Clinical Question
Is it possible to determine which patients with acute abdominal pain are likely to have diverticulitis and therefore do not require imaging?
Evidence Summary
Each year in the United States, acute abdominal pain costs $10.2 billion and accounts for more than 12 million (9%) ambulatory emergency department visits.1,2 In 2014, diverticulitis accounted for 372,000 emergency department visits, led to 160,000 hospital admissions, and was associated with 674 in-hospital deaths.2 Computed tomography is sensitive (94%) and specific (99%) for diverticulitis.3 Because up to 85% of patients with diverticulitis are treated nonoperatively,4 use of a clinical prediction rule to determine the likelihood of acute diverticulitis would help reduce the number of emergency department visits for acute abdominal pain leading to computed tomography, reducing cost and radiation exposure.1
A Dutch research group created a clinical prediction rule for acute diverticulitis that includes three indicators: absence of vomiting, a C-reactive protein level greater than 5 mg per dL (50 mg per L), and tenderness limited to the left lower quadrant (Table 1).5 Presence of all three indicators had a sensitivity of 36% (95% CI, 26% to 47%), specificity of 98% (95% CI, 89% to 100%), positive predictive value of 97% (95% CI, 83% to 99%), and negative predictive value of 47% (95% CI, 37% to 57%) in those suspected of having diverticulitis (63% of the derivation cohort).5
TABLE 1. Three-Item Clinical Prediction Rule for Acute Diverticulitis
An external validation study of the three-item rule showed a specificity of 93% (95% CI, 88% to 96%) and positive predictive value of 81% (95% CI, 69% to 89%) among a cohort in which acute diverticulitis was suspected based on information recorded on imaging orders. The positive likelihood ratio for this group was 5.29 (95% CI, 2.89 to 9.68), and the negative likelihood ratio was 0.68 (95% CI, 0.59 to 0.78). It is important to note that diverticulitis was suspected, and its prevalence was high in the validation cohort.6 In a less select cohort in which the prevalence of diverticulitis is lower, the rule would not be as effective at discriminating who has diverticulitis and who does not.
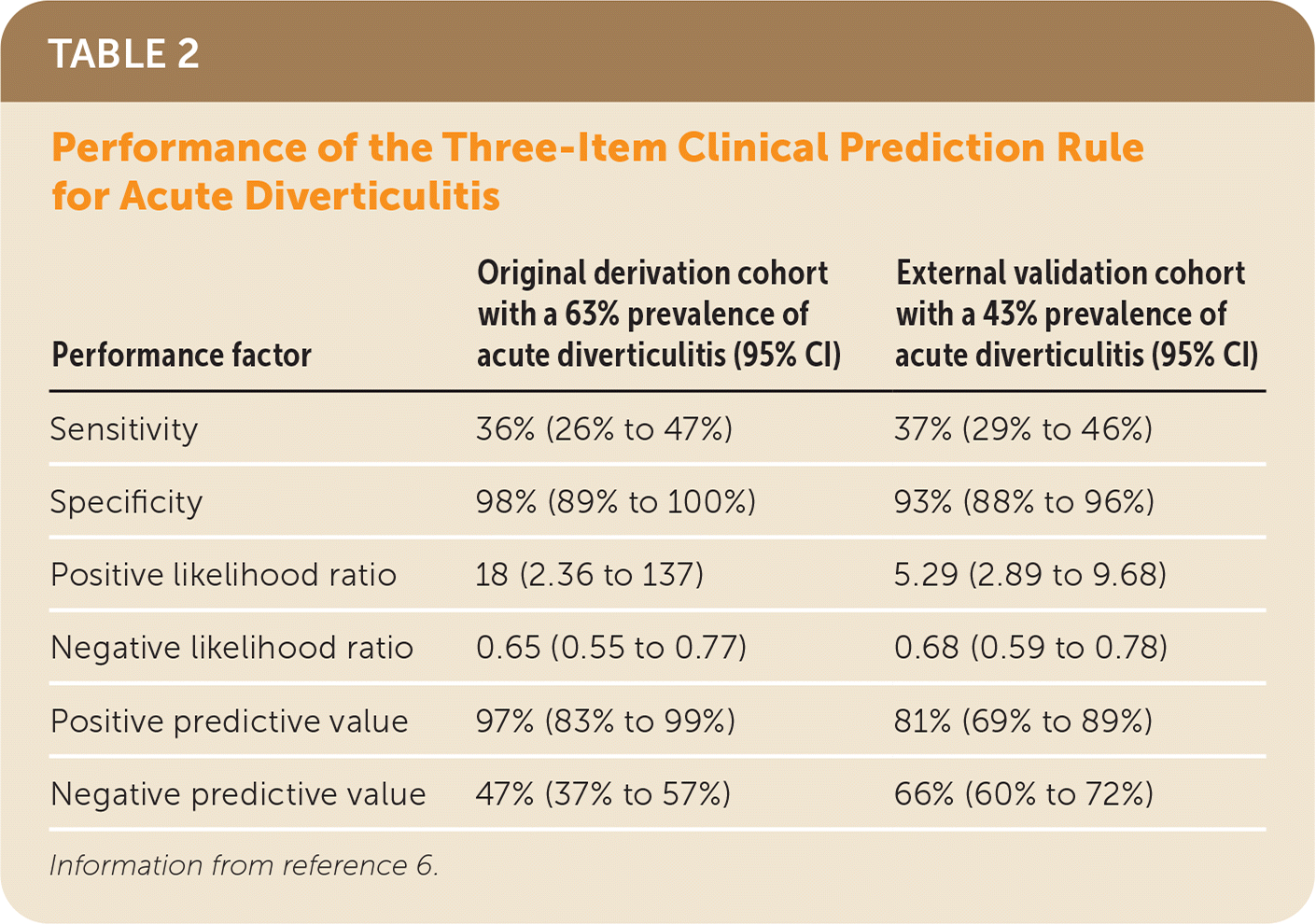
Table 2 summarizes the performance of the three-item clinical prediction rule in the derivation and validation cohorts.6
TABLE 2. Performance of the Three-Item Clinical Prediction Rule for Acute Diverticulitis
| Performance factor | Original derivation cohort with a 63% prevalence of acute diverticulitis (95% CI) | External validation cohort with a 43% prevalence of acute diverticulitis (95% CI) |
