Clinical Question
Is beta-blocker administration beneficial in the setting of acute myocardial infarction (MI)?
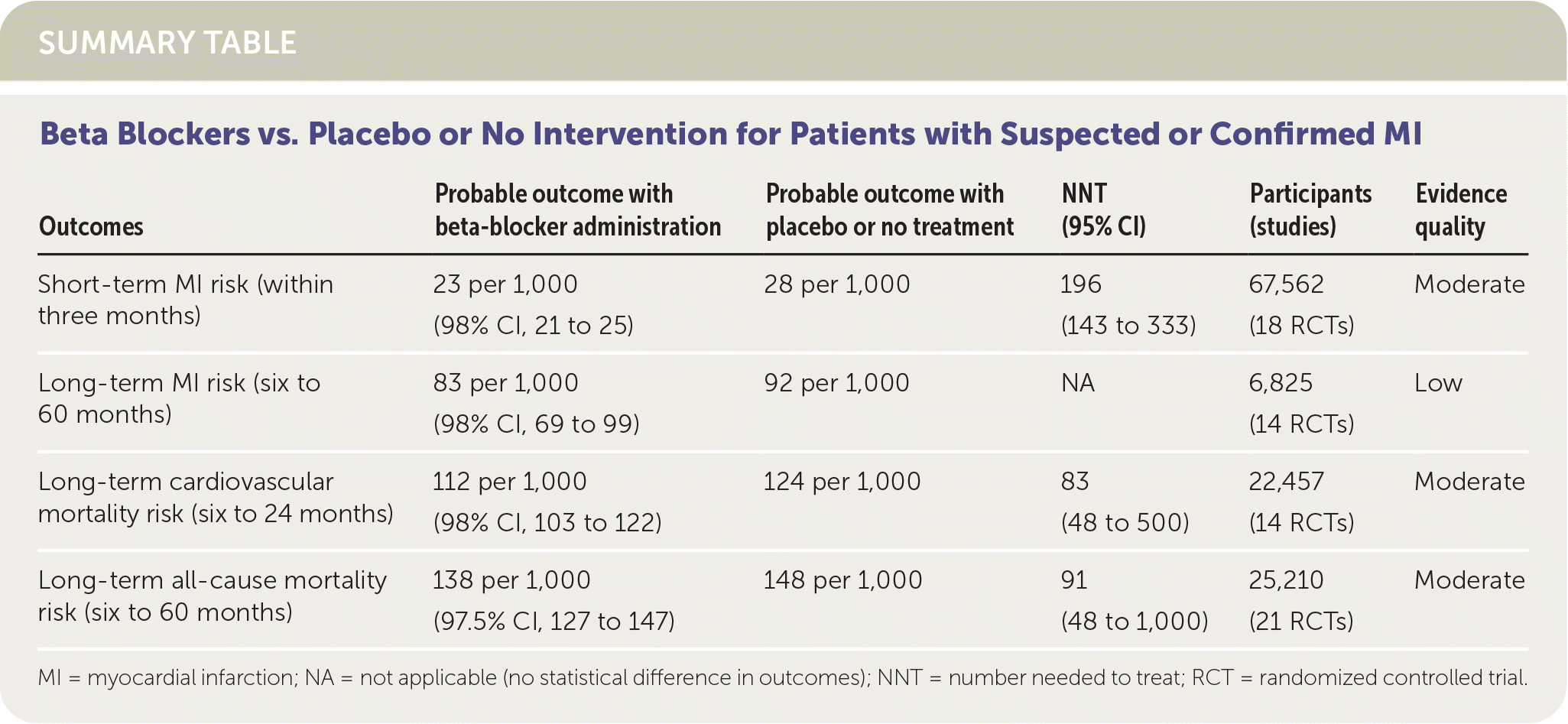
SUMMARY TABLE
| Outcomes | Probable outcome with beta-blocker administration | Probable outcome with placebo or no treatment | NNT (95% CI) | Participants (studies) | Evidence quality |
|---|---|---|---|---|---|
| Short-term MI risk (within three months) | 23 per 1,000 (98% CI, 21 to 25) | 28 per 1,000 | 196 (143 to 333) | 67,562 (18 RCTs) | Moderate |
| Long-term MI risk (six to 60 months) | 83 per 1,000 (98% CI, 69 to 99) | 92 per 1,000 | NA | 6,825 (14 RCTs) | Low |
| Long-term cardiovascular mortality risk (six to 24 months) | 112 per 1,000 (98% CI, 103 to 122) | 124 per 1,000 | 83 (48 to 500) | 22,457 (14 RCTs) | Moderate |
| Long-term all-cause mortality risk (six to 60 months) | 138 per 1,000 (97.5% CI, 127 to 147) | 148 per 1,000 | 91 (48 to 1,000) | 25,210 (21 RCTs) | Moderate |
MI = myocardial infarction; NA = not applicable (no statistical difference in outcomes); NNT = number needed to treat; RCT = randomized controlled trial.
