Summary of Recommendation and Evidence
The USPSTF recommends that clinicians offer or refer adults with a body mass index (BMI) of 30 or higher (calculated as weight in kilograms divided by height in meters squared) to intensive, multicomponent behavioral interventions (Table 1). B recommendation.
TABLE 1. Behavioral Weight Loss Interventions to Prevent Obesity-Related Morbidity and Mortality in Adults: Clinical Summary of the USPSTF Recommendation
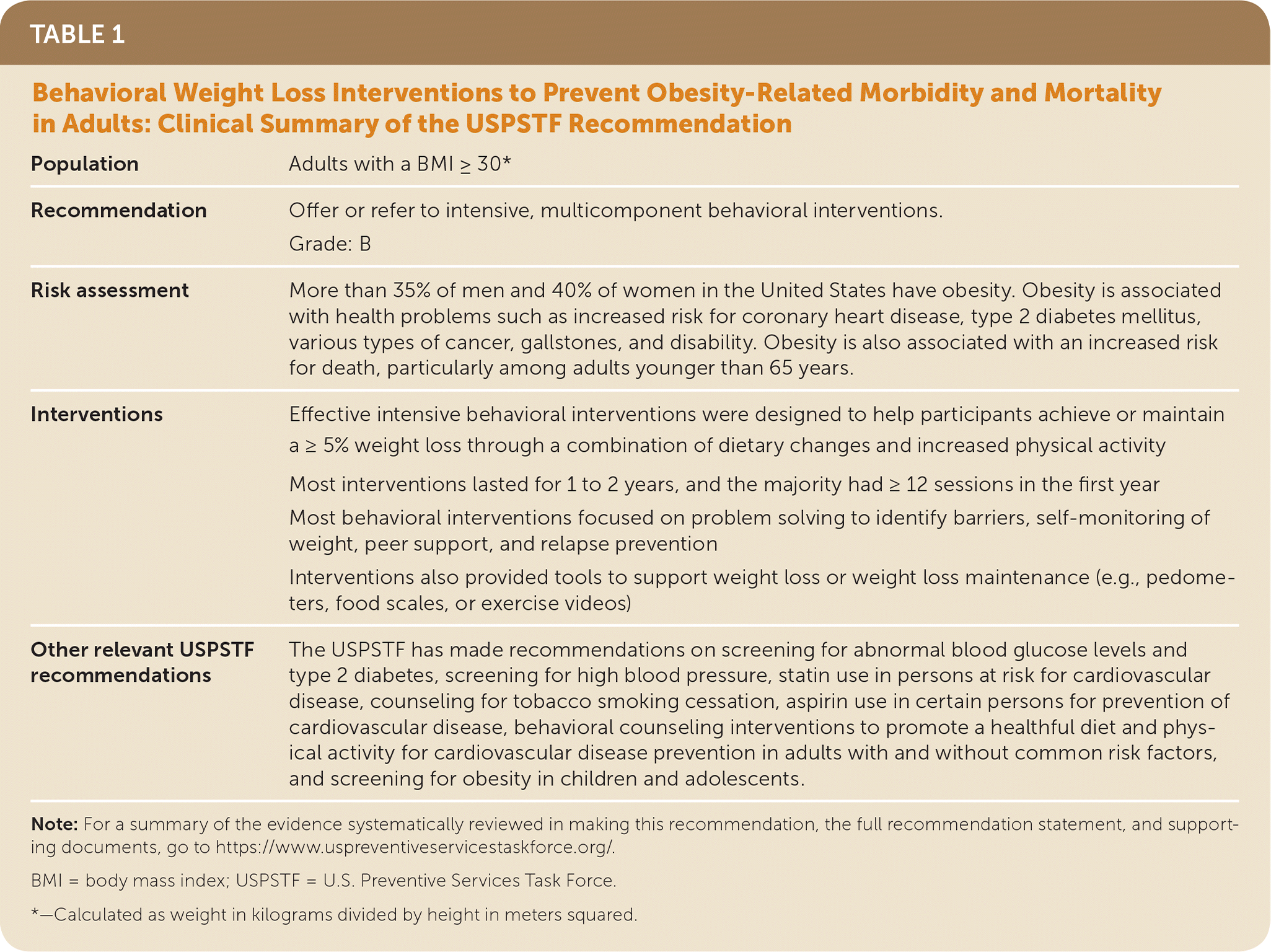
| Population | Adults with a BMI ≥ 30* |
| Recommendation | Offer or refer to intensive, multicomponent behavioral interventions. Grade: B |
| Risk assessment | More than 35% of men and 40% of women in the United States have obesity. Obesity is associated with health problems such as increased risk for coronary heart disease, type 2 diabetes mellitus, various types of cancer, gallstones, and disability. Obesity is also associated with an increased risk for death, particularly among adults younger than 65 years. |
| Interventions | Effective intensive behavioral interventions were designed to help participants achieve or maintain a ≥ 5% weight loss through a combination of dietary changes and increased physical activity Most interventions lasted for 1 to 2 years, and the majority had ≥ 12 sessions in the first year Most behavioral interventions focused on problem solving to identify barriers, self-monitoring of weight, peer support, and relapse prevention Interventions also provided tools to support weight loss or weight loss maintenance (e.g., pedometers, food scales, or exercise videos) |
| Other relevant USPSTF recommendations | The USPSTF has made recommendations on screening for abnormal blood glucose levels and type 2 diabetes, screening for high blood pressure, statin use in persons at risk for cardiovascular disease, counseling for tobacco smoking cessation, aspirin use in certain persons for prevention of cardiovascular disease, behavioral counseling interventions to promote a healthful diet and physical activity for cardiovascular disease prevention in adults with and without common risk factors, and screening for obesity in children and adolescents. |
