Developmental disabilities are attributable to a cognitive impairment, physical impairment, or both. They manifest during the developmental period from birth to early adulthood, and are likely to continue indefinitely. The life expectancy of most persons with developmental disabilities now approaches that of the general population. According to the neurodiversity model of care, developmental disability is accepted as a valued part of human neurologic diversity. The social model focuses on improving participation in society with accommodations such as adaptive equipment or improvements to the social and physical environment. The goal of health care for patients with developmental disabilities is to improve their well-being, function, and participation in family and community. Physicians should communicate directly with their patients, even those who have communication or cognitive differences. Communication may include speech, sign language, writing, letter boards, voice output devices, pictures, facial expressions, gestures, vocalizations, and behavior. Supported decision making is a paradigm, support practice, and emerging legal structure that focuses on assisting patients with communicating their wants and needs as an alternative to guardianship or power of attorney. When establishing care, it is critical to get a detailed history of baseline traits and characteristics in the areas of cognition and communication; neuromuscular function; sensory function such as vision, hearing, and sensory processing; seizure threshold; mental health; and behavior. In general, guidelines for age-appropriate health maintenance in the general population should be followed unless the risk outweighs the benefit for an individual patient. With accurate diagnosis, psychiatric conditions can be treated effectively with the same medical, behavioral, and therapeutic modalities used in the general population. Just like any patient, those with developmental disabilities should have access to a full range of life-sustaining, curative, and end-of-life services.
Developmental disabilities are attributable to a cognitive impairment, physical impairment, or both. They manifest during the developmental period from birth to early adulthood, and are likely to continue indefinitely. Developmental disabilities result in substantial functional limitations in three or more areas of major life activity, including self-care, receptive and expressive language, learning, mobility, self-direction, capacity for independent living, and economic self-sufficiency.1 Common diagnoses associated with developmental disabilities include cerebral palsy, intellectual disability, autism, and epilepsy.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Physicians can support full inclusion and access to medical care for patients with disabilities by ensuring that their practices comply with guidelines for physical access. | C | 7 |
| Supported decision making should be offered to patients with developmental disabilities as an alternative to guardianship or power of attorney. | C | 13, 14 |
| Because unrecognized and undertreated medical problems are common in persons with developmental disabilities, physicians should perform a yearly health check. | C | 28, 29 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
The life expectancy of most persons with developmental disabilities now approaches that of the general population.2 For example, the mean age of death for a person with an intellectual disability was 19 years in the 1930s and 66 years by the 1990s, and it continues to improve.2 The civil rights of persons with disabilities have also advanced as they have been fully integrated into mainstream society, including medical practices. Family physicians can help patients with developmental disabilities maximize their potential by presuming they have an ability to learn and using appropriate communication support tools. Physicians can also help by responding promptly to urgent medical problems, providing age-appropriate health maintenance, and assessing risk to prevent secondary complications.
Medical vs. Neurodiversity and Social Models of Disability
Persons with disabilities are often healthy, and disability should be distinguished from illness. In the medical model, disability is viewed as a deficiency or disease that needs to be overcome. However, persons with developmental disabilities have a wide range of strengths, challenges, and support needs. The neurodiversity and social models view disability as a natural part of the human experience. They focus on maximizing potential as opposed to normalization, and encourage individuals with disabilities to pursue their strengths while mitigating weaknesses.3 The neurodiversity model accepts developmental disability as a valued part of human neurologic diversity.4,5 The social model focuses on improving participation in society with accommodations such as adaptive equipment or improvements to the social and physical environment.6
The goal of health care for patients with developmental disabilities is to improve their well-being, function, and participation in family and community. It is not always necessary or desirable to try to change a person's traits and characteristics to make them appear or behave more normally. The distinction between the medical, neurodiversity, and social models has important implications for medical care.