|---|---|---|
| Sensitivity | 36% (26% to 47%) | 37% (29% to 46%) |
| Specificity | 98% (89% to 100%) | 93% (88% to 96%) |
| Positive likelihood ratio | 18 (2.36 to 137) | 5.29 (2.89 to 9.68) |
| Negative likelihood ratio | 0.65 (0.55 to 0.77) | 0.68 (0.59 to 0.78) |
| Positive predictive value | 97% (83% to 99%) | 81% (69% to 89%) |
| Negative predictive value | 47% (37% to 57%) | 66% (60% to 72%) |
Information from reference 6.
Acute diverticulitis is one of the many pathologies that may cause acute abdominal pain. Dutch guidelines recommend additional imaging for cases deemed urgent—first ultrasonography, then computed tomography if the ultrasound result is inconclusive or is negative but clinical suspicion remains.7 Japanese guidelines state that computed tomography may be indicated in all patients with acute abdominal pain but caution about radiation exposure.8 The American College of Radiology Appropriateness Criteria state that for those with left lower quadrant pain and suspected diverticulitis, computed tomography of the abdomen and pelvis with intravenous contrast media is usually appropriate and that ultrasonography may be appropriate.9
Use of a clinical prediction rule with a high positive predictive value for acute diverticulitis may increase diagnostic certainty and help obviate the need for imaging, avoiding radiation exposure in patients who are candidates for nonsurgical management.
Applying the Evidence
A 59-year-old patient presents with left lower quadrant pain. The patient has a history of diverticulosis as shown on a screening colonoscopy and has had one previous episode of diverticulitis; medical history is otherwise unremarkable. The patient has no nausea or vomiting, but pain worsens with walking. On examination, tenderness is present only in the left lower quadrant and no rebound or guarding is noted. A point-of-care C-reactive protein measurement is 6.2 mg per dL (62 mg per L).
The patient meets all criteria on the three-item clinical prediction rule. With a positive predictive value of 81% to 97% for acute diverticulitis, the patient likely has the disease. A follow-up appointment is scheduled for the next day with instructions to return if the abdominal pain worsens or if additional symptoms develop.
Editor's Note: Dr. Saguil is a contributing editor for AFP.
The opinions and assertions contained herein are the private views of the author and are not to be construed as official or as reflecting the views of the Uniformed Services University of the Health Sciences or the Department of the Army.


