Childhood bullying is common and can lead to serious adverse physical and mental health effects for both the victim and the bully. In teenagers, risk factors for becoming a victim of bullying include being lesbian, gay, bisexual, or transgender; having a disability or medical condition such as asthma, diabetes mellitus, a skin condition, or food allergy; or being an outlier in weight and stature. An estimated 20% of youth have been bullied on school property, and 16% have been bullied electronically in the past year. Bullying can result in emotional distress, depression, anxiety, social isolation, low self-esteem, school avoidance/refusal, and substance abuse for the victim and the bully. Preventive measures include encouraging patients to find enjoyable activities that promote confidence and self-esteem, modeling how to treat others with kindness and respect, and encouraging patients to seek positive friendships. For those who feel concern or guilt about sharing their experiences, it may be useful to explain that revealing the bullying may not only help end the cycle for them but for others as well. Once bullying has been identified, family physicians have an important role in screening for its harmful effects, such as depression and anxiety. A comprehensive, multitiered approach involving families, schools, and community resources can help combat bullying. Family physicians are integral in recognizing children and adolescents who are affected by bullying—as victims, bullies, or bully-victims—so they can benefit from the intervention process.
Bullying, a common experience for children and adolescents, has gained increasing attention over the past three decades as its long-term implications and lasting consequences have become more apparent. Key elements that define bullying include an unwanted, aggressive attack or intimidation tactic that is intended to cause fear, distress, or harm to the victim; an imbalance of power between the bully and victim; and repetitive occurrences of the behaviors.1–6 Bullying can be direct (physical or verbal), indirect (relational/social, social exclusion, spreading rumors, psychological/stalking), or cyberbullying (performed via electronic or digital means).7,8 In cyberbullying, the element of repetition does not need to be present because a public post on social media can potentially be seen by many individuals.8–10
