Summary of Recommendation and Evidence
The USPSTF recommends vision screening at least once in all children aged 3 to 5 years to detect amblyopia or its risk factors (Table 1).
B recommendation
The USPSTF concludes that the current evidence is insufficient to assess the balance of benefits and harms of vision screening in children younger than 3 years. I statement.
Table 1. Vision Screening in Children Aged 6 Months to 5 Years: Clinical Summary of the USPSTF Recommendation

| Population | Children aged 3 to 5 years | Children younger than 3 years |
| Recommendation | Screen at least once to detect amblyopia or its risk factors. | No recommendation. |
| Grade: B | Grade: I (insufficient evidence) | |
| Risk assessment | All children aged 3 to 5 years are at risk of vision abnormalities and should be screened; specific risk factors include strabismus, refractive errors, and media opacity. Additional risk factors associated with amblyopia, strabismus, or refractive errors include family history in a first-degree relative, prematurity, low birth weight, maternal substance abuse, maternal smoking during pregnancy, and low levels of parental education. | |
| Screening tests | Various screening tests are used in primary care to identify vision abnormalities in children, including: the red reflex test, the cover-uncover test, the corneal light reflex test, visual acuity tests (such as Snellen, Lea Symbols, and HOTV charts), autorefractors and photoscreeners, and stereoacuity tests. | |
| Treatments | Primary treatment includes correction of any underlying refractive error with the use of corrective lenses, occlusion therapy for amblyopia (eye patching, atropine eye drops, or Bangerter occlusion foils), or a combination of treatments. | |
| Balance of harms and benefits | The USPSTF concludes with moderate certainty that vision screening to detect amblyopia or its risk factors in children aged 3 to 5 years has a moderate net benefit. | The USPSTF concludes that the benefits of vision screening to detect amblyopia or its risk factors in children younger than 3 years are uncertain, and that the balance of benefits and harms cannot be determined. |
note: For a summary of the evidence systematically reviewed in making this recommendation, the full recommendation statement, and supporting documents, go to http://www.uspreventiveservicestaskforce.org/.
USPSTF = U.S. Preventive Services Task Force.
Rationale
IMPORTANCE
One of the most important causes of vision abnormalities in children is amblyopia (also known as “lazy eye”). Amblyopia is an alteration in the visual neural pathway in a child's developing brain that can lead to permanent vision loss in the affected eye.1,2 It usually occurs in 1 eye but can occur in both. Risk factors associated with the development of amblyopia include strabismus (ocular misalignment); vision deprivation caused by media opacity (e.g., cataracts); high, uncorrected refractive errors (e.g., myopia, hyperopia, and astigmatism), and anisometropia (Table 2). Other common causes of vision abnormalities are nonamblyopic strabismus and nonamblyopic refractive error.1 Among children younger than 6 years, 1% to 6% have amblyopia or its risk factors (strabismus, anisometropia, or both), which, if left untreated, could lead to amblyopia.1,3–7 Early identification of vision abnormalities could prevent the development of amblyopia.