For example, in the medical model, persons with a mobility impairment might receive intensive physical therapy, surgery, and braces to help them walk. In the social model, interventions might include a motorized wheelchair; wheelchair lifts, ramps, and scales; and adaptive physical education for strength and cardiovascular health. In the medical model, someone with dysarthria might be referred for speech therapy to improve articulation because people primarily communicate through speech. However, in the neurodiversity model, the individual's most effective means of communication would be accepted because his or her potential for producing clear, fluent speech might be limited, slow, and effortful. Therefore, he or she might use augmentative and alternative communication such as pointing to picture icons or typing on a keyboard, which might allow more complex thoughts to be communicated clearly and to a broader audience. He or she also might receive a voice output device to translate picture icons or text into sound. In the medical model, persons with short stature might receive growth hormone, whereas in the social or neurodiversity model, they may be referred to vocational training to pursue a career that interests them and for which they can perform the essential functions with or without accommodations.
Accommodations and Access
Regardless of functional limitations, with appropriate medical care, accommodations, and decision-making support, persons with developmental disabilities can live quality lives in their own homes and communities. Accommodations can include disability services, housing modifications, and adaptive equipment. Physicians can support full inclusion and access to medical care for patients with disabilities by ensuring that their practices comply with guidelines for physical access.7 This may require investments in adaptive equipment, such as wheelchair scales and lifts and high-low examination tables, and implementation of programmatic changes, such as longer appointments, reduced wait times, and home visits. For some patients, access can be improved with changes to the sensory environment, such as eliminating strong scents, and turning down alarms, televisions, and fluorescent or bright lights.7
Approach to Communication and Supported Decision Making
Communication is the foundation of patient care. Communication can include speech, sign language, writing, letter boards, voice output devices, pictures, facial expressions, gestures, vocalizations, and behavior.8 The physician should first note the patient's intent because, for example, not all movements are meant to be communication. Persons with cerebral palsy or autism may have difficulty controlling movements, and these involuntary movements can be impulsive or reflect difficulty with inertia. This can be misinterpreted as intellectual disability, lack of interest, aggression, or defiance.9,10 Physicians should communicate directly with their patients, even those who have communication or cognitive differences. Gathering information directly from patients, as much as possible, is important because only they can report on their internal thoughts and symptoms. Patient perspectives may differ from that of family members, supporters, or physicians (see a related Close-ups piece previously published in American Family Physician at https://www.aafp.org/afp/2009/0601/p955.html). With direct, respectful communication, a more accurate history can be obtained (Table 1).