WHAT IS NEW ON THIS TOPIC
Childhood Bullying
An estimated 20% of youth have been bullied on school property in the past year, and 16% have been bullied electronically.
The American Academy of Pediatrics suggests introducing the concept of bullying to parents during the six-year-old well-child examination.
The use of electronic psychosocial assessment tools, such as myAssessment or the Rapid Assessment for Adolescent Preventive Services, to identify high-risk behaviors may increase rates of disclosure and be a time-saving step for busy clinicians.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
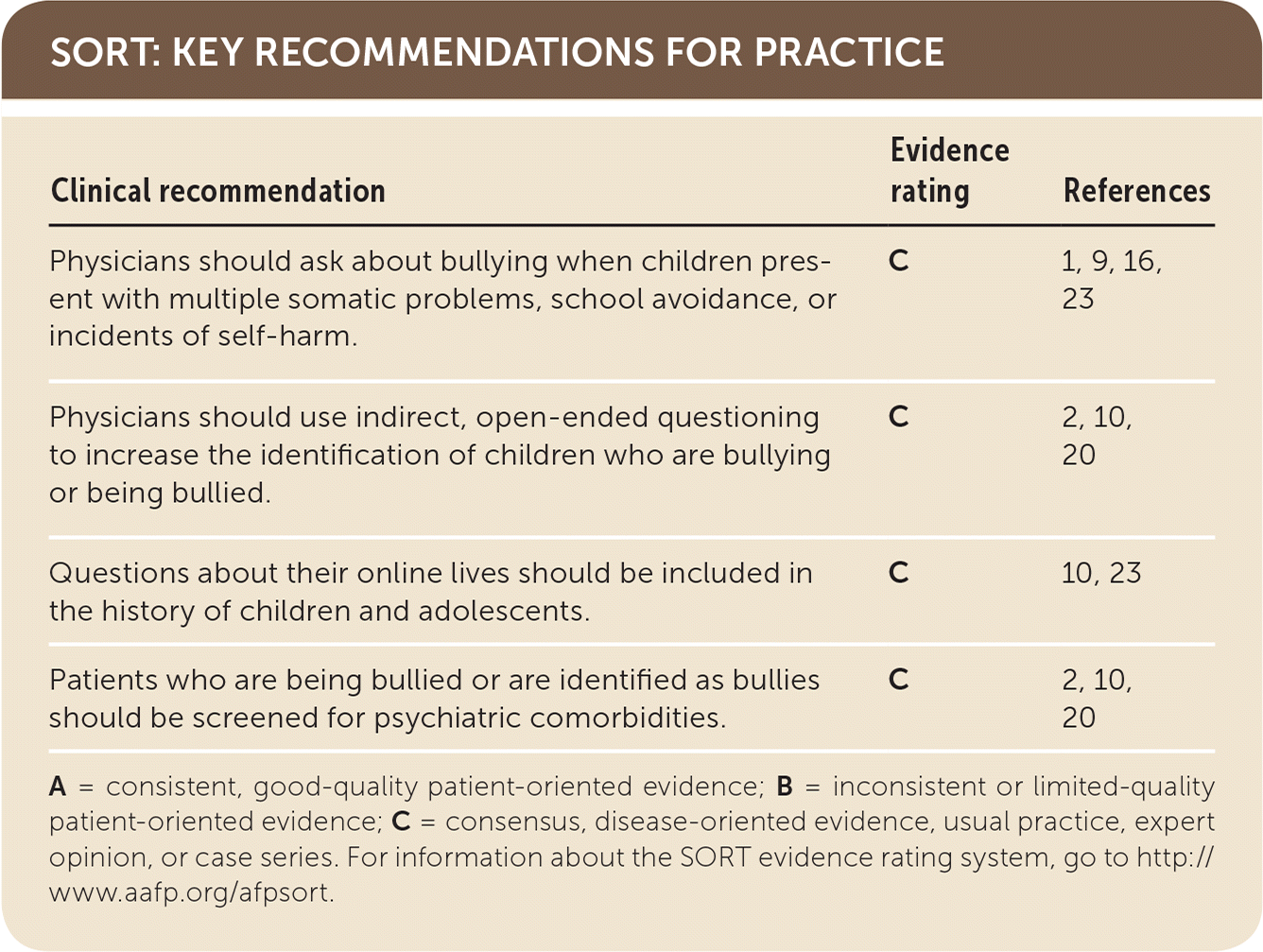
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Physicians should ask about bullying when children present with multiple somatic problems, school avoidance, or incidents of self-harm. | C | 1, 9, 16, 23 |
| Physicians should use indirect, open-ended questioning to increase the identification of children who are bullying or being bullied. | C | 2, 10, 20 |
| Questions about their online lives should be included in the history of children and adolescents. | C | 10, 23 |
| Patients who are being bullied or are identified as bullies should be screened for psychiatric comorbidities. | C | 2, 10, 20 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to http://www.aafp.org/afpsort.
Prevalence
The most recent Youth Risk Behavior Surveillance data indicate that an estimated 20% of youths were bullied on school property within the previous year, and 16% were cyberbullied.11 Bystanders or witnesses to bullying are also affected physically and emotionally, and when they are taken into account, the percentage of young people who are impacted by bullying rises to 72%.1,12
Risk Factors for Being Bullied and Characteristics of Bullies