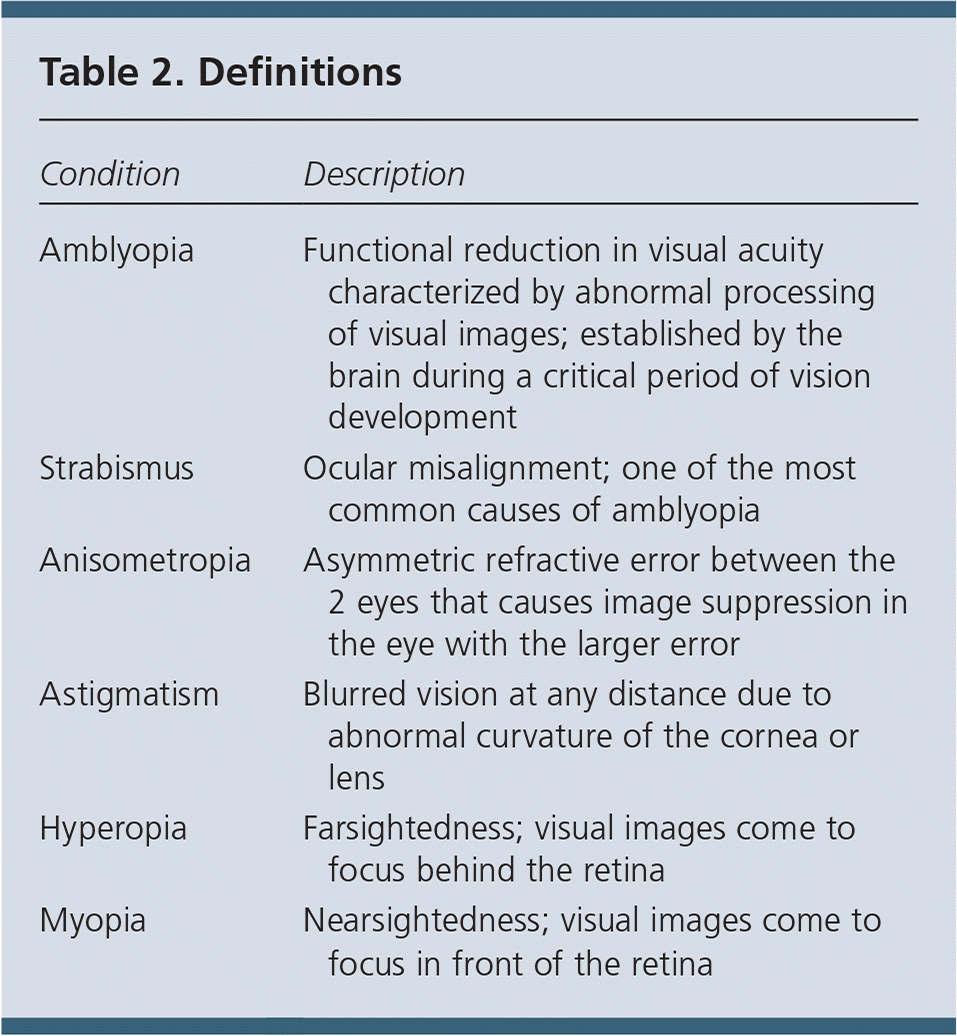
Table 2. Definitions
| Condition | Description |
|---|---|
| Amblyopia | Functional reduction in visual acuity characterized by abnormal processing of visual images; established by the brain during a critical period of vision development |
| Strabismus | Ocular misalignment; one of the most common causes of amblyopia |
| Anisometropia | Asymmetric refractive error between the 2 eyes that causes image suppression in the eye with the larger error |
| Astigmatism | Blurred vision at any distance due to abnormal curvature of the cornea or lens |
| Hyperopia | Farsightedness; visual images come to focus behind the retina |
| Myopia | Nearsightedness; visual images come to focus in front of the retina |
DETECTION
The USPSTF found adequate evidence that vision screening tools are accurate in detecting vision abnormalities, including refractive errors, strabismus, and amblyopia. There is inadequate evidence to compare screening accuracy across age groups (< 3 vs. ≥ 3 years). Many studies of clinical accuracy did not enroll children younger than 3 years.
BENEFITS OF EARLY DETECTION AND TREATMENT
The USPSTF found adequate evidence that treatment of amblyopia or its risk factors in children aged 3 to 5 years leads to improved visual acuity. The USPSTF determined that the magnitude of improvement in visual acuity is of moderate benefit. The USPSTF found inadequate evidence that treatment reduced the incidence of long-term amblyopia or improved school performance, functioning, or quality of life. Limited evidence suggests that screening can potentially reduce psychosocial harms. The USPSTF found inadequate evidence that treatment of amblyopia or its risk factors in children younger than 3 years leads to improved vision outcomes (i.e., visual acuity) or other benefits.
HARMS OF EARLY DETECTION AND TREATMENT
The USPSTF found adequate evidence to assess harms of vision screening tests in children aged 3 to 5 years, including higher false-positive rates in low-prevalence populations. False-positive screening results may lead to overdiagnosis or unnecessary treatment. Limited evidence suggests that eye patching in children aged 3 to 5 years does not worsen visual acuity in the nonamblyopic eye but may be associated with psychological harms, such as child or parental upset or concern. The USPSTF found adequate evidence to bound the potential harms of vision screening and treatment in children aged 3 to 5 years as small, based on the nature of the interventions. The USPSTF found inadequate evidence on the harms of treatment in children younger than 3 years.
USPSTF ASSESSMENT
The USPSTF concludes with moderate certainty that vision screening to detect amblyopia or its risk factors in children aged 3 to 5 years has a moderate net benefit. The USPSTF concludes that the benefits of vision screening to detect amblyopia or its risk factors in children younger than 3 years are uncertain, and that the balance of benefits and harms cannot be determined for this age group.
Clinical Considerations
PATIENT POPULATION UNDER CONSIDERATION
This recommendation applies to children aged 6 months to 5 years.
