Peripartum depression is one of the most common disorders of pregnancy. It has a higher morbidity and mortality risk than any other condition affecting pregnant people. The American Academy of Family Physicians, the American College of Obstetricians and Gynecologists, the American Academy of Pediatrics, and the U.S. Preventive Services Task Force recommend that pregnant patients be screened for depression with one of several validated tools and offered treatment with psychotherapy and medication. There are no validated tools available to identify who is at increased risk of peripartum depression. Risk factors for peripartum depression include a history of depression, a history of physical or sexual abuse, carrying an unplanned or unwanted pregnancy, and traumatic birth. The U.S. Preventive Services Task Force recommends offering psychotherapy to patients at increased risk of depression because it can decrease the development of peripartum depression by up to 39%. Untreated peripartum depression increases the risk of adverse pregnancy outcomes and mortality for the patient, as well as negative outcomes for the newborn, including growth faltering, developmental delay, and attachment disorder. Cognitive behavior therapy and interpersonal psychotherapy are the mainstay of treatment for peripartum depression; physicians should consider selective serotonin reuptake inhibitors for those with moderate to severe depression. The benefits of selective serotonin reuptake inhibitors generally outweigh the risks; however, fluoxetine and paroxetine should be avoided during pregnancy because they can cause an increased risk of birth defects.
Peripartum depression refers to depression experienced during pregnancy or in the 12 months following childbirth; it affects up to 1 in 7 pregnant patients.1 Symptoms of peripartum depression persist for more than two weeks and include anhedonia, decreased energy, reduced appetite, and poor concentration. Peripartum depression is one of the most common disorders of pregnancy, and mortality from mental health conditions is higher than mortality from any other condition in the peripartum period, accounting for 22.7% of pregnancy-related deaths from 2017 through 2019.2 Peripartum depression can also have negative impacts on the child, including growth faltering, developmental delay, and attachment disorder.3 The etiology of peripartum depression is not known.
WHAT'S NEW ON THIS TOPIC

