Ulcerative colitis is a relapsing and remitting inflammatory bowel disease of the large intestine. Risk factors include recent Salmonella or Campylobacter infection and a family history of ulcerative colitis. Diagnosis is suspected based on symptoms of urgency, tenesmus, and hematochezia and is confirmed with endoscopic findings of continuous inflammation from the rectum to more proximal colon, depending on the extent of disease. Fecal calprotectin may be used to assess disease activity and relapse. Medications available to treat the inflammation include 5-aminosalicylic acid, corticosteroids, tumor necrosis factor–alpha antibodies, anti-integrin antibodies, anti-interleukin-12 and -23 antibodies, and Janus kinase inhibitors. Choice of medication and method of delivery depend on the location and severity of mucosal inflammation. Other treatments such as fecal microbiota transplantation are considered experimental, and complementary therapies such as probiotics and curcumin have mixed data. Surgical treatment may be needed for fulminant or refractory disease. Increased risk of colorectal cancer and use of immunosuppressive therapies affect the preventive care needs for these patients.
Ulcerative colitis is a relapsing and remitting inflammatory bowel disease frequently encountered in primary care. This article provides a summary of ulcerative colitis and a review of the available evidence for management.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
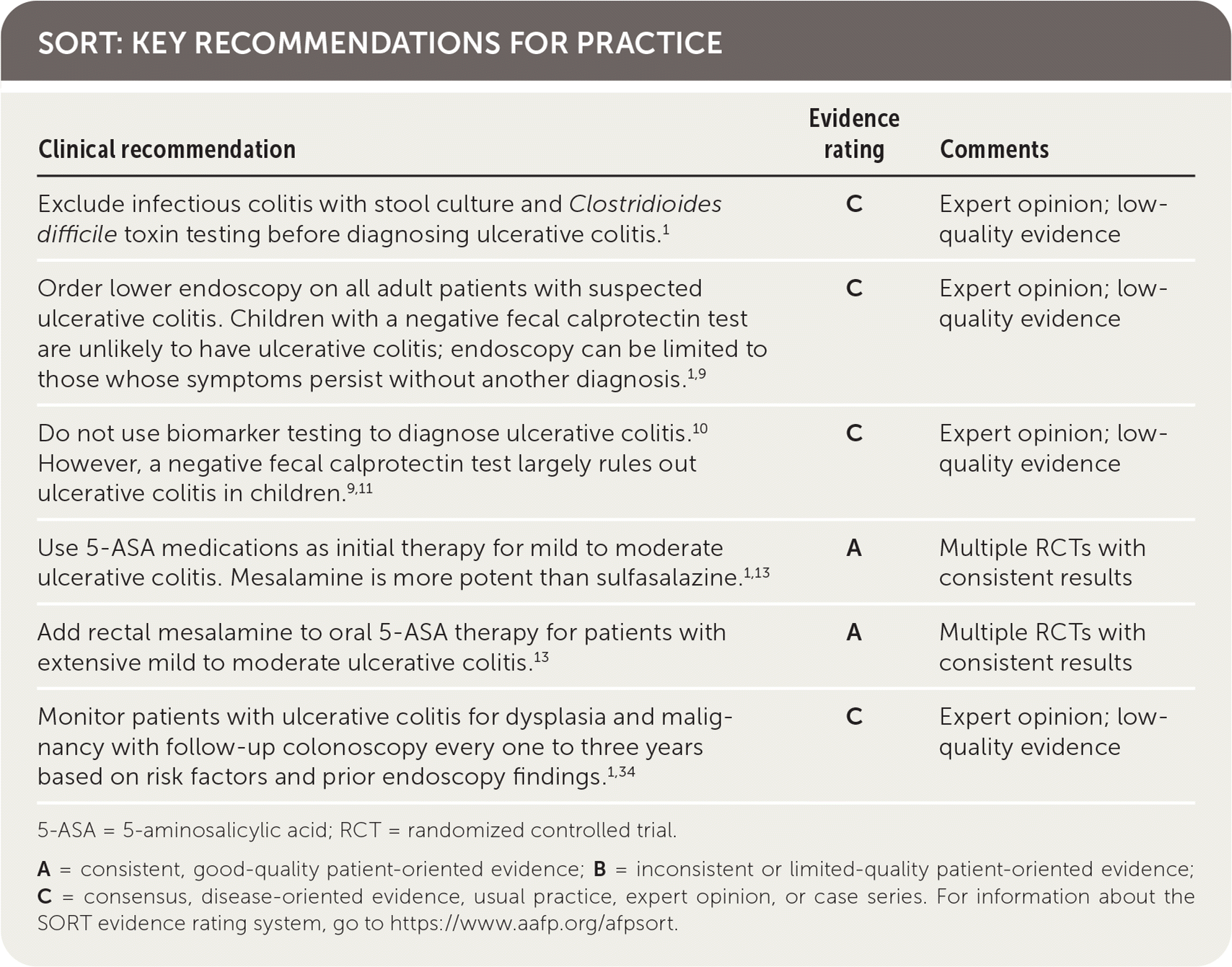
5-ASA = 5-aminosalicylic acid; RCT = randomized controlled trial.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Epidemiology and Risk Factors
- Ulcerative colitis most commonly presents between 15 and 30 years of age and is more common in industrialized nations, with a prevalence of 286 per 100,000 adults in the United States.1,2
- Incidence is similar in men and women.3
- Risk factors include urban living; family history of ulcerative colitis; recent Salmonella, Clostridioides difficile, or Campylobacter infection; tobacco cessation; and soda consumption.4,5
- Protective factors include history of appendectomy, active tobacco use, tea consumption, and having been breastfed as an infant.4,5
Diagnosis
DIFFERENTIAL DIAGNOSIS
- Active Salmonella, Shigella, Escherichia coli, Yersinia, Campylobacter, or C. difficile infection should be ruled out using stool studies.1
