Summary of Recommendation and Evidence
The USPSTF recommends screening for syphilis infection in persons who are at increased risk for infection (Table 1). A recommendation.
Table 1. Screening for Syphilis Infection in Nonpregnant Adults and Adolescents: Clinical Summary of the USPSTF Recommendation
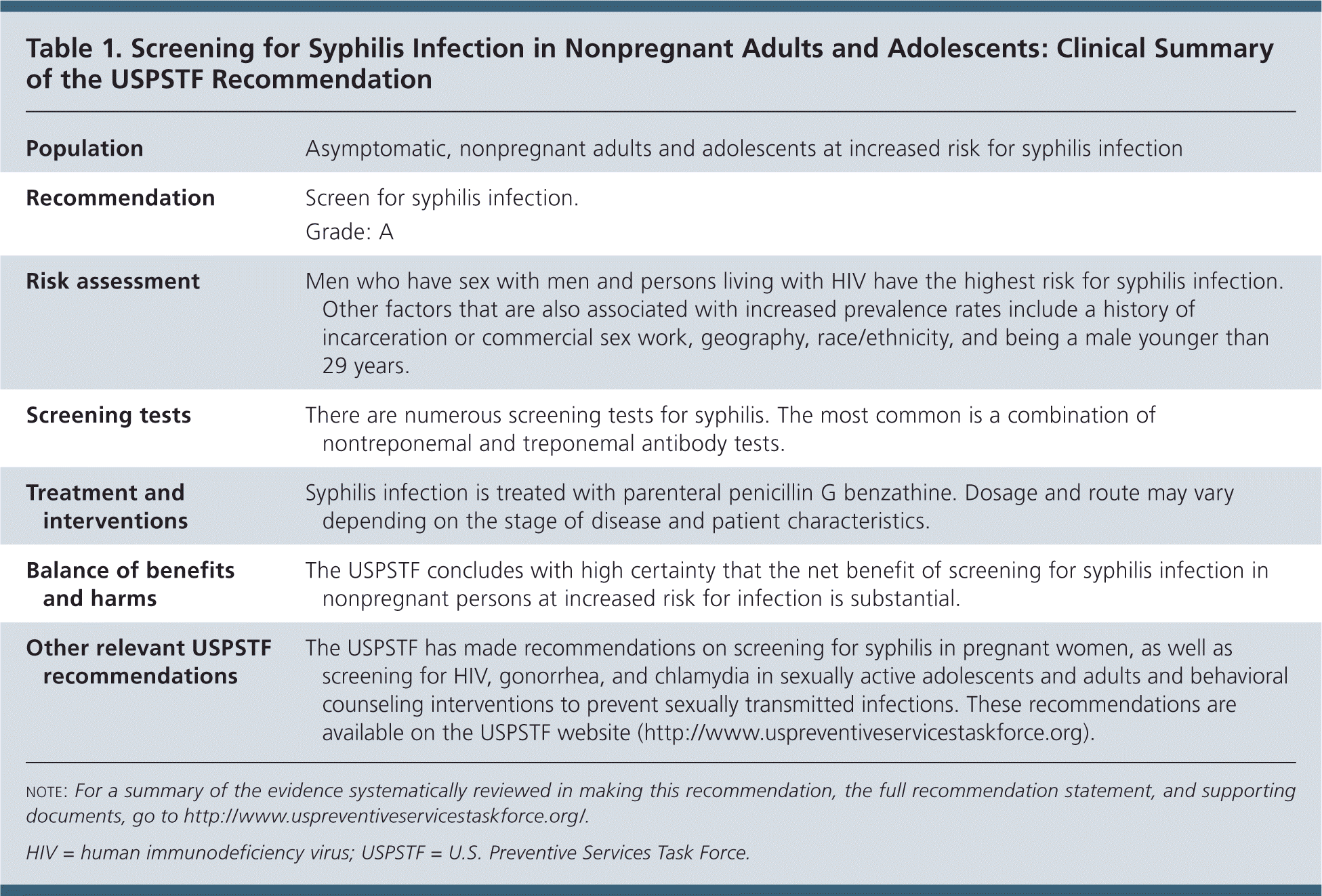
| Population | Asymptomatic, nonpregnant adults and adolescents at increased risk for syphilis infection |
| Recommendation | Screen for syphilis infection. |
| Grade: A | |
| Risk assessment | Men who have sex with men and persons living with HIV have the highest risk for syphilis infection. Other factors that are also associated with increased prevalence rates include a history of incarceration or commercial sex work, geography, race/ethnicity, and being a male younger than 29 years. |
| Screening tests | There are numerous screening tests for syphilis. The most common is a combination of nontreponemal and treponemal antibody tests. |
| Treatment and interventions | Syphilis infection is treated with parenteral penicillin G benzathine. Dosage and route may vary depending on the stage of disease and patient characteristics. |
| Balance of benefits and harms | The USPSTF concludes with high certainty that the net benefit of screening for syphilis infection in nonpregnant persons at increased risk for infection is substantial. |
| Other relevant USPSTF recommendations | The USPSTF has made recommendations on screening for syphilis in pregnant women, as well as screening for HIV, gonorrhea, and chlamydia in sexually active adolescents and adults and behavioral counseling interventions to prevent sexually transmitted infections. These recommendations are available on the USPSTF website (http://www.uspreventiveservicestaskforce.org). |
note: For a summary of the evidence systematically reviewed in making this recommendation, the full recommendation statement, and supporting documents, go to http://www.uspreventiveservicestaskforce.org/.
