Speech and language delay in children is associated with increased difficulty with reading, writing, attention, and socialization. Although physicians should be alert to parental concerns and to whether children are meeting expected developmental milestones, there currently is insufficient evidence to recommend for or against routine use of formal screening instruments in primary care to detect speech and language delay. In children not meeting the expected milestones for speech and language, a comprehensive developmental evaluation is essential, because atypical language development can be a secondary characteristic of other physical and developmental problems that may first manifest as language problems. Types of primary speech and language delay include developmental speech and language delay, expressive language disorder, and receptive language disorder. Secondary speech and language delays are attributable to another condition such as hearing loss, intellectual disability, autism spectrum disorder, physical speech problems, or selective mutism. When speech and language delay is suspected, the primary care physician should discuss this concern with the parents and recommend referral to a speech-language pathologist and an audiologist. There is good evidence that speech-language therapy is helpful, particularly for children with expressive language disorder.
Definition of Speech and Language
Speech is the verbal production of language, whereas language is the conceptual processing of communication. Language includes receptive language (understanding) and expressive language (the ability to convey information, feelings, thoughts, and ideas). Language is commonly thought of in its spoken form, but may also include a visual form, such as American Sign Language.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
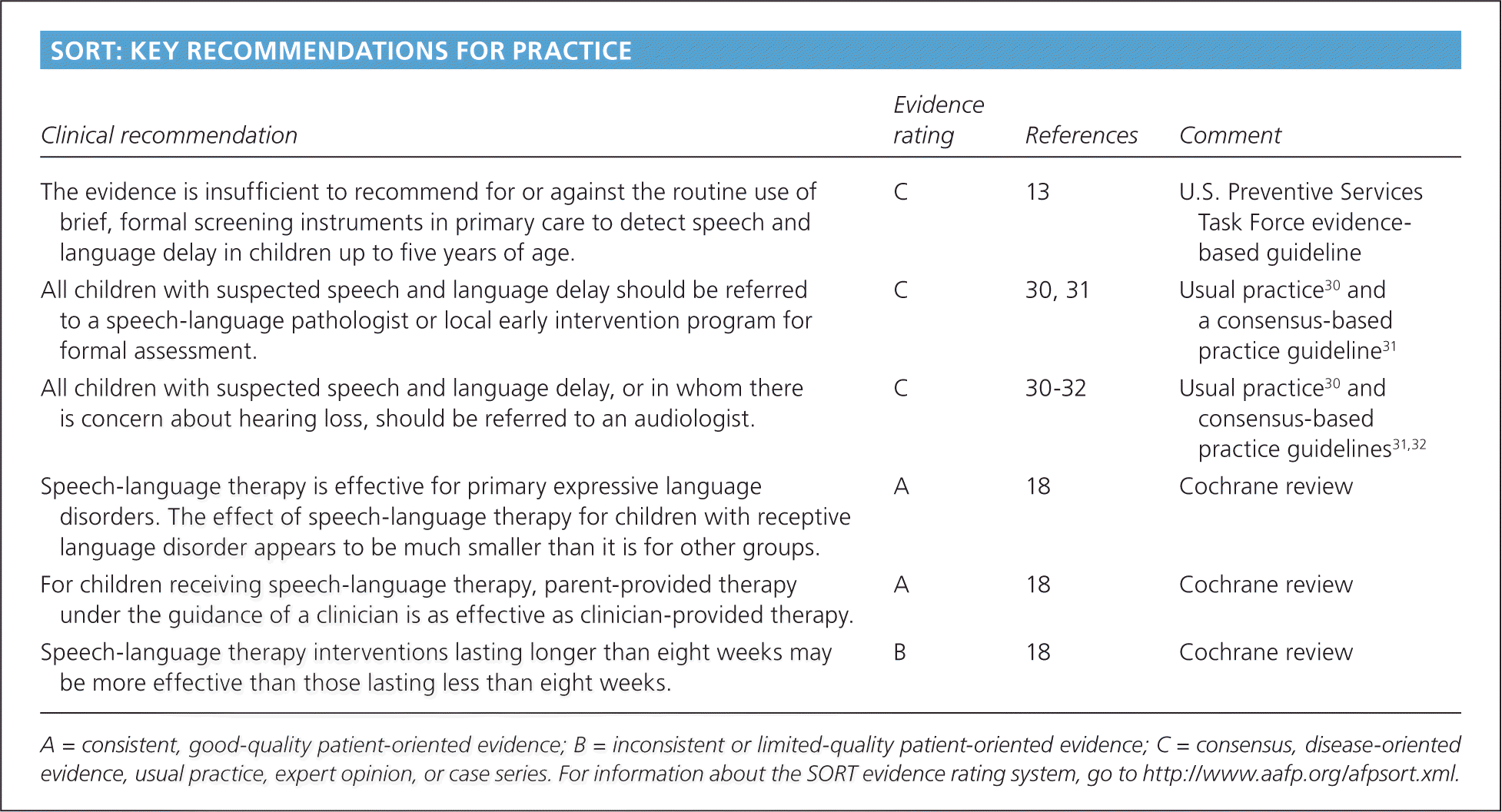
| Clinical recommendation | Evidence rating | References | Comment |
|---|---|---|---|
| The evidence is insufficient to recommend for or against the routine use of brief, formal screening instruments in primary care to detect speech and language delay in children up to five years of age. | C | 13 | U.S. Preventive Services Task Force evidence-based guideline |
| All children with suspected speech and language delay should be referred to a speech-language pathologist or local early intervention program for formal assessment. | C | 30, 31 | Usual practice30 and a consensus-based practice guideline31 |
| All children with suspected speech and language delay, or in whom there is concern about hearing loss, should be referred to an audiologist. | C | 30–32 | Usual practice30 and consensus-based practice guidelines31 ,32 |
| Speech-language therapy is effective for primary expressive language disorders. The effect of speech-language therapy for children with receptive language disorder appears to be much smaller than it is for other groups. | A | 18 | Cochrane review |
| For children receiving speech-language therapy, parent-provided therapy under the guidance of a clinician is as effective as clinician-provided therapy. | A | 18 | Cochrane review |
