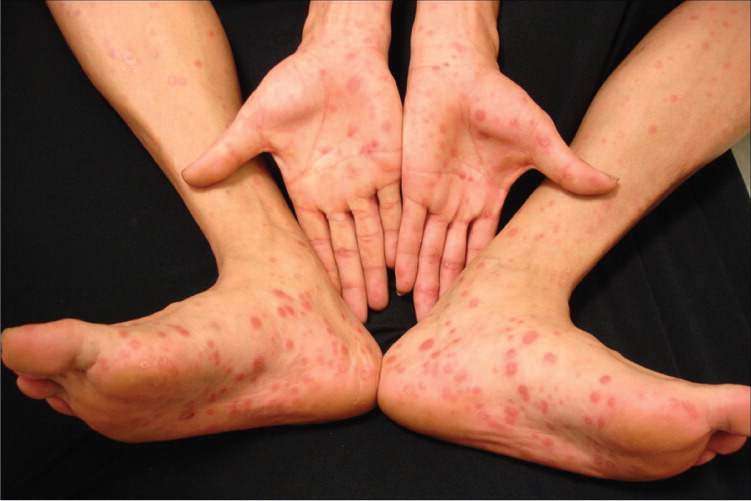
A 35-year-old man presented with a progressive, generalized skin rash that had persisted for one month. The rash was mildly pruritic and did not respond to topical corticosteroids. He did not have fever, arthralgia, myalgia, or lymphadenopathy, but had some general malaise. He had regular unprotected sex with sex workers. Physical examination revealed multiple oval, erythematous, scaling plaques of various sizes over the trunk, bilateral forearms, legs, palms, and soles (Figures 1 and 2).
Figure 1.
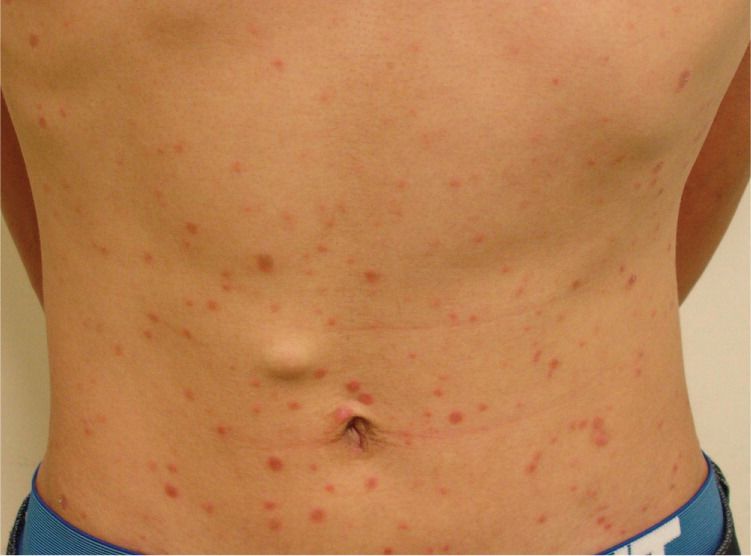
Figure 2.
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Erythema multiforme.
B. Pityriasis rosea.
C. Secondary syphilis.
D. Subacute lupus erythematosus.
E. Tinea corporis.
Discussion
The answer is C: secondary syphilis. Secondary syphilis usually presents three to 12 weeks after the primary chancre and recedes within two to 12 weeks.1 During this stage, the spirochetes (Treponema pallidum) multiply and spread throughout the body. Patients with secondary syphilis often have malaise, loss of appetite, fever, headache, myalgias, arthralgias, nasal discharge, and depression.
Most patients have a skin eruption, although it may be subtle. A localized or diffuse mucocutaneous rash is typical, and is generally nonpruritic and bilaterally symmetrical. Most eruptions are macular and/or papular, although nodular and pustular eruptions are rare. The lesions contain treponemes and are contagious. Papulosquamous eruptions have discoid, copper-colored or erythematous, oval or circular, indurated papules or plaques with a flat, shiny, scaly surface. A thin, white ring of scaling on the surface of a lesion (Biett collarette) is a valuable, but not pathognomonic, diagnostic sign.1 The palms and soles are often involved.2
Serologic testing is the standard diagnostic method for all stages of syphilis. Nontreponemal serology screening using Venereal Disease Research Laboratories or rapid plasma reagin testing should be performed. Because of the possibility of false-positive results, positive or equivocal nontreponemal test results should be followed with a treponemal test, such as the fluorescent treponemal antibody absorption, T. pallidum hemagglutination, and T. pallidum particle agglutination tests.3 Penicillin is the standard and most effective treatment for syphilis.4
Erythema multiforme is an acute and self-limited disease associated with herpes simplex virus infection, Mycoplasma pneumoniae infection, and drug use. The typical manifestation is nonpruritic, concentric target lesions appearing symmetrically on the extremities, with centripetal spreading.
Pityriasis rosea is a common benign papulosquamous disease. It typically begins with a salmon-colored patch with a collarette of fine scale inside the well-demarcated border (herald patch). Generalized, pruritic, salmon-colored macules or patches with a classic Christmas tree pattern appear on the trunk about one to two weeks after the herald patch.