| Mental health conditions accounted for 22.7% of pregnancy-related deaths from 2017 through 2019, a higher mortality than that from any other condition in the peripartum period. |
| A systematic review showed no consistent changes in thyroid-stimulating hormone, prolactin, or cortisol levels in patients with peripartum depression. |
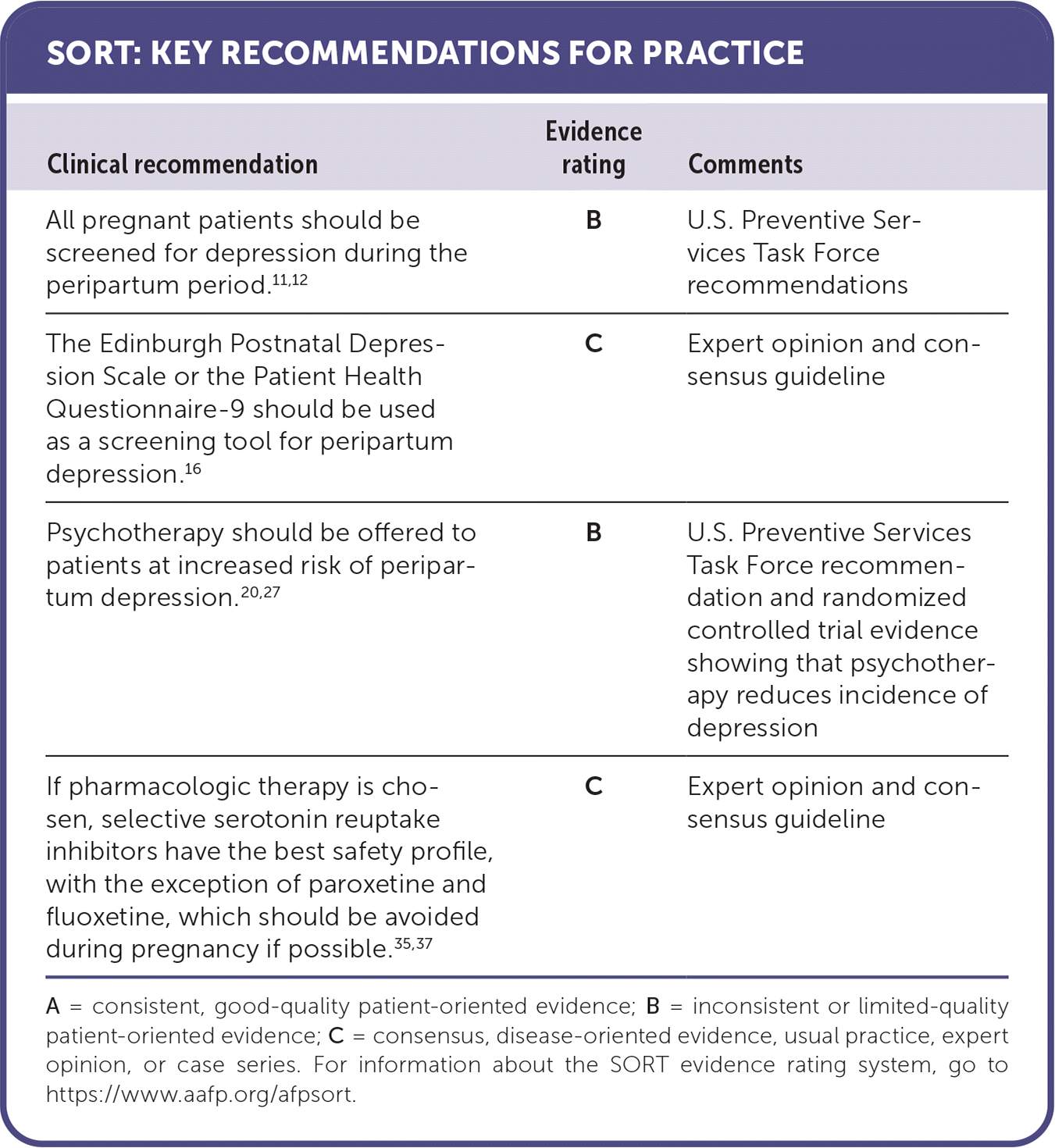
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | Comments |
|---|---|---|
| All pregnant patients should be screened for depression during the peripartum period.11,12 | B | U.S. Preventive Services Task Force recommendations |
| The Edinburgh Postnatal Depression Scale or the Patient Health Questionnaire-9 should be used as a screening tool for peripartum depression.16 | C | Expert opinion and consensus guideline |
| Psychotherapy should be offered to patients at increased risk of peripartum depression.20,27 | B | U.S. Preventive Services Task Force recommendation and randomized controlled trial evidence showing that psychotherapy reduces incidence of depression |
| If pharmacologic therapy is chosen, selective serotonin reuptake inhibitors have the best safety profile, with the exception of paroxetine and fluoxetine, which should be avoided during pregnancy if possible.35,37 | C | Expert opinion and consensus guideline |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Incidence and Prevalence
In different studies, rates of peripartum depression ranged from 12.4% to 14.3%.1,4 During the COVID-19 pandemic, one study noted a depression rate that was more than twice as high in people who were pregnant during the pandemic compared with those whose pregnancy occurred before the pandemic, with 40% of all patients experiencing symptoms of depression during the pandemic.5 Recurrence rates are as high as 25% if a patient had depression with a previous pregnancy and 56% if depression occurred in two past pregnancies.6 Peak point prevalence of peripartum depression is at three months postpartum.1
Risk Factors
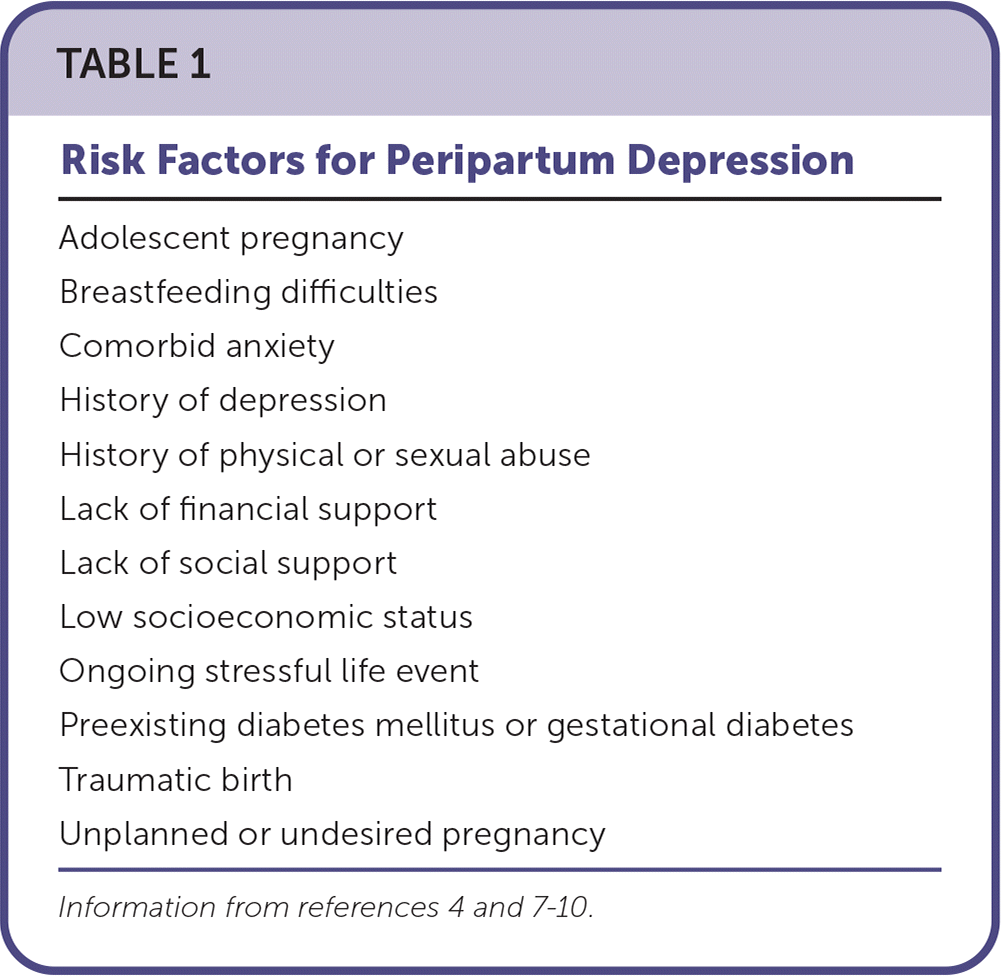
There are many risk factors for peripartum depression (Table 1).4,7–10 Notably, patients with a history of depression outside of the peripartum period have a twofold risk of recurrence during pregnancy.4
TABLE 1. Risk Factors for Peripartum Depression
| Adolescent pregnancy |
| Breastfeeding difficulties |
| Comorbid anxiety |
| History of depression |
| History of physical or sexual abuse |
| Lack of financial support |
| Lack of social support |