- Amebic dysentery should be considered if an appropriate travel or exposure history exists. Cytomegalovirus infection should be excluded in immunocompromised patients.1
- Other causes of bloody diarrhea include ischemic colitis, Crohn disease, and colitis caused by medications or radiation. Non-bloody diarrhea can be caused by microscopic colitis, irritable bowel syndrome, celiac disease, or food intolerances.6
SIGNS AND SYMPTOMS
- The most common presenting symptom is bloody diarrhea. Other common symptoms include abdominal pain, tenesmus, and fecal urgency.1,2
- Extraintestinal manifestations include arthropathies, erythema nodosum, pyoderma gangrenosum, uveitis, iritis, and primary sclerosing cholangitis. These may be present before the onset of gastrointestinal symptoms.7,8
- Overall, extraintestinal manifestations are only 6% more common in patients with inflammatory bowel disease than in the general population and are more common with Crohn disease compared with ulcerative colitis.8
DIAGNOSTIC TESTING
- Lower endoscopy should be performed on all adult patients with suspected ulcerative colitis.1,9
- Fecal calprotectin testing has a high negative predictive value and helps to differentiate inflammatory bowel disease from irritable bowel syndrome, but no serum biomarkers alone are sufficient for the diagnosis of ulcerative colitis.10 A normal fecal calprotectin level (100 mcg per g or less) in children virtually excludes the diagnosis of ulcerative colitis (100% negative predictive value; 95% CI, 98% to 100%). Therefore, in children with a negative fecal calprotectin test, endoscopy can be limited to those whose symptoms persist without another diagnosis.9,11
- Bacterial stool culture, including C. difficile toxin assay and stool examination for ova and parasites, should be performed. Other tests, such as complete blood count, erythrocyte sedimentation rate, and measurement of C-reactive protein, may be useful but are nonspecific.1
- Endoscopic evidence of continuous colonic inflammation starting at the rectum with confirmatory biopsies establishes the diagnosis of ulcerative colitis.1
- Elevation in serial measurements of fecal calprotectin predicts relapse, whereas serial values in the normal range predict continued remission over time.12
Treatment
INDUCTION AND MAINTENANCE OF REMISSION
- The goal of managing patients with ulcerative colitis is to attain mucosal healing with symptom control so that sustained steroid-free remission can be achieved and prevent hospitalizations and surgeries.
