Attention-deficit/hyperactivity disorder (ADHD) is a multidimensional chronic neurodevelopmental condition that affects 8.4% of U.S. children between two and 17 years of age and may pose long-term morbidity if untreated. The evaluation for ADHD begins when parents or caregivers present to primary care physicians with concerns about behavior problems or poor school or social function. A comprehensive history and physical examination should assess for comorbid or other conditions that can mimic ADHD. The combination of Diagnostic and Statistical Manual of Mental Disorders, 5th ed., criteria and validated screening tools completed by parents, teachers, or other adults can aid in establishing the diagnosis. The goals of treatment include symptom reduction and improved social and cognitive function. Psychosocial interventions are the recommended first-line treatment for preschool children (four to five years) and can improve overall function when used as an adjunct therapy in elementary school children (six to 11 years of age) and adolescents (12 to 17 years of age). Stimulant medications are well-established as an effective treatment for reducing symptoms of ADHD in elementary school children and adolescents. Nonstimulant medications are less effective but reasonable as adjunct or alternative therapy when stimulants are ineffective or not tolerated. Regular follow-up is key in the management of ADHD and should assess symptoms, overall function, presence of comorbidities, adverse effects of treatment, and medication use.
Attention-deficit/hyperactivity disorder (ADHD) is the most common neurodevelopmental condition in U.S. children, and it affects 8.4% of children between two and 17 years of age (greater than 5 million).1 Of the children who are affected, 62% are treated with medication, less than one-half have received behavioral treatment, and nearly one-fourth have not received treatment.1 Children with ADHD are at risk of long-term morbidities, including poor academic performance, low self-esteem, difficult relationships, substance use, injury, and other maladaptive behaviors.2 This article presents evidence-based answers to common questions about the evaluation and management of childhood ADHD.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
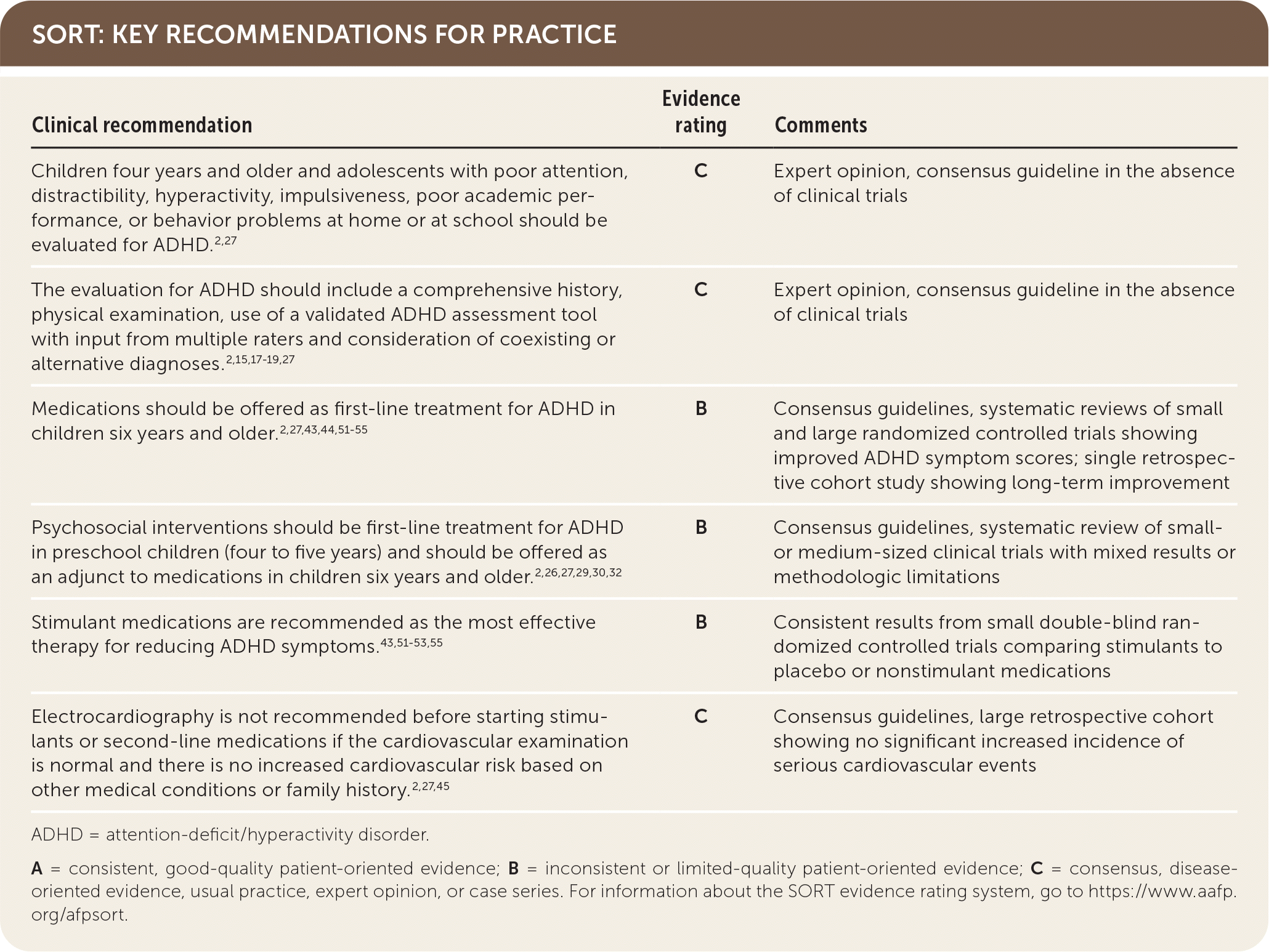
ADHD = attention-deficit/hyperactivity disorder.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
What Are the Risk Factors for ADHD?