The family physician will come into contact with bullies, victims of bullying, and bully-victims (those who are bullied and reactively bully others). Risk factors for becoming a target of bullying include being lesbian, gay, bisexual, or transgender (LGBT); having a disability or medical condition such as asthma, diabetes mellitus, a skin condition, or food allergy; or being an outlier in weight and stature.13–15 Personality traits and behavioral factors that have a role in a person becoming a bully and/or victim are summarized in Table 1.3,12,16–21
TABLE 1. Characteristics and Effects of Childhood Bullying
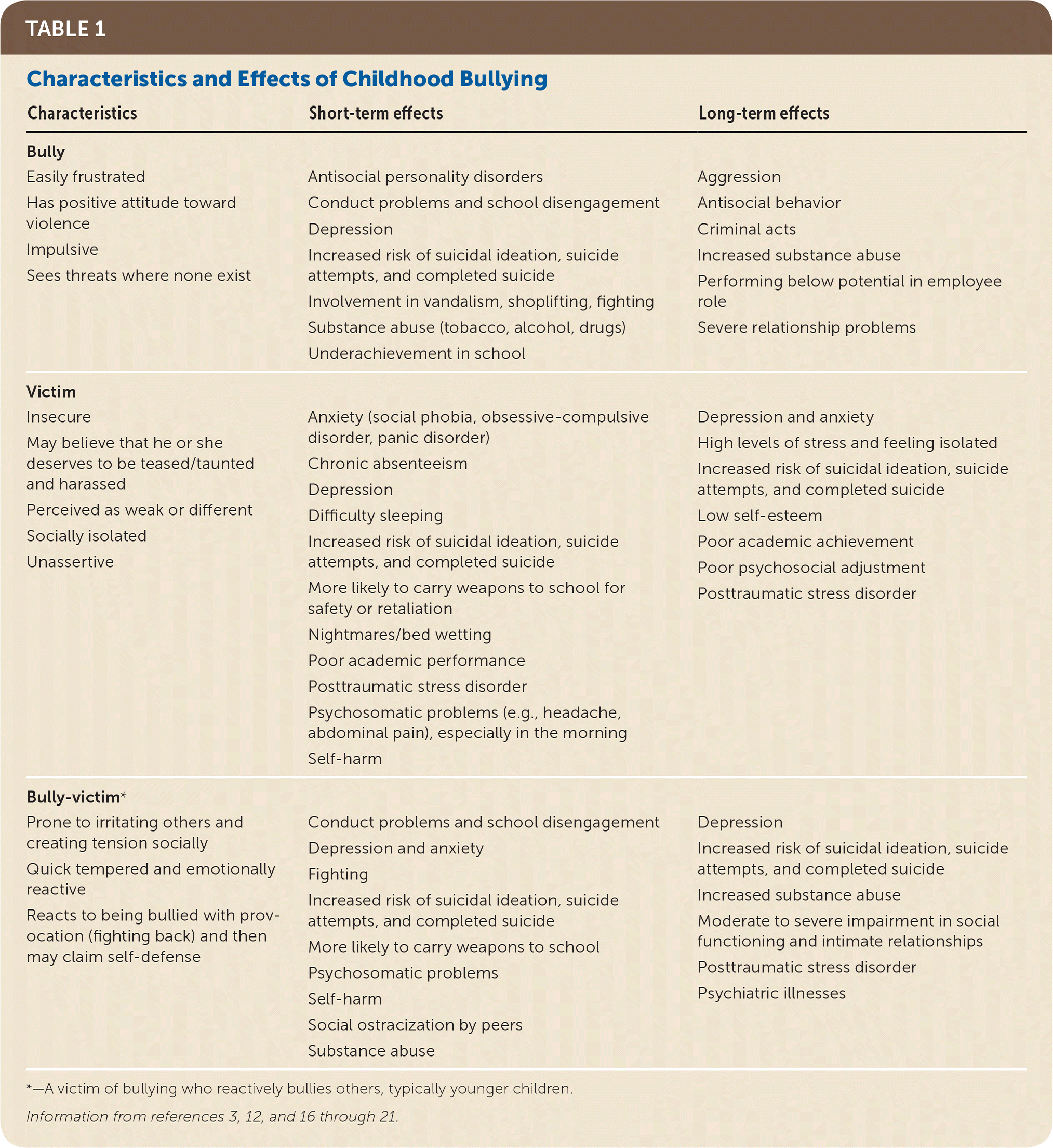
| Characteristics | Short-term effects | Long-term effects |
|---|---|---|
| Bully | ||
|
|
|
| Victim | ||
|
|
|
| Bully-victim* | ||
|
|
|
*—A victim of bullying who reactively bullies others, typically younger children.
Clinical Approach
Bullying can lead to adverse physical and mental health effects for both the victim and bully (Table 1).3,12,16–21 The bully-victim is at particularly high risk.
Bullying can result in emotional distress, depression, anxiety, social isolation, low self-esteem, school avoidance/refusal, and substance abuse for the victim and the bully.3,16,17,22–25 In addition, victims of bullying often present with multiple somatic problems, including insomnia, headaches, abdominal pain, digestive issues, disordered eating habits, dizziness, skin problems, and localized pain in the extremities.1,3,18,20,23–26 There is a direct association between bullying and low academic performance in victims because bullying leads to increased school absenteeism and reduced investment in academics.9,16 There is a significant association between bullying and incidents of self-harm and increased rates of suicidality (suicidal thoughts and attempts), especially for victims and bully-victims.2,23
Family physicians have a role in identifying and intervening in bullying by focusing on prevention, screening early for bullying, recognizing signs of bullying, and supporting patients who are affected by bullying and their families.