- Initiation of treatment begins with stratifying disease activity into mild vs. moderate to severe. The American College of Gastroenterology Ulcerative Colitis Activity Index provides a set of criteria to help determine if the disease is in remission, mild, moderate to severe, or fulminant.1
- Therapy and medication delivery modes (Table 1) are based on the location and extent of mucosal inflammation. This is broadly divided into proctitis (i.e., 18 cm from the true anal verge), left-sided colitis (i.e., extending to the splenic flexure), and pancolitis (i.e., extending proximal to the splenic flexure).1
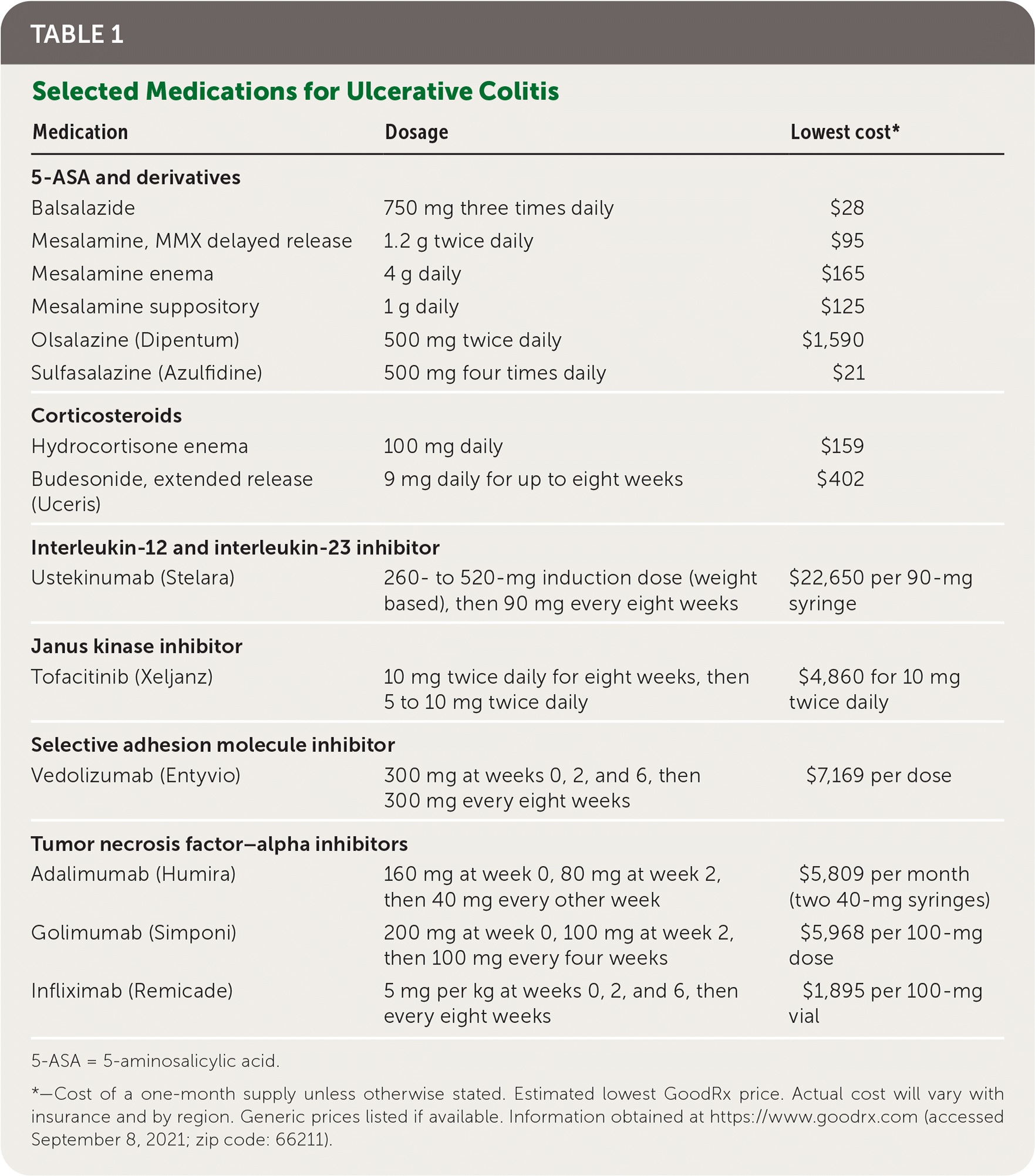
TABLE 1. Selected Medications for Ulcerative Colitis
| Medication | Dosage | Lowest cost* |
|---|---|---|
| 5-ASA and derivatives | ||
| Balsalazide | 750 mg three times daily | $28 |
| Mesalamine, MMX delayed release | 1.2 g twice daily | $95 |
| Mesalamine enema | 4 g daily | $165 |
| Mesalamine suppository | 1 g daily | $125 |
| Olsalazine (Dipentum) | 500 mg twice daily | $1,590 |
| Sulfasalazine (Azulfidine) | 500 mg four times daily | $21 |
| Corticosteroids | ||
| Hydrocortisone enema | 100 mg daily | $159 |
| Budesonide, extended release (Uceris) | 9 mg daily for up to eight weeks | $402 |
| Interleukin-12 and interleukin-23 inhibitor | ||
| Ustekinumab (Stelara) | 260- to 520-mg induction dose (weight based), then 90 mg every eight weeks | $22,650 per 90-mg syringe |
| Janus kinase inhibitor | ||
| Tofacitinib (Xeljanz) | 10 mg twice daily for eight weeks, then 5 to 10 mg twice daily | $4,860 for 10 mg twice daily |
| Selective adhesion molecule inhibitor | ||
| Vedolizumab (Entyvio) | 300 mg at weeks 0, 2, and 6, then 300 mg every eight weeks | $7,169 per dose |
| Tumor necrosis factor–alpha inhibitors | ||
