Group A beta-hemolytic streptococcal pharyngitis is a common infection responsible for more than 6 million office visits in the United States annually. Only 10% of adults seeking care for a sore throat have group A beta-hemolytic streptococcal pharyngitis; however, 60% or more are prescribed antibiotics. Guidelines recommend using clinical decision rules to assess the risk of group A beta-hemolytic streptococcal infection, followed by rapid antigen testing if a diagnosis is unclear, before prescribing antibiotics. Fever, tonsillar exudate, cervical lymphadenitis, and patient ages of 3 to 15 years increase clinical suspicion. A cough is more suggestive of a viral etiology. The limited history used in these decision rules is amenable to virtual visits. After a negative rapid antigen test result, a throat culture is recommended in children and adolescents. Penicillin and amoxicillin are first-line antibiotics, with a recommended course of 10 days; first-generation cephalosporins are recommended for patients with nonanaphylactic allergies to penicillin. There is significant resistance to azithromycin and clarithromycin in some parts of the United States. Steroids are not recommended for symptomatic treatment. Patients with worsening symptoms after appropriate antibiotic initiation or with symptoms lasting 5 days after the start of treatment should be reevaluated. Tonsillectomy is rarely recommended as a preventive measure: seven episodes of streptococcal pharyngitis in 1 year, five episodes in each of the past 2 years, or three episodes in each of the past 3 years are commonly used thresholds for considering surgery.
More than 24 million episodes of pharyngitis are diagnosed annually in the United States, with more than 6 million office visits attributable to group A beta-hemolytic streptococcal infection.1 This article provides a summary of the best available patient-oriented evidence about streptococcal pharyngitis and guideline recommendations using clinical decision rules to assess the risk of group A beta-hemolytic streptococcal infection, followed by rapid antigen testing if a diagnosis is unclear.
WHAT'S NEW ON THIS TOPIC