RISK FACTORS ASSOCIATED WITH AMBLYOPIA
Although all children aged 3 to 5 years are at risk of vision abnormalities and should be screened, there are certain risk factors that increase risk. Risk factors for amblyopia include strabismus; high, uncorrected refractive errors (e.g., myopia, hyperopia, and astigmatism); anisometropia; and media opacity.1–3 Additional risk factors associated with amblyopia, strabismus, or refractive errors include family history in a first-degree relative, prematurity, low birth weight, maternal substance abuse, maternal smoking during pregnancy, and low levels of parental education.1,8–13
SCREENING TESTS
A variety of screening tests are used to identify vision abnormalities in children in primary care settings (Table 3). Visual acuity tests screen for visual deficits associated with amblyopia and refractive error. Ocular alignment tests screen for strabismus. Stereoacuity tests assess depth perception.1,14 For children younger than 3 years, screening may include the fixation and follow test (for visual acuity), the red reflex test (for media opacity), and the corneal light reflex test (for strabismus).1,14 Instrument-based vision screening (i.e., with autorefractors and photoscreeners) may be used in very young children, including infants. Autorefractors are computerized instruments that detect refractive errors; photoscreeners detect amblyopia risk factors (ocular alignment and media opacity) and refractive errors.1,15 Vision screening in children older than 3 years may include the red reflex test, the cover-uncover test (for strabismus), the corneal light reflex test, visual acuity tests (e.g., Snellen, Lea Symbols [Lea-Test], and HOTV [Precision Vision] charts), autorefractors and photoscreeners, and stereoacuity tests.1,14 Children with positive findings should be referred for a complete eye examination to confirm the presence of vision problems and for further treatment.
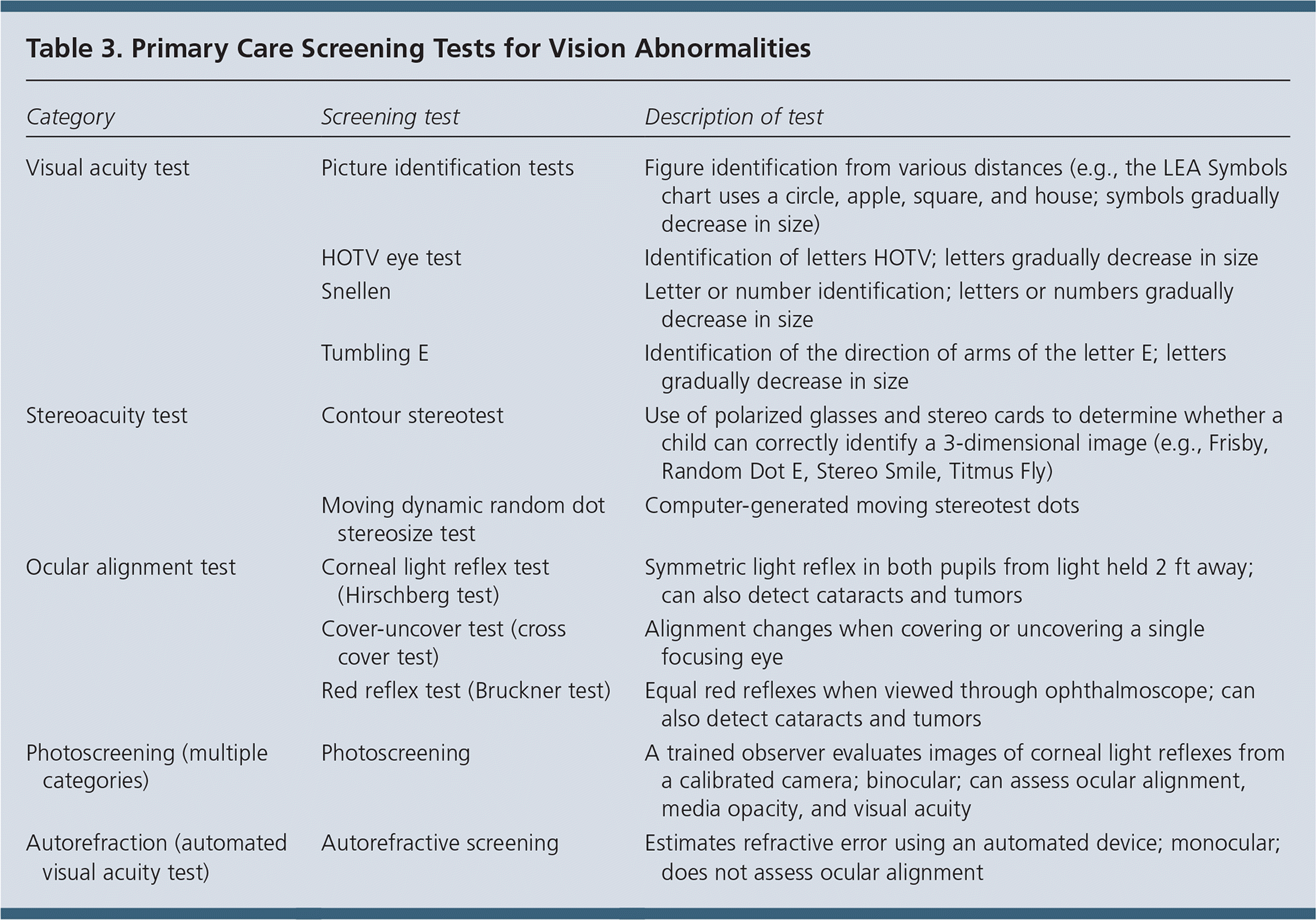
Table 3. Primary Care Screening Tests for Vision Abnormalities
| Category | Screening test | Description of test |
|---|---|---|
| Visual acuity test | Picture identification tests | Figure identification from various distances (e.g., the LEA Symbols chart uses a circle, apple, square, and house; symbols gradually decrease in size) |
| HOTV eye test | Identification of letters HOTV; letters gradually decrease in size | |
| Snellen | Letter or number identification; letters or numbers gradually decrease in size | |
| Tumbling E | Identification of the direction of arms of the letter E; letters gradually decrease in size | |
| Stereoacuity test | Contour stereotest | Use of polarized glasses and stereo cards to determine whether a child can correctly identify a 3-dimensional image (e.g., Frisby, Random Dot E, Stereo Smile, Titmus Fly) |
| Moving dynamic random dot stereosize test | Computer-generated moving stereotest dots | |
| Ocular alignment test | Corneal light reflex test (Hirschberg test) | Symmetric light reflex in both pupils from light held 2 ft away; can also detect cataracts and tumors |
| Cover-uncover test (cross cover test) | Alignment changes when covering or uncovering a single focusing eye | |