| Adalimumab (Humira) | 160 mg at week 0, 80 mg at week 2, then 40 mg every other week | $5,809 per month (two 40-mg syringes) |
| Golimumab (Simponi) | 200 mg at week 0, 100 mg at week 2, then 100 mg every four weeks | $5,968 per 100-mg dose |
| Infliximab (Remicade) | 5 mg per kg at weeks 0, 2, and 6, then every eight weeks | $1,895 per 100-mg vial |
5-ASA = 5-aminosalicylic acid.
*—Cost of a one-month supply unless otherwise stated. Estimated lowest GoodRx price. Actual cost will vary with insurance and by region. Generic prices listed if available. Information obtained at https://www.goodrx.com (accessed September 8, 2021; zip code: 66211).
TREATMENT OF MILD DISEASE
- The 2019 guidelines from the American College of Gastroenterology recommend treatment of mild ulcerative proctitis with rectal 5-amino-salicylic acid (5-ASA) therapies.1
- Mild to moderate colitis should be treated with a combination of rectal 5-ASA enemas and oral 5-ASA therapies. Rectal 5-ASA enemas are preferred to rectal steroid formulations. Mesalamine is more potent than sulfasalazine for inducing remission.1,13
- Patients who are unresponsive to or intolerant of 5-ASA should use oral budesonide, extended release (Uceris; multimatrix formulation designed to deliver medication to the colonic mucosa).1
TREATMENT OF MODERATE TO SEVERE DISEASE
- First-line therapy for moderate to severe ulcerative colitis is biologics.14
- Biologic agents with or without glucocorticoids and immune modulators should be used to induce and maintain remission. Thiopurines or methotrexate should not be used as monotherapy.1
- Systemic corticosteroids are effective in inducing remission, but dosages and treatment duration should be limited. Other options for inducing remission include tumor necrosis factor–alpha antibodies, anti-integrin antibodies, anti-interleukin antibodies, and Janus kinase inhibitors1 (Table 1).
