Case Scenario
D.H., a 24-year-old patient with opioid use disorder, presents to my clinic for care following minor injuries sustained during an altercation with the police. D.H. spent the weekend in a detention center before being able to post bail. During initial screening for mental health and substance use, D.H. reports symptoms of hypervigilance and increased opioid cravings. What specific clinical or medicolegal issues should I, as the treating family physician, consider or be aware of to optimize the quality of care provided to this patient?
Commentary
Justice system involvement is defined as regular interactions with legal, law enforcement, and carceral systems, including detention, incarceration, or community supervision1; Table 1 outlines common justice system involvement definitions.2 In 2020, the Bureau of Justice Statistics stated that around 21% of U.S. residents (nearly 54 million people) 16 years or older had some type of contact with the police.3 More than 50% of those contacts (more than 25 million) were initiated by the police (i.e., traffic stops, arrests).3 Although the number has been decreasing in the past few years, in 2020 an estimated 5.5 million people were under correctional system control, which includes incarceration and community supervision.3
TABLE 1. Key Definitions of Justice System Involvement Terminology
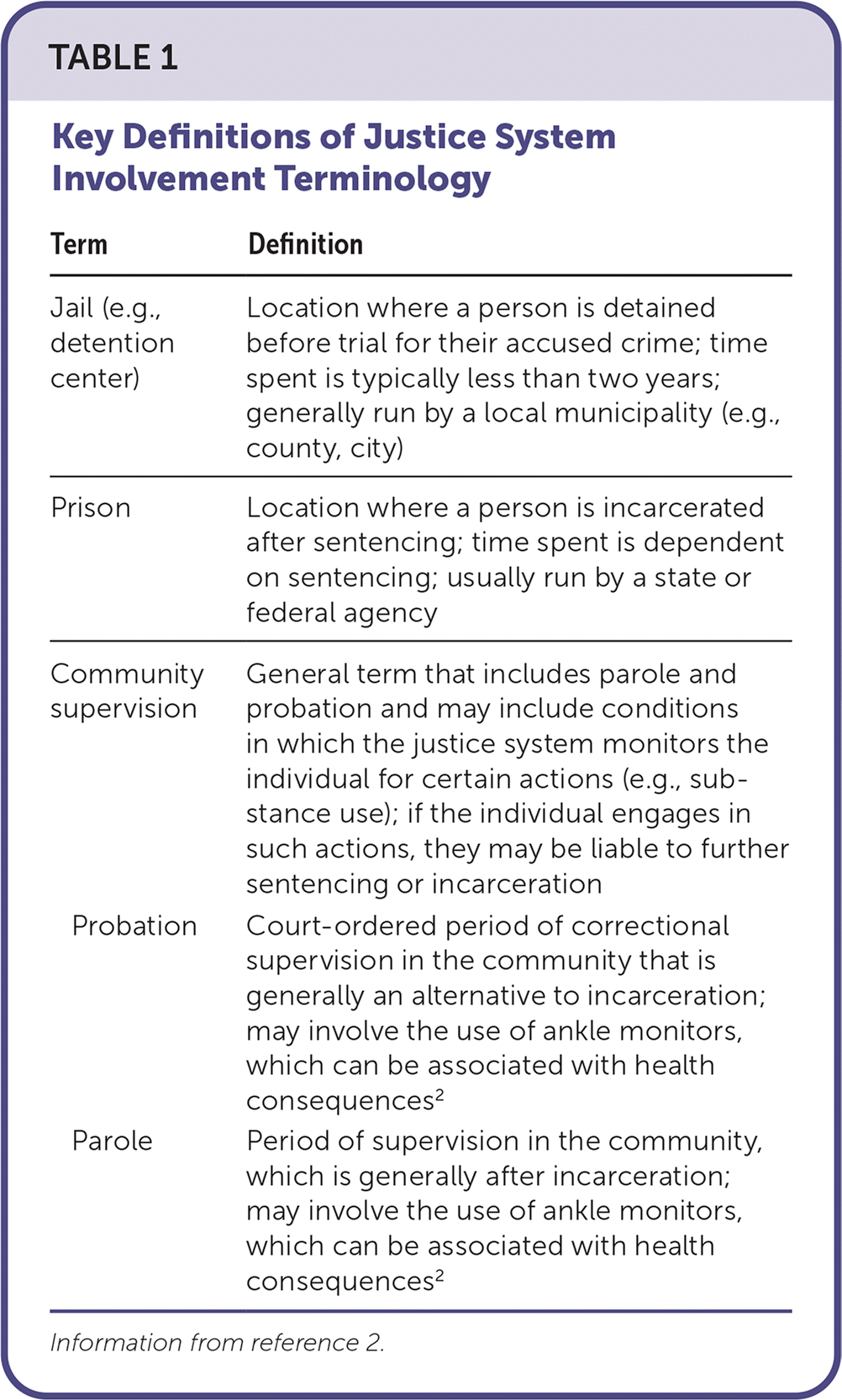
| Term | Definition |
|---|---|
| Jail (e.g., detention center) | Location where a person is detained before trial for their accused crime; time spent is typically less than two years; generally run by a local municipality (e.g., county, city) |
| Prison | Location where a person is incarcerated after sentencing; time spent is dependent on sentencing; usually run by a state or federal agency |
| Community supervision | General term that includes parole and probation and may include conditions in which the justice system monitors the individual for certain actions (e.g., substance use); if the individual engages in such actions, they may be liable to further sentencing or incarceration |
| Probation | Court-ordered period of correctional supervision in the community that is generally an alternative to incarceration; may involve the use of ankle monitors, which can be associated with health consequences2 |
| Parole | Period of supervision in the community, which is generally after incarceration; may involve the use of ankle monitors, which can be associated with health consequences2 |
Information from reference 2.