The etiology of ADHD involves a complex interaction of genetic, social, and environmental factors, including prenatal and childhood exposures.3
EVIDENCE SUMMARY
Research among families, twins, and children who are adopted support substantial heritability (74%) for ADHD.4 The search to identify specific genes responsible for ADHD implicates a complex polygenic mechanism.3,4 Males are diagnosed with ADHD at nearly two times the rate of females1,5; however, differences in presentation between sexes may result in missed or delayed diagnosis in females.5,6 Males present with more recognizable externalizing symptoms and behaviors (e.g., impulsivity, defiant conduct), whereas females present with inattention and possibly impaired cognitive function.5–7
Children born preterm (before 37 weeks' gestation) are diagnosed with ADHD two times as often as children born at term (odds ratio [OR] = 1.6; 95% CI, 1.3 to 1.8; 74 studies; N = 64,061]),8 and risk of ADHD diagnosis or symptoms may increase with the severity of prematurity or low birth weight.9 The risk of ADHD is greater for children whose mothers smoked during pregnancy (OR = 1.60; 95% CI, 1.45 to 1.76; N = 50,044)10 and had hypertensive disorders in pregnancy (OR = 1.29; 95% CI, 1.22 to 1.36; six studies; N = 1,395,605).11 Despite ongoing public concern and scientific inquiry, the evidence is inconsistent in supporting direct links between ADHD and exposure to digital or “screen” media12 or chemical toxins,3 including lead.13
When and How Should Physicians Evaluate a Child for ADHD?
Primary care physicians should initiate evaluation for ADHD when parents or caregivers present with concerns about a child's academic or behavior problems, including symptoms of inattention, hyperactivity, or impulsivity in children between four and 17 years of age.2
EVIDENCE SUMMARY
ADHD is diagnosed using criteria from the Diagnostic and Statistical Manual of Mental Disorders, 5th ed., (Table 114 ) after a comprehensive history and physical examination, with attention to family, birth, and early childhood development2,14–16 (Table 22,15–17 ). The assessment of symptoms should explore the duration and context in which they occur and the effects on function or development.2,15 The dysfunction classified in ADHD must occur in more than one setting; therefore, clinicians should seek evaluations from other adults with whom the child interacts outside of the home (e.g., educators, school counselors, coaches).2,18 Routine laboratory tests, genetic testing, and neuroimaging are not recommended unless specific concerns result from the history or examination.15,19
TABLE 1. DSM-5 Diagnostic Criteria for Attention-Deficit/Hyperactivity Disorder

| A. A persistent pattern of inattention and/or hyperactivity–impulsivity that interferes with functioning or development, as characterized by 1 and/or 2: 1. Inattention: Six (or more) of the following symptoms have persisted for at least six months to a degree that is inconsistent with developmental level and that negatively impacts directly on social and academic/occupational activities: Note: The symptoms are not solely a manifestation of oppositional behavior, defiance, hostility, or failure to understand tasks or instructions. For older adolescents and adults (age 17 and older), at least five symptoms are required.
2. Hyperactivity and impulsivity: Six (or more) of the following symptoms have persisted for at least six months to a degree that is inconsistent with developmental level and that negatively impacts directly on social and academic/occupational activities: Note: The symptoms are not solely a manifestation of oppositional behavior, defiance, hostility, or failure to understand tasks or instructions. For older adolescents and adults (age 17 and older), at least five symptoms are required.
B. Several inattentive or hyperactive-impulsive symptoms were present prior to age 12 years. C. Several inattentive or hyperactive-impulsive symptoms are present in two or more settings (e.g., at home, school, or work; with friends or relatives; in other activities). D. There is clear evidence that the symptoms interfere with, or reduce the quality of, social, academic, or occupational functioning. E. The symptoms do not occur exclusively during the course of schizophrenia or another psychotic disorder and are not better explained by another mental disorder (e.g., mood disorder, anxiety disorder, dissociative disorder, personality disorder; substance intoxication or withdrawal). Specify whether: 314.01 (F90.2) Combined presentation: If both Criterion A1 (inattention) and Criterion A2 (hyperactivity-impulsivity) are met for the past six months. 314.00 (F90.0) Predominantly inattentive presentation: If Criterion A1 (inattention) is met, but Criterion A2 (hyperactivity-impulsivity) is not met for the past six months. 314.01 (F90.1) Predominantly hyperactive-impulsive presentation: If Criterion A2 (hyperactivity-impulsivity) is met and Criterion A1 (inattention) is not met for the past six months. |
Reprinted with permission from the Diagnostic and Statistical Manual of Mental Disorders. 5th ed. American Psychiatric Association; 2013:59–60.