TABLE 1. Communicating Respect When Interacting with Patients with Developmental Disabilities and Their Supporters
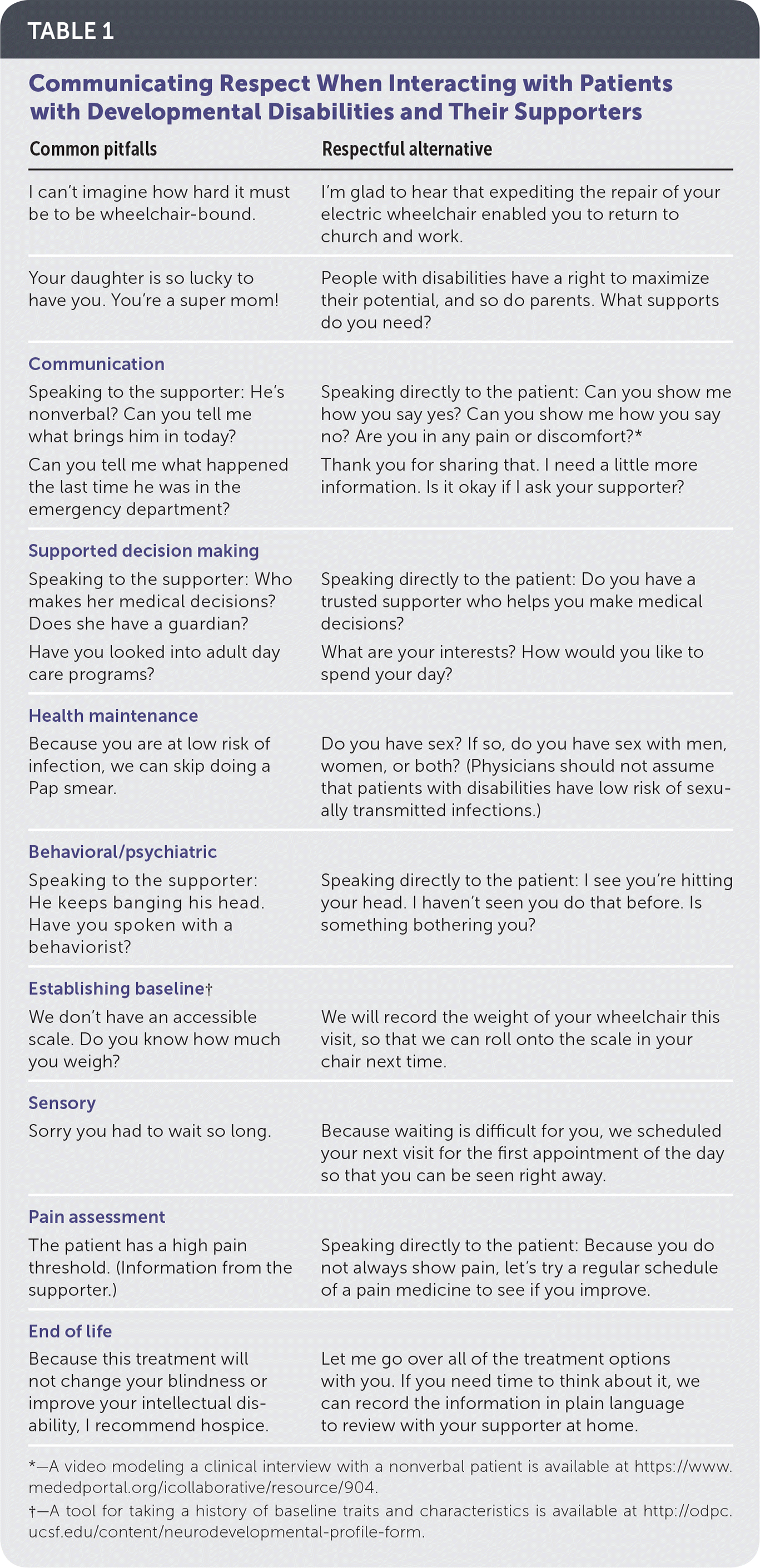
| Common pitfalls | Respectful alternative |
|---|---|
| I can't imagine how hard it must be to be wheelchair-bound. | I'm glad to hear that expediting the repair of your electric wheelchair enabled you to return to church and work. |
| Your daughter is so lucky to have you. You're a super mom! | People with disabilities have a right to maximize their potential, and so do parents. What supports do you need? |
| Communication | |
| Speaking to the supporter: He's nonverbal? Can you tell me what brings him in today? | Speaking directly to the patient: Can you show me how you say yes? Can you show me how you say no? Are you in any pain or discomfort?* |
| Can you tell me what happened the last time he was in the emergency department? | Thank you for sharing that. I need a little more information. Is it okay if I ask your supporter? |
| Supported decision making | |
| Speaking to the supporter: Who makes her medical decisions? Does she have a guardian? | Speaking directly to the patient: Do you have a trusted supporter who helps you make medical decisions? |
| Have you looked into adult day care programs? | What are your interests? How would you like to spend your day? |
| Health maintenance | |
| Because you are at low risk of infection, we can skip doing a Pap smear. | Do you have sex? If so, do you have sex with men, women, or both? (Physicians should not assume that patients with disabilities have low risk of sexually transmitted infections.) |
| Behavioral/psychiatric | |
| Speaking to the supporter: He keeps banging his head. Have you spoken with a behaviorist? | Speaking directly to the patient: I see you're hitting your head. I haven't seen you do that before. Is something bothering you? |
| Establishing baseline† | |
| We don't have an accessible scale. Do you know how much you weigh? | We will record the weight of your wheelchair this visit, so that we can roll onto the scale in your chair next time. |
| Sensory | |
| Sorry you had to wait so long. | Because waiting is difficult for you, we scheduled your next visit for the first appointment of the day so that you can be seen right away. |
| Pain assessment | |
| The patient has a high pain threshold. (Information from the supporter.) | Speaking directly to the patient: Because you do not always show pain, let's try a regular schedule of a pain medicine to see if you improve. |
| End of life | |
| Because this treatment will not change your blindness or improve your intellectual disability, I recommend hospice. | Let me go over all of the treatment options with you. If you need time to think about it, we can record the information in plain language to review with your supporter at home. |
*—A video modeling a clinical interview with a nonverbal patient is available at https://www.mededportal.org/icollaborative/resource/904.
