Summary of Recommendation and Evidence
The USPSTF recommends screening for abnormal blood glucose as part of cardiovascular risk assessment in adults aged 40 to 70 years who are overweight or obese. Clinicians should offer or refer patients with abnormal blood glucose to intensive behavioral counseling interventions to promote a healthful diet and physical activity (Table 1). B recommendation.
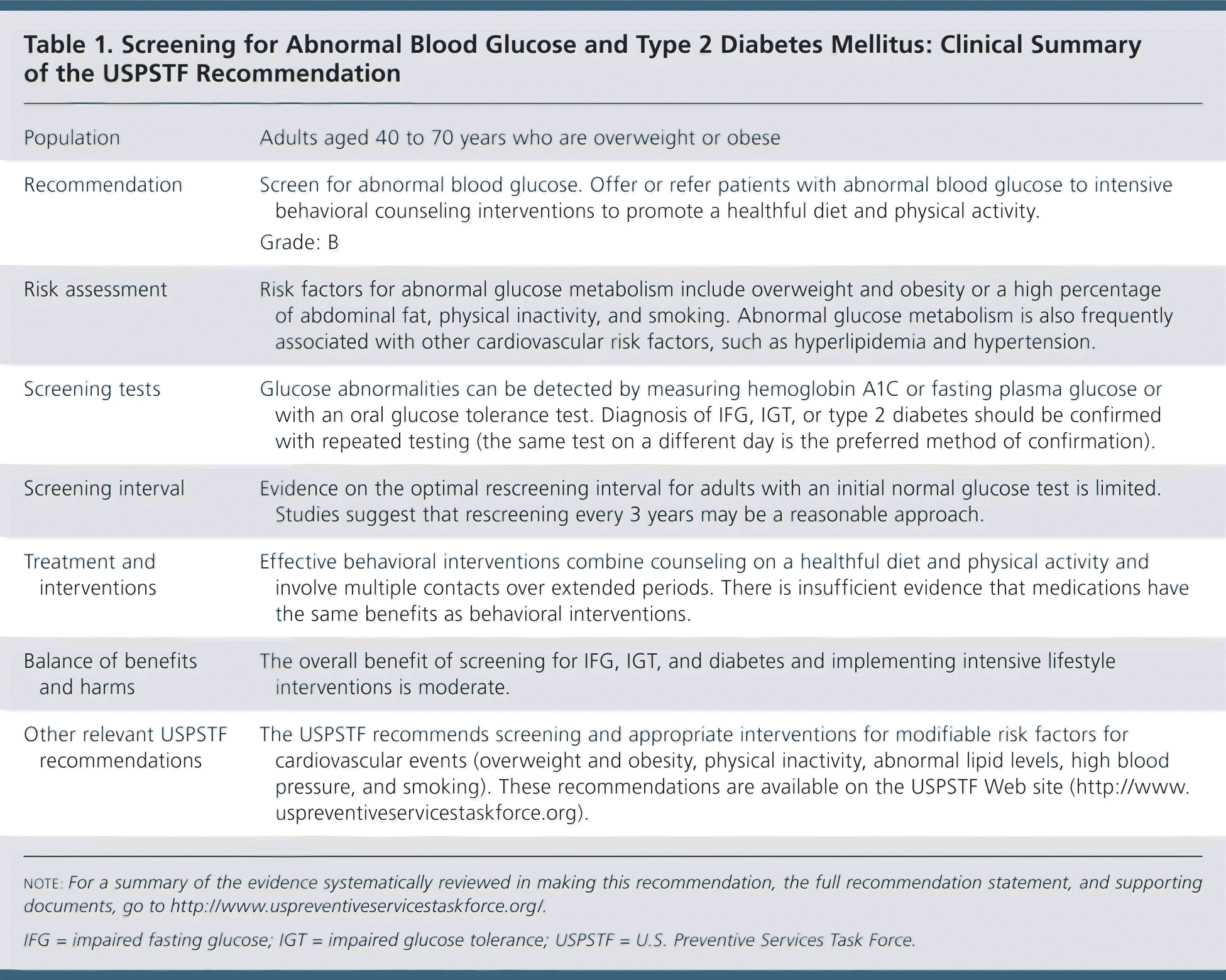
Table 1. Screening for Abnormal Blood Glucose and Type 2 Diabetes Mellitus: Clinical Summary of the USPSTF Recommendation
| Population | Adults aged 40 to 70 years who are overweight or obese |
| Recommendation | Screen for abnormal blood glucose. Offer or refer patients with abnormal blood glucose to intensive behavioral counseling interventions to promote a healthful diet and physical activity. |
| Grade: B | |
| Risk assessment | Risk factors for abnormal glucose metabolism include overweight and obesity or a high percentage of abdominal fat, physical inactivity, and smoking. Abnormal glucose metabolism is also frequently associated with other cardiovascular risk factors, such as hyperlipidemia and hypertension. |
| Screening tests | Glucose abnormalities can be detected by measuring hemoglobin A1C or fasting plasma glucose or with an oral glucose tolerance test. Diagnosis of IFG, IGT, or type 2 diabetes should be confirmed with repeated testing (the same test on a different day is the preferred method of confirmation). |
| Screening interval | Evidence on the optimal rescreening interval for adults with an initial normal glucose test is limited. Studies suggest that rescreening every 3 years may be a reasonable approach. |
| Treatment and interventions | Effective behavioral interventions combine counseling on a healthful diet and physical activity and involve multiple contacts over extended periods. There is insufficient evidence that medications have the same benefits as behavioral interventions. |
| Balance of benefits and harms | The overall benefit of screening for IFG, IGT, and diabetes and implementing intensive lifestyle interventions is moderate. |
| Other relevant USPSTF recommendations | The USPSTF recommends screening and appropriate interventions for modifiable risk factors for cardiovascular events (overweight and obesity, physical inactivity, abnormal lipid levels, high blood pressure, and smoking). These recommendations are available on the USPSTF Web site (http://www.uspreventiveservicestaskforce.org). |