Subacute lupus erythematosus manifests as papulosquamous, erythematous, scaly plaques predominantly on sun-exposed areas. Most patients have a history of photosensitivity and test results positive for anti-Ro antibodies.5
Tinea corporis, a superficial dermatophyte infection affecting the trunk and extremities, usually manifests as annular, erythematous, scaly, pruritic patches or plaques. Septated hyphae observed on potassium hydroxide examination can help confirm the diagnosis.
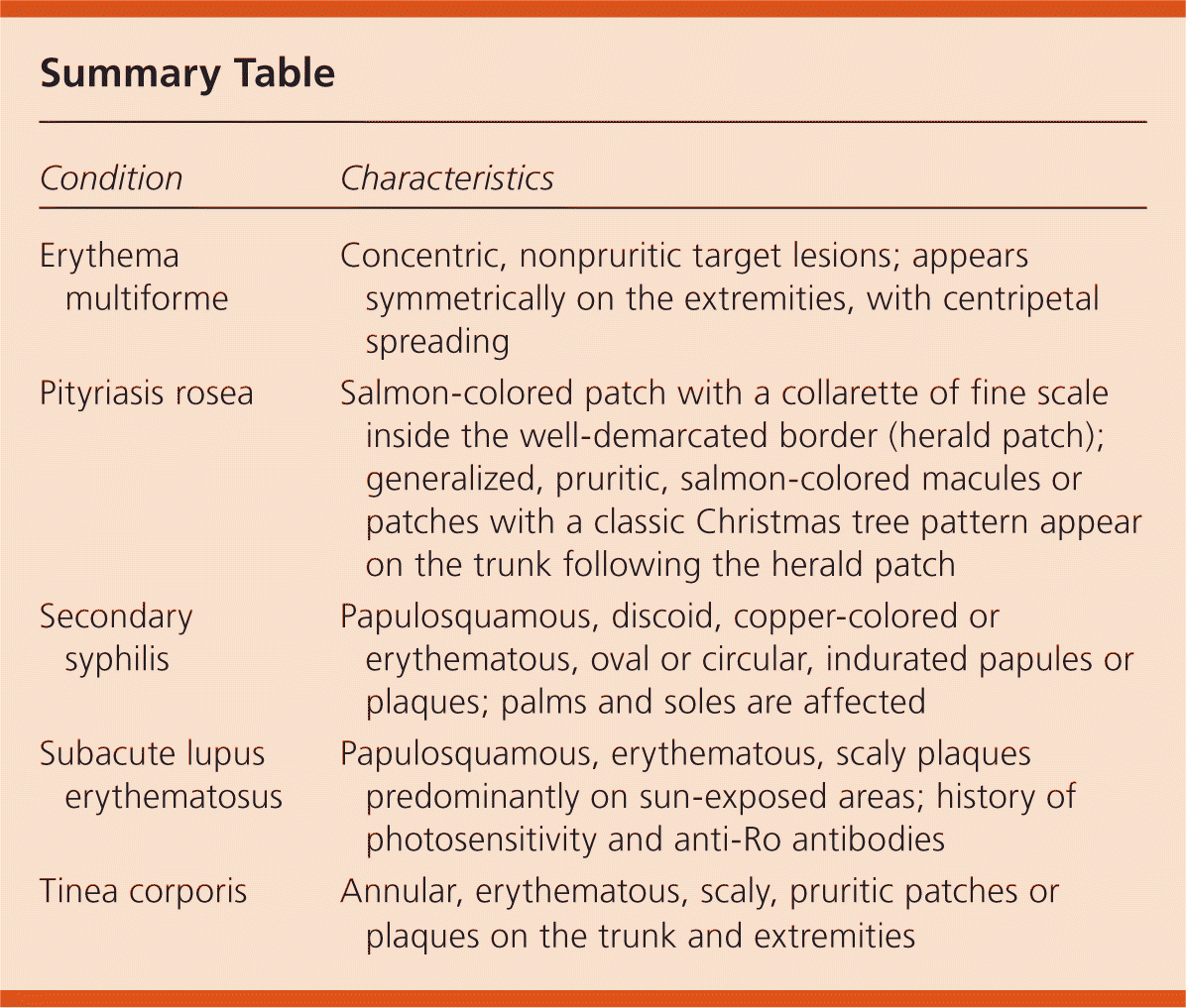
Summary Table
| Condition | Characteristics |
|---|---|
| Erythema multiforme | Concentric, nonpruritic target lesions; appears symmetrically on the extremities, with centripetal spreading |
| Pityriasis rosea | Salmon-colored patch with a collarette of fine scale inside the well-demarcated border (herald patch); generalized, pruritic, salmon-colored macules or patches with a classic Christmas tree pattern appear on the trunk following the herald patch |
| Secondary syphilis | Papulosquamous, discoid, copper-colored or erythematous, oval or circular, indurated papules or plaques; palms and soles are affected |
| Subacute lupus erythematosus | Papulosquamous, erythematous, scaly plaques predominantly on sun-exposed areas; history of photosensitivity and anti-Ro antibodies |
| Tinea corporis | Annular, erythematous, scaly, pruritic patches or plaques on the trunk and extremities |