Note: For a summary of the evidence systematically reviewed in making this recommendation, the full recommendation statement, and supporting documents, go to https://www.uspreventiveservicestaskforce.org/.
BMI = body mass index; USPSTF = U.S. Preventive Services Task Force.
*—Calculated as weight in kilograms divided by height in meters squared.
Rationale
IMPORTANCE
More than 35% of men and 40% of women in the United States are obese.1,2 Obesity is associated with health problems such as increased risk for coronary heart disease, type 2 diabetes mellitus, various types of cancer, gallstones, and disability.1,3–7 Obesity is also associated with an increased risk for death, particularly among adults younger than 65 years.1 The leading causes of death among adults with obesity include ischemic heart disease, type 2 diabetes, respiratory diseases, and cancer (e.g., liver, kidney, breast, endometrial, prostate, and colon cancers).1,3,8–12
BENEFITS OF BEHAVIORAL COUNSELING INTERVENTIONS
The USPSTF found adequate evidence that behavior-based weight loss interventions in adults with obesity can lead to clinically significant improvements in weight status and reduced incidence of type 2 diabetes among adults with obesity and elevated plasma glucose levels. The USPSTF found adequate evidence that behavior-based weight loss maintenance interventions are associated with less weight gain after the cessation of interventions, compared with control groups. The magnitude of these benefits is moderate.
HARMS OF BEHAVIORAL COUNSELING INTERVENTIONS
The USPSTF found adequate evidence to bound the harms of intensive, multicomponent behavioral interventions (i.e., behavior-based weight loss and weight loss maintenance interventions) in adults with obesity as small to none, based on the absence of reported harms in the evidence and the noninvasive nature of the interventions. When direct evidence is limited, absent, or restricted to select populations or clinical scenarios, the USPSTF may place conceptual upper or lower bounds on the magnitude of benefit or harms.
USPSTF ASSESSMENT
The USPSTF concludes with moderate certainty that offering or referring adults with obesity to intensive, multicomponent behavioral interventions (i.e., behavior-based weight loss and weight loss maintenance interventions) has a moderate net benefit.