Evidence-Based Answer
Compared with placebo, beta-blocker use in patients with acute MI reduces short-term (less than three months) risk of MI (number needed to treat [NNT] = 196; 95% CI, 143 to 333) and long-term (more than three months) risk of cardiovascular mortality (NNT = 83; 95% CI, 48 to 500) and all-cause mortality (NNT = 91; 95% CI, 48 to 1,000). There are no significant harms.1 (Strength of Recommendation: A, based on consistent, good-quality patient-oriented evidence.)
Practice Pointers
Heart disease was the leading cause of death in the United States in 2018, according to data from the Centers for Disease Control and Prevention.2 Among the contributors to death from heart disease are the acute coronary syndromes, which include ST elevation MI (STEMI), non–ST elevation MI (NSTEMI), and unstable angina. This Cochrane review examined whether beta-blocker administration in the acute or subacute phase after MI impacts morbidity and/or mortality.1
The authors included 63 randomized controlled trials and 85,550 patients and evaluated the use of beta blockers compared with placebo or no intervention in people with suspected or acute MI. Trials were conducted between 1966 and 2018 in 31 countries, including 15 trials in the United Kingdom and four in the United States. The mean patient age was 57.4 years (range = 45.9 to 70.0 years), and 25.5% of participants were women. Fifty-six trials examined beta-blocker use in the post-MI acute phase (within 48 hours of symptom onset), whereas the remaining seven trials considered the subacute phase (three days to 21 days after symptom onset). Selective and nonselective beta blockers were used; the most common was propranolol, which is nonselective. Most trials included all acute coronary syndromes, whereas seven focused only on the use of beta blockers in patients with STEMI. Primary outcomes were all-cause mortality and major adverse cardiovascular events (MACE, encompassing cardiovascular mortality and nonfatal MI), as well as risk of other serious adverse events. Secondary outcomes included quality of life, angina, cardiovascular mortality, and recurrent MI. Each outcome was considered in the short term (less than three months) and long term (six to 60 months).
This Cochrane review demonstrated a significant reduction in long-term all-cause and cardiovascular mortality with beta blockers. They also reduced the short-term risk of MI. Use of beta blockers did not reduce the risk of angina, and there was insufficient evidence to determine if their use altered quality-of-life scores, MACE, or other serious adverse events. It is notable that most trials were conducted before the introduction of what is now standard reperfusion therapy. However, a reassuring subgroup analysis found that the above conclusions were statistically valid for patients who had and had not received reperfusion therapy (coronary artery bypass grafting, percutaneous coronary intervention, or thrombolytics).
Current guidelines for the management of STEMI and NSTEMI acute coronary syndromes (including unstable angina) recommend initiation of beta-blocker therapy within the first 24 hours of presentation and continuation after hospitalization for patients without contraindications.3,4 Family physicians should continue to incorporate beta-blocker therapy in the care of patients with a history of MI.
The practice recommendations in this activity are available at http://www.cochrane.org/CD012484.
Editor's Note: The numbers needed to treat and CIs reported in this Cochrane for Clinicians were calculated by the authors based on raw data provided in the original Cochrane review.
The definition of “early” beta blocker used in this review should not be interpreted as “immediate” because in the included studies early use was defined as initiation within 48 hours to up to 21 days after a myocardial infarction; immediate use of intravenous beta blockers may be harmful. Consistent with the cited guidelines, clinicians should consider initiating oral beta blockers no sooner than 24 hours post myocardial infarction, and only then when the patient is hemodynamically stable.

