Physical activity has many health-related benefits, including prevention and management of chronic disease, weight management, and improved mental health. Active girls and women of all ages and abilities are at risk of relative energy deficiency in sport, a syndrome encompassing low energy availability, menstrual irregularities, and disordered bone metabolism. Presence of amenorrhea or oligomenorrhea may suggest reduced energy availability. Active females are at risk of overuse injuries, including patellofemoral pain syndrome, iliotibial band syndrome, and stress fractures; treatment usually includes activity modification, a period of rest, and physical therapy. Active females are also at risk of acute injuries, including concussion and anterior cruciate ligament injuries. Pregnant patients without contraindications who were physically active before pregnancy can continue these activities, and those who were not previously active may gradually increase their activity level to a goal of 150 minutes per week. Moderate exercise during pregnancy reduces the risk of gestational diabetes mellitus, preeclampsia, and cesarean delivery. Postpartum exercise focused on core and pelvic floor strengthening can improve pelvic floor dysfunction. Supervised exercise programs focused on strength and balance have been consistently shown to reduce the risk of falls and injurious falls in older women.
Since the passing of Title IX in 1972, female participation in sports at all levels has steadily increased1; however, overall, females continue to be less active than males, starting in childhood.2 Active play in childhood has a major impact on weight management, socialization, and self-confidence. Girls can be encouraged to be physically active during early childhood to cultivate a lifetime enjoyment of sport. Education on participation in multiple sports as opposed to early specialization can help promote