†—A tool for taking a history of baseline traits and characteristics is available at http://odpc.ucsf.edu/content/neurodevelopmental-profile-form.
Even with the best efforts, it is not always possible to accurately interpret someone's verbal or nonverbal communication. However, success rates improve with practice and employing a variety of strategies, such as establishing how a patient communicates yes and no, offering choices, or allowing extra time for the patient to respond. Using communication aids, such as plain language, picture supports, demonstrations, and alternative formats (e.g., electronic readers; large print; translations, such as into braille or the reader's native language) may be helpful. If a communication attempt is unsuccessful, future attempts are still important. At a minimum, patients should be included in discussions about decisions that impact them. At those meetings, physicians and others present should communicate directly with patients, even if they do not reliably respond.11 For patients who do not have an effective method of expressive communication, a toolkit to assist with accessing communication assessments, adaptive equipment, and augmentative and alternative communication is available at http://odpc.ucsf.edu/communications-paper.
Individuals who accompany patients to appointments or who provide personal assistance have traditionally been called caregivers. However, the term supporter can encourage person-centered thinking that respects the patient's autonomy, even if the patient requires assistance to communicate or make decisions.12 Supporters are helpful in a variety of ways. They can provide ancillary information, translate or interpret unclear speech or nonverbal communication, and break down concepts in a way the patient can understand. They can also report back if the patient needs time to process information outside of the appointment or help implement the health care plan. When a supporter speaks for a patient and the physician is unable to confirm the information directly with the patient, he or she can clarify the authenticity of the information by asking the supporter, “How do you know?” or “Did you ask the patient?” A video on working with persons who cannot communicate clearly is available at http://www.uctv.tv/shows/When-Listening-is-Complicated-Skills-for-Honoring-the-Individual-Perspectives-of-Every-Person-with-Disabilities-32191.
Supported decision making is a paradigm, support practice, and emerging legal structure that focuses on assisting patients with communicating their wants and needs. It is an alternative to guardianship or power of attorney, which rely on the opinion of a third party to determine what is in the patient's best interest.13,14 With supported decision making, patients retain their legal capacity. Instead of transferring decision making to a power of attorney or having a judge or hospital protocol assign a proxy decision maker, patients choose one or more supporters they trust, select the type of support they want, and receive help to make decisions or to communicate. Supported decision making acknowledges that a person's capacity fluctuates, while assuming that the ability to make and communicate choices often improves with support.
Even without disabilities, learning to make decisions in one's own best interest takes practice, some risk-taking, and learning from mistakes.13,14 For example, few adults would make all of the same decisions they did when they were younger because they have had the opportunity to learn from their experiences. Supported decision making affords persons with disabilities the same opportunity. eTable A includes resources for more information about supported decision making.
eTABLE A Resources on Supported Decision Making for Persons with Developmental Disabilities
| American Bar Association |
| American Civil Liberties Union |
| Autistic Self Advocacy Network |
| National Resource Center for Supported Decision-Making |
| Office of Developmental Primary Care |
| United Nations Convention on the Rights of Persons with Disabilities Article 12: Equal Recognition Before the Law |
Baseline Traits and Characteristics
In patients with complex disabilities, illness often presents as a change in behavior or function. Therefore, when establishing care, it is critical to get a detailed history of baseline traits and characteristics in the areas of cognition and communication; neuromuscular function; sensory function such as vision, hearing, and sensory processing; seizure threshold; mental health; and behavior. This baseline assessment will also help determine whether the patient is at risk of secondary medical problems and which primary and secondary prevention strategies, accommodations, and adaptive equipment are most likely to be beneficial (Table 215–24 ).