note: For a summary of the evidence systematically reviewed in making this recommendation, the full recommendation statement, and supporting documents, go to http://www.uspreventiveservicestaskforce.org/.
IFG = impaired fasting glucose; IGT = impaired glucose tolerance; USPSTF = U.S. Preventive Services Task Force.
Rationale
IMPORTANCE
Cardiovascular disease (CVD) is the leading cause of death in the United States, and nearly one-quarter of deaths caused by CVD are considered to be preventable. Modifiable cardiovascular risk factors include abnormal blood glucose, hypertension, hyperlipidemia or dyslipidemia, smoking, overweight and obesity, physical inactivity, and an unhealthy diet. Type 2 diabetes mellitus is a metabolic disorder characterized by insulin resistance and relative insulin deficiency, resulting in hyperglycemia. Type 2 diabetes typically develops slowly, and progression from normal blood glucose to glucose abnormalities that meet generally accepted criteria for diabetes (Table 2) may take a decade or longer. Glucose abnormalities that do not meet the criteria for diabetes include impaired fasting glucose (IFG), an impaired response to oral glucose intake (impaired glucose tolerance [IGT]), or an increased average blood glucose level as evidenced by increased levels of hemoglobin A1C (HbA1C). Abnormal glucose metabolism is a risk factor for CVD and, in some individuals, may progress to meet the threshold for the diagnosis of diabetes.
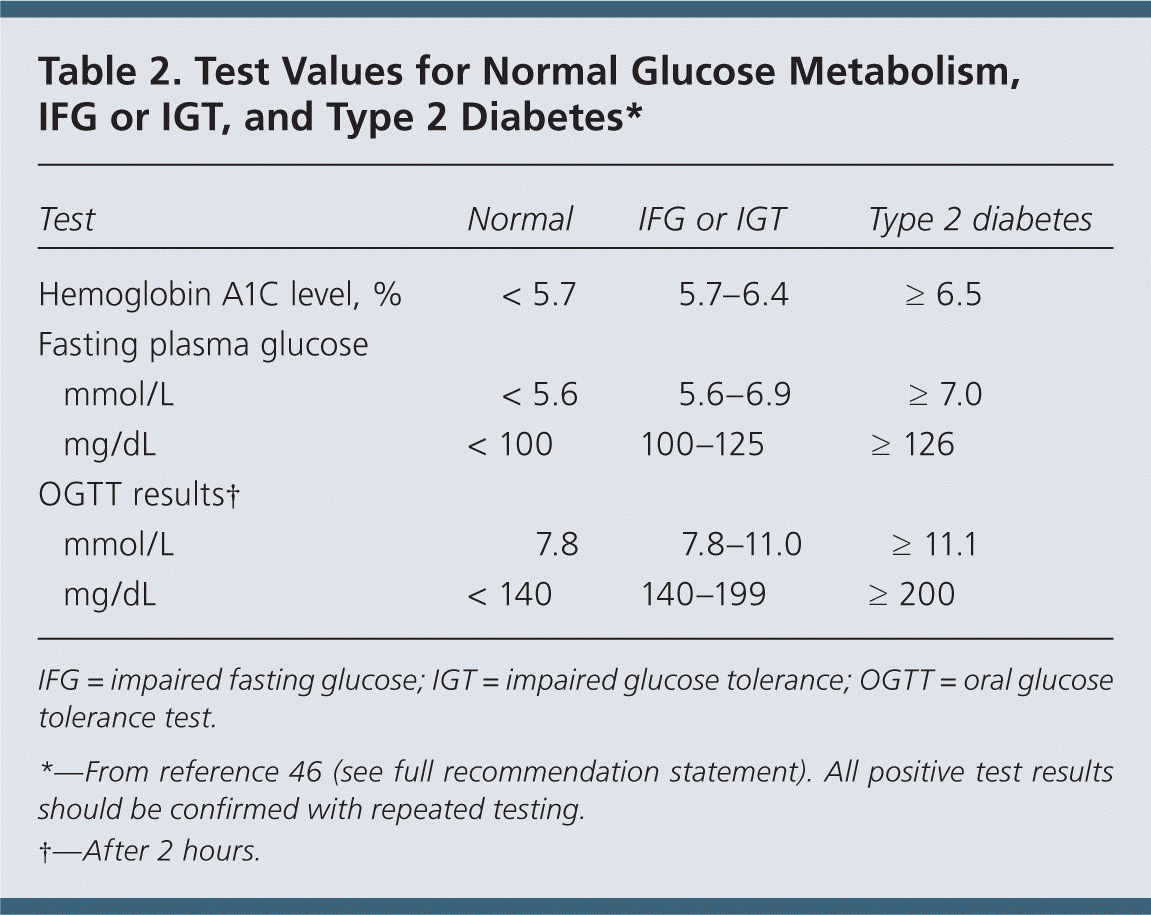
Table 2. Test Values for Normal Glucose Metabolism, IFG or IGT, and Type 2 Diabetes*
| Test | Normal | IFG or IGT | Type 2 diabetes | |
|---|---|---|---|---|
| Hemoglobin A1C level, % | < 5.7 | 5.7–6.4 | ≥ 6.5 | |
| Fasting plasma glucose | ||||
| mmol/L | < 5.6 | 5.6–6.9 | ≥ 7.0 | |
| mg/dL | < 100 | 100–125 | ≥ 126 | |
| OGTT results† | ||||
| mmol/L | 7.8 | 7.8–11.0 | ≥ 11.1 | |
| mg/dL | < 140 | 140–199 | ≥ 200 | |
IFG = impaired fasting glucose; IGT = impaired glucose tolerance; OGTT = oral glucose tolerance test.
*—From reference 46 (see full recommendation statement). All positive test results should be confirmed with repeated testing.
†—After 2 hours.