TABLE 2. Initial Evaluation of ADHD in Children

| Key categories | Additional considerations or descriptions |
|---|---|
| History | |
| Pregnancy and birth history | Screen for prenatal risk factors for ADHD: |
| Maternal substance use (tobacco, drugs, alcohol)? | |
| Other complications during pregnancy, at birth, or the early neonatal period (e.g., maternal hypertensive disorders, prematurity, low birth weight)? | |
| Early childhood development | History of delayed milestones or language/speech development? |
| Concerns about sleep and dietary habits? | |
| How do parents/caregivers describe the child's temperament? | |
| Medical history (includes, neurologic and vision or hearing concerns) | History of tics, seizure disorder, central nervous system infections, head trauma? |
| Has the child received an abnormal vision or hearing screening result, or have the parents been concerned about vision or hearing? | |
| Family medical history (e.g., cardiac, neurodevelopmental) | Family history of sudden cardiac death |
| Has anyone in the family been diagnosed with ADHD or had significant academic struggles, truancy, or other behavior troubles without a known diagnosis of ADHD? | |
| Physical examination | |
| Vital signs and growth parameters | Measure height, weight, head circumference, and vital signs |
| Review current and past growth charts, if available | |
| Neurologic examination | |
| Vision and hearing | Assess vision with an age-appropriate wall chart; refer for formal testing if abnormal, or if parent has concerns |
| Refer for formal audiogram if there is clinician or parent concern about child's hearing | |
| Fine motor skills and coordination (finger to nose, rapid alternating movements, trace a maze, use scissors to cut paper) | Observe for verbal or motor tics and for mixed laterality (i.e., ambidexterity) |
| Some children with ADHD have more difficulty with fine motor tasks and coordination, which can be observed during the physical examination | |
| Behavior assessment (includes communication and activity level) | Does the child fidget or have difficulty sitting still? Is the speech loud, interruptive? |
| Observing the child's behavior in the office can be helpful but is not diagnostic; physicians should interpret this with caution in the clinical environment |
ADHD = attention-deficit/hyperactivity disorder.
Approximately 60% of children with ADHD meet criteria for at least one other mood, behavior, or neurodevelopmental disorder1 (Table 32,17,19–21 ). The initial evaluation should screen for alternative diagnoses (e.g., anxiety, oppositional defiant disorder) that might otherwise explain the presentation.2,15 Because these conditions may coexist with ADHD or emerge over time, screening annually during follow-up at a minimum is important.20
TABLE 3. Conditions that May Mimic or Coexist with Attention-Deficit/Hyperactivity Disorder

| Comorbid or confounding diagnoses |
| Anxiety disorders (e.g., generalized, obsessive-compulsive, separation) |
| Autism spectrum disorders |
| Developmental or speech delays |
| Fetal alcohol syndrome |
| Genetic (e.g., fragile X, neurofibromatosis, 22q11 deletion syndromes) |
| Hearing loss |
| Mood disorders (e.g., dysthymia, major depression, bipolar disorder) |
| Neurologic disorders (e.g., seizures, traumatic brain injury, Tourette syndrome, or other tic disorders) |
| Oppositional defiant disorder/conduct disorder |
| Sleep disorders (e.g., insomnia, obstructive sleep apnea, restless legs syndrome, periodic limb movement disorder) |
| Specific learning disability (reading, math, writing) |
| Situational factors |
| Academic (poor performance, failure) |
| Behavior (e.g., school suspensions, expulsion) |
| Home/family (increased likelihood to be a survivor of child abuse) |
| Motivation (loss of motivation; learned helplessness) |
| Physical problems (motor coordination difficulty; unintentional injuries) |
| Psychosocial difficulty (e.g., bullying, peer rejection, adult disapproval, poor self-esteem, difficulty learning rules and understanding social cues) |
| Substance use |
What Are the Best Diagnostic Tools for ADHD?
Several psychometric tools can assist in making a diagnosis of ADHD (Table 417,21–23 ); they vary in scope, accessibility, and diagnostic accuracy. Physicians must consider age-specific challenges related to the diagnosis of ADHD in preschool children (four to five years of age) and adolescents (12 to 17 years of age).
TABLE 4. Diagnostic Tools and CPT Coding for ADHD
ADHD = attention-deficit/hyperactivity disorder.
*—Available for free.
†—Validated for preschool children.
EVIDENCE SUMMARY
Some tools evaluate for ADHD and comorbid conditions, and others are specific to ADHD. Tools with a broad scope may be preferable to follow patients over time as children are reevaluated for the emergence of comorbidities.20 A 2016 meta-analysis (five studies; N = 972) found that the Conners Abbreviated Symptom Questionnaire (CASQ) had a high sensitivity (83%) and specificity (84%) and best overall positive (5.3) and negative (0.2) likelihood ratios for diagnosing ADHD.22,24 Some scales, such as the CASQ, have a cost associated with use; therefore, it may be practical to consider freely accessible tools with similar sensitivities, including the Child and Adolescent Behavior Inventory (sensitivity = 82.8%; CI, 75.6% to 88.5%, and specificity = 91.5%; CI, 87.9% to 94.3%)23 or the NICHQ Vanderbilt Assessment Scale (parent rating scale: sensitivity = 80%; CI, 71% to 87%, and specificity = 75%; CI, 66 to 83; and teacher rating scale: sensitivity = 69%; CI, 43% to 87%, and specificity = 85%; CI, 78% to 89%).22
Preschool children may display certain ADHD-like behaviors (e.g., inattention, impulsivity) as part of normal development, and they tend to be in fewer environments outside the home; therefore, it is challenging to apply standard diagnostic criteria for ADHD to this age group.21 Several tools are validated for preschool children (Table 417,21–23 ). Children who are diagnosed with ADHD should be reevaluated as they age to confirm the persistence of the diagnosis, emergence of comorbidities, and the need for treatment.18,21
Adolescents experience more variation in teacher exposure and less parental observation compared with young children; these and other factors such as substance use, social pressures, or comorbid mood disorders may blur diagnostic accuracy.20 Before attributing an adolescent's behavior or academic difficulties to ADHD, the clinician should confirm that symptoms of ADHD were present before 12 years of age.2,20
Which Psychosocial Interventions Are Effective for ADHD?
