitosis firmly believe that their bodies are infested by some type of organism. Frequently, they have elaborate ideas about how these “organisms” mate, reproduce, move around in the skin and, sometimes, exit the skin. These patients often present with the “matchbox” sign, in which small bits of excoriated skin, debris or unrelated insects or insect parts are brought in matchboxes or other containers as “proof” of infestation (Figure 2).
The psychiatric differential diagnosis includes schizophrenia, psychotic depression, psychosis in patients with florid mania or drug-induced psychosis, and formication without delusion, in which the patient experiences crawling, biting and stinging sensations without believing that they are caused by organisms.6 Other organic causes such as withdrawal from cocaine, amphetamines or alcohol, vitamin B12 deficiency, multiple sclerosis, cerebrovascular disease or syphilis should also be considered. If any of these underlying causes are diagnosed, a separate diagnosis of delusions of parasitosis should not be made.9
The treatment of choice for delusions of parasitosis is an antipsychotic medication called pimozide (Orap). Pimozide is similar to haloperidol (Haldol) in chemical structure and potency, and has been shown to be uniquely effective in the treatment of this condition, especially in decreasing formication.10 This medication has been labeled by the U.S. Food and Drug Administration (FDA) for the treatment of Tourette's syndrome; its use in the treatment of delusions of parasitosis is off-label. The dosage of pimozide for treatment of delusions of parasitosis is much lower than that used for chronic schizophrenia. Pimozide therapy is generally started at the lowest possible dosage of one half of a 2-mg tablet (i.e., 1 mg) daily and increased by 1 mg per week.11 By the time the usual daily dosage of 4 to 6 mg (i.e., 2 to 3 tablets) is reached, most patients have experienced a decrease in crawling and biting sensations, as well as in the sensations of “organisms” moving in their skin. Optimal therapeutic effect may not occur for 6 to 8 weeks. During the treatment course, patients become less agitated.
FIGURE 2.

Delusions of parasitosis—the “matchbox sign.” Patients with delusions of parasitosis often try to bring specimens to the physician as proof that they have an infestation.
In younger patients, pimozide can be continued at the lowest effective dosage for several months and gradually tapered off without necessarily inviting the recurrence of symptoms. If the condition recurs, another course of therapy with pimozide can be instituted.11 In elderly patients, long-term maintenance with low dosages of pimozide (1 to 2 mg per day) is sometimes required. Tardive dyskinesias can occur, but with low-dose (6 mg per day or less) intermittent usage, the risk is lessened. In patients with cardiac arrhythmias, advanced age or dosages of more than 10 mg per day, serial electrocardiography is required.
As with other antipsychotic agents, extra-pyramidal side effects (i.e., pseudo-parkinsonian effects) may develop with the use of pimozide.12 Stiffness and restlessness respond to benztropine (Cogentin), in a dosage of 2 mg up to four times per day, as needed. Diphenhydramine (Benadryl), in a dosage of 25 mg up to three times per day as tolerated and needed, may be substituted.
The challenge in managing patients with delusions of parasitosis is in introducing the use of an antipsychotic medication without offending the patient. This step requires a delicate balance between the patient's right to informed consent and the goal of pursuing the most appropriate therapy. The authors recommend a sensitive, empathic and diplomatic approach. The medication should be presented as a “therapeutic trial,” and any contentious argument regarding the pathogenesis of the disorder or the mechanism of action of pimozide should be purposely avoided. Encouragement suggesting that pimozide may “help one focus less on the skin and more on enjoying life” may help. Because the FDA-labeled use of pimozide in the United States is for treatment of Tourette's syndrome and not psychosis, there is less stigma attached to this medication than other antipsychotic agents.
NEUROTIC EXCORIATIONS, FACTITIAL DERMATITIS AND SKIN LESIONS IN RESPONSE TO A DELUSIONAL BELIEF
The terms “neurotic excoriations” and “psychologic excoriations” are used when patients self-inflict excoriations (scratch marks) with their fingernails. Factitial dermatitis (dermatitis artefacta) generally refers to a condition in which the patient uses something more elaborate than the fingernails, such as burning cigarettes, chemicals or sharp instruments, to damage his or her own skin.13
FIGURE 3.
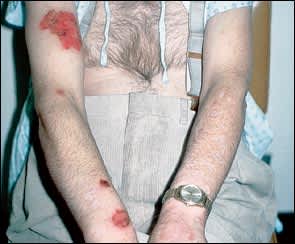
Neurotic excoriation. This man became severely depressed when a stroke paralyzed his right arm. He then used his functional arm to induce skin lesions.
The most common underlying psychopathologies are major depressive episodes, anxiety and obsessive-compulsive disorders. Rarely, patients excoriate their skin in response to delusional ideation; in such cases, the appropriate diagnosis would be psychosis. Patients with neurotic excoriations usually have depression or anxiety, whereas those with factitial dermatitis often have other psychiatric illnesses. Borderline personality disorder is just one of the more serious diagnoses associated with factitial dermatitis.
If the patient has underlying depression that results in neurotic excoriations, one anti-depressant frequently used by dermatologists is doxepin (Sinequan). Doxepin is a tricyclic antidepressant with one of the most powerful anti-itch and antihistaminic effects, as well as sedative/tranquilizing effects. Because many people with depression who excoriate their skin are agitated (i.e., have “agitated depression”), the sedative and tranquilizing effects of doxepin frequently prove to be therapeutic.14 Moreover, the profound antipruritic effect of this drug is an added benefit. Although these patients create their own skin lesions as they continue to pick at their skin, not allowing it to heal, the “itch-scratch cycle” may create intensely itchy patches that can benefit from the antipruritic effect of doxepin (Figures 3,4 and 5).