According to national data estimates from 2012, approximately 86 million Americans aged 20 years or older have IFG or IGT.1 Approximately 15% to 30% of these persons will develop type 2 diabetes within 5 years if they do not implement lifestyle changes to improve their health.1
Modifiable risk factors for abnormal glucose metabolism (manifested as either diabetes or abnormal glucose levels below the threshold for diabetes) include overweight and obesity or a high percentage of abdominal fat, physical inactivity, and smoking. Abnormal glucose metabolism is also frequently associated with other cardiovascular risk factors, such as hyperlipidemia and hypertension.
Given the increasing prevalence of abnormal glucose metabolism in the U.S. population, the USPSTF sought to examine the benefits and harms of screening for IFG, IGT, and type 2 diabetes.
BENEFITS OF EARLY DETECTION AND TREATMENT
The USPSTF found inadequate direct evidence that measuring blood glucose leads to improvements in mortality or cardiovascular morbidity.
The USPSTF previously found adequate evidence that intensive behavioral counseling interventions for persons at increased risk for CVD have moderate benefits in lowering CVD risk. Populations in which these benefits have been shown include persons who are obese or overweight and have hypertension, hyperlipidemia or dyslipidemia, and/or IFG or IGT. Benefits of behavioral interventions include reductions in blood pressure, glucose and lipid levels, and obesity and an increase in physical activity. Studies that specifically treat persons who have IFG or IGT with intensive lifestyle interventions to prevent the development of diabetes consistently show a moderate benefit in reducing progression to diabetes. Lifestyle interventions have greater effects on reducing progression to diabetes than metformin or other medications.
HARMS OF EARLY DETECTION AND TREATMENT
The USPSTF found that measuring blood glucose is associated with short-term anxiety but not long-term psychological harms. The USPSTF found adequate evidence that the harms of lifestyle interventions to reduce the incidence of diabetes are small to none. The harms of drug therapy for the prevention of diabetes are small to moderate, depending on the drug and dosage used.
USPSTF ASSESSMENT
The USPSTF concludes with moderate certainty that there is a moderate net benefit to measuring blood glucose to detect IFG, IGT, or diabetes and implementing intensive lifestyle interventions for persons found to have abnormal blood glucose.