Profound racial disparities are evident in rates of street stops (e.g., traffic, foot patrol), use of force, arrests, pretrial detention, incarceration, and sentencing.3,4 Overrepresentation of Black and Hispanic individuals in the justice system is a concern, especially given historic and current law enforcement practices, such as overpolicing communities of color.5,6
BUILDING TRUST AND TRAUMA-INFORMED CARE IN CLINICAL ENCOUNTERS WITH PATIENTS WHO HAVE JUSTICE SYSTEM INVOLVEMENT
Patients with justice system involvement face stigmatization in most areas of society, including health care. To minimize bias, family physicians should first identify and address their own personal biases regarding people with justice system involvement, substance use disorders (SUDs), or mental health disorders. Family physicians should be cognizant of the variety of psychosocial challenges that patients with justice system involvement experience7,8 and of their patients' potential mistrust of major institutions, including the medical system.9 Family physicians should engage in trauma-informed care with this population.10 Table 2 provides a list of resources for family physicians to reference when caring for a patient who is involved with the justice system.
TABLE 2. Resources for Family Physicians Treating Patients in the Justice System
| General guidelines | |
| Social drivers of health (e.g., connecting individuals involved in the justice system with key income support, health insurance) | 211 Comprehensive source of information about local resources and services https://www.211.org/ American Academy of Family Physicians The EveryONE Project: assessment and action https://www.aafp.org/family-physician/patient-care/the-everyone-project/toolkit/assessment.html Aunt Bertha Website dedicated to helping people find and connect to social services in their area https://www.auntbertha.com/widget/660x234?c=2F8BC5&d=connectva Leading Into New Communities Language of incarceration https://lincnc.org/language-of-incarceration/ State Policies Connecting Justice-Involved Populations to Medicaid Coverage and Care https://www.kff.org/medicaid/issue-brief/state-policies-connecting-justice-involved-populations-to-medicaid-coverage-and-care/ Substance Abuse and Mental Health Services Administration FAQs for working with people who are involved with the justice system https://soarworks.samhsa.gov/article/faqs-for-working-with-justice-involved-persons |
| Reentry guidance | |
| State and federal resources for system-based approaches to enhance the health of individuals who are reentering the general population | Centers for Disease Control and Prevention Reentry for people who were formerly incarcerated https://www.cdc.gov/correctionalhealth/reentry.html Correctional health resources https://www.cdc.gov/correctionalhealth/resources.html Library of Congress Reentry and employment resources for justice-involved individuals https://guides.loc.gov/reentry-resources Substance Abuse and Mental Health Services Administration Reentry resources for individuals, providers, communities, and states https://www.samhsa.gov/sites/default/files/topics/criminal_juvenile_justice/reentry-resources-for-consumers-providers-communities-states.pdf |
| Sharing of information with law enforcement | |
| Issues of verbal or oral consent to release information, perform justice system–requested examinations, and maintain confidentiality | American Hospital Association Guidelines for releasing patient information to law enforcement https://www.aha.org/standardsguidelines/2018-03-08-guidelines-releasing-patient-information-law-enforcement Council of State Governments Justice Center Information sharing in criminal justice-mental health collaborations: working with HIPAA and other privacy laws https://csgjusticecenter.org/publications/information-sharing-in-criminal-justice-mental-health-collaborations/ Tessier W, Keegan W. Mandatory blood testing: when can police compel a health provider to draw a patient's blood to determine blood levels of alcohol or other intoxicants? Mo Med. 2019; 116(4): 274–277. |