this enjoyment because children who participate in multiple sports are less likely to experience overuse injury and burnout.3,4 The benefits from athletics in childhood continue throughout adulthood. In adult women, exercise is associated with myriad benefits, including reduced risk of depression, chronic diseases (e.g., cardiovascular disease, chronic obstructive pulmonary disease, diabetes mellitus, obesity), breast and ovarian cancers, and falls and fractures. Although there are significant benefits of exercise across all populations and ages, active females are also at risk of overuse and traumatic injuries. This article discusses special considerations for the active, female-gender-assigned-at-birth patient. Information about caring for transgender athletes can be found in a previous issue of American Family Physician (AFP).5,6
SORT: KEY RECOMMENDATIONS FOR PRACTICE
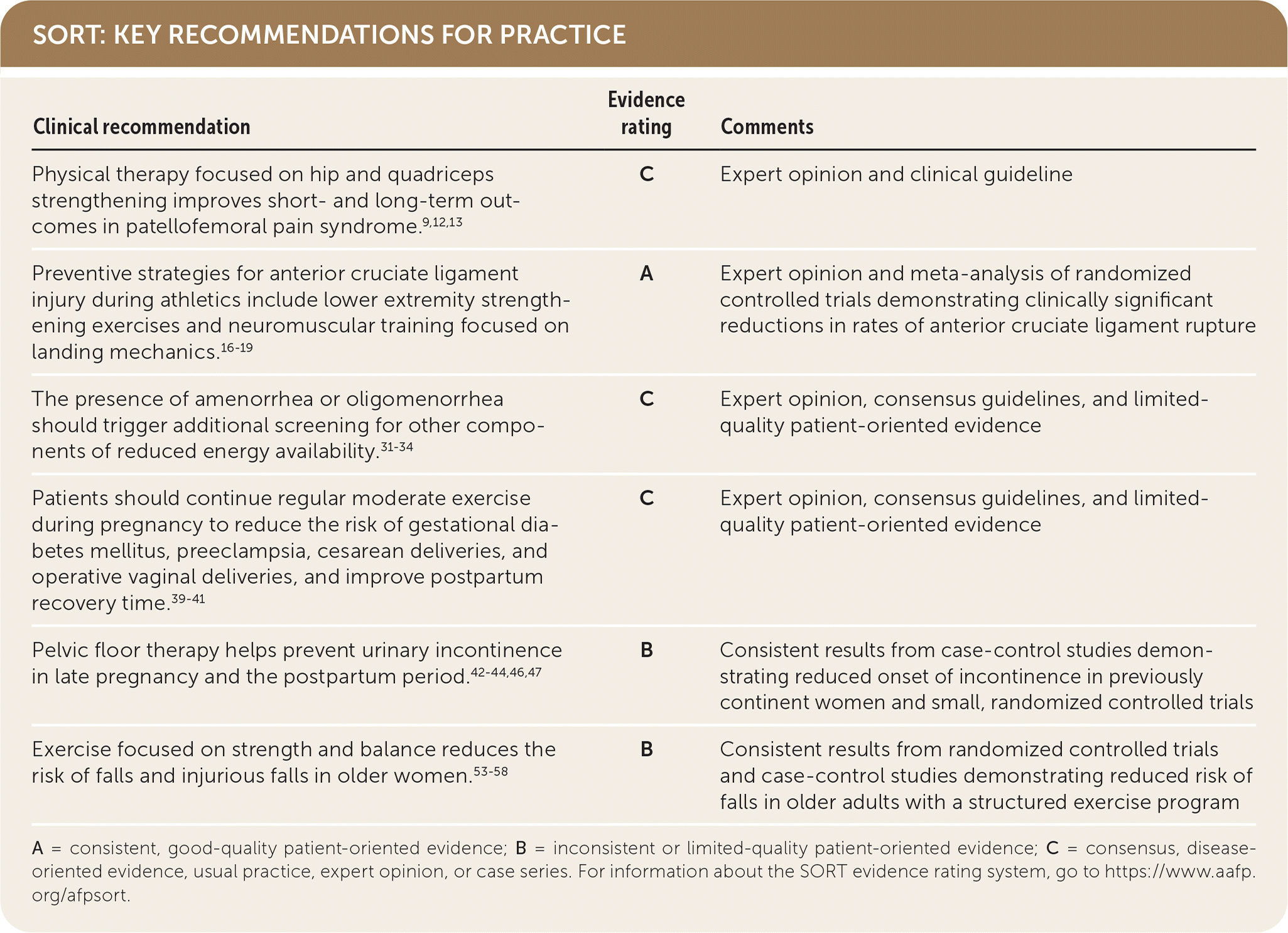
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Common Concerns in the Active Female
OVERUSE INJURIES
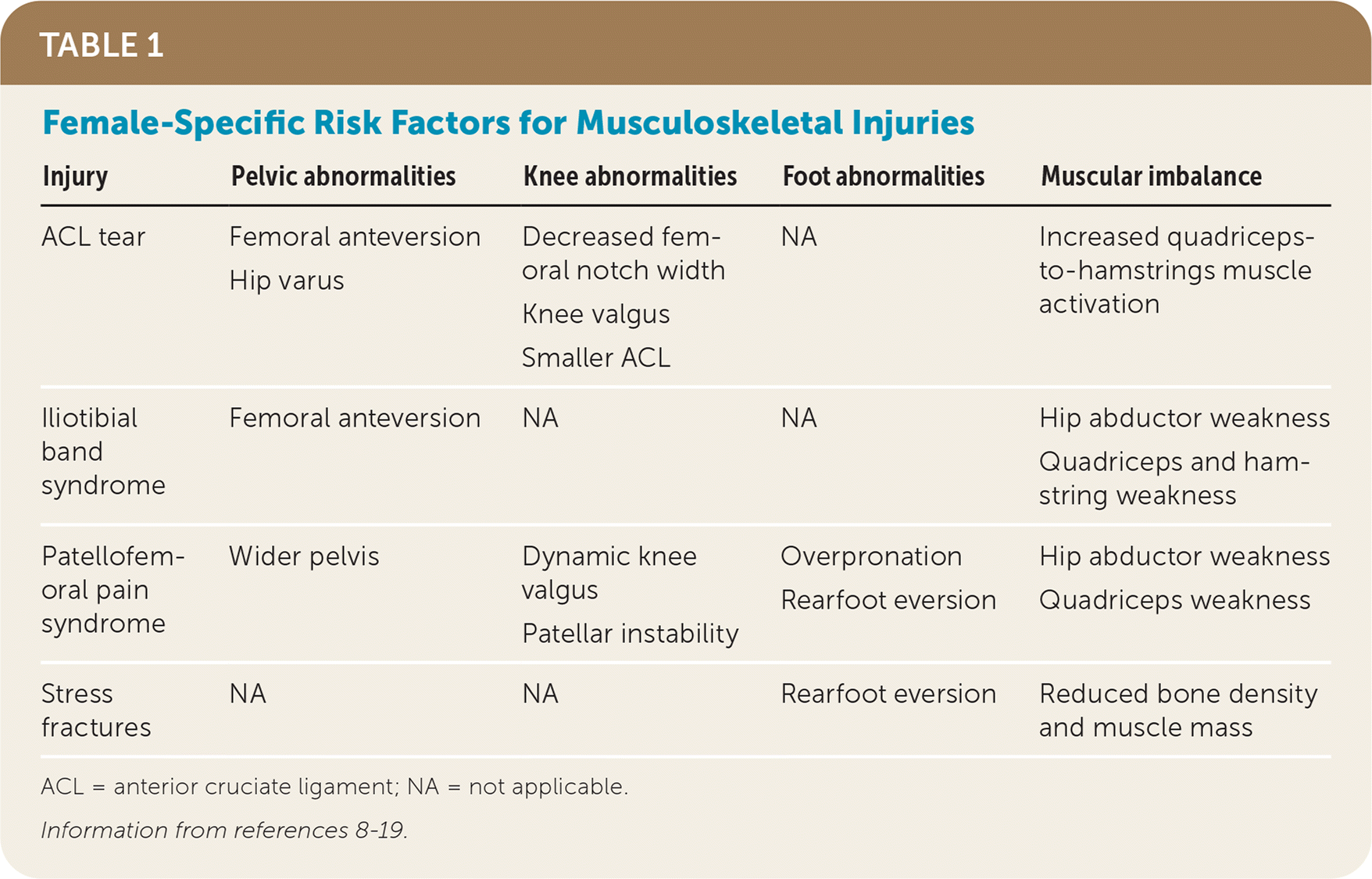
Overuse injuries are more common in active females than acute musculoskeletal injuries.7,8 Several anatomic considerations predispose females to specific overuse injuries, including iliotibial band syndrome, patellofemoral pain syndrome, and stress fractures; Table 1 describes these considerations, which include pelvic and knee alignment, increased joint laxity, and decreased average muscle mass compared with males.8–19
TABLE 1. Female-Specific Risk Factors for Musculoskeletal Injuries
| Injury | Pelvic abnormalities | Knee abnormalities | Foot abnormalities | Muscular imbalance |
|---|---|---|---|---|
| ACL tear | Femoral anteversion Hip varus | Decreased femoral notch width Knee valgus Smaller ACL | NA | Increased quadriceps to-hamstrings muscle activation |
| Iliotibial band syndrome | Femoral anteversion | NA | NA | Hip abductor weakness Quadriceps and hamstring weakness |
