Hypertension is a leading modifiable risk factor for cardiovascular disease and the most common chronic condition seen by family physicians. Treatment of hypertension reduces morbidity and mortality due to coronary artery disease, myocardial infarction, heart failure, stroke, and chronic kidney disease. The use of ambulatory and home blood pressure monitoring improves diagnostic accuracy. Assessment of adults with hypertension should focus on identifying complications of the condition and comorbid cardiovascular risk factors. Physicians should counsel all patients with elevated blood pressure about effective lifestyle interventions, including the Dietary Approaches to Stop Hypertension (DASH) diet, dietary sodium restriction, potassium enrichment, regular exercise, weight loss, and moderation of alcohol consumption. First-line antihypertensive medications include angiotensin-converting enzyme inhibitors, angiotensin receptor blockers, calcium channel blockers, and thiazide diuretics. Thresholds for pharmacologic intervention and blood pressure goals differ according to various guidelines. Evidence strongly supports reducing blood pressure to less than 140/90 mm Hg to reduce the risk of all-cause and cardiovascular mortality in adults with hypertension. Lowering blood pressure to less than 135/85 mm Hg may further reduce the risk of myocardial infarction. Clinical judgment and shared decision-making should guide treatment of patients with mild hypertension and older adults who may be more susceptible to adverse effects of antihypertensive medications and tight blood pressure control.
Hypertension is the persistent elevation of systolic and/or diastolic blood pressure and a leading modifiable risk factor for cardiovascular disease; it is the most common chronic condition seen by family physicians. Cardiovascular and cerebrovascular risk each increase linearly with blood pressure higher than 110/75 mm Hg, and risk accumulates with the addition of other cardiovascular risk factors. Treatment of hypertension reduces morbidity and mortality due to coronary artery disease, myocardial infarction, heart failure, stroke, and chronic kidney disease.1–4