| Special populations | |
| Women, adolescents, LGBTQIA individuals | National Institute of Corrections National Resource Center on Justice-Involved Women https://nicic.gov/sources/national-resource-center-justice-involved-women-nrcjiw-washington-dc Georgetown University Center for Juvenile Justice Reform: publications https://cjjr.georgetown.edu/resources/publications/ Institute for Justice Research and Development Working with justice-involved LGBTQ+ individuals—mutual respect https://ijrd.csw.fsu.edu/training-catalog/working-justice-involved-lgbtq-juveniles-adults-mutual-respect Movement Advancement Project Unjust: LGBTQ Youth Incarcerated in the Juvenile Justice System https://www.lgbtmap.org/policy-and-issue-analysis/criminal-justice-youth-detention Prison Policy Initiative Visualizing the unequal treatment of LGBTQ people in the criminal justice system https://www.prisonpolicy.org/blog/2021/03/02/lgbtq/ |
FAQs = frequently asked questions; HIPAA = Health Insurance Portability and Accountability Act of 1996; LGBTQ = lesbian, gay, bisexual, trans-gender, queer; LGBTQIA = lesbian, gay, bisexual, transgender, queer, intersex, asexual.
HISTORY TAKING AND SCREENING DURING CLINICAL ENCOUNTERS
The population involved in the justice system has an increased prevalence of a variety of health-related conditions compared with the general population.1,11 These conditions include severe mental health disorders (including schizophrenia, bipolar disorder, and posttraumatic stress disorder); SUDs (including alcohol, opioids, and stimulants); and infectious diseases associated with SUDs (e.g., hepatitis C, HIV/AIDS), sexual activity, and congregate settings (e.g., tuberculosis, COVID-19). Other chronic conditions, such as obesity, hypertension, and type 2 diabetes mellitus, are also included.1,11,12 In addition, individuals with justice system involvement are more likely to experience negative social drivers of health, including financial insecurity, housing instability, poverty, and a history of adverse childhood experiences.1,11,12
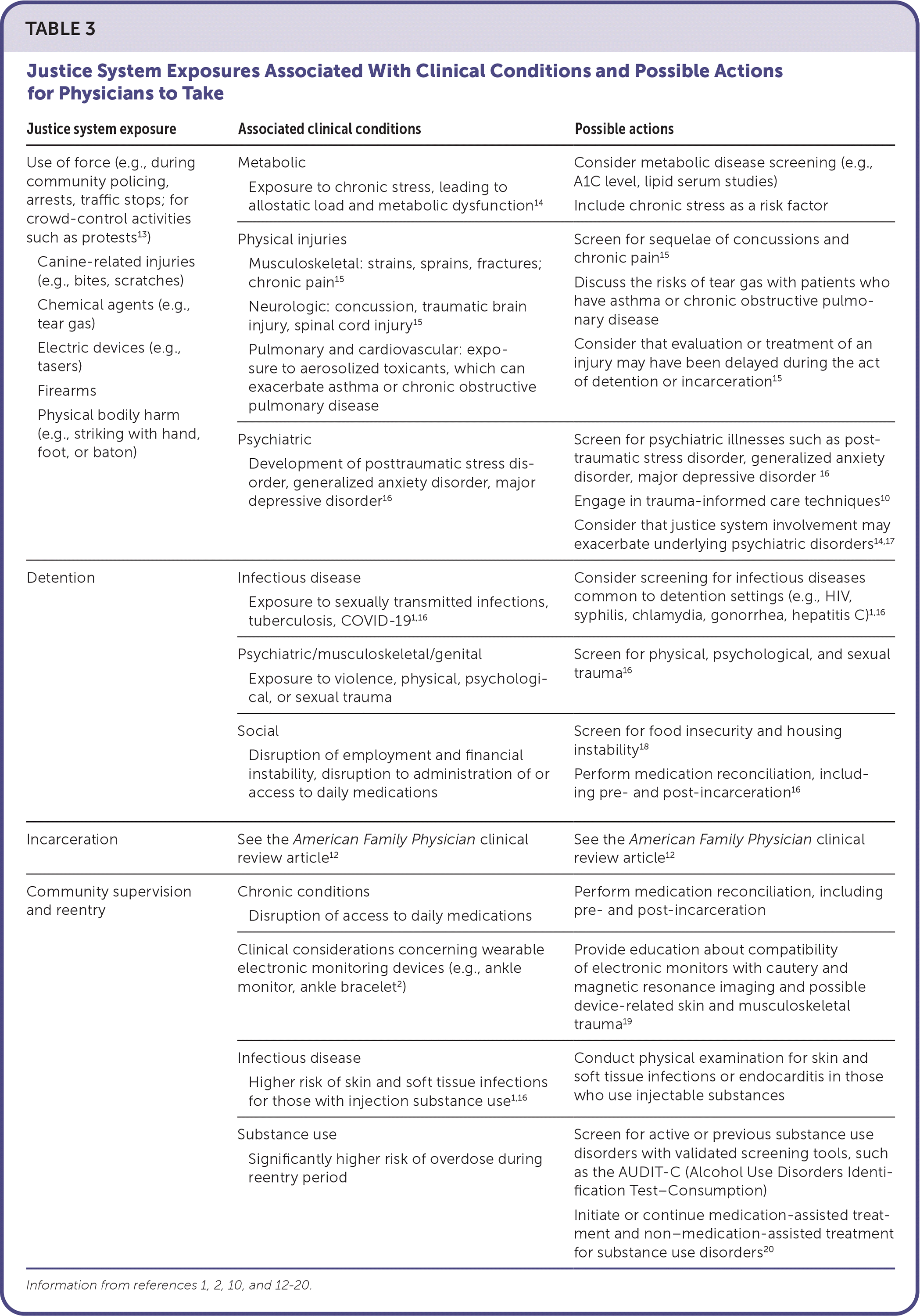
When engaging with patients involved in the justice system, family physicians can focus on exposures related to the four major types of interaction with the justice system: (1) community-based interactions with law enforcement (e.g., during policing activities, crowd-control events during protests, excessive use of force during traffic stops), (2) detention, (3) incarceration, and (4) community reentry, especially if community supervision is required. Table 3 outlines the major conditions associated with exposure type as well as potential actions family physicians might take to address these conditions.1,2,10,12–20
TABLE 3. Justice System Exposures Associated With Clinical Conditions and Possible Actions for Physicians to Take
| Justice system exposure | Associated clinical conditions | Possible actions |
|---|---|---|
| Use of force (e.g., during community policing, arrests, traffic stops; for crowd-control activities such as protests13) Canine-related injuries (e.g., bites, scratches) Chemical agents (e.g., tear gas) Electric devices (e.g., tasers) Firearms Physical bodily harm (e.g., striking with hand, foot, or baton) | Metabolic Exposure to chronic stress, leading to allostatic load and metabolic dysfunction14 | Consider metabolic disease screening (e.g., A1C level, lipid serum studies) Include chronic stress as a risk factor |