The use of doxepin requires the usual precautions taken with older tricyclic antidepressants. This includes carefully limiting the amount of medication that may be dispensed at one time to minimize the risk of suicide. A detailed description is beyond the space available in this article; however, it should be mentioned that if the patient is truly depressed, adequate dosages of antidepressants are required to prevent undertreatment of the patient. Elderly patients may respond to lower dosages. SSRIs may also be used.15
FIGURE 4.
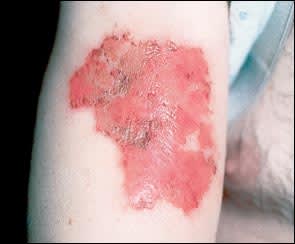
Neurotic excoriation. Self-induced skin lesions often have a bizarre appearance without evidence of primary skin disorder.
TRICHOTILLOMANIA
Trichotillomania, according to the dermatologic use of the word, is a condition in which a person pulls out his or her own hair. The psychiatric definition of trichotillomania requires the presence of “impulsivity.”16 However, using the less specific dermatologic definition, the physician once again must ascertain the nature of the underlying psychopathology to select the most appropriate treatment.
The most common underlying psychopathology is obsessive-compulsive behavior, whether or not it formally meets the criteria of the Diagnostic and Statistical Manual of Mental Disorders, 4th ed., for obsessive-compulsive disorder.17 The other possible underlying psychiatric diagnoses include simple habit disorder, reaction to situational stress, mental retardation, depression and anxiety, as well as extremely rare cases of delusion in which the patient pulls out his or her hair based on a delusional belief that something in the roots needs to be “dug out” so the hair can grow normally. This latter, rare condition is called “trichophobia.” The differential diagnosis of trichotillomania includes pseudopelade, alopecia areata, syphilis and tinea capitis.
Trichotillomania is one of the rare conditions in which pathologic examination of the skin can be diagnostic. The hair root undergoes a unique change called trichomalacia, which only occurs in patients with trichotillomania.18 Thus, if the patient continues to deny pulling his or her own hair, a skin biopsy can be helpful in determining the diagnosis.
FIGURE 5.
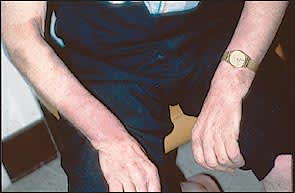
Neurotic excoriation. The patient shown in Figure 3 after successful treatment with an antidepressant. When the underlying psychopathology resolved, the patient stopped excoriating his skin.
As with other conditions, the treatment of trichotillomania is based on the nature of the underlying psychopathology. Because the most commonly encountered underlying psychopathogy is obsessive-compulsive tendency, medications such as fluoxetine (Prozac), paroxetine (Paxil), sertraline (Zoloft), fluvoxamine (Luvox) and clomipramine (Anafranil), in dosages appropriate for the treatment of obsessive-compulsive disorder, can be helpful in the pharmacologic management of trichotillomania.19 It should be noted that the anti–obsessive-compulsive dosage for any of these medications tends to be higher than the antidepressant dosage. The nonpharmacologic approach includes psychotherapy, which may be useful if the patient has a definable issue that can be discussed. Behavior therapy is another treatment modality.
Secondary Psychiatric Disorders
Although skin conditions are usually not life-threatening, because of their visibility they can be “life-ruining.” Persons with disfigurement frequently feel psychologically and socially devastated as a result (Figure 6). Moreover, persons with skin disorders have trouble getting jobs in which appearance is important.20 It is also well documented that persons with visible disfigurement face discrimination, especially if the condition is perceived to be contagious.21
FIGURE 6.
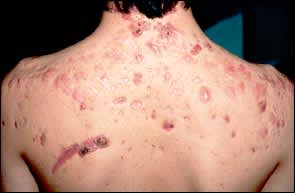
Psychologic impact of disfigurement. This student with treatment-resistant cystic acne became severely depressed and refused to go to school; he had been a top student before the onset of acne.
Even though many patients adjust to their skin disease, if the physician notes that the patient is experiencing significant distress it is important to explore this issue and decide whether referral to a mental health professional or dermatologic support group might help. If the depression, social phobia or secondary psychopathology is of significant intensity, referral to a psychiatrist may be warranted. Table 3 lists contact information for some dermatologic support groups.
TABLE 3 Contact Information for Dermatologic Support Groups
| National Psoriasis Foundation | |
| 6600 SW 92nd Ave., Suite 300 | |
| Portland, OR 97223 | |
| Ph: 503-244-7404 or 800-723-9166 | |
| Web:http://www.psoriasis.org | |
| National Alopecia Areata Foundation | |
| 710 “C” St., Suite 11 | |
| San Rafael, CA 94901 | |
| Ph: 415-456-4644 | |
| Web:http://www.alopeciaareata.com | |
| National Vitiligo Foundation | |
| P.O. Box 6337 | |
| 611 South Fleishel Ave. | |
| Tyler, TX 75701 | |
| Ph: 903-531-0074 | |
| Web:http://www.vitiligofoundation.org | |
| National Eczema Association for Science and Education | |
| 1220 SW Morrison, Suite 433 | |
| Portland, OR 97205 | |
| Ph: 503-228-4430 or 800-818-7546 | |
| Web:http://www.eczema-assn.org | |
| Obsessive-Compulsive Foundation | |
| 337 Notch Hill Rd. | |
| North Branford, CT 06471 | |
| Ph: 203-315-2190 | |
| Web:http://www.ocfoundation.org | |

