The family physician often provides the first and only medical intervention for fingertip injuries. Proper diagnosis and management of fingertip injuries are vital to maintaining proper function of the hand and preventing permanent disability. A subungual hematoma is a painful condition that involves bleeding beneath the nail, usually after trauma. Treatment requires subungual decompression, which is achieved by creating small holes in the nail. A nail bed laceration is treated by removing the nail and suturing the injured nail bed. Closed fractures of the distal phalanx may require reduction but usually are minimally displaced and stable, and can be splinted. Open or intra-articular fractures of the distal phalanx may warrant referral. Patients with mallet finger cannot extend the distal interphalangeal joint because of a disruption of the extensor mechanism. Radiographs help to differentiate between tendinous and bony mallet types. Most mallet finger injuries heal with six to eight weeks of splinting, but some require referral. Flexor digitorum profundus avulsion always requires referral. Dislocations of the distal interphalangeal joint are rare and usually occur dorsally.
Fingertip injuries comprise many of the hand injuries treated by family physicians and are generally caused by athletic participation, occupational activities or domestic accidents. Recognition and proper management of fingertip injuries are vital to maintaining proper hand function and preventing permanent disability (Table 1).
TABLE 1 Diagnosis and Treatment of Fingertip Injuries
| Condition | Presentation | Diagnosis | Treatment | |
|---|---|---|---|---|
| Subungual hematoma | Painful, throbbing fingertip History of a crush injury is typical | Discolored nail Radiographs (AP, lateral, oblique) to rule out associated fractures | Subungual decompression through two to three small holes in nail created with cautery unit or heated paper clip Large subungual hematomas (involving ≥ 50 percent of the nail) may require nail removal and nail bed suturing. Splint the fingertip until tenderness subsides. | |
| Nail bed laceration | Painful fingertip with active bleeding | Grossly deformed nail with visible nail fracture and nail bed laceration History of a high-force crush injury or high-speed laceration (i.e., machine press or rotary saw) Nail bed lacerations may be associated with large subungual hematomas (involving ≥ 50 percent of the nail) Radiographs (AP, lateral, oblique) to rule out associated fractures | Nail plate removal with blunt dissection Primary suturing of the nail bed with 6-0 or 7-0 absorbable suture Maintain the space of the nail fold to allow for a new nail plate by placing the original nail or petroleum gauze over the nail bed and into the nail fold for two to three weeks. Refer nail bed lacerations involving distal tip amputation. | |
| Distal phalanx fracture | Painful, swollen fingertip History of a crush injury May have associated soft tissue damage to the finger pulp or nail bed laceration | Radiographs (AP, lateral, oblique) Three fracture patterns: longitudinal, transverse, comminuted | Closed fractures usually will not require reduction unless significantly angulated or displaced. Splint finger for three weeks. Open fractures may require referral unless physician is comfortable and familiar with the reparative process. Refer fractures that are irreducible, unstable or intra-articular and involving one third or more of the articular surface. | |
| Mallet finger | Flexion deformity of the DIPJ Painful, swollen fingertip May have occurred when trying to catch a ball | Inability to extend the distal phalanx at the DIPJ Radiographs (AP, lateral, oblique) Two forms of mallet finger: Tendinous—extensor tendon rupture Bony—bony avulsion fracture of the distal phalanx | Continuous splinting for six to eight weeks DIPJ must not be allowed to drop in flexion during treatment. Bony avulsions involving less than one third of the articular surface can be reduced with dorsal pressure and dorsal splinting for six to eight weeks. Post-reduction radiographs are essential to assess proper alignment. Refer failed nonsurgical treatment, bony avulsions that are irreducible or involve one third or more of the articular surface, or volar subluxation of the distal phalanx. | |
| FDP avulsion (“jersey finger”) | Painful, swollen finger, especially at the volar DIPJ History of failure to grab an object (e.g., football jersey or car door handle) Ring finger commonly involved | Inability to flex at the DIPJ PIPJ and MCPJ flexion preserved Radiographs (AP, lateral, oblique) to assess for tendinous rupture or bony avulsion fracture | Splint finger in comfortable position; refer to hand surgeon as soon as possible. | |
| DIPJ dislocation | Painful, swollen fingertip History of hyperextension injury is common Rare injury | Grossly deformed DIPJ Radiographs (AP, lateral, oblique); dislocations are often dorsal Splint in slight flexion for two weeks. | Reduction with hyperextension and longitudinal traction after digital nerve block | |
AP = anteroposterior; DIPJ = distal interphalangeal joint; FDP = flexion digitorum profundus; PIPJ = proximal interphalangeal joint; MCPJ = metacarpophalangeal joint.