| A 2021 study of patients who had telemedicine and face-to-face visits on the same day noted that patients assessed as having low-risk McIsaac scores in the telemedicine visit also had low-risk scores in face-to-face visits. |
| In a cohort study, the use of broad-spectrum antibiotics for children with group A beta-hemolytic streptococcal pharyngitis was not associated with a reduction in the rate of treatment failure compared with narrow-spectrum antibiotics. |
| Acute rheumatic fever is increasingly rare. It has an estimated incidence of 0.5 episodes per 100,000 people in the continental United States, with higher rates in the Pacific Islands. Rheumatic heart disease develops in 50% to 70% of people with rheumatic fever. |
SORT: KEY RECOMMENDATIONS FOR PRACTICE
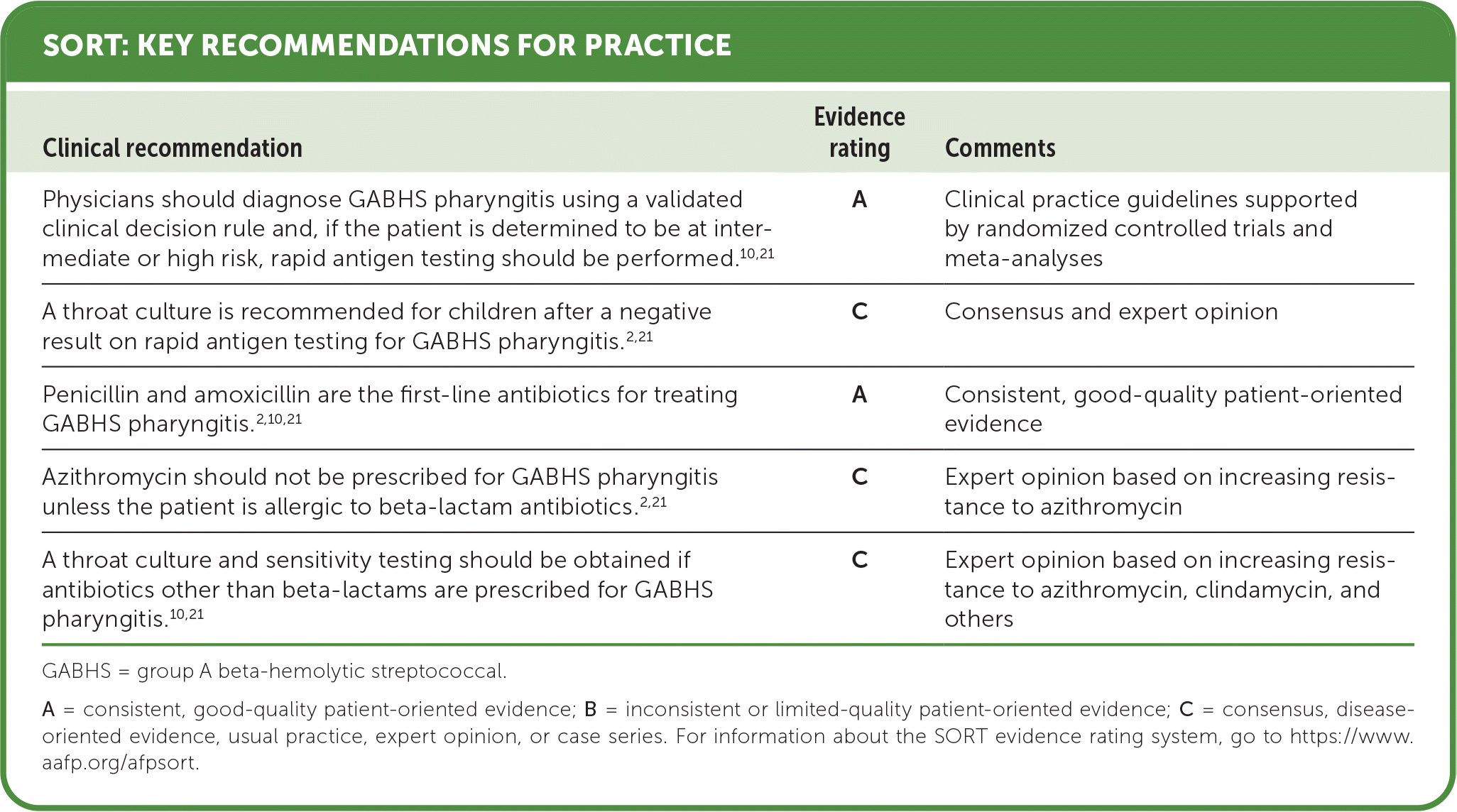
GABHS = group A beta-hemolytic streptococcal.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Epidemiology
- Streptococcal pharyngitis is highly unlikely in children younger than 3 years.2
- In the United States, group A beta-hemolytic streptococcal pharyngitis is associated with more than 90 outpatient diagnoses per 1,000 children 3 to 9 years of age each year and 40 diagnoses per 1,000 people 10 to 19 years of age each year; among people 40 to 64 years of age, the number of outpatient diagnoses declines to 1 per 1,000 people each year.1
- It is estimated that 10% to 15% of adults presenting with a “sore throat” have group A beta-hemolytic streptococcal infection; however, 60% to 70% receive antibiotic prescriptions.1,3
- Incidence varies seasonally, with higher rates in the late winter and early spring.4,5
Diagnosis
SIGNS AND SYMPTOMS
- Group A beta-hemolytic streptococcal pharyngitis should be suspected in patients with fever, tonsillar exudate, palatal petechiae, and enlarged, tender anterior cervical lymph nodes.2,6–8 Clinical suspicion should be increased for patients between 3 and 15 years of age.1,2
- Cough, coryza, and hoarseness are associated with a viral infection.2,6,7
- The differential diagnosis includes viral upper respiratory infections, infectious mononucleosis, and COVID-19.9,10
- If symptoms worsen or persist longer than 5 days, peritonsillar abscess, Lemierre syndrome, pharyngeal gonorrhea, or acute HIV infection should be considered.9–11 Peritonsillar abscesses and Lemierre syndrome likely have unilateral presentations.