| Red reflex test (Bruckner test) | Equal red reflexes when viewed through ophthalmoscope; can also detect cataracts and tumors | |
| Photoscreening (multiple categories) | Photoscreening | A trained observer evaluates images of corneal light reflexes from a calibrated camera; binocular; can assess ocular alignment, media opacity, and visual acuity |
| Autorefraction (automated visual acuity test) | Autorefractive screening | Estimates refractive error using an automated device; monocular; does not assess ocular alignment |
SCREENING INTERVAL
The USPSTF did not find adequate evidence to determine the optimal screening interval in children aged 3 to 5 years.
TREATMENT
Treatment depends on the specific condition and includes correction of any underlying refractive error with the use of corrective lenses, occlusion therapy for amblyopia (e.g., eye patching, atropine eye drops, or Bangerter occlusion foils), or surgical interventions for some causes of refractory strabismus.
SUGGESTIONS FOR PRACTICE REGARDING THE I STATEMENT
Potential Preventable Burden. Untreated amblyopia is not likely to spontaneously resolve.1,16,17 Treatment efficacy decreases with age, with a risk of irreversible vision loss.1,18–20 Untreated vision abnormalities can result in short- and long-term physical and psychological harms, such as accidents and injuries, experiencing bullying behaviors, poor visual motor skills, depression and anxiety, poor self-esteem, and problems at school and work.21–25
Current Practice. Vision screening is routinely offered in most primary care settings. Screening rates among children aged 3 years are approximately 40% and increase with age.1,26 One survey reported that 3% of pediatricians began vision screening at age 6 months.1,27 Typical components of vision screening include assessments of visual acuity and strabismus. Younger children (< 3 years) are often unable to cooperate with some of the clinical screening tests performed in clinical practice, such as visual acuity testing, which may result in false-positive results. Some clinical practice guidelines now recommend using handheld autorefractors and photoscreeners as alternative approaches to screening in children 6 months and older because of improved child cooperation and improved accuracy.1,28 One potential disadvantage of using some types of photoscreeners is the need for external interpretation of screening results. Children with positive findings should be referred for a complete eye examination to confirm the presence of vision abnormalities and for further treatment.
This recommendation statement was first published in JAMA. 2017;318(9):836–844.
The “Other Considerations,” “Discussion,” “Recommendations of Others,” and “Update of Previous Recommendation” sections of this recommendation statement are available at https://www.uspreventiveservicestaskforce.org/Page/Document/UpdateSummaryFinal/vision-in-children-ages-6-months-to-5-years-screening.
The USPSTF recommendations are independent of the U.S. government. They do not represent the views of the Agency for Healthcare Research and Quality, the U.S. Department of Health and Human Services, or the U.S. Public Health Service.

