Key Clinical Issue
Which noninvasive nonpharmacologic treatments for chronic neck pain improve function or pain for at least one month?
Evidence-Based Answer
Combination exercise (including three of four exercise categories: muscle performance, mobility, muscle reeducation, and aerobic) slightly improves function and pain in the short term (one to less than six months). (Strength of Recommendation [SOR]: B, based on inconsistent or limited-quality patient-oriented evidence.) Low-level laser therapy moderately improves function and pain in the short term. (SOR: B, based on inconsistent or limited-quality patient-oriented evidence.) Acupuncture slightly improves function in the short and intermediate term (six to less than 12 months) but is not more effective than sham acupuncture for pain. (SOR: B, based on inconsistent or limited-quality patient-oriented evidence.) The Alexander technique, a mind-body practice, slightly improves function in the short and intermediate term. (SOR: B, based on inconsistent or limited-quality patient-oriented evidence.) Massage does not improve function in the short or intermediate term. (SOR: B, based on inconsistent or limited-quality patient-oriented evidence.) Physical therapist–led relaxation techniques do not improve pain or function when compared with no treatment or advice alone.1 (SOR: B, based on inconsistent or limited-quality patient-oriented evidence.)
CLINICAL BOTTOM LINE
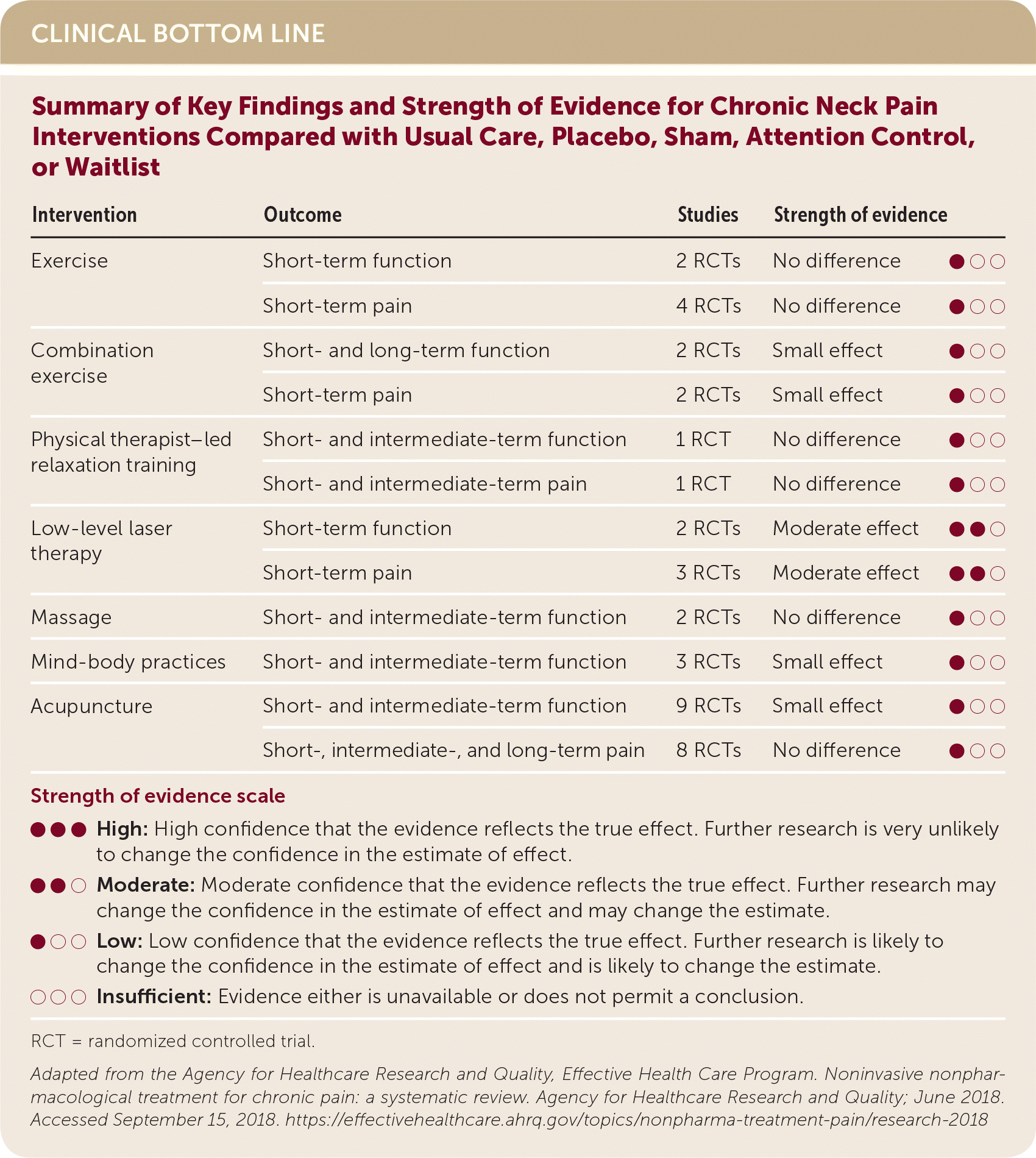
| Summary of Key Findings and Strength of Evidence for Chronic Neck Pain Interventions Compared with Usual Care, Placebo, Sham, Attention Control, or Waitlist | ||||
| Intervention | Outcome | Studies | Strength of evidence | |
|---|---|---|---|---|
| Exercise | Short-term function | 2 RCTs | No difference | ● ○ ○ |
| Short-term pain | 4 RCTs | No difference | ● ○ ○ | |
| Combination exercise | Short- and long-term function | 2 RCTs | Small effect | ● ○ ○ |
| Short-term pain | 2 RCTs | Small effect | ● ○ ○ | |
| Physical therapist–led relaxation training | Short- and intermediate-term function | 1 RCT | No difference | ● ○ ○ |
| Short- and intermediate-term pain | 1 RCT | No difference | ● ○ ○ | |
| Low-level laser therapy | Short-term function | 2 RCTs | Moderate effect | ● ● ○ |
| Short-term pain | 3 RCTs | Moderate effect | ● ● ○ | |
| Massage | Short- and intermediate-term function | 2 RCTs | No difference | ● ○ ○ |
| Mind-body practices | Short- and intermediate-term function | 3 RCTs | Small effect | ● ○ ○ |
| Acupuncture | Short- and intermediate-term function | 9 RCTs | Small effect | ● ○ ○ |
| Short-, intermediate-, and long-term pain | 8 RCTs | No difference | ● ○ ○ | |
Strength of evidence scale
● ● ● High: High confidence that the evidence reflects the true effect. Further research is very unlikely to change the confidence in the estimate of effect.