SORT: KEY RECOMMENDATIONS FOR PRACTICE
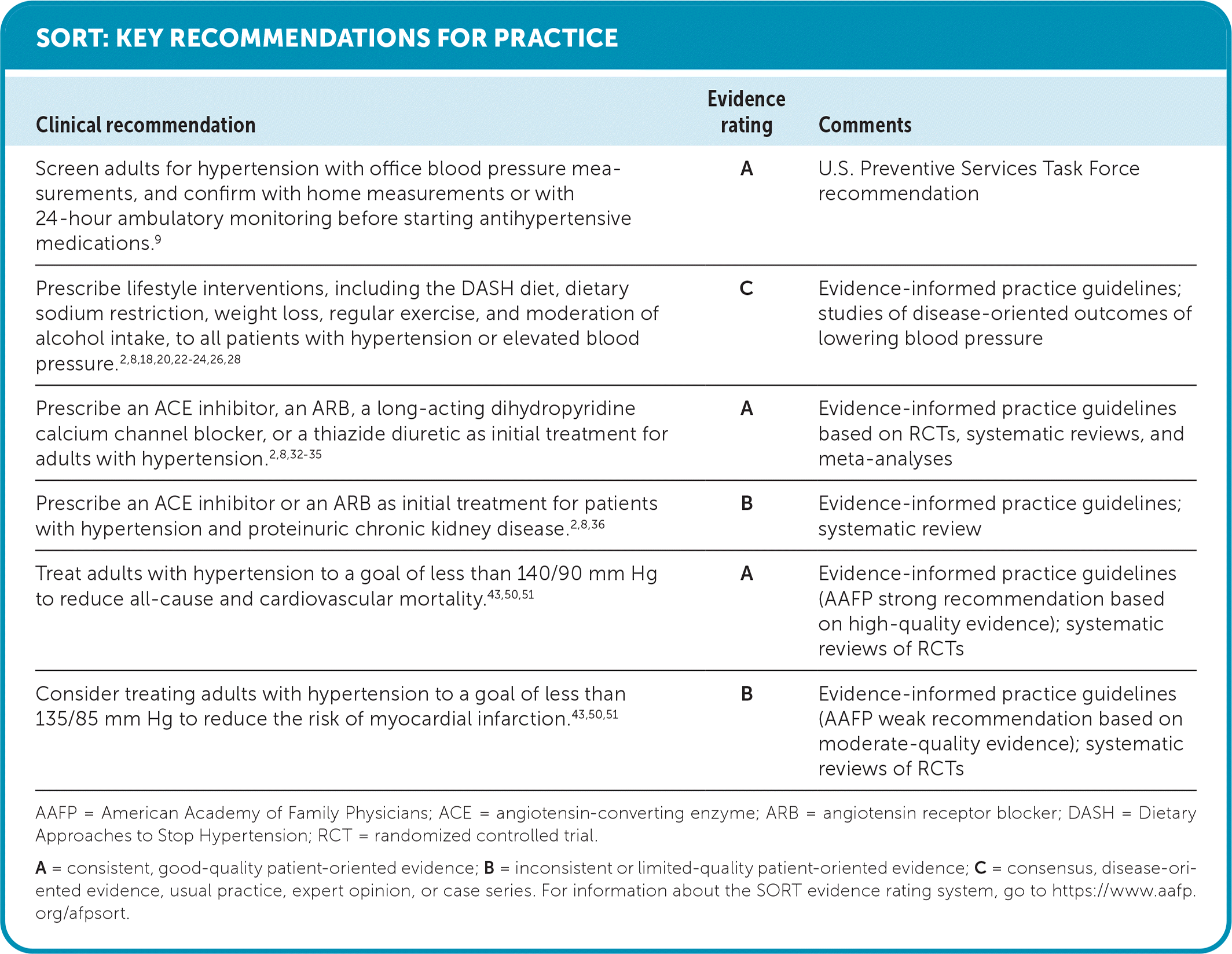
AAFP = American Academy of Family Physicians; ACE = angiotensin-converting enzyme; ARB = angiotensin receptor blocker; DASH = Dietary Approaches to Stop Hypertension; RCT = randomized controlled trial.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
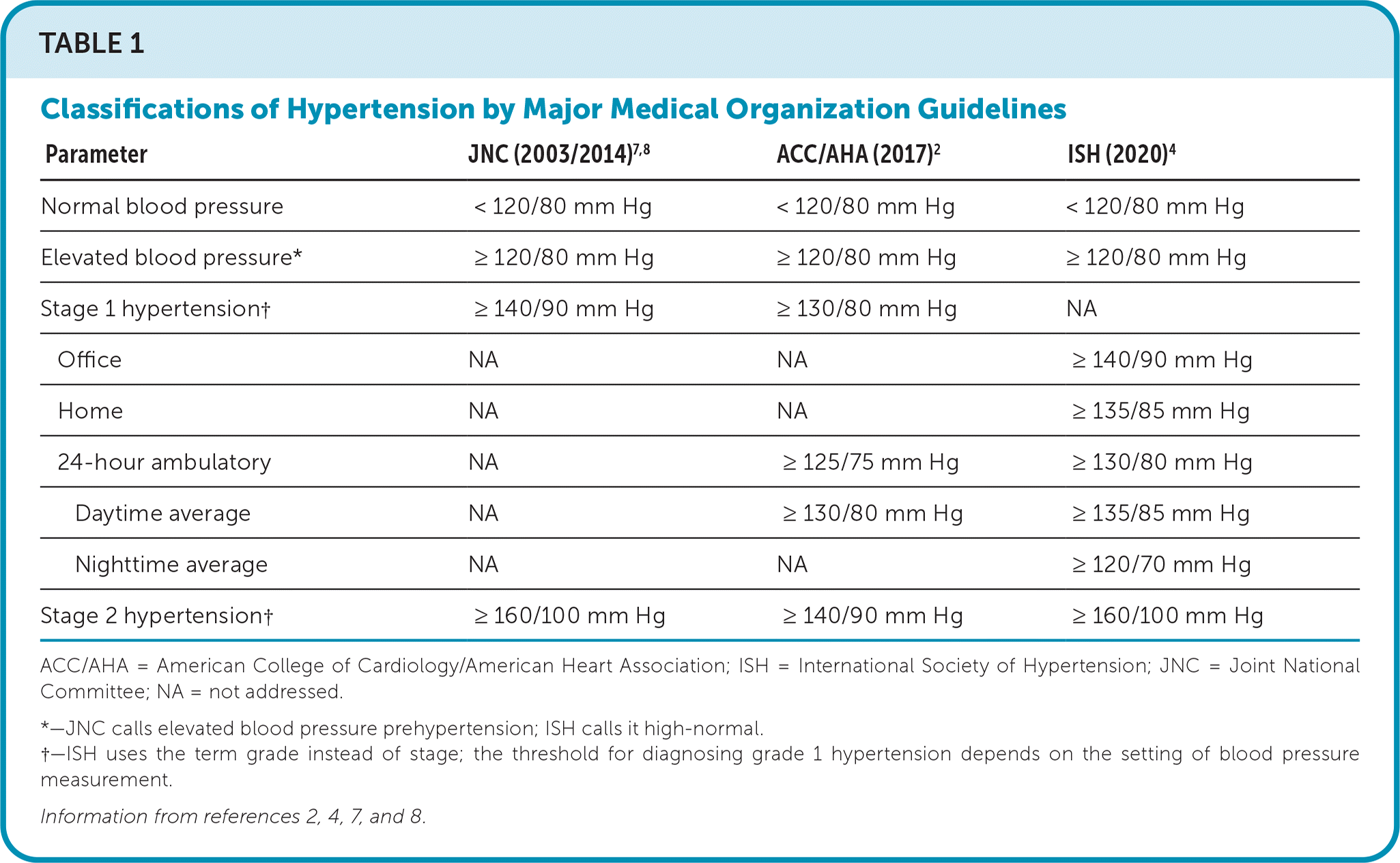
Depending on the threshold used for diagnosis, hypertension affects 32% to 46% of U.S. adults, and prevalence increases with age.2 Black individuals are affected at least 30% more than White individuals; this racial disparity is greatest among women, according to data from the National Health and Nutrition Examination Survey.5 Reasons for these disparities are not completely understood, but access to care and social determinants of health play a significant role.6 Classifications of hypertension according to recent guidelines are shown in Table 1.2,4,7,8
TABLE 1. Classifications of Hypertension by Major Medical Organization Guidelines
| Parameter | JNC (2003/2014)7,8 | ACC/AHA (2017)2 | ISH (2020)4 |
|---|---|---|---|
| Normal blood pressure | < 120/80 mm Hg | < 120/80 mm Hg | < 120/80 mm Hg |
| Elevated blood pressure* | ≥ 120/80 mm Hg | ≥ 120/80 mm Hg | ≥ 120/80 mm Hg |
| Stage 1 hypertension† | ≥ 140/90 mm Hg | ≥ 130/80 mm Hg | NA |
| Office | NA | NA | ≥ 140/90 mm Hg |
| Home | NA | NA | ≥ 135/85 mm Hg |
| 24-hour ambulatory | NA | ≥ 125/75 mm Hg | ≥ 130/80 mm Hg |
| Daytime average | NA | ≥ 130/80 mm Hg | ≥ 135/85 mm Hg |
| Nighttime average | NA | NA | ≥ 120/70 mm Hg |
| Stage 2 hypertension† | ≥ 160/100 mm Hg | ≥ 140/90 mm Hg | ≥ 160/100 mm Hg |
ACC/AHA = American College of Cardiology/American Heart Association; ISH = International Society of Hypertension; JNC = Joint National Committee; NA = not addressed.
