A healthy 18-year-old man with no significant medical history presented with right shoulder weakness and pain that had been present for one week. He had recently started a daily intensive physical fitness regimen similar to military boot camp. The week before his symptoms began, he had a particularly grueling workout session that involved multiple repetitions of push-ups, inchworms, and bear crawls that the patient found difficult to complete.
He had weakness in his right arm and could not lift it over his head, and he had dull, achy pain in his right shoulder. He had no numbness or tingling. He noticed that his right shoulder blade was protruding compared with the left side.
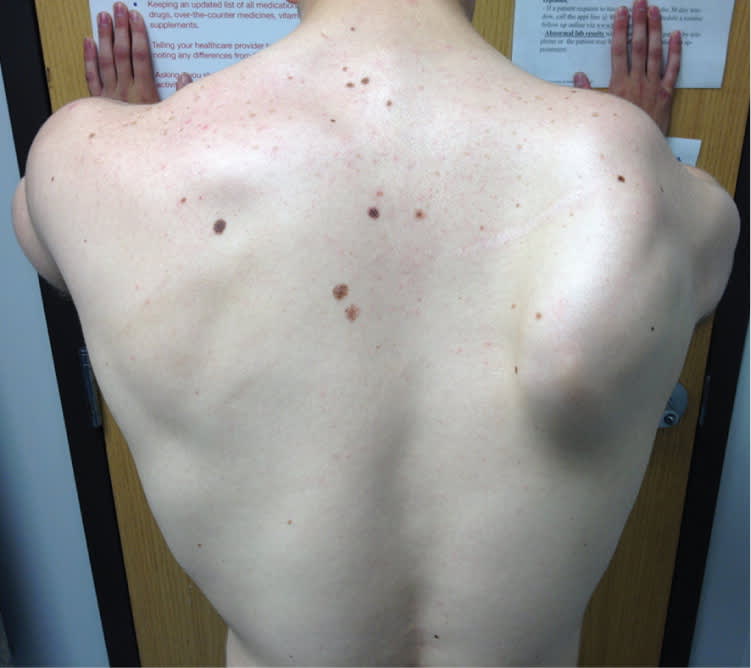
The examination revealed an obvious deformity (Figure 1). He was unable to abduct his arm above 90 degrees without assistance. He had full passive range of motion. Otherwise, his musculoskeletal and neurologic examination findings were normal, except for 4/5 strength in shoulder abduction.
Figure 1.
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Amyotrophic lateral sclerosis.
B. Backpack palsy.
C. Hereditary neuropathy.
D. Monomelic amyotrophy.
E. Neuralgic amyotrophy.
Discussion
The answer is C: hereditary neuropathy with liability to pressure palsies. This is a rare autosomal dominant neuropathy characterized by recurrent mononeuropathies that are typically associated with compression or minor trauma. In this case, the patient had carried two large duffel bags over his shoulders and participated in intensive workouts prior to the symptoms. The patient had a total palsy of the right long thoracic nerve, which accounted for the significant scapular winging seen on examination. Electromyography and nerve conduction studies also found slowed conduction in multiple nerves bilaterally without an apparent clinical manifestation, which is common with this disorder.
This hereditary neuropathy is usually associated with a deletion in the gene encoding peripheral myelin protein 22, although the pathophysiology is not completely understood. Typical sites of focal nerve block are identified with nerve entrapment. However, mild slowing of nerve conduction velocities, prolonged distal motor latencies, and reduced amplitudes in clinically unaffected nerves also occur. For most patients, the first mononeuropathy occurs before 40 years of age, and the typical pattern of abnormalities in nerve conduction studies is usually found in patients older than 15 years.1 Treatment focuses on avoiding repeated trauma to peripheral nerves, which may lead to additional mononeuropathies.1
Amyotrophic lateral sclerosis is characterized by both upper and lower motor neuron dysfunction. Clinical manifestations vary widely based on involvement of different motor neurons in the brain, brainstem, and spinal cord. One or more body regions may be affected by a combination of spasticity, decreased coordination, weakness, atrophy, fasciculations, and decreased reflexes. There is no pain or sensory disturbance.2
Backpack palsy is typically associated with activities that involve wearing a backpack, such as hiking, mountaineering, and military duty, and affects the shoulder girdle and elbow flexors, with sensory disturbances in the lateral shoulder and upper arm and in the radial forearm and hand. Symptoms commonly include paresis, numbness, and paresthesias of the upper extremities. The long thoracic nerve is most often affected.3
Monomelic amyotrophy typically presents in males in their late teens to early 20s. It has an insidious onset and leads to slow progression of unilateral weakness. There is atrophy of a distal upper extremity, most often the hand or forearm. Sensory disturbances, tendon reflex abnormalities, and upper motor neuron signs are rare. Nerve conduction studies of clinically unaffected nerves may have abnormal results.4
Neuralgic amyotrophy presents as acute, severe pain in the shoulder or arm that lasts for days to weeks. Weakness, atrophy, and sensory loss develop as the pain diminishes. Bilateral involvement of the brachial plexus occurs in 30% of patients, but clinical features are commonly asymmetric. Symptoms may be preceded by viral infections, immunizations, and strenuous exercise, or in the perioperative or peripartum period.5
Summary Table

| Condition | Characteristics |
|---|---|
| Amyotrophic lateral sclerosis | Upper and lower motor neuron dysfunction; combination of spasticity, decreased coordination, muscle weakness, atrophy, fasciculations, and decreased reflexes |
| Backpack palsy | Affects the shoulder girdle and elbow flexors, with sensory disturbances in the lateral shoulder and upper arm and in the radial forearm and hand; paresis, numbness, and paresthesias of the upper extremities after carrying a heavy backpack |
| Hereditary neuropathy with liability to pressure palsies | Mononeuropathy; localization in areas of frequent trauma or compression |
| Monomelic amyotrophy | Atrophy of a distal upper extremity, most often the hand or forearm, usually in the absence of sensory disturbances, tendon reflex abnormalities, and upper motor neuron signs |
| Neuralgic amyotrophy | Acute, severe pain in the shoulder or arm; pain is followed by muscle weakness, atrophy, and sensory loss; may be preceded by viral infection, immunization, or strenuous exercise, or in the perioperative or peripartum periods |
The author thanks Stacie M. Wrobel, RN, for her assistance in editing the manuscript.
The opinions and assertions contained herein are the private views of the author and are not to be construed as official or as reflecting the views of the U.S. Air Force Medical Dept. or the U.S. Air Force at large.