TABLE 2. Tips for Prevention and Treatment of Common Medical Problems in Patients with Developmental Disabilities

Gastrointestinal (constipation)
| Oral
|
Musculoskeletal
| Respiratory care
|
Neurologic
| Skin
|
Most adults with developmental disabilities have had genetic, diagnostic, cognitive, speech, occupational, physical, educational, vocational, or developmental assessments. If assessments are outdated, referrals may be warranted. Accurate and thorough record keeping is critical because patients and supporters may not be able to provide a detailed medical history. Some conditions, such as dementia, may be more difficult to diagnose in the future without this baseline information. Systematically comparing current with past function is essential to recognizing treatable medical problems and rehabilitation potential.
Each area of function should be assessed independently because deficits in one area can be mistaken for deficits in another. For example, many patients who cannot speak or hear are assumed to have intellectual disabilities. Patients who routinely use wheelchairs to attend medical appointments may also be able to stand, walk, or crawl up stairs. Strengths in one area can mask challenges in another. For example, a patient who is fluently conversational may have significant problems with basic activities of daily living because of issues with memory or executive function that are not apparent in an examination room.
Health Maintenance
In general, guidelines for age-appropriate health maintenance in the general population should be followed for those with developmental disabilities unless the risk outweighs the benefit for an individual patient. In addition, because targeted physical examination and diagnostic testing may be less reliable in persons with communication, sensory, or cognitive challenges, physicians should be proactive at health maintenance visits to identify possible health problems with a complete history, physical examination, screening tests, and functional assessment.25,26 Because of risk factors for dental problems in persons with developmental disabilities (eTable B), preventive dental care is paramount.27
eTABLE B Risk Factors for Tooth and Gum Disease

Barriers to accessing dental care
|
Barriers to adequate hygiene
|
Chronic gastroesophageal reflux causing damage to the enamel
|
Habits
|
Medications
|
Trauma causing broken teeth
|
Information from U.S. Department of Health and Human Services. National Institute of Dental and Craniofacial Research. Developmental disabilities and oral health. http://www.nidcr.nih.gov/health-info/developmental-disabilities/more-info. Accessed April 18, 2017.
Studies of comprehensive yearly health checks in persons with developmental disabilities reveal that unrecognized and undertreated medical problems are common.28 Illnesses are often recognized later in the disease process, and atypical presentations of illness may not be triaged appropriately. Examples of presenting signs and symptoms of commonly unrecognized and undertreated conditions in patients with developmental disabilities are included in Table 3. Ensuring timely care may require more frequent office visits and adjustments to office protocols.29 Table 4 includes toolkits to help physicians optimize care for patients with developmental disabilities.
TABLE 3. Common Unrecognized or Undertreated Medical Problems in Persons with Developmental Disabilities

| Medical problem | Possible presentations in nonverbal patients |
|---|---|
| Abuse or neglect | Aggression, defiance, withdrawal, meltdowns |
| Constipation | Small stools, liquid stools, soiling, rectal digging, urinary retention |
| Deconditioning | Worsening contractures, constipation, decreased mobility |
| Dental caries or periodontal disease | Feeding problems, head banging, agitation |
| Drug or alcohol use | Memory loss, confabulation, unsteady gait |
| Dysphagia/microaspiration | Shortness of breath or cough with or after meals, slight elevation of body temperature, tachycardia |
| Endocrine or metabolic disorders (especially hypothyroidism and syndrome of inappropriate antidiuretic hormone) | Sedation, changes in drug metabolism |
| Kidney or gallstones | Urinary retention, irritability |
| Medication adverse effects/polypharmacy | Behavior problems, sedation, paradoxical reactions, atypical drug metabolism |
| Nutritional deficiency | Amenorrhea, spontaneous fractures, constipation, pressure sores |
| Occult fractures or injuries, arthritis, nerve compression, osteoporosis | Changes in mobility, sedation |
| Pain syndromes | Irritability; insomnia; decreased participation; change in function; aggression; scratching, banging, or touching the body part that hurts |
| Rashes | Irritability |
| Seizures, including less common seizure types | Emotional lability, unresponsiveness, fatigue, automatisms |
| Sleep apnea | Elevated hematocrit, sedation |
| Urinary retention | Grabbing genitals, abdominal distention, urinary tract infections |
| Urinary tract infections | Irritability, aggression, sedation |
| Vision and hearing deficits | Decreased participation or mobility; easily startled; aggression |
TABLE 4. Toolkits to Help Optimize Care for Patients with Developmental Disabilities