| Physical injuries Musculoskeletal: strains, sprains, fractures; chronic pain15 Neurologic: concussion, traumatic brain injury, spinal cord injury15 Pulmonary and cardiovascular: exposure to aerosolized toxicants, which can exacerbate asthma or chronic obstructive pulmonary disease | Screen for sequelae of concussions and chronic pain15 Discuss the risks of tear gas with patients who have asthma or chronic obstructive pulmonary disease Consider that evaluation or treatment of an injury may have been delayed during the act of detention or incarceration15 | |
| Psychiatric Development of posttraumatic stress disorder, generalized anxiety disorder, major depressive disorder16 | Screen for psychiatric illnesses such as posttraumatic stress disorder, generalized anxiety disorder, major depressive disorder 16 Engage in trauma-informed care techniques10 Consider that justice system involvement may exacerbate underlying psychiatric disorders14,17 | |
| Detention | Infectious disease Exposure to sexually transmitted infections, tuberculosis, COVID-191,16 | Consider screening for infectious diseases common to detention settings (e.g., HIV, syphilis, chlamydia, gonorrhea, hepatitis C)1,16 |
| Psychiatric/musculoskeletal/genital Exposure to violence, physical, psychological, or sexual trauma | Screen for physical, psychological, and sexual trauma16 | |
| Social Disruption of employment and financial instability, disruption to administration of or access to daily medications | Screen for food insecurity and housing instability18 Perform medication reconciliation, including pre- and post-incarceration16 | |
| Incarceration | See the American Family Physician clinical review article12 | See the American Family Physician clinical review article12 |
| Community supervision and reentry | Chronic conditions Disruption of access to daily medications | Perform medication reconciliation, including pre- and post-incarceration |
| Clinical considerations concerning wearable electronic monitoring devices (e.g., ankle monitor, ankle bracelet2) | Provide education about compatibility of electronic monitors with cautery and magnetic resonance imaging and possible device-related skin and musculoskeletal trauma19 | |
| Infectious disease Higher risk of skin and soft tissue infections for those with injection substance use1,16 | Conduct physical examination for skin and soft tissue infections or endocarditis in those who use injectable substances | |
| Substance use Significantly higher risk of overdose during reentry period | Screen for active or previous substance use disorders with validated screening tools, such as the AUDIT-C (Alcohol Use Disorders Identification Test–Consumption) Initiate or continue medication-assisted treatment and non–medication-assisted treatment for substance use disorders20 |
If a patient indicates recent law enforcement interaction, family physicians should inquire about musculoskeletal trauma, exposure to crowd-control agents (e.g., toxins known as tear gas, rubber bullets), and symptoms of anxiety or posttraumatic stress disorder.14,17,21,22 Repeated interactions with police can lead to chronic stress, which has been linked with increased allostatic load and metabolic disease.14,17,21
Individuals who have been detained might have been exposed to physical, psychological, and sexual trauma as well as infectious diseases, including sexually transmitted infections (e.g., HIV, hepatitis C), COVID-19, and tuberculosis.11,12 Family physicians should consider laboratory and mental health screening based on an individual's risk. Detention causes multiple social interruptions, such as discontinuation of employment, housing, telephone services, and health insurance. If equipped to address, physicians should use validated social screening tools and referrals to assist the patient's life needs, which can include access to medications, specialists, safe housing, and healthy food.18 A previous article published by American Family Physician outlines the adverse effects of incarceration or detention.12