Clinical Considerations
PATIENT POPULATION UNDER CONSIDERATION
This recommendation applies to adults aged 40 to 70 years seen in primary care settings who do not have symptoms of diabetes and are overweight or obese. The target population includes persons who are most likely to have glucose abnormalities that are associated with increased CVD risk and can be expected to benefit from primary prevention of CVD through risk factor modification.
Persons who have a family history of diabetes, have a history of gestational diabetes or polycystic ovarian syndrome, or are members of certain racial/ethnic groups (that is, African Americans, American Indians or Alaskan Natives, Asian Americans, Hispanics or Latinos, or Native Hawaiians or Pacific Islanders) may be at increased risk for diabetes at a younger age or at a lower body mass index. Clinicians should consider screening earlier in persons with 1 or more of these characteristics.
SCREENING TESTS
Glucose abnormalities can be detected by measuring HbA1C or fasting plasma glucose or with an oral glucose tolerance test. Table 2 shows test values for normal glucose metabolism, IFG, IGT, and type 2 diabetes. HbA1C is a measure of long-term blood glucose concentration and is not affected by acute changes in glucose levels due to stress or illness. Because HbA1C measurements do not require fasting, they are more convenient than using a fasting plasma glucose or oral glucose tolerance test. The oral glucose tolerance test is done in the morning in a fasting state; blood glucose concentration is measured 2 hours after ingestion of a 75-g oral glucose load.
The diagnosis of IFG, IGT, or type 2 diabetes should be confirmed; repeated testing with the same test on a different day is the preferred method of confirmation.
THRESHOLD FOR BEHAVIORAL INTERVENTIONS
Many studies assessed intensive behavioral interventions for persons at increased CVD risk, but none report a consistent threshold for intervention among persons with abnormal blood glucose. Many studies include persons with multiple risk factors, and CVD risk increases with the number of risk factors and glucose level. Perceived readiness for change and access to appropriate interventions will probably influence treatment recommendations. Although direct evidence that preventing a diagnosis of type 2 diabetes results in improved health outcomes is limited, primary prevention that reduces the chances of a diagnosis may reduce the adverse consequences of disease management. Because the average reduction in glucose levels resulting from intensive behavioral interventions is modest, persons with higher glucose levels may be more likely to benefit and avoid a diabetes diagnosis than those whose glucose levels are closer to normal.
TYPE OF INTERVENTION
Behavioral interventions that have an effect on CVD risk and delay or avoid progression of glucose abnormalities to type 2 diabetes combine counseling on a healthful diet and physical activity and are intensive, with multiple contacts over extended periods. The evidence is insufficient to conclude that pharmacologic interventions have the same multi-factorial benefits (for example, weight loss or reductions in glucose levels, blood pressure, and lipid levels) as behavioral interventions.
SCREENING INTERVALS
Evidence on the optimal rescreening interval for adults with an initial normal glucose test result is limited.2 Cohort and modeling studies suggest that rescreening every 3 years may be a reasonable approach for adults with normal blood glucose levels.3–7
OTHER APPROACHES TO PREVENTION
Because overweight and obesity, physical inactivity, abnormal lipid levels, high blood pressure, and smoking are all modifiable risk factors for cardiovascular events, the USPSTF recommends screening and appropriate interventions for these conditions (available at http://www.uspreventiveservicestaskforce.org).
The USPSTF recommends screening for obesity in adults and offering or referring those with a body mass index of 30 kg/m2 or greater to intensive, multicomponent behavioral interventions. Although intensive interventions may not be practical in many primary care settings, patients can be referred from primary care to community-based programs for these interventions.
The USPSTF recommends offering or referring adults who are overweight (body mass index > 25 kg/m2) and have additional cardiovascular risk factors to intensive behavioral counseling interventions to promote a healthful diet and physical activity for CVD prevention.
The USPSTF recommends screening for lipid disorders in men aged 35 years or older and women aged 45 years or older who are at increased risk for coronary heart disease. The USPSTF also recommends screening for hypertension in adults aged 18 years or older and that clinicians ask all adults about tobacco use and provide tobacco cessation interventions to those who use tobacco products.
USEFUL RESOURCES
The Community Preventive Services Task Force recommends combined diet and physical activity promotion programs for persons who are at increased risk for type 2 diabetes. It found that these programs are effective across a range of counseling intensities, settings, and facilitators. Effective programs commonly include setting a weight loss goal, individual or group sessions about diet and exercise, meetings with a trained diet or exercise counselor, or individually tailored diet or exercise plans. More information is available at http://www.thecommunityguide.org/diabetes/combineddietandpa.html.