Clinical Considerations
PATIENT POPULATION UNDER CONSIDERATION
This recommendation applies to adults 18 years or older. The USPSTF uses the following terms to define categories of increased BMI: overweight is a BMI of 25 to 29.9, and obesity is a BMI of 30 or higher. Obesity can be categorized as class 1 (BMI of 30.0 to 34.9), class 2 (BMI of 35.0 to 39.9), or class 3 (BMI ≥ 40) (see Table 213 for other USPSTF recommendations related to weight).
TABLE 2. Summary of Related USPSTF Recommendations

| Population | Normal weight (BMI 18.5 to < 25)* | Overweight (BMI 25 to < 30)* | Obese (BMI ≥ 30)* |
|---|---|---|---|
| No hypertension, dyslipidemia, or abnormal blood glucose levels | Individualize the decision to provide or refer to behavioral counseling | Individualize the decision to provide or refer to behavioral counseling | Provide or refer to intensive behavioral counseling |
| Hypertension, dyslipidemia, or both | Individualize the decision to provide or refer to behavioral counseling | Provide or refer to intensive behavioral counseling | Provide or refer to intensive behavioral counseling |
| Abnormal blood glucose levels or diabetes mellitus | Provide or refer to intensive behavioral counseling† | Provide or refer to intensive behavioral counseling | Provide or refer to intensive behavioral counseling |
BMI = body mass index; USPSTF = U.S. Preventive Services Task Force.
*—BMI calculated as weight in kilograms divided by height in meters squared.
†—The USPSTF recommends screening for abnormal blood glucose levels as part of cardiovascular risk assessment in adults aged 40 to 70 years who are overweight or have obesity. Patients with certain risk factors (family history of diabetes, personal history of gestational diabetes or polycystic ovarian syndrome, or being a member of certain racial/ethnic groups [African American, American Indian or Alaska Native, Asian American, Hispanic or Latino, or Native Hawaiian or Pacific Islander]) may also be at increased risk of diabetes at a younger age or at a lower BMI and should be considered for screening.13
BEHAVIORAL COUNSELING INTERVENTIONS
Many of the effective intensive behavioral interventions considered by the USPSTF were designed to help participants achieve or maintain a 5% or greater weight loss through a combination of dietary changes and increased physical activity. The U.S. Food and Drug Administration considers a weight loss of 5% as clinically important.1
Most of the intensive behavioral weight loss interventions considered by the USPSTF lasted for 1 to 2 years, and the majority had 12 or more sessions in the first year.1 One-third of the interventions had a core phase (ranging from 3–12 months) followed by a support or maintenance phase (ranging from 9–12 months).1 Most behavioral interventions encouraged self-monitoring of weight and provided tools to support weight loss or weight loss maintenance (e.g., pedometers, food scales, or exercise videos).1 Similar behavior change techniques and weight loss messages were used across the trials.1 Some trials provided interventions modeled after the Diabetes Prevention Program lifestyle intervention for use in a primary care or community setting.1 Study heterogeneity, trial quality, and differences in populations and settings made it difficult to identify the most effective intervention characteristics (e.g., number of sessions, in-person vs remote sessions, or group- vs individual-based).1 Benefits may depend on tailoring interventions to social, environmental, and individual factors.
Interventionists varied across the trials, and interventions included varied interactions with a primary care clinician. Primary care clinician involvement ranged from limited interactions with participants in interventions conducted by other practitioners or individuals (i.e., group-based interventions conducted by lifestyle coaches or registered dietitians) to reinforcing intervention messages through brief counseling sessions.1 Few interventions included a primary care clinician as the primary interventionist over 3 to 12 months of individual counseling. In the trials not involving a primary care clinician, the interventionists were highly diverse and included behavioral therapists, psychologists, registered dietitians, exercise physiologists, lifestyle coaches, and other staff. The majority of the trials focused on individual participants, but a few interventions invited family members to participate.1
Trials used various delivery methods (group, individual, mixed, and technology- or print-based). Group-based interventions ranged from 8 group sessions over 2.5 months to weekly group sessions over 1 year (median, 23 total sessions in the first year). These interventions consisted of classroom-style sessions lasting 1 to 2 hours.1 Within the group-based interventions, some trials offered supplemental support with 1 brief individual counseling session, while other trials provided referral and free access to commercially available group-based weight loss programs.