PREVENTION
Family physicians can provide anticipatory guidance to parents and patients during well-child visits beginning at a young age. The American Academy of Pediatrics recommends introducing the concept of bullying to parents during the six-year-old well-child visit.27 Opening a discussion about bullying can draw attention to the problem and empower patients and caregivers to seek support or additional information.28 Other preventive recommendations include providing support to patients, encouraging them to find enjoyable activities that promote confidence and self-esteem and to seek positive friendships, and modeling how to treat others with kindness and respect.9,29 Students who feel more connected to their school environments are more likely to do well in school, stay in school, and make healthy choices, and are less likely to engage in high-risk behaviors.30 The parent-child relationship is a significant predictor of a child's involvement in all roles of bullying at school.31 Interventions aimed at parents of high-risk young persons that focus on positive parenting skills can lead to decreased bullying and violent behavior.32
SCREENING
Because rates of bullying increase as a child progresses through elementary school and into middle school, early screening and identification can assist in effective prevention efforts.33 Screening can be provided for all youth patients or focus on high-risk groups.27
There are no evidence-based screening tools specific to the identification of bullying or bullies. Family physicians may consider using the HEEADSSS (home environment, education and employment, eating, peer-related activities, drugs, sexuality, suicide/depression, safety) tool as a general approach to assess risk in children and adolescents, and inquire about bullying during visits for preventive care.7,14,22,34 However, the use of electronic psychosocial assessment tools, such as the myAssessment mobile app or the Rapid Assessment for Adolescent Preventive Services, to identify high-risk behaviors may increase rates of disclosure and save time during a busy office visit.35,36
Physicians should be careful how they ask questions when assessing the risk of bullying behaviors (Table 27,17,37 ). Because children and adolescents may not realize their own involvement in bullying, using the term bully is less likely to produce disclosure than asking patients to describe the behaviors of themselves or others in an indirect, open-ended question.2,10,20 Questions about their online lives should be included in the history of youth patients.10,23 Because of the close relationship between bullying and suicidality, family physicians may also want to screen patients at risk of being bullied for coexisting depression or suicidality using evidence-based tools such as the Beck Depression Inventory-II or the Beck Scale for Suicide Ideation.38
TABLE 2. Suggested Questions for Young Patients Regarding Bullying and School Experiences

| Do you feel safe at school? (critical question) |
| How do you get along with teachers and other students? |
| Have your grades changed recently? |
| Many young people experience bullying at school or via social media. Have you ever had this happen to you or anyone you know? Or Are you or is anyone you know being bullied through social media or other electronic means? |
| Follow-up questions: Is there anyone at school or at home you can talk to about your concerns? How could your parents help you with this problem? |
Parents should be asked about any changes in behaviors or attitude their children have had at school and if they have talked to their children about bullying or witnessed their children being picked on.1 Although parental involvement in most health-related concerns is optimal, particularly for adolescents, it is also recommended that at least part of the assessment be conducted with the child alone to provide a confidential opportunity for disclosure and discussion of risk behaviors.7
THE SYMPTOMATIC PATIENT
Not all children and adolescents are willing or able to disclose their experiences related to bullying, but they may show signs of being affected by bullying. Victims of bullying may have physical and mental health problems, including headaches, abdominal pain, bed wetting, and feelings of anxiety and depression.17 Such symptoms should trigger physicians to ask about bullying. The physician showing care and concern for the patient has been identified as a predictor of disclosure.39
SUPPORT AFTER DISCLOSURE
Helping patients to disclose their experiences to their parents, if appropriate, is the first step in building a supportive network of empathy around the patient.39 Table 3 provides resources to assist physicians in counseling patients and their families about bullying, as well as the next steps to stop the bullying.