HIV = human immunodeficiency virus; USPSTF = U.S. Preventive Services Task Force.
Go to the Clinical Considerations section for information on risk factors for infection.
Rationale
IMPORTANCE
The number of cases of primary and secondary syphilis has increased since 2000. In 2014, 19,999 cases (6.3 cases per 100,000 persons) of primary and secondary syphilis were reported in the United States.1 Left untreated, syphilis can progress to late-stage disease in approximately 15% of persons who are infected.2 Consequences of late-stage syphilis include development of inflammatory lesions throughout the body (e.g., aortitis, gummatous lesions, and osteitis), which can lead to cardiovascular or organ dysfunction. Syphilis infection of the central nervous system (neurosyphilis) can occur at any stage of disease and can result in blindness, paresis, tabes dorsalis, and dementia. Syphilis infection also increases the risk for acquiring or transmitting HIV infection.
The USPSTF addresses screening for syphilis in pregnant women in a separate recommendation statement.3
DETECTION
There are numerous screening tests for syphilis. Most common is a combination of non-treponemal and treponemal antibody tests. The USPSTF found convincing evidence that screening algorithms with high sensitivity and specificity are available to accurately detect syphilis.
BENEFITS OF EARLY DETECTION AND TREATMENT
The USPSTF found convincing evidence that treatment with antibiotics can lead to substantial health benefits in nonpregnant persons who are at increased risk for syphilis infection by curing syphilis infection, preventing manifestations of late-stage disease, and preventing sexual transmission to others.
HARMS OF EARLY DETECTION AND TREATMENT
The USPSTF found no direct evidence on the harms of screening for syphilis in non-pregnant persons who are at increased risk for infection. Potential harms of screening include false-positive results that require clinical evaluation, unnecessary anxiety to the patient, and the potential stigma of having a sexually transmitted infection. The harms of antibiotic treatment are well established, and the magnitude of these harms is no greater than small.
USPSTF ASSESSMENT
The USPSTF concludes with high certainty that the net benefit of screening for syphilis infection in nonpregnant persons who are at increased risk for infection is substantial.
Clinical Considerations
PATIENT POPULATION UNDER CONSIDERATION
This recommendation applies to asymptomatic, nonpregnant adults and adolescents who are at increased risk for syphilis infection. Screening for syphilis in nonpregnant populations is an important public health approach to preventing the sexual transmission of syphilis and subsequent vertical transmission of congenital syphilis.
ASSESSMENT OF RISK
The USPSTF recommends screening for syphilis in persons who are at increased risk for infection. Based on 2014 surveillance data,1 men who have sex with men (MSM) and men and women living with HIV have the highest risk for syphilis infection; 61.1% of cases of primary and secondary syphilis occurred among MSM, and approximately one-half of all MSM diagnosed with syphilis were also coinfected with HIV. One study found that rates of syphilis coinfection were 5 times higher in MSM living with HIV compared with men living with HIV who do not have sex with men.4 Based on older study data from northern California, the adjusted relative risk for syphilis infection in persons living with HIV (vs. those without HIV) was 86.0 (95% CI, 78.6 to 94.1); 97% of those living with HIV and with incident syphilis were male.5
When deciding which other persons to screen for syphilis, clinicians should be aware of the prevalence of infection in the communities they serve, as well as other sociodemographic factors that may be associated with increased risk of syphilis infection. Factors associated with increased prevalence that clinicians should consider include history of incarceration, history of commercial sex work, certain racial/ethnic groups, and being a male younger than 29 years, as well as regional variations that are well described. Men accounted for 90.8% of all cases of primary and secondary syphilis in 2014. Men aged 20 to 29 years had the highest prevalence rate, nearly 3 times higher than that in the average U.S. male population.1 Syphilis prevalence rates are also higher in certain racial/ethnic groups (among both men and women); in 2014, prevalence rates of primary and secondary syphilis were 18.9 cases per 100,000 black individuals, 7.6 cases per 100,000 Hispanic individuals, 7.6 cases per 100,000 American Indian/Alaska Native individuals, 6.5 cases per 100,000 Native Hawaiian/Pacific Islander individuals, 3.5 cases per 100,000 white individuals, and 2.8 cases per 100,000 Asian individuals.1 The southern United States comprises the largest proportion of syphilis cases (41%); however, the case rate is currently highest in the western United States (7.9 cases per 100,000 persons). Metropolitan areas in general have increased prevalence rates of syphilis.1 Risk factors for syphilis often do not present independently and may frequently overlap. In addition, local prevalence rates may change over time, so clinicians should be aware of the latest data and trends for their specific population and geographic area.