Psychosocial interventions are effective monotherapy for preschool children with ADHD,2 and they may improve academic function and organizational skills in older children and adolescents with ADHD.25,26 Physicians should recommend psychosocial interventions as a critical part of the management of ADHD and assist patients in accessing them.2,27
EVIDENCE SUMMARY
Psychosocial interventions are used less often in the treatment of ADHD compared with medications.1,28 This is likely attributed to many factors: variations in available techniques, inconsistent results for effectiveness, lack of clear guidance for implementation, barriers to access, and time-intensive nature.2,28–30 The best available evidence and guidelines support two types of psychosocial interventions for ADHD: parent training in behavior management and classroom interventions.2,31
Parent training in behavior management is typically provided by specialists who help parents learn strategies to reinforce desired behaviors and discourage unwanted or problematic behaviors.31 eTable A lists resources to assist parents and clinicians with accessing parent training in behavior management programs. Classroom interventions incorporate proactive behavior strategies (e.g., frequent reminders of classroom rules, daily report cards) and environmental adaptations, and may also include individualized education programs.2,25 Physicians and parents should seek guidance from school authorities to determine if a child with ADHD qualifies for additional services under section 504 of the Rehabilitation Act or the Individuals with Disability Education Act.2
eTABLE A ADHD Resources
ADHD = attention-deficit/hyperactivity disorder.
Adapted with permission from Felt BT, Biermann B, Christner JG, et al. Diagnosis and management of ADHD in children. Am Fam Physician. 2014;90(7):460.
Current guidelines recommend parent training in behavior management and classroom behavior interventions as first-line therapy for preschool children who exhibit ADHD-like behaviors or have been diagnosed with ADHD.2,27 In elementary school children, parent training in behavior management and classroom interventions should be initiated at the time of diagnosis even when medications are used.2 A single randomized treatment sequencing trial in children with ADHD (five to 12 years of age; N = 146) showed that initial management with parent training in behavior management and brief classroom intervention was comparable with children who began treatment with medication only, and was sufficient as monotherapy for some.32
Although there are fewer studies of psychosocial interventions in adolescents compared with younger children, physicians should consider offering interventions to foster the growth of skills needed in adulthood.2,26 One systematic review of adolescents with ADHD (17 trials; N = 2,668) who received behavior or motivational training demonstrated minimal or inconsistent effects on ADHD symptoms but modest improvements in academic and organizational skills.26
OTHER BEHAVIOR INTERVENTIONS
Adequate sleep and regular physical activity are recommended for all children and are shown to benefit children with ADHD.33,34 One randomized controlled trial (RCT; N = 244) of children in Australia treated with stimulants for ADHD showed that a series of two sleep counseling sessions (delivered two weeks apart) resulted in improved symptoms of ADHD, behavior, health-related quality of life, and parental work function at three and six months postintervention.33 The counseling sessions included education and formulation of a tailored sleep management plan; notably, the sessions were administered by clinicians with no prior expertise in sleep management but who had recently completed a six-hour sleep training program. Physical activity may be important for managing comorbid problems in ADHD. A meta-analysis (14 studies; N = 574) in children with ADHD compared physical activity to a control group and showed significant reductions in anxiety and depression, aggressive behaviors, and social problems; however, actual ADHD symptom improvement was not significant.34
Which Dietary or Complementary/Alternative Interventions Are Effective?
There is no clear benefit for dietary interventions or complementary and alternative therapies in the treatment of ADHD, and current guidelines do not support their use.2,27
EVIDENCE SUMMARY
Numerous studies have assessed for, but did not demonstrate, a role for dietary interventions including a focus on supplementation with essential fatty acids and elimination diets for the management of ADHD.29,31,35 A meta-analysis (13 trials; N = 1,011) of children with ADHD receiving omega-3 and/or omega-6 polyunsaturated fatty acid supplementation showed no statistically significant difference in parent- or teacher-rated symptoms when all groups were compared with placebo.36 A meta-analysis (24 trials; N = 794) evaluating the effects of restriction diets or synthetic food colors showed weak or inconsistent evidence of improved parental symptom scores in children with ADHD.37 Studies of B and D vitamins, St. John's wort, and ginkgo show inconsistent results and do not support their use.31,35
Studies of complementary or integrative medicine techniques for the treatment of ADHD in children are limited in size or quality and do not show substantial evidence for benefit, including studies for acupuncture,38 yoga,31 mindfulness,31 chiropractic or manual therapy,39 and external trigeminal nerve stimulation.2 Although the risk of harm with these treatments may be low, these interventions are not currently recommended.2,27
How Should Physicians Approach Drug Selection and Dosing?