Nail Anatomy
The nail is a structure of keratinized squamous cells that acts as a protective plate and enhances sensation of the fingertip. Two-point discrimination decreases if the nail is not present to act as a counterforce to the tip of the finger when an object is touched.1 The germinal matrix at the base of the nail bed gives rise to the nail (Figure 1). The dorsal fold that lies on the surface of the nail is the eponychium, or cuticle. The paronychium makes up the lateral borders of the When the edges of the nail are subjected to minor trauma, they can strip, producing hangnails.1 The junction of the nail bed and fingertip skin is the hyponychium.1 The nail bed, which is also known as the sterile matrix, adheres to the nail by adding squamous epithelial cells to the advancing nail, making it thicker, stronger and more adherent.2
FIGURE 1.
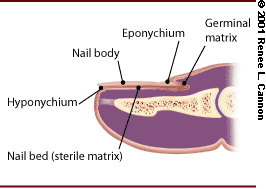
Fingernail anatomy.
Subungual Hematoma
A subungual hematoma is a painful condition that occurs when bleeding develops beneath the nail.2 This is typically caused by a crush injury. The hematoma becomes trapped between the rigid structures of the nail on top and the distal phalanx below (Figure 2).
FIGURE 2.
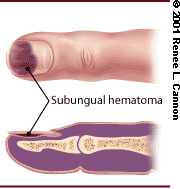
Subungual hematoma of the fingernail.
On clinical presentation, the patient complains of severe, throbbing pain in the finger. The affected nail is discolored from the hematoma, and the fingertip is exquisitely tender and swollen. Three-view radiographs (i.e., anteroposterior, lateral and oblique) of the finger are recommended because distal tuft fractures can occur with the injury. Distal tuft fractures that accompany subungual hematomas are usually comminuted, and reduction is seldom necessary. Two to three weeks of splinting after subungual decompression is recommended to allow the distal tuft to heal.
Treatment of the subungual hematoma relies on decompression, which is achieved by making small holes in the nail over the hematoma. A hand-held cautery unit or a heated paper clip can be used to burn two to three small holes, allowing the hematoma to drain (Figure 3). An Alumafoam splint (Conco Medical Company, Bridgeport, Conn.) can be applied to protect the fingertip for up to three days until the tenderness subsides. Large subungual hematomas that involve 50 percent or more of the nail are likely to have significant nail bed laceration requiring nail removal and primary suturing of the nail bed.2
FIGURE 3.
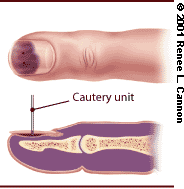
Decompression of subungual hematoma.
Nail Bed Lacerations
The mechanism of injury for nail bed lacerations is usually a high-force crush (e.g., injury by machine press) or high-speed laceration (e.g., injury by rotary saw). Radiographs are advisable because distal tuft fractures often accompany nail bed lacerations.
Attention to detail is critical in treating nail bed lacerations because regrowth of a nail with a normal appearance requires a smooth nail bed.3 If the nail bed laceration is allowed to heal by secondary intention, the resulting scar is likely to cause the healing nail to split or become nonadherent, producing a cosmetically unacceptable or painful nail.