CLINICAL DECISION RULES
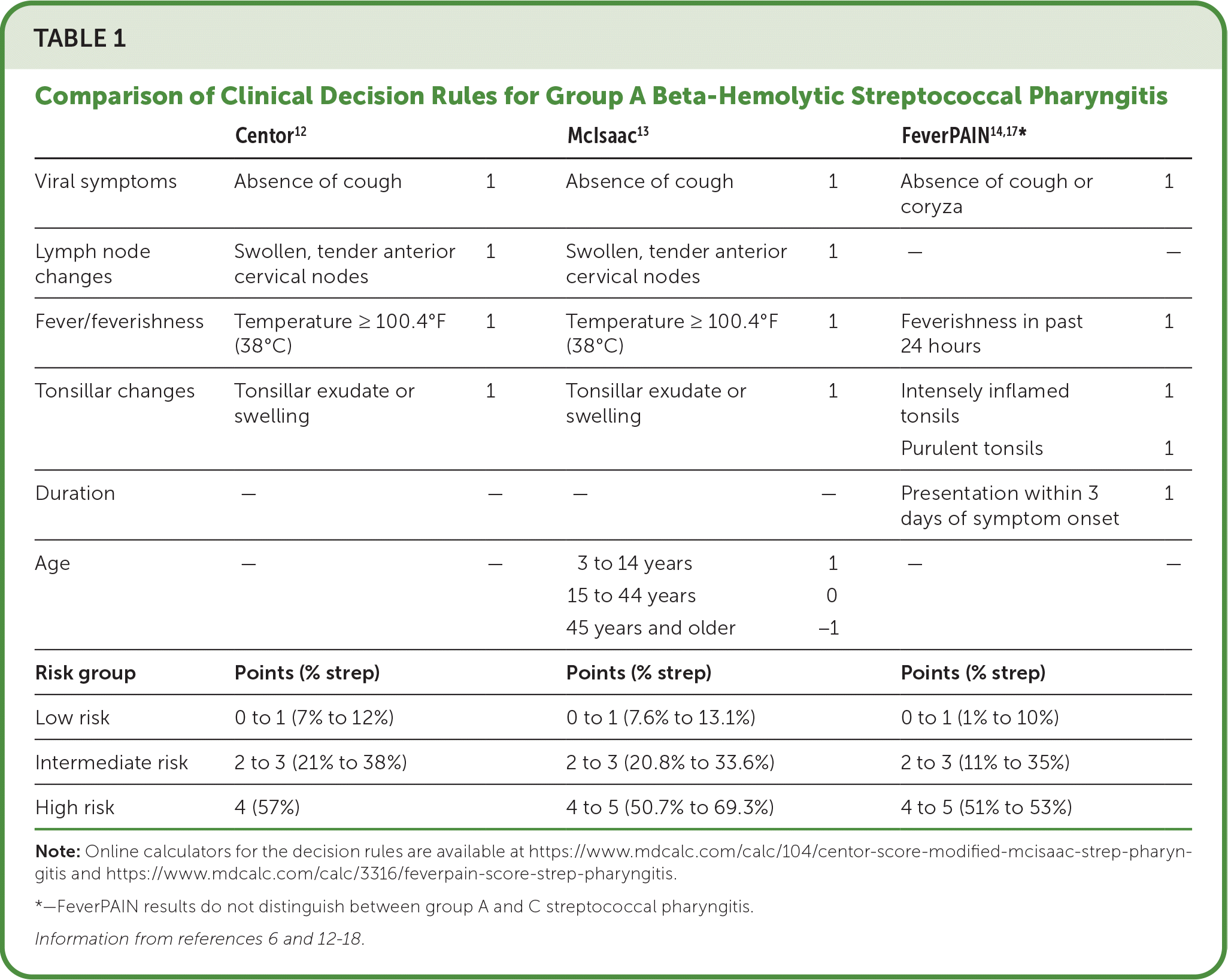
- Validated clinical decision rules for streptococcal pharyngitis include Centor,12 McIsaac (i.e., modified Centor),13 and FeverPAIN14 (Table 16,12–18 ). These decision rules have equivalent clinical performance.16,19,20
- No further diagnostic testing for group A beta-hemolytic streptococcal pharyngitis is recommended for patients determined to be at low risk based on these decision rules.2,10,21
- Using decision rules alone does not decrease antibiotic use compared with usual practice; however, using rapid diagnostic testing in conjunction with these rules does decrease antibiotic use.22
TABLE 1. Comparison of Clinical Decision Rules for Group A Beta-Hemolytic Streptococcal Pharyngitis
| Centor12 | McIsaac13 | FeverPAIN14,17 * | ||||
| Viral symptoms | Absence of cough | 1 | Absence of cough | 1 | Absence of cough or coryza | 1 |
| Lymph node changes | Swollen, tender anterior cervical nodes | 1 | Swollen, tender anterior cervical nodes | 1 | — | — |
| Fever/feverishness | Temperature ≥ 100.4°F (38°C) | 1 | Temperature ≥ 100.4°F (38°C) | 1 | Feverishness in past 24 hours | 1 |
| Tonsillar changes | Tonsillar exudate or swelling | 1 | Tonsillar exudate or swelling | 1 | Intensely inflamed tonsils Purulent tonsils | 1 1 |
| Duration | — | — | — | — | Presentation within 3 days of symptom onset | 1 |
| Age | — | — | 3 to 14 years 15 to 44 years 45 years and older | 1 0 −1 | — | — |
| Risk group | Points (% strep) | Points (% strep) | Points (% strep) | |||
| Low risk | 0 to 1 (7% to 12%) | 0 to 1 (7.6% to 13.1%) | 0 to 1 (1% to 10%) | |||
| Intermediate risk | 2 to 3 (21% to 38%) | 2 to 3 (20.8% to 33.6%) | 2 to 3 (11% to 35%) | |||
| High risk | 4 (57%) | 4 to 5 (50.7% to 69.3%) | 4 to 5 (51% to 53%) |
Note: Online calculators for the decision rules are available at https://www.mdcalc.com/calc/104/centor-score-modified-mcisaac-strep-pharyngitis and https://www.mdcalc.com/calc/3316/feverpain-score-strep-pharyngitis.
*—FeverPAIN results do not distinguish between group A and C streptococcal pharyngitis.
TELEMEDICINE