| Patellofemoral pain syndrome | Wider pelvis | Dynamic knee valgus Patellar instability | Overpronation Rearfoot eversion | Hip abductor weakness Quadriceps weakness |
| Stress fractures | NA | NA | Rearfoot eversion | Reduced bone density and muscle mass |
ACL = anterior cruciate ligament; NA = not applicable.
Patellofemoral pain syndrome, one of the most common knee problems affecting females, causes knee pain as the patella glides along the femoral condyles. Patients present with insidious onset, poorly localized anterior knee pain exacerbated by using stairs and prolonged sitting, kneeling, and squatting. Patellofemoral pain syndrome is more common in females compared with males, and 70% of cases present between 16 and 25 years of age.8,9 Risk factors include repetitive knee flexion and extension activities, including running and squatting, knee and foot position, increased activity, and quadriceps weakness9–13 (Table 18–19). Physical therapy focused on posterior hip and quadriceps exercises results in more short- and long-term benefits than quadriceps exercises alone.9,12,13 Patellar taping and bracing and foot orthoses for those with overpronation offer short-term improvement when combined with therapy but do not show prolonged benefit. Ice and anti-inflammatories may also provide short-term relief.12,13
Iliotibial band syndrome is a common cause of lateral knee pain in female athletes due to repetitive knee flexion and extension activities. Risk factors include high weekly running mileage and weak hip abductors.13 Patients describe insidious onset, lateral knee pain following activities that is worse with downhill running or a longer stride. A short period of active rest, stretching, anti-inflammatories, and exercises to strengthen hip abductor muscles offer short-term benefit. Most patients return to activity in two to six weeks.