| Academic-Autistic Spectrum Partnership in Research and Education Healthcare Toolkit: resources for adults on the autism spectrum and their primary care providers; includes a tool for creating a personalized accommodation letter |
| American Academy for Cerebral Palsy Developmental Medicine: care pathways, fact sheets, systematic reviews |
| Autistic Self Advocacy Network: resources for accessing home and community-based services and resources on nondiscrimination, transition, communication, and exercising rights |
| Coalition for Compassionate Care of California: advance care planning for persons with developmental disabilities |
| Health Care for Adults with Intellectual and Developmental Disabilities: clinical algorithms |
| Massachusetts Department of Developmental Services: 2017 adult screening recommendations |
| National Institute of Dental and Craniofacial Research: information about providing dental care for persons with developmental disabilities |
| University of California, San Francisco, Office of Developmental Primary Care: chart forms, training materials, practice pearls |
Sexual Health
Persons with developmental disabilities can and do have sex, marry, and have children.30,31 They have a full range of sexual orientations. Gender dysphoria has been found to be particularly common among persons with autism.32 Adults with developmental disabilities should receive sex education and access to a full range of reproductive services.33
Pain Assessment
Because pain is an internal sensation, communication difficulties can complicate the assessment. Persons with developmental disabilities often have atypical behavior in response to pain. For example, they may not grimace, cry, or clutch the part of the body that hurts. Supporters often report that patients with developmental disabilities have a high pain threshold. This interpretation may be accurate because of atypical sensory processing, or the patient may feel the pain but does not show recognizable signs of distress. Conversely, some persons with developmental disabilities may be sensitive to normally benign stimuli such as touch, sounds, or abrupt changes in light, which create painful sensations. Empiric trials of pain medication may be necessary when assessment is uncertain.
Psychiatric and Behavioral Concerns
Persons with developmental disabilities have high rates of psychiatric problems.34 The Diagnostic and Statistical Manual for Intellectual Disability (DSM-ID-2) can assist physicians in making psychiatric diagnoses in persons with intellectual disabilities who may have atypical signs and symptoms.35 Generally, with accurate diagnosis, psychiatric conditions in patients with developmental disabilities can be managed effectively with the same range of medical, behavioral, and therapeutic modalities used to treat these conditions in the general population.36
When assessing maladaptive behaviors, it is important to evaluate and treat the cause rather than merely suppress the behavior. Maladaptive behavior is often a manifestation of a medical or environmental problem, and is an opportunity to improve communication or to provide a better way to make sure the patient's needs are being met.
When interpreting behavior, it is important to consider the patient's ability to respond to potential mis-treatment or abuse. Some persons with developmental disabilities have had extensive educational and therapeutic interventions focused on improving their compliance with the expectations of authority figures such as parents and teachers.
Persons with developmental disabilities who have been taught to comply, especially those who need assistance with activities of daily living, may not have been encouraged or taught to set personal boundaries or to recognize or communicate when they are being mistreated or abused. These patients may be particularly vulnerable.
End-of-Life Care
Supported decision-making principles are particularly important when patients are facing a life-threatening illness. Terminal illness does not have to lead to a loss of autonomy, dignity, relationships, housing, or self-determination. Persons with developmental disabilities typically report higher quality of life than is perceived by others who are not disabled.37 Awareness of unconscious bias and how it can influence goals of care conversations is paramount.38 Family physicians can help hospital teams distinguish patients who have significant functional limitations but who are relatively healthy from patients who have serious, progressive illnesses. Family physicians are important advocates for their patients to access a full range of life-sustaining, curative, palliative care, and hospice services.
This article updates a previous article on this topic by Prater and Zylstra.39
Data Sources: A PubMed search was completed in Clinical Queries using the key terms supported decision making and developmental disability. The search included systematic reviews, randomized controlled trials, and clinical trials. Also searched were Essential Evidence Plus, the Canadian Task Force on Preventive Health Care, National Guideline Clearinghouse, Cochrane Database of Systematic Reviews, and the Agency for Healthcare Research and Quality Clinical Guidelines and Evidence Reports. Search date: January 4, 2017.