| Speech-language therapy interventions lasting longer than eight weeks may be more effective than those lasting less than eight weeks. | B | 18 | Cochrane review |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Prevalence and Prognosis
The reported prevalence of language delay in children two to seven years of age ranges from 2.3 to 19 percent.1–5 Severe speech and language disorders in young children can negatively affect later educational achievement, even after intensive intervention.6 Several studies have shown that children with speech and language problems at two and a half to five years of age have increased difficulty reading in the elementary school years.7–9 Children in whom speech and language impairments persist past five and a half years of age have an increased incidence of attention and social difficulties.10 Children with specific speech and language impairments at seven and a half to 13 years of age have been shown to have impaired writing skills, with marked deficits in spelling and punctuation compared with children without speech and language impairments.11 The likelihood of persistent difficulties for young children with speech and language problems appears to be directly related to the range of language functions that are impaired, with the best prognosis for children who have a developmental speech delay.12
Screening
The U.S. Preventive Services Task Force found that there was insufficient evidence to recommend for or against routine use of brief, formal screening instruments in primary care to detect speech and language delay in children up to five years of age. Specific groups of children known to be at higher-than-average risk of speech and language delay, such as those with hearing deficits or craniofacial abnormalities, were not included in this review. Studies of other risk factors for speech and language delay show inconsistent results, so the U.S. Preventive Services Task Force was unable to develop a list of specific risk factors to guide primary care physicians in selective screening. The most consistently reported risk factors were a family history of speech and language delay, male sex, prematurity, and low birth weight. Other risk factors that were reported less consistently included levels of parental education, childhood illness, late birth order, and larger family size.13
The physician should elicit any concerns that parents have about their child's speech and language. In addition to observing the child's speech in the clinic setting, the physician should ask the parents if this behavior is typical of that at home, at school, and in other social environments. The American Academy of Pediatrics publishes Bright Futures guidelines that include speech and language milestones to be covered at each well-child visit.14 A free PDF download of the pocket version and a PDA version that can be purchased are available at http://brightfutures.aap.org/3rd_Edition_Guidelines_and_Pocket_Guide.html. The Milcom Well-Child Record System, parts of which were reviewed and approved by the Society of Teachers of Family Medicine, includes age-appropriate screening questions for speech and language milestones, and is available for purchase at http://www.briggscorp.com.