PRESCHOOL CHILDREN (FOUR TO FIVE YEARS OF AGE)
If moderate to severe symptoms and behavior dysfunction persist despite an adequate course of parent training in behavior management and classroom interventions, methylphenidate (Ritalin) can be considered in preschool children with ADHD.2,27
EVIDENCE SUMMARY
In the Preschool ADHD Treatment Study, children taking immediate-release methylphenidate in dosages of 2.5 mg, 5 mg, and 7.5 mg three times per day had decreases in ADHD symptoms, although the treatment effect sizes (0.48, 0.52, 0.87, respectively) were smaller in preschool children, and more emotional lability was reported.40 An effect size of 0.2 is considered small, 0.5 medium, and 0.8 large.41 In a follow-up study of children in the Preschool ADHD Treatment Study, 65% and 70.9% stayed on ADHD medications at three and six years of follow-up, respectively; however, one out of four children had discontinued medications.42 This suggests that early and severe ADHD symptoms may be more likely to persist. If psychosocial interventions are not available, the risk of starting stimulants before six years of age must be weighed against potential harms of delaying treatment.2,17,27
CHILDREN SIX TO 17 YEARS OF AGE
Medication can be offered as first-line treatment for elementary school children and adolescents with ADHD, with evidence-based psychosocial interventions encouraged as an adjunct therapy.2,27 Stimulants (e.g., methylphenidate, dextroamphetamine, and mixed amphetamine salts) are the most effective(Table 52,17,40,43–49 ); other medications include selective norepinephrine reuptake inhibitors (atomoxetine [Strattera]) and alpha-2 receptor agonists2,17,50 (guanfacine and clonidine; Table 62,17,40,43–49).
TABLE 5. U.S. Food and Drug Administration–Approved Stimulant Medications for Attention-Deficit/Hyperactivity Disorder
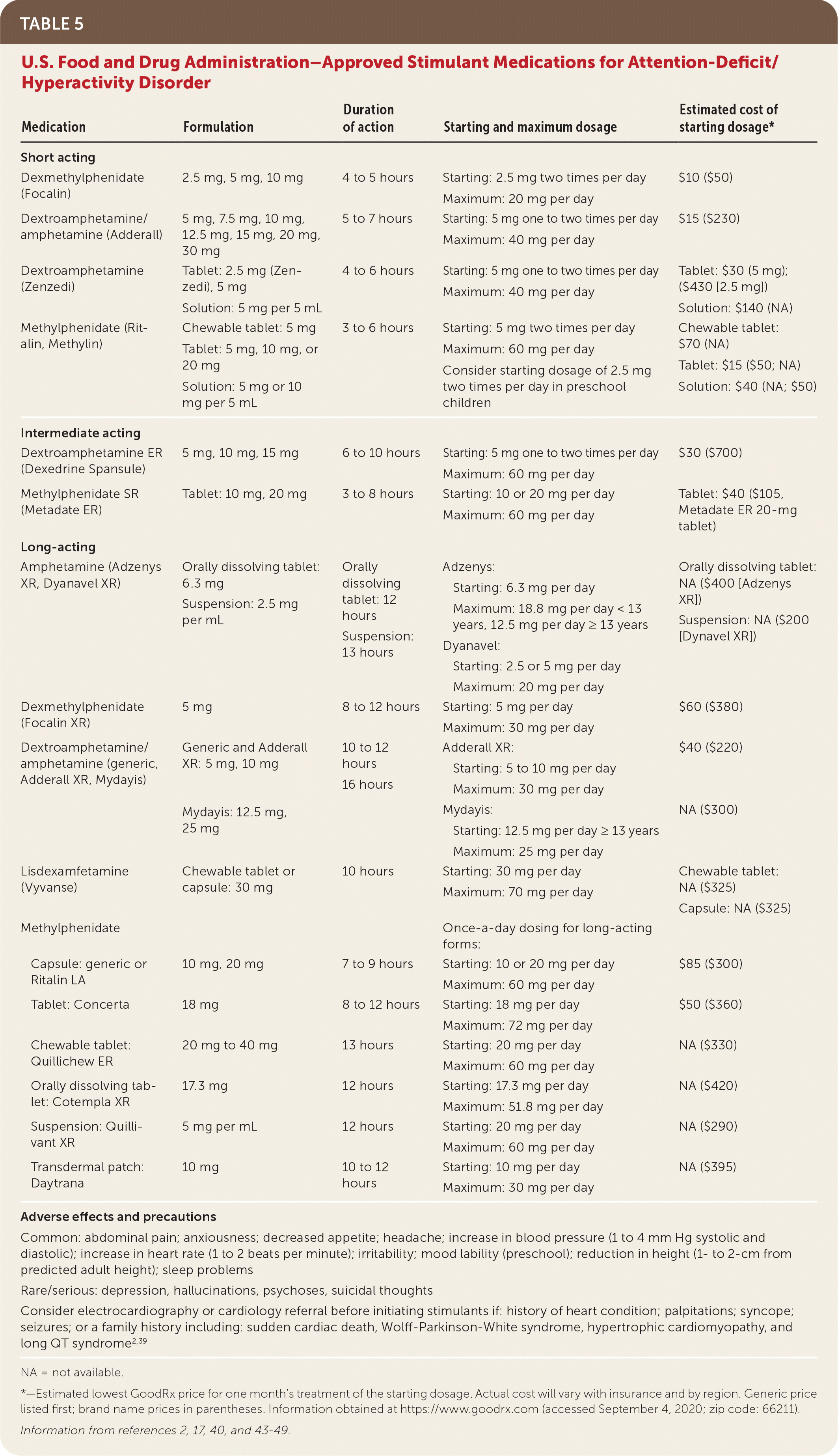
| Medication | Formulation | Duration of action | Starting and maximum dosage | Estimated cost of starting dosage* |
|---|---|---|---|---|
| Short acting | ||||
| Dexmethylphenidate (Focalin) | 2.5 mg, 5 mg, 10 mg | 4 to 5 hours | Starting: 2.5 mg two times per day Maximum: 20 mg per day | $10 ($50) |
| Dextroamphetamine/amphetamine (Adderall) | 5 mg, 7.5 mg, 10 mg, 12.5 mg, 15 mg, 20 mg, 30 mg | 5 to 7 hours | Starting: 5 mg one to two times per day Maximum: 40 mg per day | $15 ($230) |
| Dextroamphetamine (Zenzedi) | Tablet: 2.5 mg (Zenzedi), 5 mg Solution: 5 mg per 5 mL | 4 to 6 hours | Starting: 5 mg one to two times per day Maximum: 40 mg per day | Tablet: $30 (5 mg); ($430 [2.5 mg]) Solution: $140 (NA) |
| Methylphenidate (Ritalin, Methylin) | Chewable tablet: 5 mg | 3 to 6 hours | Starting: 5 mg two times per day | Chewable tablet: $70 (NA) |
| Tablet: 5 mg, 10 mg, or 20 mg Solution: 5 mg or 10 mg per 5 mL | Maximum: 60 mg per day Consider starting dosage of 2.5 mg two times per day in preschool children | Tablet: $15 ($50; NA) Solution: $40 (NA; $50) | ||
| Intermediate acting | ||||
| Dextroamphetamine ER (Dexedrine Spansule) | 5 mg, 10 mg, 15 mg | 6 to 10 hours | Starting: 5 mg one to two times per day Maximum: 60 mg per day | $30 ($700) |