Stress fractures occur in males and females due to overtraining or increased repetitive forces; however, females have a higher incidence of stress fractures.13,14 Lower-extremity bones are usually affected; the tibia is the most common location for all patients, but femoral neck, tarsal navicular, metatarsal, and pelvic stress fractures present more frequently in females than males. Patients describe pain aggravated with activity and often recall an antecedent increase in activity level. On examination, patients present with localized tenderness and pain with range-of-motion exercises. Stress fractures can be reliably diagnosed by magnetic resonance imaging and bone scan, but radiography is often normal. Treatment involves a period of relative rest and protected weight bearing until the patient is symptom free, usually three to four weeks, then progression to full weight bearing and physical therapy with gradual return to activities over four to six weeks. High-risk stress fractures at risk of progression to frank fractures due to poor blood supply or persistent tension forces (i.e., the tension side of the femoral neck, patella, anterior cortex of the tibia, medial malleolus, talus, tarsal navicular, fifth metatarsal, and great toe sesamoids) require orthopedic evaluation.
ACUTE INJURIES
Concussion. A concussion is a traumatic, transient disturbance of brain function as a result of biomechanical forces not due to drug, alcohol, or medication use or other comorbidities.20,21 Females are at increased risk of concussion compared with males playing the same sport.22,23 Females are more likely to report concussive symptoms after a traumatic event24 and have a greater risk of protracted recovery known as persistent postconcussive symptoms.20–23 Contact sports, including football, soccer, basketball, and ice hockey, have the highest risk of concussion, although noncontact sports such as gymnastics and cheerleading also carry significant risk.23 Contact sport participation increases concussions by up to three times.23 Female-specific risk factors include decreased head and neck strength and increased peak head angular acceleration.
Concussions can present with loss of consciousness, seizures, tonic posturing, or gross motor instability but more often involve balance issues, confusion, or amnesia after a head injury.20–23 Initial sideline assessment may be aided by using the Sport Concussion Assessment Tool—5th edition24 (SCAT5; https://bjsm.bmj.com/content/bjsports/51/11/851.full.pdf) or Child SCAT5 (https://bjsm.bmj.com/content/bjsports/early/2017/04/26/bjsports-2017-097492childscat5.full.pdf).
Any athlete with a suspected concussion must immediately be removed from play. There is no safe same-day return-to-play for athletes assumed to be concussed. Most concussion symptoms resolve spontaneously, and most athletes are able to return to pre-injury levels of function within two weeks. Active rest, which involves 24 to 48 hours of symptom-limited cognitive rest immediately after concussion, followed by a gradual increase in activity while staying below symptom thresholds is recommended. New research suggests that early subsymptom threshold physical activity is safe and may improve recovery.20 Electronic device use, crowded or loud activities, and testing may need to be limited and progressed as symptoms improve. All students should be fully integrated in school before initiating a graded return to sport.25
Persistent postconcussive symptoms, which last more than four weeks in children and two weeks in adults, may not reflect ongoing injury to the brain but rather previously undiagnosed neurologic or mental health conditions.20 Treatment recommendations are a more gradual version of the concussion response, including progressive symptom-limited aerobic exercise and academic modifications. These patients may benefit from referral to a multidisciplinary care team. Frequently suggested prevention interventions are unproven, including neck-strengthening programs and avoiding headers in soccer before a certain age.20,21 More information about concussions can be found in a previous AFP article.26
ACL Injury. One of the most commonly injured ligaments is the anterior cruciate ligament (ACL). The ACL stabilizes the knee by preventing anterior translation of the tibia against the femur and protects against varus and valgus knee forces.15 Females sustain up to eight times more ACL tears compared with males,15–18 most commonly in sports such as soccer and basketball. Female-specific risk factors are reviewed in Table 1 and include smaller ACL size, increased ligamentous laxity, different hip and knee alignment, and increased quadriceps-to-hamstrings activation with landing.8–19
After an ACL tear, athletes typically describe an acceleration and deceleration event associated with a knee valgus moment. Physical examination findings suggestive of an ACL tear include effusion and ACL-specific tests, which are often impractical to perform immediately after injury. If tolerated, the Lachman test is more accurate than the anterior drawer test. Magnetic resonance imaging is diagnostic and can show associated injuries. Following ACL rupture, reconstruction is recommended for younger patients wishing to return to pivoting sports. A previous AFP article provides more information about diagnosis, management, and prevention of ACL injuries.27
Prevention focuses on increased hamstring and core strength and jumping/landing biomechanics.16–19 The Landing Error Scoring System (LESS) can identify athletes at risk of ACL tear.28 Neuromuscular training programs focusing on lower-body strengthening and landing mechanics beginning in preseason and continued throughout the season can reduce the risk of ACL tears by up to 50%.19
RELATIVE ENERGY DEFICIENCY IN SPORT
Any active patient may develop an energy imbalance between caloric intake and expenditure. Appropriate energy availability is crucial for normal growth and athletic development. The female athlete triad was defined in 1984 by the American College of Sports Medicine as a syndrome comprising disordered eating, amenorrhea, and premature osteoporosis.29–31 In 2014, recognizing that low energy availability affects other systems (e.g., neurologic, hematologic, endocrine, gastrointestinal, musculoskeletal), the International Olympic Committee renamed the syndrome relative energy deficiency in sport (RED-S) to address the complex interplay between impaired energy availability and normal physiologic function.29,31 Prolonged states of low energy availability place patients at risk of decreased endurance, muscle and bone strength, concentration and coordination, and fertility; increased injury; delayed healing; impaired judgment; and depression.