| Low socioeconomic status |
| Ongoing stressful life event |
| Preexisting diabetes mellitus or gestational diabetes |
| Traumatic birth |
| Unplanned or undesired pregnancy |
Screening, Evaluation, and Diagnosis
Family physicians have the opportunity to screen patients during prenatal, postpartum, and infant clinic visits. The U.S. Preventive Services Task Force recommends depression screening for adults, including those who are pregnant or in the postpartum period.11,12 The American College of Obstetricians and Gynecologists recommends screening for depression at least once during the peripartum period and again postpartum if the initial screening took place during pregnancy.13
Family physicians often provide care to the birthing parent and child after delivery. The American Academy of Pediatrics recommends screening the birthing parent for depression at the one-, two-, four-, and six-month well-child visits.14 In 2016, the Centers for Medicare and Medicaid Services directed state Medicaid agencies to allow billing for depression screening of the birthing parent at well-child visits.15
Several validated screening tools are available. The most widely used are the Edinburgh Postnatal Depression Scale (EPDS) and the Patient Health Questionnaire-9 (PHQ-9); both are recommended by the U.S. Preventive Services Task Force, American College of Obstetricians and Gynecologists, American Academy of Family Physicians, and American Academy of Pediatrics to screen patients for peripartum depression. These tools take less than five minutes to complete and have no more than 10 questions each. The PHQ-9 includes questions about constitutional symptoms, such as fatigue and change in appetite, that are common in postpartum patients without depression, so the specificity of this test may be lower than that of the EPDS. Table 2 provides resources for each tool.16
The diagnosis of peripartum depression can be made using the Diagnostic and Statistical Manual of Mental Disorders, 5th ed. (DSM-5).17 The DSM-5 criteria require the onset of depression to occur within the first four weeks after delivery; however, most experts in the field define peripartum depression as having an onset anytime during pregnancy or up to 12 months postpartum.18 Peripartum depression must be differentiated from the baby blues. Although the baby blues typically occur within two to three days of delivery and recede by 10 days postpartum, peripartum depression lasts for more than two weeks.