Normal Development
Speech and language developmental milestones are noted in Table 1.14,15 It is important for the physician to have an understanding of these milestones to determine whether children have a delay in speech or language. Normal speech progresses through stages of cooing, babbling, words, and word combinations, whereas normal language progresses through stages of understanding and expressing more complex concepts. Development of proficiency in vocabulary and language use depends heavily on family and early school experiences. Families can aid their children's language development by telling stories, playing word games, reciting rhymes and songs, engaging in questions and conversation, and reading books together.14
Table 1. Developmental Milestones for Speech and Language in Children

| Age | Receptive | Expressive |
|---|---|---|
| 6 months | Turns to rattling sound* | |
| Turns to voice† | ||
| 9 months | — | |
| 12 months | Follows one-step command15 | |
| 15 months | — | |
| 18 months | Points to at least one body part | |
| 2 years | Points to two pictures* |
|
| Follows two-step command15 | ||
| 2.5 years | Points to six body parts* | |
| 3 years | — | |
| 4 years | — |
note: Except where otherwise cited, milestones are adapted from Bright Futures: Guidelines for Health Supervision of Infants, Children, and Adolescents.14
*—More than 90 percent of children pass this item.
†—50 to 90 percent of children pass this item.
The proportion of a child's speech that should be understandable to a stranger in the absence of any contextual cues increases with age. Milestones for this can be remembered by using the “rule of fours”: if the child's age in years is divided by four, the quotient is approximately equal to the amount of speech that should be understandable. Thus, a one-year-old should be understandable 25 percent of the time, a two-year-old 50 percent of the time, a three-year-old 75 percent of the time, and a four-year-old close to 100 percent of the time.15
BILINGUAL LANGUAGE LEARNING
Children growing up in a bilingual environment will typically have some degree of mixing of the two languages, which decreases with a growth in language development.16 These children usually become proficient in both languages by five years of age.17 Bilingual language learning does not typically necessitate services from a speech-language pathologist unless there is a difficulty in the primary language. Bilingual children should be referred based on the same criteria used for monolingual children.
Atypical Development
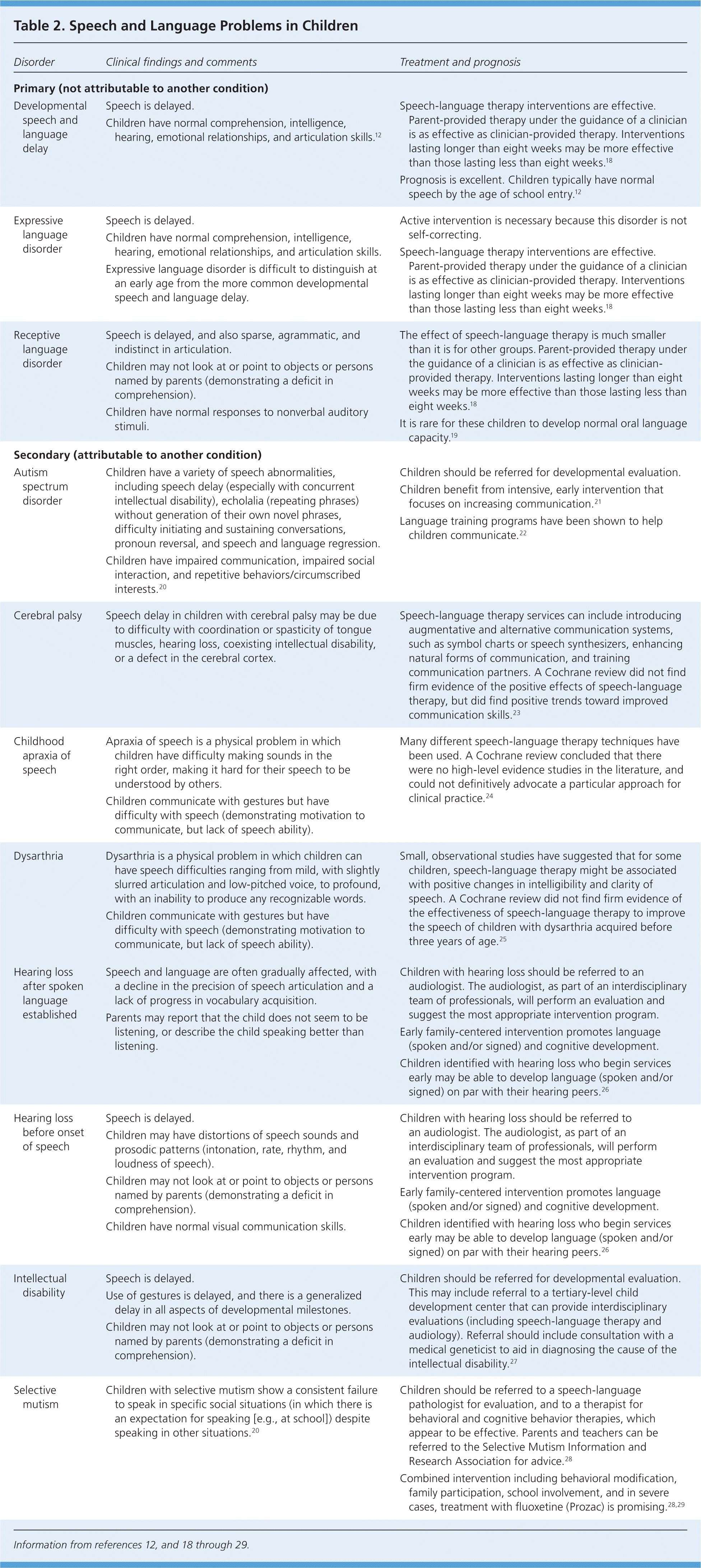