| Methylphenidate SR (Metadate ER) | Tablet: 10 mg, 20 mg | 3 to 8 hours | Starting: 10 or 20 mg per day Maximum: 60 mg per day | Tablet: $40 ($105, Metadate ER 20-mg tablet) |
| Long-acting | ||||
| Amphetamine (Adzenys XR, Dyanavel XR) | Orally dissolving tablet: 6.3 mg Suspension: 2.5 mg per mL | Orally dissolving tablet: 12 hours Suspension: 13 hours | Adzenys: Starting: 6.3 mg per day Maximum: 18.8 mg per day < 13 years, 12.5 mg per day ≥ 13 years | Orally dissolving tablet: NA ($400 [Adzenys XR]) |
| Dyanavel: Starting: 2.5 or 5 mg per day Maximum: 20 mg per day | Suspension: NA ($200 [Dynavel XR]) | |||
| Dexmethylphenidate (Focalin XR) | 5 mg | 8 to 12 hours | Starting: 5 mg per day Maximum: 30 mg per day | $60 ($380) |
| Dextroamphetamine/amphetamine (generic, Adderall XR, Mydayis) | Generic and Adderall XR: 5 mg, 10 mg Mydayis: 12.5 mg, 25 mg | 10 to 12 hours 16 hours | Adderall XR: Starting: 5 to 10 mg per day Maximum: 30 mg per day | $40 ($220) |
| Mydayis: Starting: 12.5 mg per day ≥ 13 years Maximum: 25 mg per day | NA ($300) | |||
| Lisdexamfetamine (Vyvanse) | Chewable tablet or capsule: 30 mg | 10 hours | Starting: 30 mg per day Maximum: 70 mg per day | Chewable tablet: NA ($325) Capsule: NA ($325) |
| Methylphenidate | Once-a-day dosing for long-acting forms: | |||
| Capsule: generic or Ritalin LA | 10 mg, 20 mg | 7 to 9 hours | Starting: 10 or 20 mg per day Maximum: 60 mg per day | $85 ($300) |
| Tablet: Concerta | 18 mg | 8 to 12 hours | Starting: 18 mg per day Maximum: 72 mg per day | $50 ($360) |
| Chewable tablet: Quillichew ER | 20 mg to 40 mg | 13 hours | Starting: 20 mg per day Maximum: 60 mg per day | NA ($330) |
| Orally dissolving tablet: Cotempla XR | 17.3 mg | 12 hours | Starting: 17.3 mg per day Maximum: 51.8 mg per day | NA ($420) |
| Suspension: Quillivant XR | 5 mg per mL | 12 hours | Starting: 20 mg per day Maximum: 60 mg per day | NA ($290) |
| Transdermal patch: Daytrana | 10 mg | 10 to 12 hours | Starting: 10 mg per day Maximum: 30 mg per day | NA ($395) |
| Adverse effects and precautions | ||||
| Common: abdominal pain; anxiousness; decreased appetite; headache; increase in blood pressure (1 to 4 mm Hg systolic and diastolic); increase in heart rate (1 to 2 beats per minute); irritability; mood lability (preschool); reduction in height (1- to 2-cm from predicted adult height); sleep problems | ||||
| Rare/serious: depression, hallucinations, psychoses, suicidal thoughts | ||||
| Consider electrocardiography or cardiology referral before initiating stimulants if: history of heart condition; palpitations; syncope; seizures; or a family history including: sudden cardiac death, Wolff-Parkinson-White syndrome, hypertrophic cardiomyopathy, and long QT syndrome 2,39 | ||||
NA = not available.
*—Estimated lowest GoodRx price for one month's treatment of the starting dosage. Actual cost will vary with insurance and by region. Generic price listed first; brand name prices in parentheses. Information obtained at https://www.goodrx.com (accessed September 4, 2020; zip code: 66211).