When peripartum depression is identified, further evaluation should occur. The patient should be screened for suicidal ideation, particularly if the screening tool reveals thoughts of self-harm. Questions such as “Have you ever tried to hurt yourself?” and “Do you have a plan for how you would hurt yourself?” as well as “Have you ever wished you could go to sleep and not wake up?” can be useful in these situations.16 Homicidal ideation, including asking whether the patient has had thoughts of harming their child or others, should be evaluated as well. Screening for anxiety should also be considered, given its high comorbidity rate with depression.
Evidence of mania should be elicited in patients identified to have peripartum depression. The Mood Disorder Questionnaire (https://www.mdapp.co/mood-disorder-questionnaire-mdq-calculator-208/) can be used to elicit further information.
Laboratory tests are not routinely recommended. A systematic review showed no consistent correlation between a change in thyroid-stimulating hormone, prolactin, or cortisol levels and having peripartum depression.19 Thyroid studies may be indicated if other symptoms such as constipation, dry skin, and bradycardia are present. Anemia can lead to fatigue, which may be mistaken for depression; therefore, obtaining a hemoglobin level may be considered.
Prevention
The U.S. Preventive Services Task Force recommends referral for cognitive behavior therapy (i.e., talk therapy that focuses on one's negative thinking and explores ways to change it) and interpersonal psychotherapy (i.e., talk therapy that focuses on interpersonal functioning) for all pregnant people at increased risk of perinatal depression.20 Psychotherapy is the most widely studied intervention, with a reduction of up to 39% in the risk of development of peripartum depression.20 A validated screening tool is not available to assess risk, although a variety of risk factors have been identified that should prompt screening and early referral (Table 1).4,7–10
Psychosocial interventions have shown some promising results in a meta-analysis that included 28 trials and involved almost 17,000 participants.21 Intensive and individualized home visits with nurses or midwives, peer-based telephone support, and interpersonal psychotherapy all decrease rates of peripartum depression.21 Both professional support and peer-based support are effective.21 Physical activity may have a small protective effect, particularly when participants are engaged in structured or supervised activities.22
Identification of people who have experienced birth trauma may be an important factor in prevention. A randomized controlled trial with 103 participants found that for those who perceived the birthing experience as traumatic, a brief intervention within 72 hours and at four to six weeks postpartum resulted in a statistically significant decrease in posttraumatic and depressive symptoms.23 In this trial, a traumatic birth was considered one in which the birthing parent feared for their life or the life of their newborn or worried about serious damage to themself or their newborn. Small studies have investigated the use of prophylactic antidepressants such as amitriptyline or sertraline in the postpartum period, although only low-quality evidence supports thispractice, and an increased rate of adverse effects has been observed.24 There is insufficient evidence to support the prophylactic use of hypnosis and omega fatty acid supplementation.25,26
Treatment of Peripartum Depression
NONPHARMACOLOGIC
Nonpharmacologic treatment strategies are similar to prevention strategies, with the U.S. Preventive Services Task Force recommending referral for psychotherapy as the mainstay of treatment.27 Cognitive behavior therapy and interpersonal psychotherapy are the best studied and have the most robust supporting evidence.27 Group and individual approaches are effective.21,27
A systematic review of nine trials that included 956 women found that psychosocial or psychological intervention of any type improved depressive symptoms at one year postpartum.28 Patients with clinically diagnosed depression and those with self-reported symptoms received benefits.28