*—JNC calls elevated blood pressure prehypertension; ISH calls it high-normal.
†—ISH uses the term grade instead of stage; the threshold for diagnosing grade 1 hypertension depends on the setting of blood pressure measurement.
Screening and Diagnosis
The U.S. Preventive Services Task Force recommends screening for hypertension in adults 18 years or older with office blood pressure measurement (grade A recommendation).9 Blood pressure should be measured using a calibrated auscultatory or oscillometric device. The cuff bladder should encircle 80% of the patient’s arm because cuffs that are too small will overestimate blood pressure.2,10 An AFP Community Blog post discusses the importance of accurate cuff size (https://www.aafp.org/pubs/afp/afp-community-blog/entry/for-accurate-blood-pressure-measurement-cuff-size-matters.html). Patients should rest quietly for five minutes in a chair, with their feet on the floor and their arm supported at heart level. At least two or three measurements should be taken at one- to two-minute intervals.2,3,10
For accurate diagnosis, blood pressure should be averaged over three or more separate visits, unless blood pressure exceeds 180/110 mm Hg or 160/100 mm Hg with evidence of end-organ damage.2–4 Office blood pressure measurements should be confirmed with home or 24-hour ambulatory measurements when possible.9,11 Typically, these will be 5 to 10 mm Hg lower than office measurements. Moreover, up to 20% of patients with high blood pressure in the clinic have normal ambulatory pressure or white coat hypertension.2,3
Evaluation
Assessment should focus on identifying complications of hypertension and comorbid cardiovascular risk factors.4 History should include a personal and family history of hypertension, cardiovascular disease, and related disorders, such as diabetes mellitus and hyperlipidemia. Prior treatment, medications, and lifestyle habits (e.g., diet; salt intake; exercise; sleep; use of alcohol, tobacco, and stimulants) should be noted.