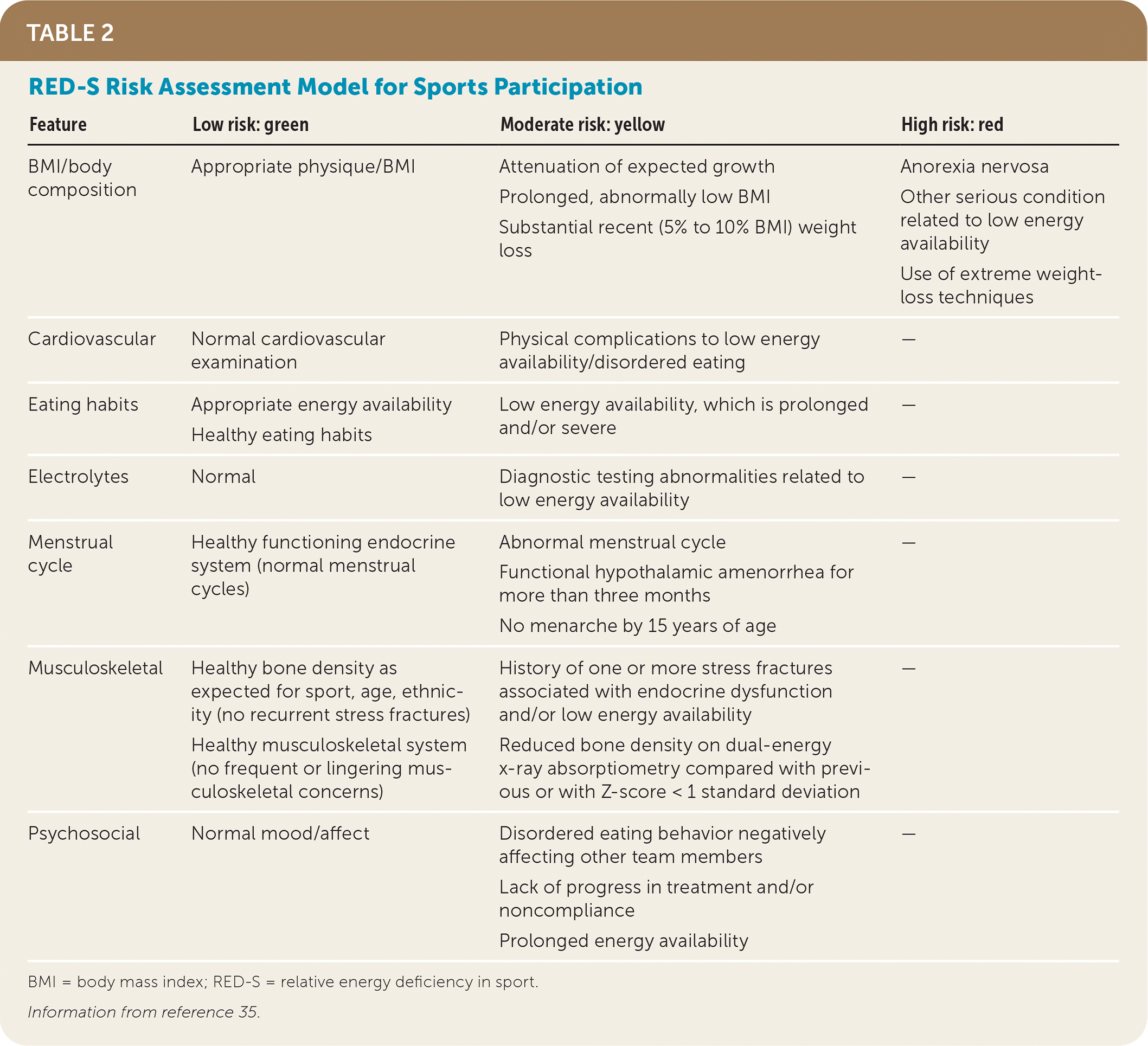
Males also are at risk of RED-S; however, female athletes have higher prevalence.30–34 The preparticipation physical examination provides an opportunity for screening.5 Standardized forms include questions asking whether the patient has ever had a menstrual period and when the patient’s most recent menstrual period occurred. If answers are abnormal, additional screening with questionnaires could be prompted, such as the Low Energy Availability in Females Questionnaire (LEAF-Q), which has been validated in females to identify states of low energy availability.33 Amenorrhea and oligomenorrhea are up to three times more common in athletes compared with nonathletes.34 This finding may trigger screening for RED-S and stress fractures, increased fatigue, recurrent muscle or tendon injuries, low body fat, or worsening athletic performance. The RED-S Risk Assessment Model for Sports Participation groups common findings into low (green), moderate (yellow), and high (red) risk categories (Table 2).35 Athletes in the yellow or red categories require ongoing monitoring and may need a period of sports restriction.35 Conditions such as contraceptive use, iron deficiency, and pregnancy can present similarly to RED-S. Contraceptive use, including oral contraceptives, implantable devices, and injectable forms of contraception, may alter normal menstrual patterns, so routine assessment of contraception use and previous menstrual function as well as associated RED-S symptoms is indicated for all active patients. Functional hypothalamic amenorrhea related to RED-S is a diagnosis of exclusion,30,34 and evaluation for primary or secondary amenorrhea is warranted to consider other causes such as pregnancy, outflow tract abnormalities, or other endocrine disorders.36
TABLE 2. RED-S Risk Assessment Model for Sports Participation
| Feature | Low risk: green | Moderate risk: yellow | High risk: red |
|---|---|---|---|