Although direct evidence on screening among non-pregnant persons who are not at increased risk for syphilis infection is lacking, based on the established test performance characteristics of current screening tests and the low prevalence rate of syphilis in this population, the yield of screening is likely low. Therefore, screening in this population may result in high false-positive rates and overtreatment.
SCREENING TESTS
Current screening tests for syphilis rely on detection of antibodies rather than direct detection of the organism. Screening for syphilis infection is a 2-step process involving an initial nontreponemal test (Venereal Disease Research Laboratory [VDRL] or rapid plasma reagin [RPR] test) followed by a confirmatory treponemal antibody detection test (fluorescent treponemal antibody absorption [FTA-ABS] or Treponema pallidum particle agglutination [TP-PA] test). A reverse sequence screening algorithm has been developed in which an automated treponemal test (such as enzyme-linked, chemiluminescence, or multiplex flow immunoassays) is performed first, followed by a nontreponemal test. If the test results are discordant in the reverse sequence algorithm, a second treponemal test (preferably using a different treponemal antibody) is performed.6 There is limited evidence on the accuracy of screening using the reverse sequence algorithm. Findings from 2 studies suggest that using a reverse sequence algorithm may detect additional cases of syphilis missed by the usual algorithm.7 However, the clinical significance of these additional cases is unclear, and more studies are needed to better understand the implications of using a reverse sequence algorithm for screening in a primary care setting. Newer screening technologies that include rapid syphilis tests are also currently emerging. These tests have the potential to be performed in nontraditional and nonclinical settings; however, more evidence is needed on the effectiveness of these tests as part of a screening program in a primary care setting.
SCREENING INTERVALS
The optimal screening frequency for persons who are at increased risk for syphilis infection is not well established. MSM or persons living with HIV may benefit from more frequent screening. Initial studies suggest that detection of syphilis infection in MSM or persons living with HIV improves when screening is performed every 3 months compared with annually.7
TREATMENT
In its 2015 guidelines on the treatment of sexually transmitted diseases, the Centers for Disease Control and Prevention (CDC) recommends parenteral penicillin G benzathine for the treatment of syphilis. Dosage and route may vary depending on the stage of disease and patient characteristics. To obtain the most up-to-date information, clinicians are encouraged to access the CDC website.8
ADDITIONAL APPROACHES TO PREVENTION
Public health agencies and local health departments have a critical role in the prevention and treatment of syphilis. Local health departments are often responsible for investigating incident cases of syphilis and identifying potential contacts who may need further testing or treatment. Primary care clinicians should be aware of applicable local public health laws and reporting requirements for syphilis cases.
USEFUL RESOURCES
Persons who are at risk for or have been diagnosed with syphilis infection may engage in behavior that increases their risk for other sexually transmitted infections. The USPSTF has made a separate recommendation on screening for syphilis in pregnant women, as well as screening for HIV, gonorrhea, and chlamydia in sexually active adolescents and adults and behavioral counseling interventions to prevent sexually transmitted infections (available at http://www.uspreventiveservicestaskforce.org).
This recommendation statement was first published in JAMA. 2016;315 (21):2321–2327.
The “Other Considerations,” “Discussion,” “Update of Previous USPSTF Recommendation,” and “Recommendations of Others” sections of this recommendation statement are available at https://www.uspreventiveservicestaskforce.org/Page/Document/UpdateSummaryFinal/syphilis-infection-in-nonpregnant-adults-and-adolescents.
The USPSTF recommendations are independent of the U.S. government. They do not represent the views of the Agency for Healthcare Research and Quality, the U.S. Department of Health and Human Services, or the U.S. Public Health Service.