The physical examination and review of systems should identify pertinent signs and symptoms of cardiac, pulmonary, neurologic, visual, renal, and peripheral vascular dysfunction. Common secondary causes of hypertension should be considered, such as obstructive sleep apnea, primary aldosteronism, renovascular disease, renal parenchymal disease, and alcohol and illicit drug use, especially in patients younger than 30 years and those with markedly elevated blood pressure.2,12
Recommended laboratory and other diagnostic tests are listed in Table 2.2,7,13 Patients 20 to 79 years of age without arteriosclerotic cardiovascular disease (ASCVD) can be risk stratified using the ASCVD Risk Estimator (https://tools.acc.org/ldl/ascvd_risk_estimator/index.html)14 or ASCVD Risk Estimator Plus (https://tools.acc.org/ascvd-risk-estimator-plus/).2,15 These tools have been shown to significantly overestimate risk in patients with predicted risk greater than 10%, higher socioeconomic status, or greater utilization of preventive care services. The tools underestimate risk in patients from certain racial or ethnic groups and in those with lower socioeconomic status or chronic inflammatory disease.16,17 Nevertheless, they may serve as a useful starting point for clinical and shared decision-making about antihypertensive treatment goals and intensity.
Lifestyle Modifications
Physicians should counsel all patients with elevated blood pressure or hypertension about effective lifestyle interventions, including the Dietary Approaches to Stop Hypertension (DASH) diet, dietary sodium restriction, dietary potassium enrichment, weight loss, regular exercise, and moderation of alcohol intake.2,8,18 The original DASH trial showed that a diet rich in fruits, vegetables, and low-fat dairy and with reduced saturated and total fat substantially lowers blood pressure in adults.19 Dietary sodium restriction to 1,500 mg or less per day or reduction by at least 1,000 mg from usual daily intake lowers blood pressure independently.18 Blood pressure reductions are greatest when dietary sodium intake is lowered to 1,200 mg per day and when sodium restriction is combined with the DASH diet.20 The benefit of sodium restriction is further supported by evidence showing that potassium-based salt substitutes lower blood pressure and reduce cardiovascular and all-cause mortality.21 The benefits of dietary potassium enrichment must be balanced with the risk of hyperkalemia in patients with chronic kidney disease or taking medications that impair potassium excretion.22