TABLE 6. U.S. Food and Drug Administration–Approved Nonstimulant Medications for Attention-Deficit/Hyperactivity Disorder
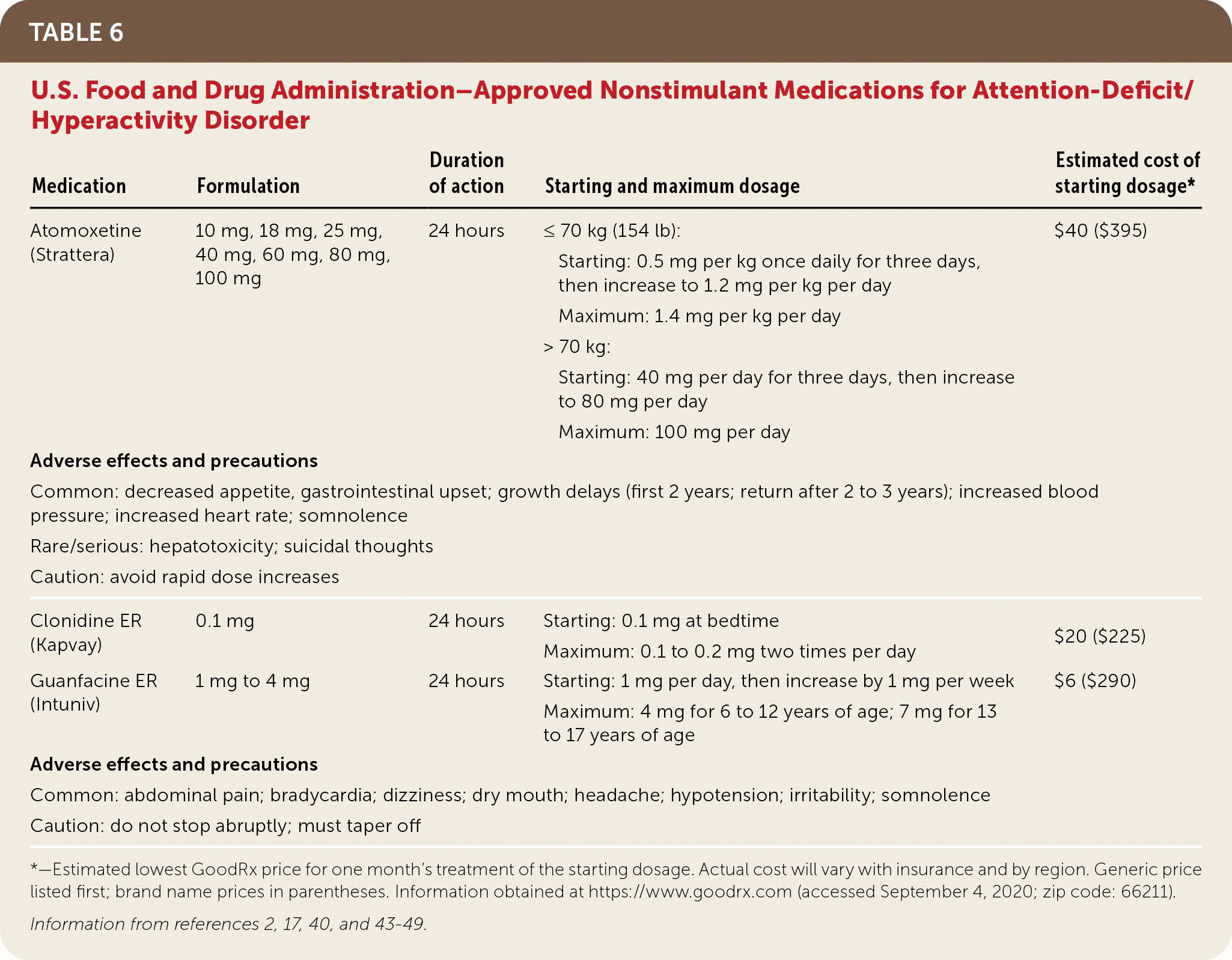
| Medication | Formulation | Duration of action | Starting and maximum dosage | Estimated cost of starting dosage* |
|---|---|---|---|---|
| Atomoxetine (Strattera) | 10 mg, 18 mg, 25 mg, 40 mg, 60 mg, 80 mg, 100 mg | 24 hours | ≤ 70 kg (154 lb): Starting: 0.5 mg per kg once daily for three days, then increase to 1.2 mg per kg per day Maximum: 1.4 mg per kg per day > 70 kg: Starting: 40 mg per day for three days, then increase to 80 mg per day Maximum: 100 mg per day | $40 ($395) |
| Adverse effects and precautions | ||||
| Common: decreased appetite, gastrointestinal upset; growth delays (first 2 years; return after 2 to 3 years); increased blood pressure; increased heart rate; somnolence | ||||
| Rare/serious: hepatotoxicity; suicidal thoughts | ||||
| Caution: avoid rapid dose increases | ||||
| Clonidine ER (Kapvay) | 0.1 mg | 24 hours | Starting: 0.1 mg at bedtime Maximum: 0.1 to 0.2 mg two times per day | $20 ($225) |
| Guanfacine ER (Intuniv) | 1 mg to 4 mg | 24 hours | Starting: 1 mg per day, then increase by 1 mg per week Maximum: 4 mg for 6 to 12 years of age; 7 mg for 13 to 17 years of age | $6 ($290) |
| Adverse effects and precautions | ||||
| Common: abdominal pain; bradycardia; dizziness; dry mouth; headache; hypotension; irritability; somnolence | ||||
| Caution: do not stop abruptly; must taper off | ||||
*—Estimated lowest GoodRx price for one month's treatment of the starting dosage. Actual cost will vary with insurance and by region. Generic price listed first; brand name prices in parentheses. Information obtained at https://www.goodrx.com (accessed September 4, 2020; zip code: 66211).