| BMI/body composition | Appropriate physique/BMI | Attenuation of expected growth Prolonged, abnormally low BMI Substantial recent (5% to 10% BMI) weight loss | Anorexia nervosa Other serious condition related to low energy availability Use of extreme weight-loss techniques |
| Cardiovascular | Normal cardiovascular examination | Physical complications to low energy availability/disordered eating | — |
| Eating habits | Appropriate energy availability Healthy eating habits | Low energy availability, which is prolonged and/or severe | — |
| Electrolytes | Normal | Diagnostic testing abnormalities related to low energy availability | — |
| Menstrual cycle | Healthy functioning endocrine system (normal menstrual cycles) | Abnormal menstrual cycle Functional hypothalamic amenorrhea for more than three months No menarche by 15 years of age | — |
| Musculoskeletal | Healthy bone density as expected for sport, age, ethnicity (no recurrent stress fractures) Healthy musculoskeletal system (no frequent or lingering musculoskeletal concerns) | History of one or more stress fractures associated with endocrine dysfunction and/or low energy availability Reduced bone density on dual-energy x-ray absorptiometry compared with previous or with Z-score < 1 standard deviation | — |
| Psychosocial | Normal mood/affect | Disordered eating behavior negatively affecting other team members Lack of progress in treatment and/or noncompliance Prolonged energy availability | — |
BMI = body mass index; RED-S = relative energy deficiency in sport.
Information from reference 35.
RED-S may or may not include disordered eating. If there is concern for an underlying eating disorder, then including a nutritionist and a psychologist in multidisciplinary care can be helpful. Antidepressants are not indicated unless a comorbid psychiatric medical condition exists.37 Oral contraceptives are also not indicated in the treatment of RED-S because they do not correct the underlying energy imbalance and may provide a false sense of reassurance.