- Patients can provide key elements of their history for the evaluation of a sore throat equivalently in telemedicine and face-to-face visits.23,24
- On self-examination, patients tended to overreport tonsillar exudate, erythema, and lymphadenitis; compared with physician review, patient reports of exudate had 76.5% sensitivity and 100% specificity.23 Patients with smartphones had difficulty obtaining clinically useful images.23
- A 2021 study of patients who had telemedicine and face-to-face visits on the same day noted that patients who were at low risk based on the McIsaac decision rule during a telemedicine visit also tended to be at low risk in face-to-face visits.24
- Group A beta-hemolytic streptococcal pharyngitis has the potential to infect and reinfect household contacts.25 A person with symptoms of pharyngitis who has close contact with someone known to have group A beta-hemolytic streptococcal pharyngitis may be considered at higher risk than someone without contact.
- Some studies have suggested the use of telemedicine to identify patients with worsening symptoms or those at high risk of bacterial pharyngitis based on clinical decision rules who should be further evaluated in person.24,26,27
DIAGNOSTIC TESTING
- Rapid antigen testing should be obtained for patients at intermediate risk of group A beta-hemolytic streptococcal pharyngitis as determined by a Centor, McIsaac, or Fever-PAIN score.2,10,21
- Rapid antigen testing may be omitted for patients at low clinical risk, including children younger than 3 years.2
- For patients at high risk, rapid antigen testing may be performed, or patients may be treated with empiric antibiotics.10,14,15 Empiric antibiotics may be preferable when rapid antigen testing is unavailable or challenging to perform because rapid antigen testing sensitivity varies with clinical technique.28
- Rapid tests based on nucleic acid amplification techniques are available in the United States. Studies suggest that these tests have a sensitivity and specificity between 93% and 99%, but they are more expensive than rapid antigen tests.28 Clinical decision rules based on their use have not been developed.