Interventions such as physical activity through group exercise or participant-chosen exercise may have a modest effect, although high-quality evidence is lacking.29 There is low-quality evidence for the use of supplements such as omega fatty acids, vitamin D, folate, and St. John's wort to treat peripartum depression; more robust studies are needed.30,31
PHARMACOLOGIC
Although psychotherapy is the mainstay of treatment, selective serotonin reuptake inhibitors (SSRIs) may be considered in those with moderate to severe peripartum depression.32 Risks of medication use during pregnancy and breastfeeding must be weighed against the risks of untreated or inadequately treated depression. Inadequately treated depression has the potential to progress to active suicidality and can lead to impaired bonding for the birth parent, impaired childhood development, and adverse pregnancy outcomes, including preterm birth, low birth weight, and hypertensive disorders.33 However, SSRI use during pregnancy has also been associated with an increased risk of poor outcomes. A Danish study found that pregnant patients taking SSRIs had an increased risk of preterm delivery (8.8%) vs. those with a psychiatric history who were not taking SSRIs (5% rate of preterm delivery), an increased risk of infant admission to the neonatal intensive care unit (16.4% vs. 9%), and an increased risk of the newborn having an Apgar score less than 8 (4.9% vs. 1%).34 Although most SSRIs have not been linked to birth defects, paroxetine and fluoxetine have been associated with an increased risk and should be avoided during pregnancy.35 Five specific birth defects that have been related to paroxetine therapy include anencephaly (odds ratio [OR] = 3.2), atrial septal defects (OR = 1.8), right ventricular outflow tract obstruction defects (OR = 2.4), gastroschisis (OR = 2.5), and omphalocele (OR = 3.5). Fluoxetine has been associated with right ventricular outflow tract obstruction defects (OR = 2.0) and craniosynostosis (OR = 1.9).35 Another large study found that paroxetine is the only SSRI linked to birth defects; it can cause a small increased risk of cardiac defects if exposure occurs in the first trimester.36 Sertraline, citalopram, and escitalopram have not been linked to birth defects.35
For patients taking SSRIs at the time of conception, it is generally recommended to continue the medication unless the risk of fetal harm outweighs the benefit of the medication.33,35,37 There is no clear recommendation on whether a person should stop taking fluoxetine or paroxetine if they become pregnant; this scenario should be addressed on an individual basis using shared decision-making. Most studies involving pharmacologic treatment of peripartum depression included SSRIs. There is insufficient evidence comparing SSRIs with other classes of antidepressants and insufficient evidence of effectiveness, safety, and acceptability of antidepressant classes other than SSRIs.32 Hormone therapies containing estrogen and progesterone are not recommended routinely for peripartum depression.38
BREASTFEEDING CONSIDERATIONS
The American College of Obstetricians and Gynecologists and the American Academy of Pediatrics have addressed safety considerations regarding medication concentrations in breast milk. Table 3 compares safety profiles.16 Parents should be instructed to monitor infants for signs of anti-depressant toxicity, including feeding difficulty, irritability, or lethargy if the breastfeeding parent is taking an antidepressant.
EMERGENCY TREATMENT
If a patient is actively suicidal or psychosis is identified, they should be referred for immediate psychiatric evaluation and treatment.
This article updates previous articles on this topic by Langan and Goodbred,16 Hirst and Moutier,39 and Epperson.40
Data Sources: A PubMed search was performed using the key words peripartum depression, postpartum depression, screening, prevention, and treatment. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. The Cochrane database and the Essential Evidence Plus, U.S. Preventive Services Task Force, American Academy of Pediatrics, and Centers for Disease Control and Prevention websites were also searched. Search dates: October 6, 2022; December 3 and 5, 2022; and July 30, 2023.