EVIDENCE SUMMARY
A retrospective cohort study (median age at follow-up was 18.4 years; N = 5,718) found that children with ADHD treated with stimulants had favorable long-term school outcomes (i.e., higher reading scores, decreased absenteeism, and decreased grade repetition).51 Smaller short-term, double-blind placebo-controlled RCTs of methylphenidate and mixed amphetamine salts have shown statistically significant decreases in ADHD symptoms and improved performance measures.52,53 A large double-blind placebo-controlled RCT of children with ADHD (six to 16 years of age; N = 516) showed significant response (decrease in ADHD Rating Scale scores) to methylphenidate (number needed to treat [NNT] = 3) and atomoxetine (NNT = 5) when each was compared with placebo.43 Effect sizes were greater for methylphenidate (0.8 to 1.0) than atomoxetine (0.5 to 0.6).43
A meta-analysis (six studies; six to seven years of age, n = 280; eight to 12 years of age, n = 860) of atomoxetine for the treatment of ADHD demonstrated effectiveness in reducing core ADHD symptoms compared with placebo (NNT = 3, six to seven years of age; NNT = 4, eight to 12 years of age).54 A meta-analysis (12 studies; six to 17 years of age; N = 2,276) of alpha-2 receptor agonists for treatment of ADHD found reductions in ADHD symptoms when used as monotherapy (effect size = 0.56 to 0.59) and to a lesser extent when used as an add-on treatment to stimulant medications (effect size = 0.32 to 0.36).44 A comparative network meta-analysis (81 studies) in children five to 17 years of age found amphetamines to be more effective than other medications compared with placebo, although they were less tolerated.55
Stimulants should be started at low doses and titrated weekly to achieve a minimum effective dose (Table 52,17,40,43–49 ). Children six years and older should be offered extended-release formulations of stimulants; additional short-acting doses may be used after school.2,17,27 Initial follow-up is recommended monthly until medication dosing is optimized, and then two to three times per year once a regimen is established.2 Follow-up visits should include body weight, heart rate, and blood pressure measurements, and the assessment of ADHD symptoms and mood.2 Some parents (25% to 70%) and clinicians use drug holidays to test the continued need for medication and to manage adverse effects and tolerance.56 There is some evidence showing a positive effect in growth with long drug holidays during the summer, and improvement in sleep and appetite with short drug holidays on weekends.50,56 Parents and providers should engage in shared decision-making about drug holidays based on parental preference and experiences of the child taking the medication.17,27,50,56
Among elementary and high school students treated with stimulants for ADHD, rates of stimulant use and diversion are reported at 5% to 9% and 7% to 24%, respectively.57 Physicians should assess for use and diversion that may occur by adolescents, parents, classmates, and acquaintances through ongoing evaluation of symptoms, attention to prescription refill requests, and use of prescription drug monitoring programs.2,27,57
What Are Common Adverse Effects of ADHD Medications?
Common adverse effects of stimulant and nonstimulant medications for ADHD include gastrointestinal and constitutional symptoms.40,43,44,50,52–54 Serious adverse effects (i.e., depression, suicidal thoughts, and psychoses) are rare but should be assessed at every follow-up.40,50 Current guidelines do not discuss the use of other medications to manage adverse effects of stimulant medications.2
EVIDENCE SUMMARY
In the Preschool ADHD Treatment Study, discontinuation of stimulants was related to emotionality or irritability.40 A comparison trial in children taking methylphenidate or atomoxetine found that both medications caused decreased appetite, increase in diastolic blood pressure, and a decrease in weight; insomnia was more common with methylphenidate, and somnolence and increased heart rate were reported more with atomoxetine.47 Atomoxetine has been associated with hepatotoxicity, but this is rare.2,50,58 Amphetamines are associated with a decrease in weight and an increase in systolic and diastolic blood pressure.55
Fatigue, sedation, and somnolence are the most commonly reported adverse effects of alpha-2 receptor agonists.44 Rates of discontinuation attributed to adverse effects are similar between alpha-2 receptor agonist and placebo groups.44
In children and young adults with no history or current suspicion of life-threatening cardiac conditions or congenital heart disease, ADHD medications do not increase the risk of serious cardiovascular events including sudden death, myocardial infarction, and stroke.45 Electrocardiography or cardiology referral is recommended only if there are concerning symptoms or family history.2,17,27,45
This article updates previous articles on this topic by Rader, et al.,59 and by Felt, et al.17
Data Sources: A PubMed search was completed in Clinical Queries using the key term attention deficit with additional search terms of therapy, diagnosis, prognosis, natural history, and prevention. Also searched was Essential Evidence Plus using the key terms amphetamine, attention-deficit disorder, hyperactivity, and attention-deficit disorder with hyperactivity. Additional PubMed searches used the key terms ADHD, prevalence, nonpharmacologic, medications, behavioral, psychosocial, diet, and genetics. Search dates: September 2019, January 2020, February 2020, May 2020, and September 4, 2020.
The contents of this article are solely the views of the authors and do not necessarily represent the official views of the Uniformed Services University of the Health Sciences, the U.S. military at large, the U.S. Department of Defense, or the U.S. government.