Treatment of RED-S is focused on restoring balance between caloric intake and expenditure through dietary monitoring and modified training activities. Online caloric calculators such as the Dietary Analysis Tool for Athletes may be used to calculate daily calorie needs and appropriate proportions of macronutrients, including fats, proteins, and carbohydrates.38 Caloric intake is individualized based on general activity level, age, and training load.31,35 Athletes with low-risk RED-S features do not require restriction from sport provided they are compliant with treatment and follow-up. Reassessment is recommended at regular intervals of one to three months. The RED-S Clinical Assessment Tool provides guidance for clinicians to clear athletes with RED-S for return-to-play (Table 3).35 Signs and symptoms of restored energy availability include weight gain, resumption of menses, and improved bone health.
TABLE 3. RED-S Return-to-Play Model

| Low risk: green | Full sport participation |
| Moderate risk: yellow | May train provided patient follows treatment plan including: Regular follow-up Adherence to meal plan Adherence to individualized weight gains May compete under supervision once medically cleared |
| High risk: red | No competition or training Adherence to written treatment contract Regular follow-up Adherence to meal plans Adherence to weight gains, minimum body mass index |
RED-S = relative energy deficiency in sport.
Information from reference 35.
Pregnancy and Postpartum
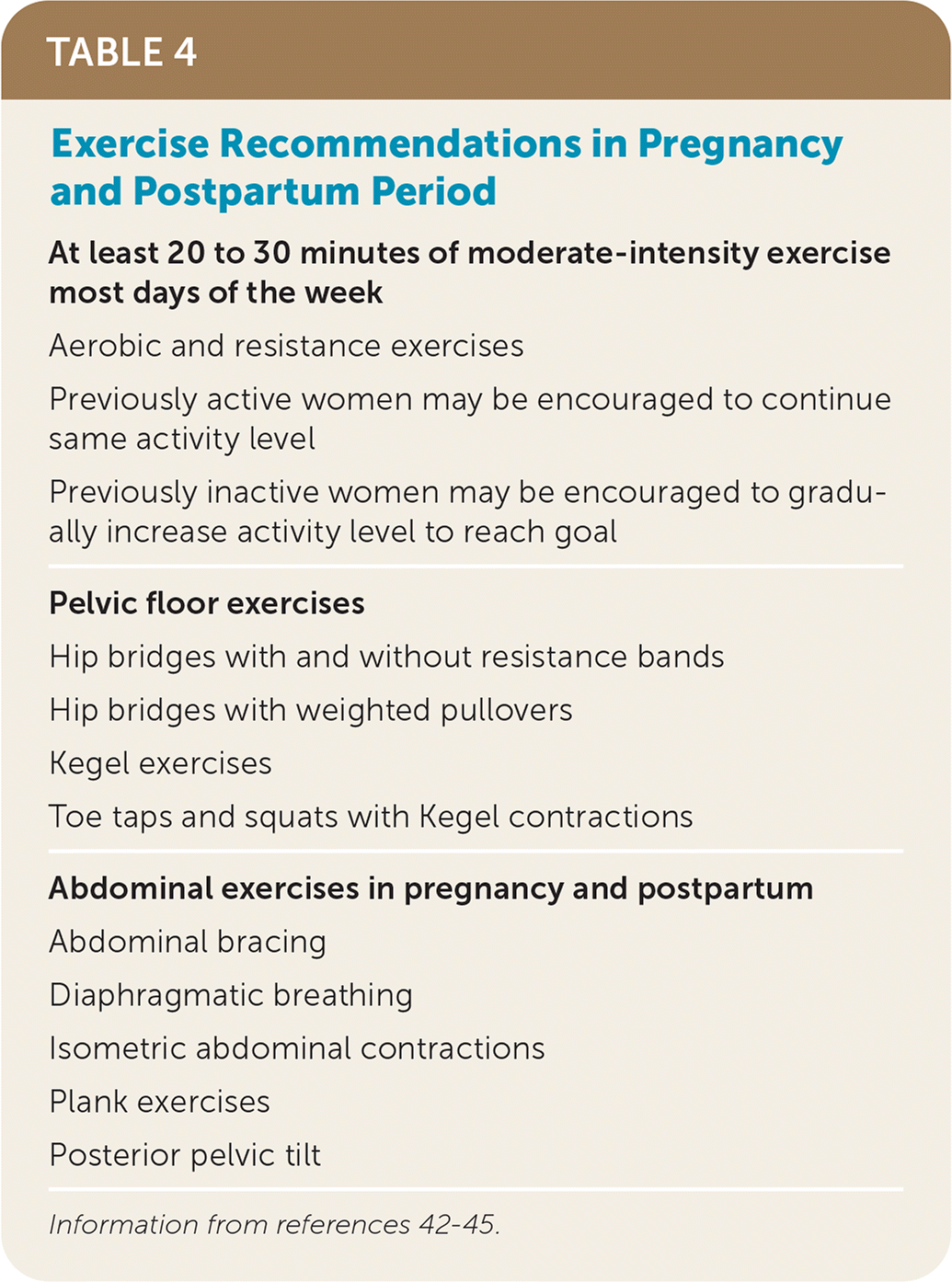
Patients who are pregnant and participate in regular exercise have a decreased risk of gestational diabetes, preeclampsia, cesarean deliveries, and operative vaginal deliveries, as well as improved postpartum recovery time.39–41 Recommendations for physical activity in uncomplicated pregnancy, including twin gestations, are the same as for the general population, comprising 150 minutes of moderate-intensity exercise that includes aerobic activity and strength conditioning. Pregnant patients without contraindications who were previously physically active may continue these activities through pregnancy, and those who were not previously physically active may begin exercise during pregnancy.41 General exercise recommendations for pregnancy and the postpartum period are provided in Table 4.42–45
TABLE 4. Exercise Recommendations in Pregnancy and Postpartum Period
| At least 20 to 30 minutes of moderate-intensity exercise most days of the week |
| Aerobic and resistance exercises |
| Previously active women may be encouraged to continue same activity level |
| Previously inactive women may be encouraged to gradually increase activity level to reach goal |
| Pelvic floor exercises |
| Hip bridges with and without resistance bands |
| Hip bridges with weighted pullovers |
| Kegel exercises |
| Toe taps and squats with Kegel contractions |
| Abdominal exercises in pregnancy and postpartum |