TABLE 3. Resources for More Information About Addressing Bullying
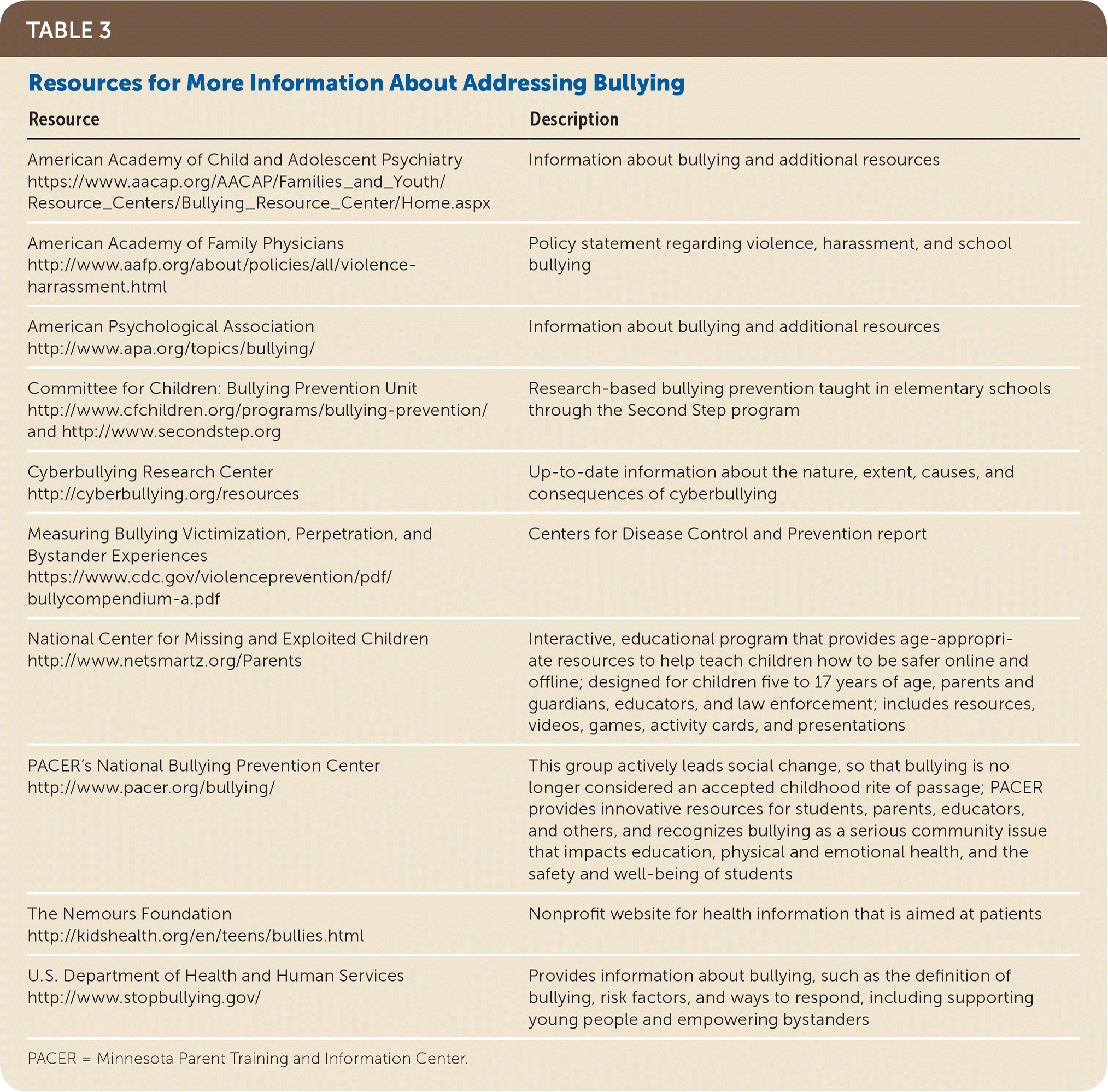
| Resource | Description |
|---|---|
| American Academy of Child and Adolescent Psychiatry https://www.aacap.org/AACAP/Families_and_Youth/Resource_Centers/Bullying_Resource_Center/Home.aspx | Information about bullying and additional resources |
| American Academy of Family Physicians http://www.aafp.org/about/policies/all/violence-harrassment.html | Policy statement regarding violence, harassment, and school bullying |
| American Psychological Association http://www.apa.org/topics/bullying/ | Information about bullying and additional resources |
| Committee for Children: Bullying Prevention Unit http://www.cfchildren.org/programs/bullying-prevention/ and http://www.secondstep.org | Research-based bullying prevention taught in elementary schools through the Second Step program |
| Cyberbullying Research Center http://cyberbullying.org/resources | Up-to-date information about the nature, extent, causes, and consequences of cyberbullying |
| Measuring Bullying Victimization, Perpetration, and Bystander Experiences https://www.cdc.gov/violenceprevention/pdf/bullycompendium-a.pdf | Centers for Disease Control and Prevention report |
| National Center for Missing and Exploited Children http://www.netsmartz.org/Parents | Interactive, educational program that provides age-appropriate resources to help teach children how to be safer online and offline; designed for children five to 17 years of age, parents and guardians, educators, and law enforcement; includes resources, videos, games, activity cards, and presentations |
| PACER's National Bullying Prevention Center http://www.pacer.org/bullying/ | This group actively leads social change, so that bullying is no longer considered an accepted childhood rite of passage; PACER provides innovative resources for students, parents, educators, and others, and recognizes bullying as a serious community issue that impacts education, physical and emotional health, and the safety and well-being of students |
| The Nemours Foundation http://kidshealth.org/en/teens/bullies.html | Nonprofit website for health information that is aimed at patients |
| U.S. Department of Health and Human Services http://www.stopbullying.gov/ | Provides information about bullying, such as the definition of bullying, risk factors, and ways to respond, including supporting young people and empowering bystanders |
PACER = Minnesota Parent Training and Information Center.
It is important to provide the parents with direct, clear information about bullying and its impact so that they are better able to engage in shared decision making and to appropriately participate in the plan to improve their child's overall health.1,27,28 For example, evidence suggests that a parent confronting another parent about bullying makes the experience worse for the victim and is not recommended.37