- Fecal microbiota transplantation induces remission in some patients with ulcerative colitis, but current use is limited to clinical trials.15–17
SURGICAL TREATMENT
- Among patients with ulcerative colitis, 15% will ultimately need colectomy. Indications include failure of medical therapy, toxic megacolon, perforation, uncontrolled hemorrhage, or dysplasia/malignancy.7
- About 50% of patients who undergo colectomy will experience postoperative inflammation of the residual rectal tissue.18
- Predictors for aggressive disease include age younger than 40 years, pancolitis, severe disease activity seen on endoscopy, presence of extraintestinal manifestations, early need for steroids, and elevated inflammatory markers.1
COMPLEMENTARY MEDICINE
- One probiotic (VSL#3) modestly improves symptoms. It also helps to prevent pouchitis, an abnormal immune response in patients susceptible to autoimmune disease that leads to inflammation of the rectal pouch fashioned after a colectomy.19–21
- A systematic review of six small studies found that curcumin (2 to 3 g daily) promotes clinical and endoscopic improvement when added to conventional therapy in patients with mild ulcerative colitis.22
- Fish oil does not improve remission rates.23,24
- Acupuncture is considered safe in addition to conventional treatment, but high-quality evidence of effectiveness is lacking.25
LIFESTYLE AND BEHAVIORAL INTERVENTIONS
- Exercise and diet interventions help improve symptom burden and quality of life.
- A low fermentable oligosaccharides, disaccharides, monosaccharides, and polyols (FODMAP) diet reduces symptoms but does not change clinical severity.26,27
- Physical activity improves quality of life and the anxiety that commonly affects patients with inflammatory bowel disease.28
HOSPITAL CARE
- Up to 25% of patients with ulcerative colitis will require hospitalization for severe disease.
- Early endoscopy should be performed to exclude cytomegalovirus colitis, and C. difficile testing should be ordered.
- Avoidance of nonsteroidal anti-inflammatory drugs, opiates, and anticholinergic medications is recommended. Antibiotics should not be used routinely.
- Surgical consultation should be obtained for patients not responding to intravenous corticosteroids after three days, or earlier if other surgical indications (e.g., toxic megacolon) arise.
- If there is failure of intravenous corticosteroids after three days of treatment, cyclosporine (Sandimmune) or infliximab (Remicade) may be used as rescue therapy.29
Preventive Care Considerations
- Vaccinations should be given according to routine recommendations from the Advisory Committee on Immunization Practices and the Centers for Disease Control and Prevention, paying special attention to additional vaccinations necessary for patients on immunosuppressive therapies.30
- Dual energy x-ray absorptiometry is recommended to check for low bone mineral density in patients with ulcerative colitis, especially those with a history of chronic oral corticosteroid use for three months or more.31
- Skin cancer occurs at higher rates in patients with inflammatory bowel disease. In addition, common therapies for ulcerative colitis increase the risk of melanoma and nonmelanoma skin cancer.32
- The American College of Obstetricians and Gynecologists recommends annual cytology screening for cervical cancer in women on immunosuppressive therapy.33
- Colonoscopy is recommended starting eight years after diagnosis of ulcerative colitis or immediately if primary sclerosing cholangitis is also present because of an increased risk of colorectal cancer. Interval surveillance in those with disease proximal to the sigmoid colon should occur every one to three years based on risk factors and prior endoscopy findings, with annual colonoscopies in patients with concomitant primary sclerosing cholangitis, due to very high risk of developing colorectal cancer.1,34
Prognosis
- Most patients with ulcerative colitis experience a mild to moderate course with periods of remission and flare-ups.
- Ulcerative colitis does not increase mortality but is associated with high morbidity.7
ULCERATIVE COLITIS AND COVID-19
- Based on a panel of international experts, in the absence of definitive data, the American Gastroenterological Association has concluded that the risk of a patient with ulcerative colitis becoming infected with SARS-CoV-2 is no higher than that of the general population, independent of treatment.
- It is unknown whether active inflammation from ulcerative colitis can increase the risk of infection with SARS-CoV-2.
- The American Gastroenterological Association recommends ongoing biologic therapy, deeming it safe for patients who are on such medications to continue working in environments with those who have known or suspected SARS-CoV-2 infection.
- Patients who test positive for SARS-CoV-2 and whose ulcerative colitis medications are held because of this can restart their medications after 14 days if they do not develop symptoms or if symptoms resolve.35
- A retrospective review of patients vaccinated against SARS-CoV-2 suggests the vaccine effectiveness and adverse event rate in patients with inflammatory bowel disease is similar to the general population.36
This article updates a previous article on this topic by Adams and Bornemann.37
Data Sources: This article was based on ACG and AGA Guidelines, the Cochrane database, Essential Evidence Plus, and a PubMed search including meta-analyses, randomized controlled trials, and systematic reviews. Search dates: December 2020 through October 2021.