Regular aerobic exercise lowers systolic and diastolic blood pressure.23,24 Physicians should advise patients to engage in moderate to vigorous aerobic physical activity for 40 minutes three or four times per week to lower blood pressure. This is consistent with recommendations to obtain at least 150 minutes per week of moderate-intensity physical activity (such as brisk walking), 75 minutes per week of vigorous aerobic exercise (such as jogging or running), or a combination of both for cardiovascular health.18 Weight loss reduces blood pressure in a graded fashion in adults who are overweight or obese.25 Weight loss of approximately 4 kg (9 lb) is associated with a modest reduction in systolic and diastolic blood pressure, but the effects on mortality are unknown.26
Light alcohol consumption (less than one standard drink per day) is associated with reduced cardiovascular disease and all-cause mortality. However, moderate or excess intake (one or more standard drinks per day) increases the risks of hypertension and associated cardiovascular disease in a dose-dependent manner.27 Reducing heavy intake to two drinks per day improves blood pressure; further reductions may not provide additional benefits.28,29 Nicotine and caffeine increase blood pressure transiently but may be relevant if used frequently or shortly before blood pressure measurement. The effects of lifestyle modifications on blood pressure are summarized in Table 3.13,18,20,22–24,26,28
Pharmacotherapy
Physicians should prescribe blood pressure–lowering medication for patients with stage 1 hypertension and clinical ASCVD, an estimated 10-year ASCVD risk of 10% or higher, diabetes, kidney disease, or hypertensive end-organ damage, as well as for patients with stage 2 hypertension.2,4,30,31 For patients with stage 1 hypertension and a lower risk of ASCVD, pharmacotherapy is indicated when blood pressure goals are not achieved with three to six months of lifestyle modifications and may be considered in combination with lifestyle measures when systolic blood pressure is more than 10 mm Hg above goal.4,31
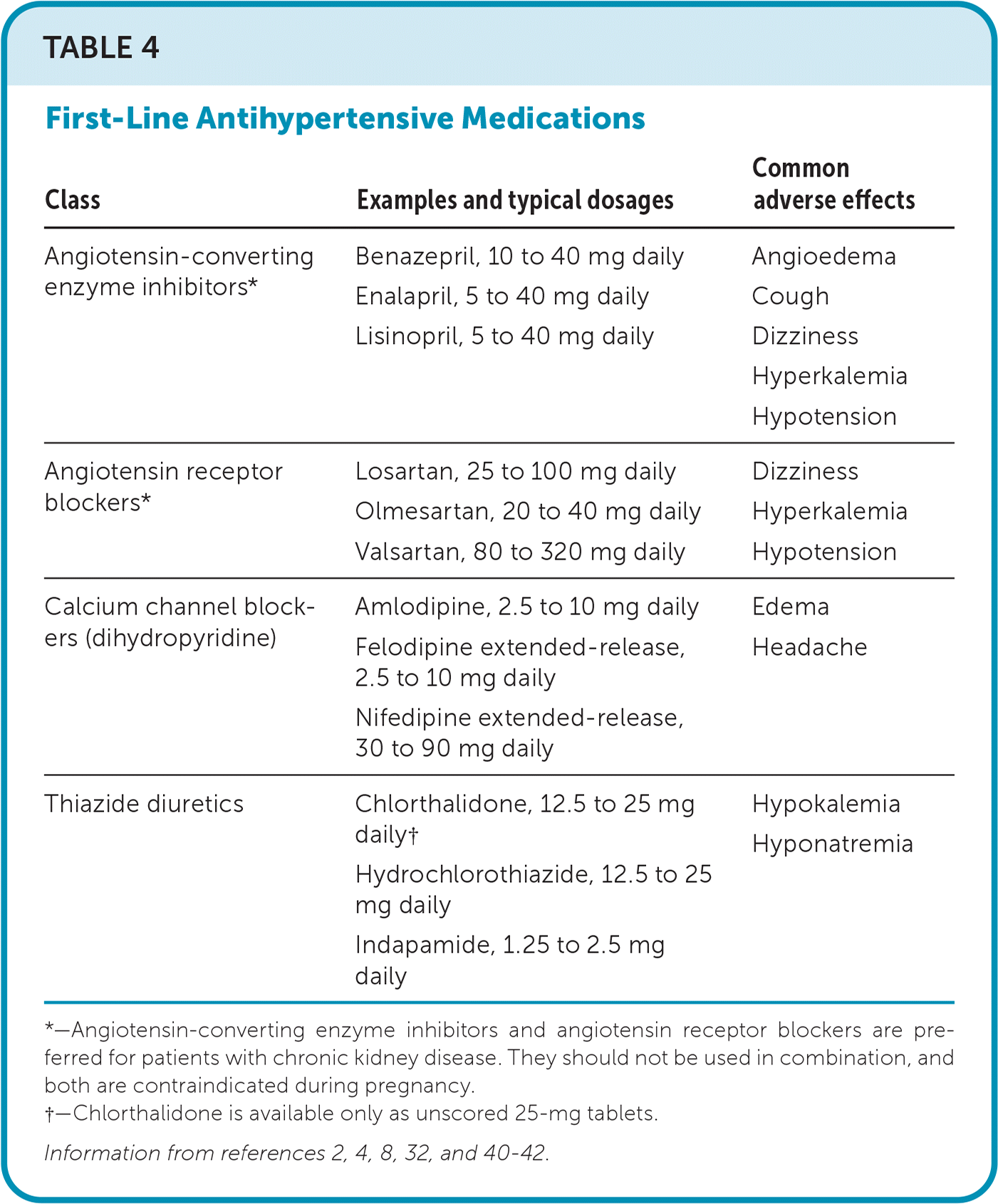
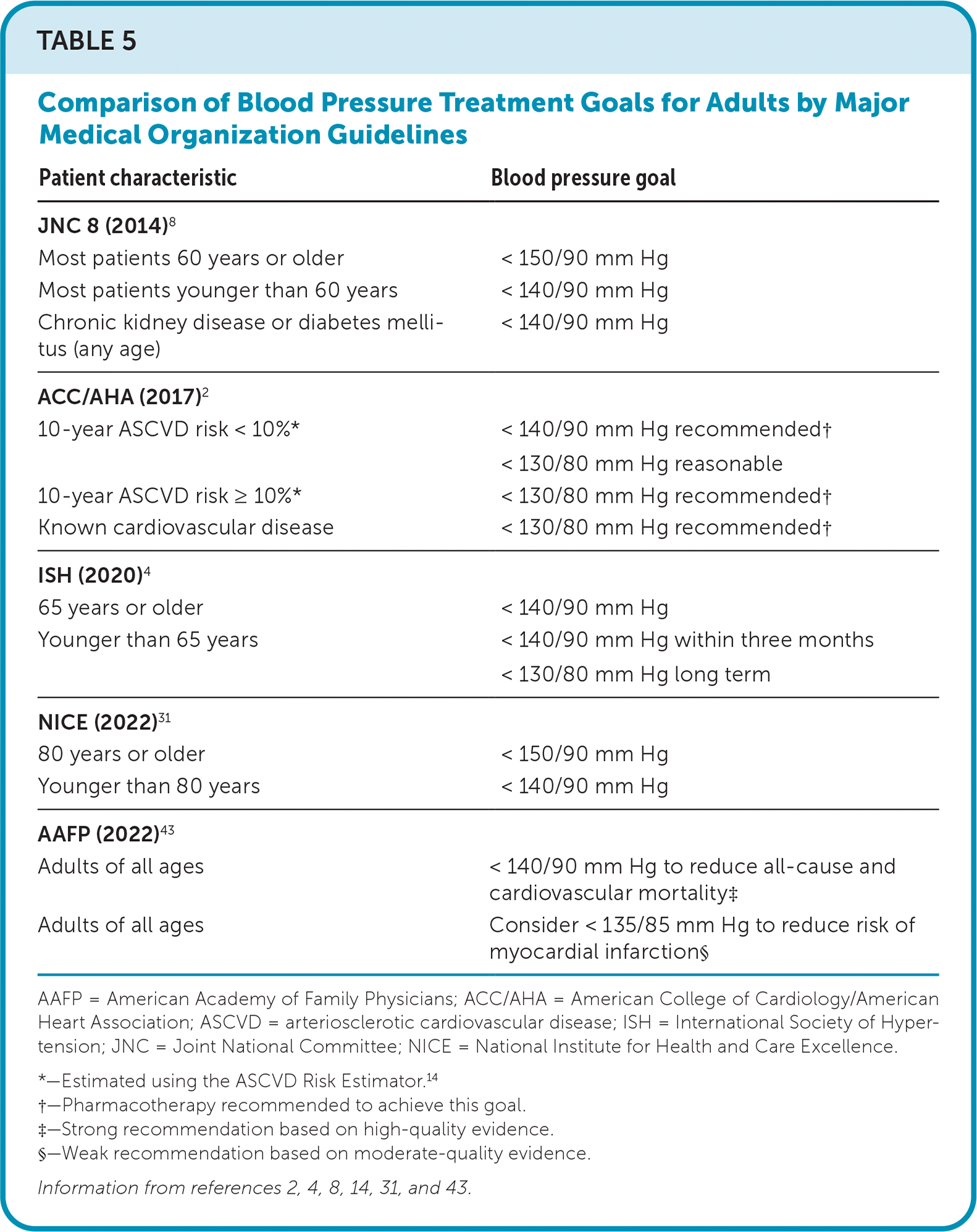