| Abdominal bracing |
| Diaphragmatic breathing |
| Isometric abdominal contractions |
| Plank exercises |
| Posterior pelvic tilt |
Women in the postpartum period may begin gentle exercise when they feel ready and gradually increase intensity. Although abdominal and pelvic floor muscles can take months to fully recover, early pelvic floor therapy and abdominal contraction exercises may reduce the risk of long-term dysfunction.42–44,46,47 All female athletes, regardless of pregnancy status, can participate in regular pelvic floor strengthening and stabilization exercises to reduce the risk of bladder and fecal incontinence. Urinary incontinence is more common in active vs. nonactive females, with the highest rates occurring in those who participate in higher impact sports.43,44 Pregnant athletes who engaged in regular pelvic floor training report reduced rates of incontinence at rest and with exercise.42–44,46,47 Similarly, nonpregnant active females with incontinence who completed pelvic floor therapy report clinically significant improvements in urinary continence. First-line treatment includes Kegel exercises, which can be performed at home. For athletes with persistent symptoms, a referral can be made to a pelvic floor rehabilitation specialist.
Before strenuous exercise, women who are breastfeeding may feed their infant or express breast milk for comfort. Moderate exercise during lactation does not affect the quantity or composition of breast milk or impact infant growth.42
Active Older Adults
Older and postmenopausal women benefit from a training program that involves cardiovascular, strength training, and balance exercises.45,48–50 Weight-bearing and strength training activities help reduce the risk of bone and muscle loss due to decreased estrogen and progesterone levels.45,48–50 Because falls are common in older women and can be catastrophic, history of falls and fall risk should be assessed, as recommended in a previous AFP article.51 A previous fall is the single best predictor of future falls.52
Physical exercise is one of the best studied interventions to reduce the risk of falls and resulting injuries.53–58 Tai chi, which incorporates strength and balance, significantly reduces falls among older adults.53–58 Other beneficial exercise programs include those that emphasize balance training with resistance training and those that integrate balance, strength, and movement.57,58
This article updates a previous article on this topic by Joy, et al.3
Data Sources: A PubMed search was completed in Clinical Queries using the key terms childhood injury, patellofemoral pain syndrome, sex differences in concussions, ACL injuries, Relative Energy Deficiency in Sport, exercise in pregnancy and postpartum, and exercise in postmenopausal women. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. The Cochrane database and ACCESSSS were also searched. Search dates: August 1, 2021, to April 3, 2022.