In children not meeting the expected developmental milestones for speech and language, a comprehensive developmental evaluation is essential. Atypical language development can be a secondary characteristic of other physical and developmental problems that may first manifest as language problems. Some of the many conditions that can account for speech and language problems in children are outlined in Table 2.12,18–29 These can be divided into primary speech and language problems, in which no other etiology can be found, and secondary speech and language problems, which are attributable to another condition.
Table 2. Speech and Language Problems in Children
| Disorder | Clinical findings and comments | Treatment and prognosis |
|---|---|---|
| Primary (not attributable to another condition) | ||
| Developmental speech and language delay | Speech is delayed. |
|
| Children have normal comprehension, intelligence, hearing, emotional relationships, and articulation skills.12 | ||
| Expressive language disorder | Speech is delayed. |
|
| Children have normal comprehension, intelligence, hearing, emotional relationships, and articulation skills. | ||
| Expressive language disorder is difficult to distinguish at an early age from the more common developmental speech and language delay. | ||
| Receptive language disorder | Speech is delayed, and also sparse, agrammatic, and indistinct in articulation. |
|
| Children may not look at or point to objects or persons named by parents (demonstrating a deficit in comprehension). | ||
| Children have normal responses to nonverbal auditory stimuli. | ||
| Secondary (attributable to another condition) | ||
| Autism spectrum disorder | Children have a variety of speech abnormalities, including speech delay (especially with concurrent intellectual disability), echolalia (repeating phrases) without generation of their own novel phrases, difficulty initiating and sustaining conversations, pronoun reversal, and speech and language regression. | |
| Children have impaired communication, impaired social interaction, and repetitive behaviors/circumscribed interests.20 | ||
| Cerebral palsy | Speech delay in children with cerebral palsy may be due to difficulty with coordination or spasticity of tongue muscles, hearing loss, coexisting intellectual disability, or a defect in the cerebral cortex. |
|
| Childhood apraxia of speech | Apraxia of speech is a physical problem in which children have difficulty making sounds in the right order, making it hard for their speech to be understood by others. |
|
| Children communicate with gestures but have difficulty with speech (demonstrating motivation to communicate, but lack of speech ability). | ||
| Dysarthria | Dysarthria is a physical problem in which children can have speech difficulties ranging from mild, with slightly slurred articulation and low-pitched voice, to profound, with an inability to produce any recognizable words. |
|
| Children communicate with gestures but have difficulty with speech (demonstrating motivation to communicate, but lack of speech ability). | ||