- A throat culture is not indicated for most adults after a negative result on rapid antigen testing but may be appropriate for patients at higher risk of complications, such as those with suppressed immune systems or previous rheumatic heart disease.2,29
- The Centers for Disease Control and Prevention and the American Academy of Pediatrics recommend obtaining a throat culture for all children and adolescents after a negative result on rapid antigen testing because of the higher risk of complications.2,21 However, modeling has shown that this practice is not cost-effective because of the very low incidence of rheumatic heart disease in the United States, with a cost of approximately $8 million per case that is avoided.30
Treatment
ANTIBIOTIC TREATMENT
- Penicillin and amoxicillin are the recommended first-line antibiotics for group A beta-hemolytic streptococcal pharyngitis.2,10,21 The Centers for Disease Control and Prevention notes, “There has never been a report of a clinical isolate of group A strep that is resistant to penicillin.”10 The use of broad-spectrum antibiotics is not associated with a reduction in treatment failure rates.31
- For patients who require oral liquids, amoxicillin is more palatable than penicillin.
- For patients with nonanaphylactic allergies to penicillin or amoxicillin, first-generation oral cephalosporins (e.g., cephalexin) are recommended.10,21
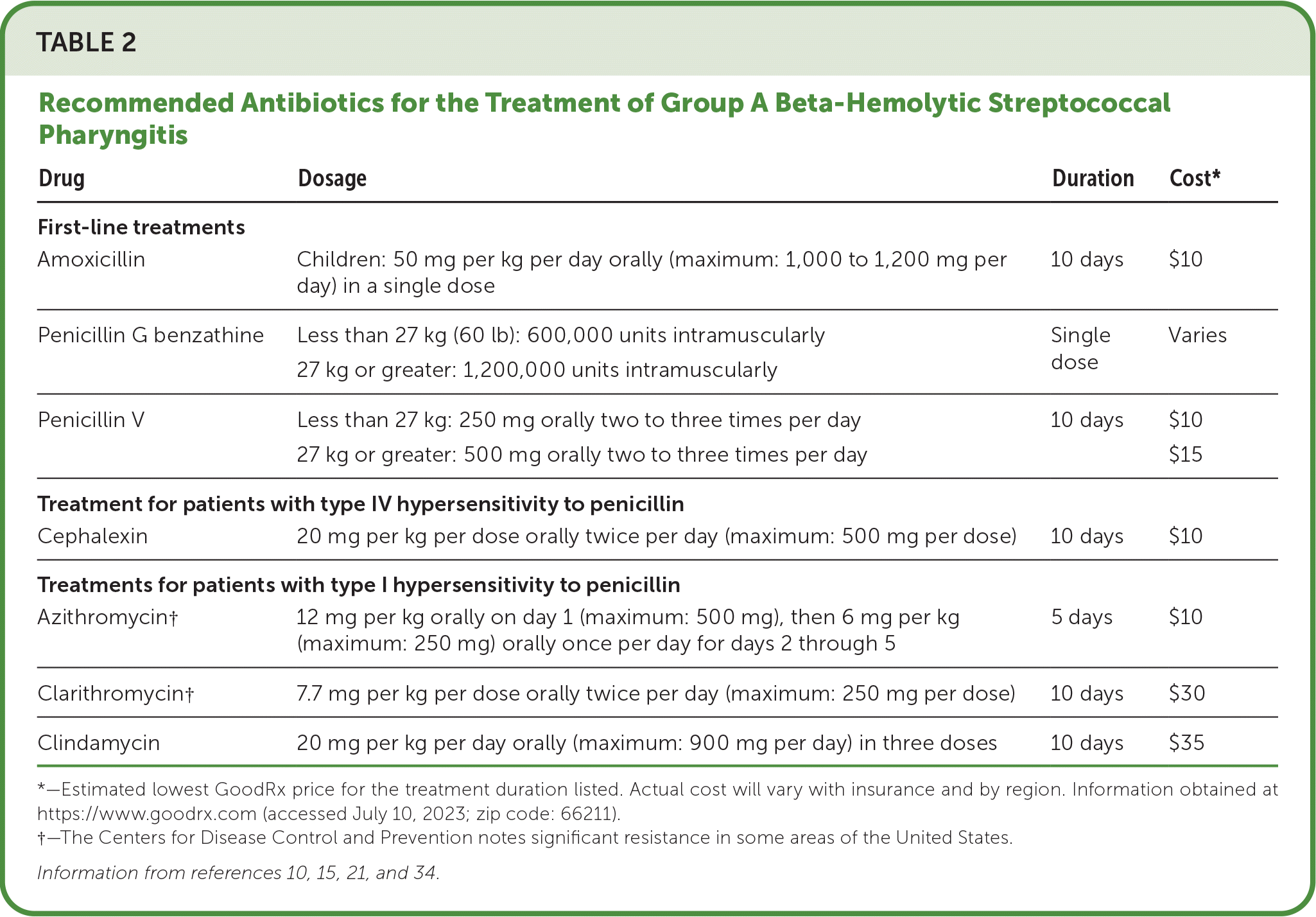
- In the case of anaphylactic allergies to beta-lactam antibiotics, a macrolide antibiotic or clindamycin may be used.10,15,21,32,33 Table 2 lists the recommended antibiotics for the treatment of group A beta-hemolytic streptococcal pharyngitis.10,15,21,34 If a non–beta-lactam antibiotic is prescribed, a throat culture and sensitivity testing should be performed because these antibiotics are associated with higher treatment failures.21
- The usual course of treatment for azithromycin is 5 days; for other antibiotics, a 10-day course is recommended by the Centers for Disease Control and Prevention and the American Academy of Pediatrics.10,21 A shorter, more intense course of treatment with penicillin V, 800 mg four times per day for 5 days, has been studied in patients 6 years and older.34,35 This shorter course is associated with fewer adverse effects and is noninferior for the resolution of symptoms.34,35