● ● ○ Moderate: Moderate confidence that the evidence reflects the true effect. Further research may change the confidence in the estimate of effect and may change the estimate.
● ○ ○ Low: Low confidence that the evidence reflects the true effect. Further research is likely to change the confidence in the estimate of effect and is likely to change the estimate.
○ ○ ○ Insufficient: Evidence either is unavailable or does not permit a conclusion.
RCT = randomized controlled trial.
Adapted from the Agency for Healthcare Research and Quality, Effective Health Care Program. Noninvasive nonpharmacological treatment for chronic pain: a systematic review. Agency for Healthcare Research and Quality; June 2018. Accessed September 15, 2018. https://effectivehealthcare.ahrq.gov/topics/nonpharma-treatment-pain/research-2018
Practice Pointers
Neck pain is a common symptom, with a worldwide mean prevalence of 23%.2 Globally, neck pain ranks fourth in terms of overall disability and leads to reduced work productivity, increased work absenteeism, and increased insurance costs.3
This Agency for Healthcare Research and Quality (AHRQ) review examined 218 publications on noninvasive nonpharmacologic treatments for several chronic pain conditions. A subset of 25 randomized controlled trials specifically evaluated the effects of treatments for chronic neck pain, defined as pain lasting more than three months, on pain or function. Most of the trials took place outside of the United States, primarily in Asia and Europe. Outcomes were classified as short term (one to less than six months following treatment completion), intermediate term (six to less than 12 months), or long term (12 months or longer).
Studied interventions included exercise (single or combined types), massage, acupuncture, relaxation techniques, mind-body practices, and physical modalities. The mind-body practice was the Alexander technique, which involves changing posture, breathing, and balance and coordination to release tension within the body. The physical modality was low-level laser therapy, which consists of using lasers at wavelengths ranging from red to infrared to induce tissue healing.
The improvements in function were small to moderate across all interventions. Function was measured using the Northwick Park Questionnaire, the Neck Disability Index, and the Neck Pain and Disability Scale, which assess pain-related limitations in daily activities. Functional improvement meant that patients were able to perform activities of daily living and other daily activities more easily.
Although no single type of exercise improved pain or function, two trials found that combination exercise produced small improvements in short- and long-term function and short-term pain.4,5 Low-level laser therapy produced moderate improvement in short-term pain and function.