| Hearing loss after spoken language established | Speech and language are often gradually affected, with a decline in the precision of speech articulation and a lack of progress in vocabulary acquisition. |
|
| Parents may report that the child does not seem to be listening, or describe the child speaking better than listening. | ||
| Hearing loss before onset of speech | Speech is delayed. |
|
| Children may have distortions of speech sounds and prosodic patterns (intonation, rate, rhythm, and loudness of speech). | ||
| Children may not look at or point to objects or persons named by parents (demonstrating a deficit in comprehension). | ||
| Children have normal visual communication skills. | ||
| Intellectual disability | Speech is delayed. |
|
| Use of gestures is delayed, and there is a generalized delay in all aspects of developmental milestones. | ||
| Children may not look at or point to objects or persons named by parents (demonstrating a deficit in comprehension). | ||
| Selective mutism | Children with selective mutism show a consistent failure to speak in specific social situations (in which there is an expectation for speaking [e.g., at school]) despite speaking in other situations.20 |
|
Indications for Referral
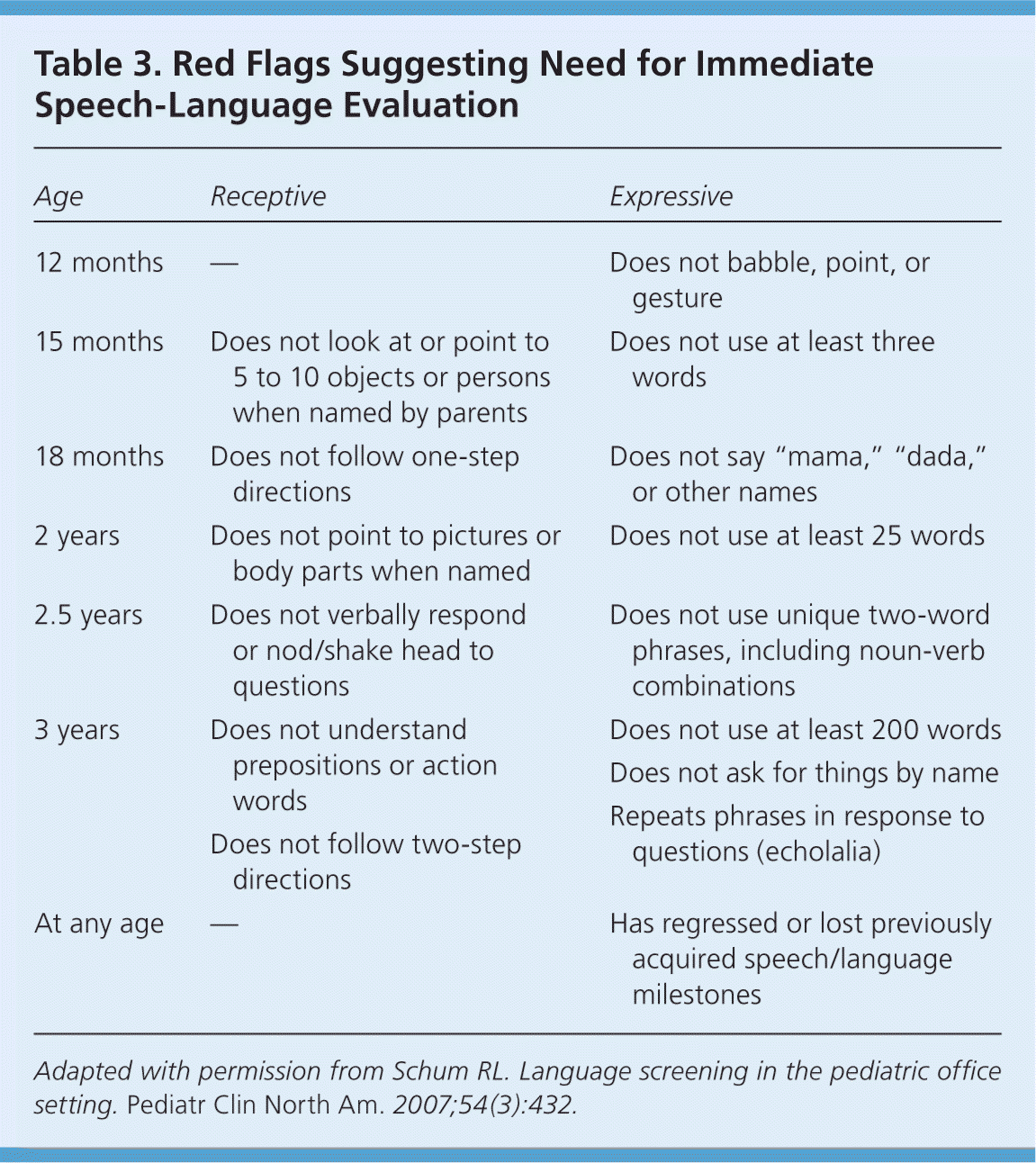
When speech and language delay is suspected, children should be referred to a speech-language pathologist or local early intervention program, and an audiologist.30–32 Table 3 lists red flags that suggest a need for immediate evaluation.30 Close monitoring before referral may be appropriate when a speech and language delay is suspected, but this approach should be used with caution, because two-thirds of children younger than three and a half years with speech and language delay will need speech therapy after one year without intervention.33 There is no certain way to determine which children will improve with the watchful waiting approach alone, but a speech-language pathologist's judgment of a child's communicative functioning appears to be the most significant predictor of linguistic outcome.33
Table 3. Red Flags Suggesting Need for Immediate Speech-Language Evaluation
For children with health insurance, options for referral include those organizations that contract with their insurance groups. Medicaid programs typically cover speech therapy, although smaller organizations may not accept those plans. Children without health insurance may be able to access therapy through services funded by grants under the Individuals with Disabilities Education Act and administered by individual states. State-administered early intervention services are available from birth to three years of age. After three years of age, children who qualify may receive speech therapy through the public school system. Uninsured children who do not qualify for these services may be able to access an organization with a sliding scale fee based on the family's economic status.