Initial antihypertensive treatment should include an angiotensin-converting enzyme (ACE) inhibitor, an angiotensin receptor blocker (ARB), a long-acting dihydropyridine calcium channel blocker, or a thiazide diuretic.2,4,8,32–35 An ACE inhibitor or an ARB is preferred for patients with proteinuric chronic kidney disease because of their ability to slow progression of the disease, especially in diabetic nephropathy.36 Nonpreferred anti-hypertensive medications may be used if indicated for comorbid conditions. For example, goal-directed medical therapy for ischemic heart disease and heart failure includes beta blockers in addition to ACE inhibitors or ARBs.2,4 Some guidelines have recommended initial drug selection based on race for monotherapy; however, despite guideline adherence, there is increasingly insufficient control of hypertension.37–39 Therefore, initial combination therapy with two antihypertensives from different classes is recommended for patients across racial groups with stage 2 hypertension or whose blood pressure is more than 20 mm Hg systolic or 10 mm Hg diastolic above goal.2,4 Common examples of first-line antihypertensive medications and their typical dosages are shown in Table 4.2,4,8,32,40–42 Guidelines on blood pressure treatment goals for adults are summarized in Table 5.2,4,8,14,31,43
TABLE 4. First-Line Antihypertensive Medications
| Class | Examples and typical dosages | Common adverse effects |
|---|---|---|
| Angiotensin-converting enzyme inhibitors* | Benazepril, 10 to 40 mg daily | Angioedema |
| Enalapril, 5 to 40 mg daily | Cough | |
| Lisinopril, 5 to 40 mg daily | Dizziness | |
| Hyperkalemia | ||
| Hypotension | ||
| Angiotensin receptor blockers* | Losartan, 25 to 100 mg daily | Dizziness |
| Olmesartan, 20 to 40 mg daily | Hyperkalemia | |
| Valsartan, 80 to 320 mg daily | Hypotension | |
| Calcium channel blockers (dihydropyridine) | Amlodipine, 2.5 to 10 mg daily | Edema |
| Felodipine extended-release, 2.5 to 10 mg daily | Headache | |
| Nifedipine extended-release, 30 to 90 mg daily | ||
| Thiazide diuretics | Chlorthalidone, 12.5 to 25 mg daily† | Hypokalemia Hyponatremia |
| Hydrochlorothiazide, 12.5 to 25 mg daily | ||
| Indapamide, 1.25 to 2.5 mg daily | ||
*—Angiotensin-converting enzyme inhibitors and angiotensin receptor blockers are preferred for patients with chronic kidney disease. They should not be used in combination, and both are contraindicated during pregnancy.