Once bullying has been identified, family physicians have an important role in screening for comorbid disorders, such as depression and anxiety, and in providing appropriate treatment.2,10,20 Even after disclosure has occurred, some patients may be inclined to minimize the incidents or the impact. Some mistreated or bullied children fear intensification of the abuse if they disclose the bullying or fear they will be seen unfavorably (e.g., as a tattletale) by their peers.7,18 For those who have concern or guilt for sharing their experiences, it may be useful to explain that revealing the bullying may help end the cycle not only for them, but for others as well.9,30
Cyberbullying
Children and adolescents may be more reluctant to admit they are being cyberbullied out of fear that their online time will be restricted or their electronics confiscated.2,13,23 As technology has advanced and adolescents have become more dependent on their electronic devices for social connection, restrictions can feel like further victimization and may separate them from a source of social support.
Cyberbullies are more likely to be male, and females and sexual minorities (LGBT) are more likely to be victims.2 In general, although cyberbullying is less common than traditional bullying, the two are highly correlated.10 Because cyberbullies have relative anonymity, the bullying takes place away from school grounds with possibly less adult support, and there are higher rates of suicidality with cyberbullying, effective interventions for cyberbullying are particularly important.2
Referral
Referral to a clinical social worker or psychologist may be appropriate for children and adolescents with significant psychological or mental health impairment.7 For bullying that takes place on school property, physicians should consider connecting patients and families with school-based health centers, guidance counselors, school nurses, or administrators. Although most states now have universal, school-based programs to teach all students about violence and bullying and provide skills to promote positive social interactions and conflict resolution, they do not specifically focus on identification and intervention for those at risk of becoming a bully or victim of bullying.4,14,24,40,41 Better collaboration among schools, primary care, and community-based mental health professionals to provide bullying interventions may be beneficial. A multidisciplinary collaboration between the physician, the patient, the family, the clinical social worker or psychologist, or other school personnel can assist in creating a safe network of empathy for the patient and effecting meaningful social change.14,42,43
In addition to providing direct care to patients, family physicians can make a difference by advocating for community and school-based bullying prevention, as well as effective multidisciplinary interventions for victims and bullies.9
This article updates a previous article on this topic by Lyznicki, et al.12
Data Sources: Ovid MEDLINE and PsycINFO database searches were performed using the key terms bully, bullying, screening, disclosure, intervention, and physician's role. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. We also searched the Cochrane database and the Centers for Disease Control and Prevention Community Guide. Search date: June 15, 2016.