Therapies
Table 2 lists some of the many causes of speech and language problems, and briefly outlines treatment principles.12,18–29 The primary goals of therapy are to teach children strategies for comprehending spoken language and producing appropriate communicative behavior, and to help parents learn ways of encouraging their children's communication skills. There are good data available to support the effectiveness of speech-language therapy, particularly for children with primary expressive language disorder.18 The effect of speech-language therapy for children with receptive language disorder appears to be much smaller than it is for other groups.18 Parents can effectively administer speech-language therapy, but must first receive training, typically from a speech-language pathologist. The response to treatment is more varied when using parent administrators, which suggests that some parents may be more suited for providing therapy than others. Therapies lasting longer than eight weeks appear to be more effective than those lasting less than eight weeks.18
Parent Counseling
When a child is not meeting the expected developmental milestones for speech and language, it is important to avoid making a specific diagnosis until a formal evaluation has been completed. Parents can be counseled that, once a diagnosis is made, there are professionals who can work with the child and parents, and that many times children show a positive response to this intervention. If the child has other developmental or behavioral problems, these problems may persist, or they may improve as the child's communication skills improve.
At follow-up visits, the physician can review the child's progress with the parents. It is often helpful to focus on positive changes that the child has made since the previous visit, rather than only noting the child's current status compared with age-based norms. The physician can also focus on what the parents can do to help their child, including recommending books for the parents to read. Two books were recommended in a recent article30: The New Language of Toys: Teaching Communication Skills to Children with Special Needs: A Guide for Parents and Teachers,34 which provides specific suggestions for using toys and books in a developmentally appropriate manner to encourage communication, and Childhood Speech, Language, and Listening Problems: What Every Parent Should Know,35 which explains different communication problems and advises parents on available resources. The American Speech-Language-Hearing Association Web site (http://www.asha.org/) may also be helpful. It offers information on childhood speech and language disorders, and provides links to national organizations.