Reentry and community supervision are particularly dangerous periods for patients because of an array of possible adverse events, including drug overdose; suicidal ideation, attempts, and completion; interruption of mental and physical health care; and medication discontinuation.23
Assessment should include the effect of justice system involvement as it extends to families and communities. Interaction with the justice system is associated with lower household income, higher rates of prenatal complications and childhood developmental behavioral and cognitive conditions, and increased rates of adult chronic medical conditions, such as cardiovascular disease, depression, and anxiety.24
DOCUMENTATION
Individuals involved with the justice system may experience judicial subpoenas, warrants, or summons in connection with legal proceedings, potentially requiring access to medical records. Family physicians must carefully consider what information is documented in the health record. For routine medical care, family physicians can document any subjective information that is pertinent to the medical condition and objective findings on clinical examination.25 They should avoid documenting subjective information that is superfluous and not related to patient care, regardless of its relation to a legal incident, unless the history taking is part of a medicolegal encounter.25 Exceptions include mandatory reporting situations (which can vary by state or municipality) such as child or elder abuse.26–28
MEDICOLEGAL INTERACTION AND SUPPORT
A family physician may interact with the justice and legal systems regarding a patient in several situations besides direct provision of clinical care. A common scenario is legal or law enforcement–requested patient health information. Several federal regulations are available that can guide family physicians in issues regarding confidentiality. The Health Insurance Portability and Accountability Act of 1996 (HIPAA) and Title 42 of the Code of Federal Regulations, Part 2, which protects the records of those with SUDs, dictate that in most circumstances law enforcement or legal inquiries require patient consent for record release unless court ordered and presented with a legal document.25,29–31 Laws vary by state, and seeking institutional legal counsel is advisable to ascertain legal duty as a physician.
Patients may request a letter of support from their family physician for legal processes, such as probation or further sentencing. When drafting a letter of support, a family physician could include objective information regarding the patient, their care, and any important clinical scenarios.31 For example, a family physician could include that the patient attended all their clinic visits for SUD, the dates of those visits, and other pertinent information such as reported remission, negative metabolite screen, or improved anxiety scores on screening. Family physicians should avoid passing moral judgment, adding superfluous information, or recommending legal outcomes.25,29–31
Case Resolution
In the case presented here, the family physician should clearly and concisely inquire about D.H.'s justice system involvement, including their police encounter and detention. The physician should assess the patient's injuries and provide follow-up care as needed. If possible, D.H. should begin taking buprenorphine and be prescribed naloxone, given their high risk of overdose.
The physician should address their fiduciary role and legal and ethical responsibilities to act in the patient's interest.
The physician should strongly encourage and facilitate follow-up with counseling, case management and/or social work support and care for SUD, and primary care.
If equipped to address, the physician should use validated social screening tools and referrals to assist the patient's life needs and other social drivers of health (Table 2).