CLINICAL BOTTOM LINE
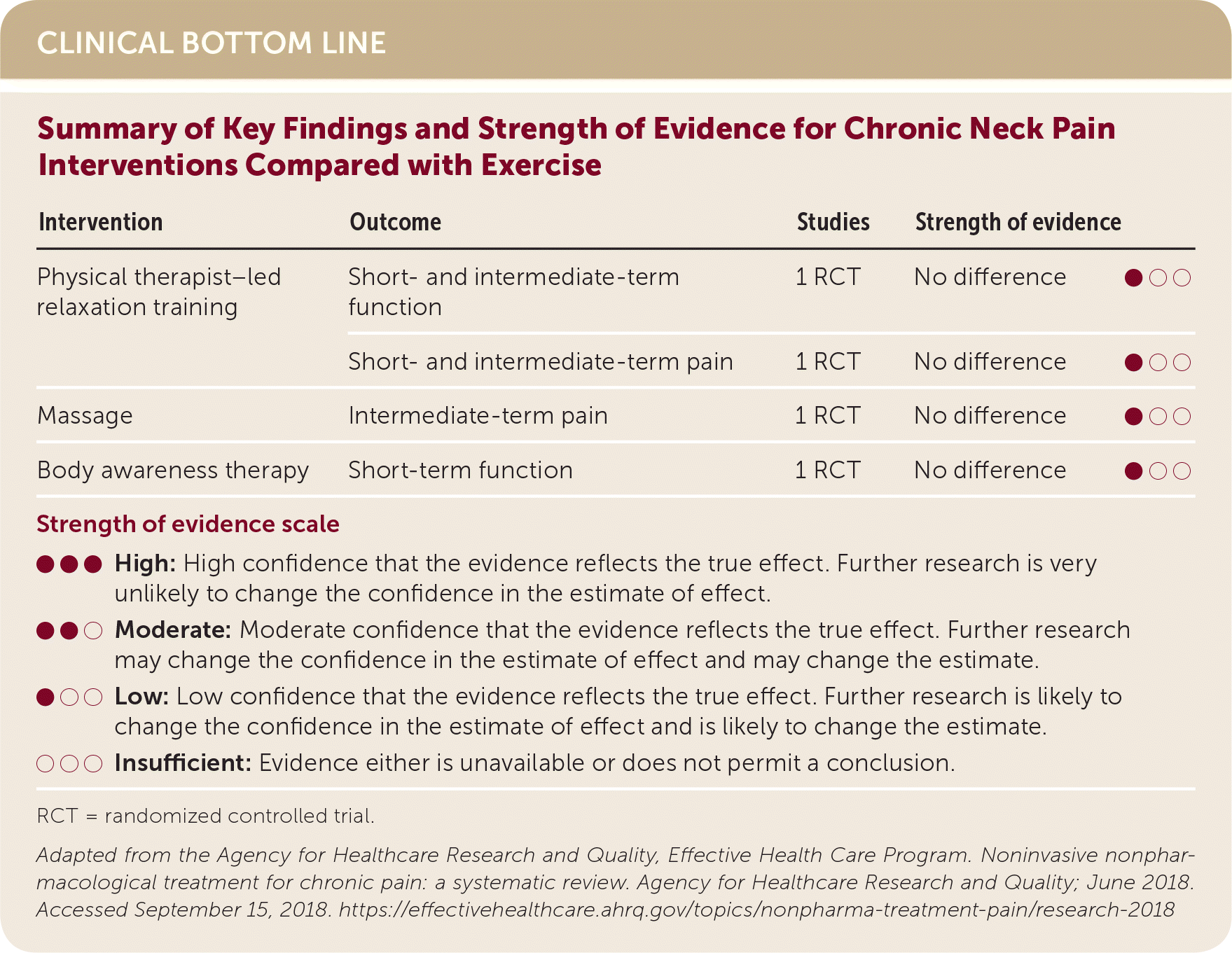
| Summary of Key Findings and Strength of Evidence for Chronic Neck Pain Interventions Compared with Exercise | ||||
| Intervention | Outcome | Studies | Strength of evidence | |
|---|---|---|---|---|
| Physical therapist–led relaxation training | Short- and intermediate-term function | 1 RCT | No difference | ● ○ ○ |
| Short- and intermediate-term pain | 1 RCT | No difference | ● ○ ○ | |
| Massage | Intermediate-term pain | 1 RCT | No difference | ● ○ ○ |
| Body awareness therapy | Short-term function | 1 RCT | No difference | ● ○ ○ |
Strength of evidence scale
● ● ● High: High confidence that the evidence reflects the true effect. Further research is very unlikely to change the confidence in the estimate of effect.
● ● ○ Moderate: Moderate confidence that the evidence reflects the true effect. Further research may change the confidence in the estimate of effect and may change the estimate.
● ○ ○ Low: Low confidence that the evidence reflects the true effect. Further research is likely to change the confidence in the estimate of effect and is likely to change the estimate.
○ ○ ○ Insufficient: Evidence either is unavailable or does not permit a conclusion.
RCT = randomized controlled trial.
Adapted from the Agency for Healthcare Research and Quality, Effective Health Care Program. Noninvasive nonpharmacological treatment for chronic pain: a systematic review. Agency for Healthcare Research and Quality; June 2018. Accessed September 15, 2018. https://effectivehealthcare.ahrq.gov/topics/nonpharma-treatment-pain/research-2018
Few trials compared nonpharmacologic with pharmacologic treatments. Two trials of acupuncture found no statistically significant differences in pain when compared with nonsteroidal anti-inflammatory drugs (NSAIDs).6,7 One trial of exercise showed no statistically significant difference in pain or function when compared with ibuprofen and thiocolchicoside.5
Despite low-quality evidence, a reasonable approach is discussing nonpharmacologic options with patients who have chronic neck pain and engaging in shared decision-making, because there are minimal harms to these therapies and documented risks associated with NSAIDs.8 Based on this AHRQ review, family physicians should consider incorporating low-level laser therapy, acupuncture, combination exercise, and/or the Alexander technique into treatment plans for patients with chronic neck pain.
Editor's Note: American Family Physician SOR ratings are different from the AHRQ Strength of Evidence ratings.