Nail bed lacerations also require nail removal and primary suturing of the injured nail bed.2 A digital nerve block provides adequate pain relief during the procedure. To control active bleeding from the injured nail bed, a tourniquet (a quarter-inch Penrose drain) should be tightly wrapped around the base of the finger and clamped with a hemostat.4
The nail plate can be separated from the nail bed with blunt dissection by introducing the tip of dissecting scissors, a fine-tipped hemostat or a periosteal elevator under the free edge of the nail at the hyponychium.3 The tip of the instrument should be pointed up during dissection so that the tip rubs underneath the surface of the nail plate and not the nail bed, which would cause further damage. The instrument should be advanced carefully toward the nail fold in a fan-like pattern until the nail plate is attached only at the fold. By grasping the nail plate using a hemostat and gentle traction, the nail plate can be removed. The nail bed laceration should be approximated with 6-0 or 7-0 absorbable sutures (Figure 4)
FIGURE 4.
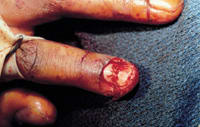
Repair of nail bed laceration.
Nail growth depends on maintaining the space of the nail fold between the dorsal roof and ventral floor. This can be accomplished by cleaning the removed nail and placing it in its original position, keeping the dorsal roof and ventral floor separated. The nail will also act as a splint if the distal phalanx is fractured. If the nail is damaged and not reusable, petroleum gauze cut in the shape of the nail can be placed over the exposed nail bed and into the nail fold. The nail or gauze should remain in place for two to three weeks to allow initial formation of a new nail plate. Full growth of the new nail will take approximately four to five months.
Referral to a hand or orthopedic surgeon is advised for nail bed lacerations that involve a distal tip amputation. A hooked nail may develop in the absence of bony support. Correction requires operative intervention that may include bone and pulp grafting.3
Distal Phalanx Fractures
The distal phalanx is the most commonly fractured bone of the hand.5 The mechanism of fracture is usually a crush injury. On clinical examination, the fingertip is swollen and painful. Extensive soft tissue damage to the finger pulp with associated nail bed laceration may occur. Examination should include evaluation of the motion of the distal interphalangeal joint (DIPJ) and two-point discrimination. Three-view radiographs should be obtained to determine the fracture pattern. Generally, three types of fracture occur: longitudinal, transverse and comminuted5 (Figures 5 and 6).
FIGURE 5.
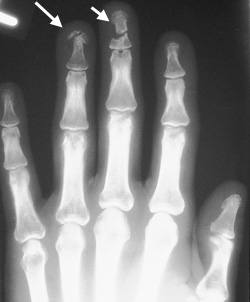
Frontal view showing distal phalanx fractures (arrows) of the middle and ring fingers.
FIGURE 6.
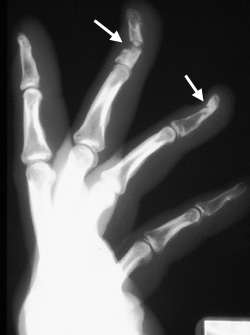
Lateral view showing distal phalanx fractures (arrows) of the middle and ring fingers.
Closed fractures are usually minimally displaced and stable. Closed reduction may be required if the fracture is significantly angulated or displaced. Following reduction, an Alumafoam splint should be used for three weeks to support and protect the distal phalanx.5 Fractures that are difficult to reduce or unstable after reduction may require orthopedic or hand referral. Often, these types of fractures will be encountered with transverse shaft or base fractures. Intra-articular fractures that involve one third or more of the articular surface warrant evaluation by an orthopedic or hand surgeon, because operative treatment is often required.6
Open fracture of the distal phalanx often necessitates referral to an orthopedic or hand subspecialist because digital nerve block, wound debridement, irrigation and soft tissue repair are required. Often, soft tissue repair will suffice to stabilize the fracture.5 Alumafoam splinting for four to six weeks, with frequent follow-up, is recommended. Prophylactic antibiotics are unnecessary, provided the wound is aggressively irrigated and debrided.7 Tetanus immunization should be updated, if necessary. Occasionally, fractures that are inadequately treated progress to a painful nonunion or osteomyelitis. Fractures of these small bones should not be taken lightly.