- Patients should stay home from work, school, or daycare until a fever has resolved and at least 12 hours have elapsed since starting antibiotics.10,21
- Guidelines recommend against treating Streptococcus dysgalactiae (previously associated with group C or G streptococcal infection) pharyngitis with antibiotics.2 However, one study showed that more than one-half of children found to have non–group A streptococcal pharyngitis were prescribed antibiotics.36 Because these infections do not lead to rheumatic fever, the use of antibiotics could be expected to reduce pain but would not prevent rheumatic heart disease.
TABLE 2. Recommended Antibiotics for the Treatment of Group A Beta-Hemolytic Streptococcal Pharyngitis
| Drug | Dosage | Duration | Cost* |
|---|---|---|---|
| First-line treatments | |||
| Amoxicillin | Children: 50 mg per kg per day orally (maximum: 1,000 to 1,200 mg per day) in a single dose | 10 days | $10 |
| Penicillin G benzathine | Less than 27 kg (60 lb): 600,000 units intramuscularly 27 kg or greater: 1,200,000 units intramuscularly | Single dose | Varies |
| Penicillin V | Less than 27 kg: 250 mg orally two to three times per day 27 kg or greater: 500 mg orally two to three times per day | 10 days | $10 $15 |
| Treatment for patients with type IV hypersensitivity to penicillin | |||
| Cephalexin | 20 mg per kg per dose orally twice per day (maximum: 500 mg per dose) | 10 days | $10 |
| Treatments for patients with type I hypersensitivity to penicillin | |||
| Azithromycin† | 12 mg per kg orally on day 1 (maximum: 500 mg), then 6 mg per kg (maximum: 250 mg) orally once per day for days 2 through 5 | 5 days | $10 |
| Clarithromycin† | 7.7 mg per kg per dose orally twice per day (maximum: 250 mg per dose) | 10 days | $30 |
| Clindamycin | 20 mg per kg per day orally (maximum: 900 mg per day) in three doses | 10 days | $35 |
*—Estimated lowest GoodRx price for the treatment duration listed. Actual cost will vary with insurance and by region. Information obtained at https://www.goodrx.com (accessed July 10, 2023; zip code: 66211).
†—The Centers for Disease Control and Prevention notes significant resistance in some areas of the United States.