†—Chlorthalidone is available only as unscored 25-mg tablets.
TABLE 5. Comparison of Blood Pressure Treatment Goals for Adults by Major Medical Organization Guidelines
| Patient characteristic | Blood pressure goal |
|---|---|
| JNC 8 (2014)8 | |
| Most patients 60 years or older | < 150/90 mm Hg |
| Most patients younger than 60 years | < 140/90 mm Hg |
| Chronic kidney disease or diabetes mellitus (any age) | < 140/90 mm Hg |
| ACC/AHA (2017)2 | |
| 10-year ASCVD risk < 10%* | < 140/90 mm Hg recommended† |
| < 130/80 mm Hg reasonable | |
| 10-year ASCVD risk ≥ 10%* | < 130/80 mm Hg recommended† |
| Known cardiovascular disease | < 130/80 mm Hg recommended† |
| ISH (2020)4 | |
| 65 years or older | < 140/90 mm Hg |
| Younger than 65 years | < 140/90 mm Hg within three months |
| < 130/80 mm Hg long term | |
| NICE (2022)31 | |
| 80 years or older | < 150/90 mm Hg |
| Younger than 80 years | < 140/90 mm Hg |
| AAFP (2022)43 | |
| Adults of all ages | < 140/90 mm Hg to reduce all-cause and cardiovascular mortality‡ |
| Adults of all ages | Consider < 135/85 mm Hg to reduce risk of myocardial infarction§ |
AAFP = American Academy of Family Physicians; ACC/AHA = American College of Cardiology/American Heart Association; ASCVD = arteriosclerotic cardiovascular disease; ISH = International Society of Hypertension; JNC = Joint National Committee; NICE = National Institute for Health and Care Excellence.
*—Estimated using the ASCVD Risk Estimator.14
†—Pharmacotherapy recommended to achieve this goal.
‡—Strong recommendation based on high-quality evidence.
§—Weak recommendation based on moderate-quality evidence.
Recommendations for lower treatment goals in the 2017 American College of Cardiolog y/American Heart Association guidelines were influenced by the SPRINT (Systolic Blood Pressure Intervention Trial), which found lower rates of major cardiovascular events (1.7% vs. 2.2%; hazard ratio = 0.75; number needed to treat [NNT] = 61) and total mortality (3.3% vs. 4.5%; hazard ratio = 0.73; NNT = 90) in patients with increased cardiovascular risk who were treated to a systolic blood pressure target of less than 120 mm Hg compared with less than 140 mm Hg.44 However, a meta-analysis of nine trials, including SPRINT, found that only combined major cardiovascular events (6.2% vs. 7.3%; relative risk [RR] = 0.84; NNT = 91) and stroke (2.4% vs. 2.9%; RR = 0.82; NNT = 200) were reduced with intensive blood pressure lowering.45 The SPRINT also observed higher rates of hypotension, syncope, electrolyte abnormalities, and acute kidney injury in the intensive treatment group than in the standard treatment group (4.7% vs. 2.5%; hazard ratio = 1.88; number needed to harm [NNH] = 45).44 Of note, a recent secondary analysis of SPRINT found that the beneficial effect of intensive hypertension control on mortality was not evident 4.5 years after the trial ended, and mean systolic blood pressure increased, further illustrating the realities of managing hypertension in the outpatient setting.46,47
The American Academy of Family Physicians (AAFP) did not endorse the American College of Cardiology/American Heart Association guidelines because of concerns that the marginal clinical benefit achieved in treating high-risk patients to a lower blood pressure target may not outweigh the associated harms of treatment, especially when lower blood pressure goals are applied to large numbers of patients with low to moderate cardiovascular risk.48 Although the SPRINT posttrial follow-up data were not available to influence this decision, a large, longitudinal cohort study found no cardiovascular or mortality benefit from treating low-risk patients with mild hypertension.49 Antihypertensive treatment was associated with higher rates of hypotension (NNH = 41), syncope (NNH = 35), electrolyte abnormalities (NNH = 111), and acute kidney injury (NNH = 91).49