Most of the individual-based interventions provided individual counseling sessions, with or without ongoing telephone support.1 The remaining interventions were provided remotely through telephone counseling calls (average time, 15–30 minutes) and web-based self-monitoring and support. The median number of sessions in the first year for individual-based interventions was 12.1
Mixed interventions included comparatively equal numbers of group- and individual-based counseling sessions, with or without other forms of support (e.g., telephone-, print-, or web-based). Most of these interventions took place for more than 1 year and involved more than 12 sessions (median, 23 total sessions in the first year).
Among technology-based interventions, intervention components included computer- or web-based intervention modules,1 web-based self-monitoring, mobile phone–based text messages, smartphone applications, social networking platforms, or DVD learning. Only 1 trial delivered its intervention through print-based tailored materials.1
Rates of participant adherence were generally high.1 More than two-thirds of study participants completed interventions. In addition, all study participants completed more than two-thirds of the intervention. Participation rates did decline over time.1
Behavior-based weight loss maintenance trials were designed to maintain weight loss by continuing dietary changes and physical activity.1 Interventions included group interventions, technology-based individual counseling sessions, or a combination of individual and group counseling. Most weight loss maintenance interventions lasted for 12 to 18 months; the majority of interventions had more than 12 sessions in the first year.1 Intervention components focused on nutrition, physical activity, self-monitoring, identifying barriers, problem solving, peer support, and relapse prevention.1 Participants used tools such as food diaries and pedometers to help maintain weight loss.1
Interventions that combined pharmacotherapy with behavioral interventions reported greater weight loss and weight loss maintenance over 12 to 18 months compared with behavioral interventions alone.1 However, the participants in the pharmacotherapy trials were required to meet highly selective inclusion criteria, including adherence to taking medications and meeting weight loss goals before enrollment. These trials also had high attrition.1 Therefore, it is unclear how well patients tolerate these medications and whether the findings from these trials are applicable to the general U.S. primary care population. In addition, data were lacking about the maintenance of improvement after discontinuation of pharmacotherapy.1 As a result, the USPSTF encourages clinicians to promote behavioral interventions as the primary focus of effective interventions for weight loss in adults.
ADDITIONAL APPROACHES TO PREVENTION
The USPSTF has made recommendations on screening for abnormal blood glucose levels and type 2 diabetes,13 screening for high blood pressure,14 statin use in persons at risk for cardiovascular disease,15 counseling for tobacco smoking cessation,16 aspirin use in certain persons for prevention of cardiovascular disease,17 and behavioral counseling interventions to promote a healthful diet and physical activity for cardiovascular disease prevention in adults with and without common risk factors18,19 (Table 213 ). The USPSTF recommends that clinicians screen for obesity in children 6 years or older and offer or refer them to a comprehensive, intensive behavioral intervention (B recommendation).20
USEFUL RESOURCES
The Community Preventive Services Task Force recommends multicomponent interventions that use technology-supported coaching or counseling to help adults lose weight and maintain weight loss.21
This summary is one in a series excerpted from the Recommendation Statements released by the USPSTF. These statements address preventive health services for use in primary care clinical settings, including screening tests, counseling, and preventive medications.
The complete version of this statement, including supporting scientific evidence, evidence tables, grading system, members of the USPSTF at the time this recommendation was finalized, and references, is available on the USPSTF website at https://www.uspreventiveservicestaskforce.org/.

