To the Editor: Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), the virus that causes coronavirus disease 2019 (COVID-19), has caused a global health crisis. COVID-19 can present with a variety of complications during the course of infection. Rhabdomyolysis is characterized by muscle necrosis and the release of intracellular muscle constituents into the systemic circulation. A prompt diagnosis is a prerequisite for successful treatment and avoiding complications.
We report on 10 patients with rhabdomyolysis associated with COVID-19 who presented to our hospital through the emergency department. COVID-19 diagnosis was made by polymerase chain reaction assay. Pertinent clinical characteristics are summarized in Table 1.
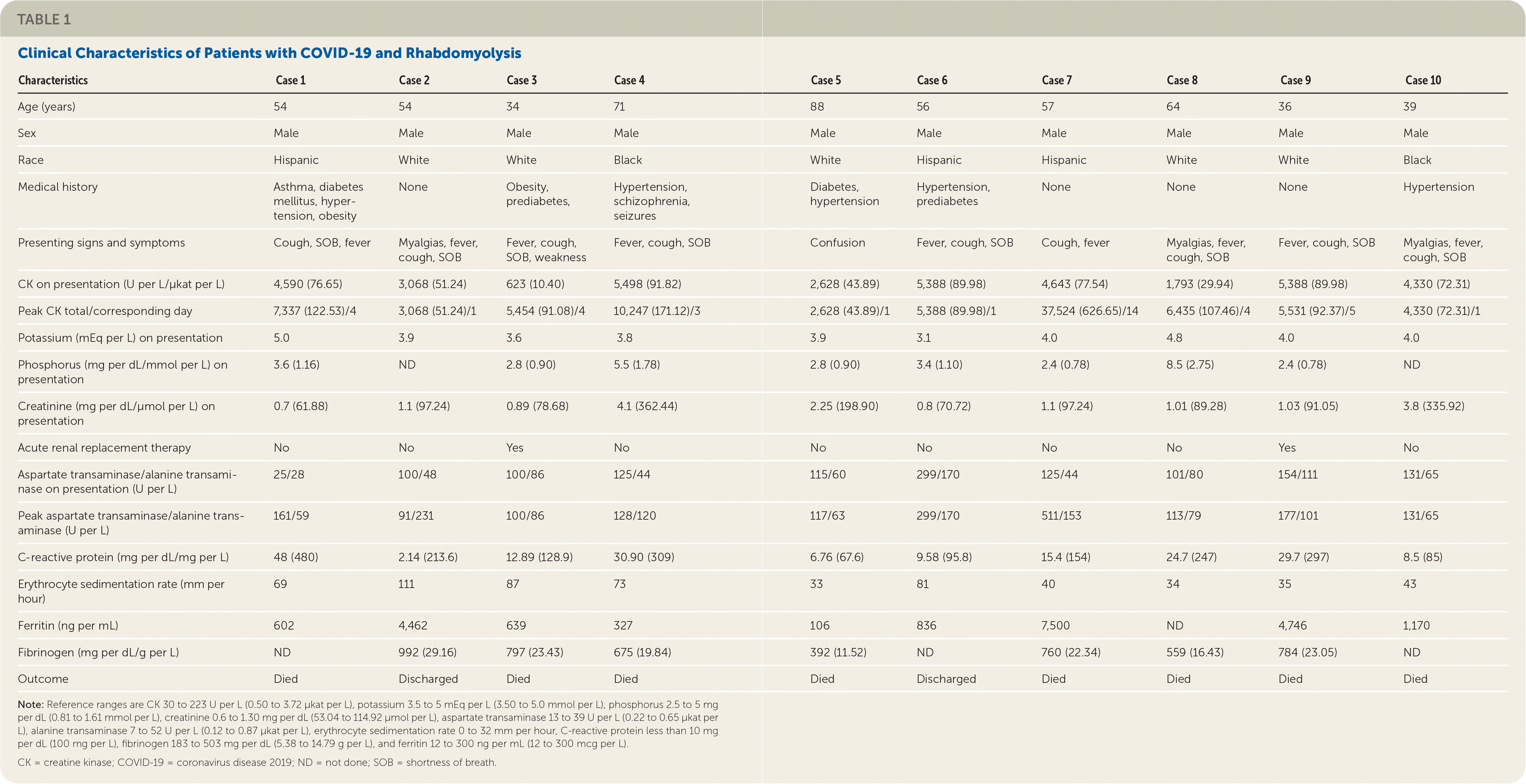
TABLE 1. Clinical Characteristics of Patients with COVID-19 and Rhabdomyolysis
| Characteristics | Case 1 | Case 2 | Case 3 | Case 4 | Case 5 | Case 6 | Case 7 | Case 8 | Case 9 | Case 10 |
|---|---|---|---|---|---|---|---|---|---|---|
| Age (years) | 54 | 54 | 34 | 71 | 88 | 56 | 57 | 64 | 36 | 39 |
| Sex | Male | Male | Male | Male | Male | Male | Male | Male | Male | Male |
| Race | Hispanic | White | White | Black | White | Hispanic | Hispanic | White | White | Black |
| Medical history | Asthma, diabetes mellitus, hypertension, obesity | None | Obesity, prediabetes, | Hypertension, schizophrenia, seizures | Diabetes, hypertension | Hypertension, prediabetes | None | None | None | Hypertension |
| Presenting signs and symptoms | Cough, SOB, fever | Myalgias, fever, cough, SOB | Fever, cough, SOB, weakness | Fever, cough, SOB | Confusion | Fever, cough, SOB | Cough, fever | Myalgias, fever, cough, SOB | Fever, cough, SOB | Myalgias, fever, cough, SOB |
| CK on presentation (U per L/μkat per L) | 4,590 (76.65) | 3,068 (51.24) | 623 (10.40) | 5,498 (91.82) | 2,628 (43.89) | 5,388 (89.98) | 4,643 (77.54) | 1,793 (29.94) | 5,388 (89.98) | 4,330 (72.31) |
| Peak CK total/corresponding day | 7,337 (122.53)/4 | 3,068 (51.24)/1 | 5,454 (91.08)/4 | 10,247 (171.12)/3 | 2,628 (43.89)/1 | 5,388 (89.98)/1 | 37,524 (626.65)/14 | 6,435 (107.46)/4 | 5,531 (92.37)/5 | 4,330 (72.31)/1 |
| Potassium (mEq per L) on presentation | 5.0 | 3.9 | 3.6 | 3.8 | 3.9 | 3.1 | 4.0 | 4.8 | 4.0 | 4.0 |
| Phosphorus (mg per dL/mmol per L) on presentation | 3.6 (1.16) | ND | 2.8 (0.90) | 5.5 (1.78) | 2.8 (0.90) | 3.4 (1.10) | 2.4 (0.78) | 8.5 (2.75) | 2.4 (0.78) | ND |
| Creatinine (mg per dL/μmol per L) on presentation | 0.7 (61.88) | 1.1 (97.24) | 0.89 (78.68) | 4.1 (362.44) | 2.25 (198.90) | 0.8 (70.72) | 1.1 (97.24) | 1.01 (89.28) | 1.03 (91.05) | 3.8 (335.92) |
| Acute renal replacement therapy | No | No | Yes | No | No | No | No | No | Yes | No |
| Aspartate transaminase/alanine transaminase on presentation (U per L) | 25/28 | 100/48 | 100/86 | 125/44 | 115/60 | 299/170 | 125/44 | 101/80 | 154/111 | 131/65 |