SYMPTOMATIC TREATMENT
- Nonsteroidal anti-inflammatory drugs and acetaminophen are recommended for treating fever and pain associated with group A beta-hemolytic streptococcal pharyngitis.2
- Because other medications with a lower potential for adverse effects are readily available, the Infectious Diseases Society of America recommends against the use of steroids.2
- More recently, a meta-analysis noted that steroids had a more rapid onset of any pain relief (i.e., 5 hours, on average) and increased pain reduction at 24 hours for patients 5 years and older; a single dose of oral dexamethasone, 0.6 mg per kg (maximum dose: 10 mg), was the intervention most commonly studied.37
- Topical anesthetics and medicated throat lozenges may improve local pain but need to be used frequently. Products containing menthol are usually recommended for use every 2 hours as needed, but one study noted that more than 12% of patients use more than 10 menthol lozenges per day.38
SURGICAL TREATMENT
- Tonsillectomy is rarely recommended to decrease the risk of recurrent group A beta-hemolytic streptococcal pharyngitis.2,39 Benefits increase in patients with a demonstrated history of multiple infections: seven episodes in 1 year, five episodes in each of the past 2 years, or three episodes in each of the past 3 years are commonly used thresholds for considering surgery.40,41
- A 2014 Cochrane review noted that tonsillectomy decreased the number of sore throat episodes in children in the first year after surgery, with the most benefit in children who had more frequent episodes of sore throat. The effect of surgery after 3 years is modest.42,43
- Tonsillectomy in adults is associated with a decrease in the number of tonsillitis episodes, but with no change in the number of hospitalizations, and an increase in the number of primary care visits.44
- Tonsillectomy may have greater benefit for patients with multiple antibiotic allergies or other factors that make treatment more difficult.41
COMPLEMENTARY THERAPY
- Complementary therapy for pharyngitis is intended for symptom relief or immune system support, not eradication of group A beta-hemolytic streptococcal infection.
- Studies of herbal treatments such as ginger, echinacea, and Pelargonium sidoides (i.e., umckaloabo) have been poorly standardized with limited controls.45 With that caveat, at least one study has shown quicker resolution of non–group A beta-hemolytic streptococcal pharyngitis symptoms with the use of an oral P. sidoides extract.46
REFERRAL, CONSULTATION, AND HOSPITALIZATION
- About 10% of patients have treatment failure or relapse.47
- Patients with worsening symptoms after appropriate antibiotic initiation or with symptoms lasting 5 days after starting treatment should be reevaluated.9,10 Causes of treatment failure should be assessed (e.g., antibiotic resistance, medication nonadherence). Peritonsillar abscess and retropharyngeal abscess may be considered.
- Worsening symptoms after initial improvement, especially unilateral pain, rigors, and night sweats in a young adult, may suggest Lemierre syndrome.9 Hospitalization for administration of intravenous antibiotics, polymerase chain reaction testing for Fusobacterium necrophorum, and imaging of the soft tissues of the neck may be needed if the patient is bacteremic.48
- If the diagnosis of group A beta-hemolytic streptococcal pharyngitis was made without obtaining a culture or rapid antigen test, nonstreptococcal infections should be considered.
Prognosis
- In most patients in the United States, group A beta-hemolytic streptococcal pharyngitis is a self-limited disease.2
- Suppurative complications of group A beta-hemolytic streptococcal pharyngitis, including peritonsillar abscess, acute otitis media, sinusitis, and cellulitis, are rare, occurring in approximately 1% of patients.17
- Acute rheumatic fever, a serious sequela of the disease, is increasingly rare. It has an estimated incidence of 0.5 episodes per 100,000 people in the continental United States, with higher rates in the Pacific Islands.49,50 Rheumatic heart disease develops in 50% to 70% of people with rheumatic fever.50
This article updates previous articles on this topic by Kalra, et al.15; Choby51; and Hayes and Williamson.52
Data Sources: A PubMed search was completed in Medline, the Cochrane database, and Essential Evidence Plus using the key terms streptococcal pharyngitis, Centor criteria, McIsaac score, FeverPAIN, throat culture, and telemedicine and pharyngitis. Search dates: April 17, 2023; June 3, 2023; and March 3, 2024.