Recent Cochrane reviews found that treating blood pressure to a goal of less than 135/85 mm Hg compared with a standard target of less than 140/90 mm Hg did not further reduce mortality in a general population of adults with hypertension or in those with hypertension and clinica l ASCVD.50,51 Moderate-quality evidence suggested that over a course of 3.7 years, slightly lower rates of myocardial infarction (2.1% vs. 2.5%; RR = 0.84; 95% CI, 0.73 to 0.96; NNT = 250) and congestive heart failure (1.9% vs. 2.5%; RR = 0.75; 95% CI, 0.60 to 0.92; NNT = 167) were accompanied by an increase in serious adverse events (9.8% vs. 6.8%; RR = 1.44; 95% CI, 1.32 to 1.59; NNH = 33).50
Accordingly, the AAFP now recommends treating adults with hypertension to a blood pressure goal of less than 140/90 mm Hg to reduce the risk of all-cause and cardiovascular mortality (strong recommendation based on high-quality evidence). In addition, the AAFP recommends considering lowering blood pressure to less than 135/85 mm Hg to reduce the risk of myocardial infarction (weak recommendation based on moderate-quality evidence).43
Although even small reductions in blood pressure translate to significant improvements in morbidity and mortality for patients with hypertension,52 physicians should proceed with caution when prescribing antihypertensive medications to patients who are older or frail and at increased risk of adverse effects, such as orthostatic hypotension and acute kidney injury. Clinical judgment and shared decision-making are recommended when treating patients with mild hypertension, especially if their estimated risk of ASCVD is low.3,49
Monitoring Response to Treatment
Physicians should monitor patients’ response to treatment using a combination of office, home, and ambulatory blood pressure measurements.53 Patients taking antihypertensive pharmacotherapy should follow up monthly until blood pressure is controlled and then every three to six months thereafter.2 Lifestyle modifications and pharmacotherapy should be intensified as needed to help patients reach target blood pressure. Most patients require treatment with two or more antihypertensive agents.2,7 Early combination therapy lowers blood pressure more effectively and with fewer adverse effects than doubling the dose of a single agent54,55; however, patients should not take ACE inhibitors and ARBs together because of increased risks of hyperkalemia and acute kidney injury.40 Switching antihypertensive classes may be considered if no response to initial therapy occurs. Physicians should simplify dosing to facilitate patient adherence, use generic medications to minimize cost, and monitor for adverse effects of treatment (Table 4).2,4,8,32,40–42 Team-based patient care using medication titration by a nonphysician team member and multilevel strategies that combine patient health coaching, home blood pressure monitoring, and physician training are also effective for controlling blood pressure.56
Serum creatinine and potassium should be monitored closely after starting or increasing treatment with an ACE inhibitor, ARB, or diuretic. After blood pressure is controlled, serum creatinine and electrolytes should be measured once or twice yearly or as clinically indicated. Urine microalbumin to creatinine ratio should be obtained every one to two years to monitor for the development of microalbuminuria, but the benefit of continued monitoring is uncertain once patients are treated with ACE inhibitors or ARBs.45
This article updates a previous article on this topic by Langan and Jones.13
Data Sources: A PubMed search was completed in Clinical Queries using the key terms hypertension, high blood pressure, and treatment. The search included clinical trials, meta-analyses, practice guidelines, randomized controlled trials, reviews, and systematic reviews. The Agency for Healthcare Research and Quality’s evidence-based reports, the Cochrane database, Essential Evidence Plus, UpToDate, and the U.S. Preventive Services Task Force were also searched. Whenever possible, if studies used race and/or gender as patient categories, but did not define how these categories were assigned, they were not included in our final review. If studies that used these categories were determined to be essential and therefore included, especially for the practice guidelines, limitations were explicitly stated in the manuscript. Search dates: May to October 2022 and August 18, 2023.