| Peak aspartate transaminase/alanine transaminase (U per L) | 161/59 | 91/231 | 100/86 | 128/120 | 117/63 | 299/170 | 511/153 | 113/79 | 177/101 | 131/65 |
| C-reactive protein (mg per dL/mg per L) | 48 (480) | 2.14 (213.6) | 12.89 (128.9) | 30.90 (309) | 6.76 (67.6) | 9.58 (95.8) | 15.4 (154) | 24.7 (247) | 29.7 (297) | 8.5 (85) |
| Erythrocyte sedimentation rate (mm per hour) | 69 | 111 | 87 | 73 | 33 | 81 | 40 | 34 | 35 | 43 |
| Ferritin (ng per mL) | 602 | 4,462 | 639 | 327 | 106 | 836 | 7,500 | ND | 4,746 | 1,170 |
| Fibrinogen (mg per dL/g per L) | ND | 992 (29.16) | 797 (23.43) | 675 (19.84) | 392 (11.52) | ND | 760 (22.34) | 559 (16.43) | 784 (23.05) | ND |
| Outcome | Died | Discharged | Died | Died | Died | Discharged | Died | Died | Died | Died |
Note: Reference ranges are CK 30 to 223 U per L (0.50 to 3.72 μkat per L), potassium 3.5 to 5 mEq per L (3.50 to 5.0 mmol per L), phosphorus 2.5 to 5 mg per dL (0.81 to 1.61 mmol per L), creatinine 0.6 to 1.30 mg per dL (53.04 to 114.92 μmol per L), aspartate transaminase 13 to 39 U per L (0.22 to 0.65 μkat per L), alanine transaminase 7 to 52 U per L (0.12 to 0.87 μkat per L), erythrocyte sedimentation rate 0 to 32 mm per hour, C-reactive protein less than 10 mg per dL (100 mg per L), fibrinogen 183 to 503 mg per dL (5.38 to 14.79 g per L), and ferritin 12 to 300 ng per mL (12 to 300 mcg per L).
CK = creatine kinase; COVID-19 = coronavirus disease 2019; ND = not done; SOB = shortness of breath.
The median age of the participants was 55 years and all were male. Presenting symptoms included cough, shortness of breath, fever, myalgias, and confusion. None of the patients were receiving statins or other medications known to cause rhabdomyolysis or had risk factors for rhabdomyolysis. The median creatine kinase level on presentation was 4,460 U per L (74.48 μkat per L). Three patients had acute kidney injury on presentation and liver enzymes were elevated in all patients except one. Inflammatory markers (erythrocyte sedimentation rate, C-reactive protein, fibrinogen, and ferritin) were elevated in all patients. Influenza was negative in five patients and other viral causes of rhabdomyolysis (e.g., parainfluenza, enterovirus, adenovirus) were negative in four patients.1 Eight out of 10 patients died.
Acute viral infections associated with rhabdomyolysis include influenza A and B, coxsackieviruses, Epstein-Barr virus, herpes simplex, parainfluenza, adenovirus, echo-virus, HIV, and cytomegalovirus.2 Others have reported cases of rhabdomyolysis associated with COVID-19.3,4 The pathologic mechanism leading to this complication is currently unknown. Clinicians should be aware of this life-threatening manifestation of COVID-19 so that prompt and appropriate interventions can be undertaken if it is suspected or confirmed. Further studies are needed to characterize the muscle injury consequences of SARS-CoV-2 infection.