Mallet Finger
Mallet finger is a flexion deformity of the DIPJ caused by a disruption of the extensor mechanism. This injury is also known as “baseball finger” or, more accurately, “drop finger.” The two forms of mallet finger are a tendinous mallet, which involves only the extensor tendon, and a bony mallet, which involves an avulsion fracture of the distal phalanx.5
Mallet finger injury is caused by forcibly flexing the DIPJ during active extension (e.g., striking the fingertip when attempting to catch a ball). Acutely, the patient presents with a painful and swollen distal finger and is unable to actively extend the DIPJ. Three-view radiographs are recommended because a bony mallet is difficult to diagnose by physical examination. The lateral view is optimal to visualize a bony avulsion at the dorsal base of the distal phalanx. With serious injury, the bony avulsion may be accompanied by a volar subluxation of the distal phalanx. Radiographs of a tendinous mallet may disclose only soft tissue swelling.
Nonoperative treatment is recommended for most mallet finger injuries; however, bony avulsions involving one third or more of the articular surface of the distal phalanx or those with volar subluxation of the distal phalanx should be referred.6 Bony avulsions involving less than one third of the articular surface of the distal phalanx can be reduced with dorsal pressure followed by dorsal splinting. Post-reduction radiographs with the splint applied must be obtained to assess proper alignment. Bony avulsions that cannot be reduced and that fail nonsurgical treatment should be referred as well.
Continuous splinting for six to eight weeks is the recommended treatment for mallet finger injuries. Dorsal, volar and stack splints have been used with good results.8 Splinting should hold the DIPJ in neutral extension or slight hyperextension. To avoid skin necrosis, extreme hyperextension and pressure to the dorsum of the DIPJ should be avoided. The proximal interphalangeal joint is not immobilized. The physician must stress to the patient that the DIPJ should never be allowed to drop in flexion. When changing splints and examining the finger, the patient must be shown how to support the distal phalanx on a flat surface such as the edge of a table or a thumb. The patient should be aware that assistance may be necessary when applying a new splint.9
Follow-up examinations should be performed at two-week intervals until the injury has healed. Bony avulsions require radiographs at these times. After healing has occurred, night splinting should be continued for two to three additional weeks.
Flexor Digitorum Profundus Avulsion (Jersey Finger)
Flexor digitorum profundus (FDP) avulsion, or “jersey finger,” occurs when the actively flexed DIPJ is forced into extension, as may occur when a football player grabs another player's jersey during a tackle. Simple movements, such as lifting the latch on a car door, can also cause an FDP avulsion. The ring finger is most commonly affected.10 Because the ring finger protrudes the farthest in the grasping position, it is more susceptible to injury. FDP avulsion causes an inability to flex at the DIPJ.
Accurate diagnosis is critical because FDP avulsion requires operative repair. This injury is often overlooked, and delays in treatment can lead to irreparable fibrosis and scarring of the tendon sheath. Diagnosis can be made on the basis of a history of the typical mechanism of injury and the inability to flex the injured finger at the DIPJ.
On clinical examination, the finger may be swollen and tender along the volar surface of the DIPJ. With the finger extended to isolate the FDP, DIPJ flexion is absent. Flexion at the proximal interphalangeal joint and the metacarpophalangeal joint is preserved because of the flexor digitorum superficialis and lumbrical muscles, respectively. Three-view radiographs are recommended because a bony avulsion from the volar aspect of the distal phalanx can occur. If a large bony fragment is present, retraction of the FDP could be limited to the level of the middle phalanx. In pure tendinous injuries, the FDP can retract to the level of the palm. Once the diagnosis has been made, the finger should be splinted, and the patient should be referred to a hand surgeon as soon as possible.
Distal Interphalangeal Joint Dislocation
Dislocations of the distal interphalangeal joint are rare and often dorsal rather than volar. Distal phalanx fractures and tendon injuries may be associated. Hyperextension is the common mechanism of injury.
Clinically, the DIPJ will be grossly deformed. The dislocation is clearly demonstrated on lateral radiograph. Digital nerve block followed by hyperextension and longitudinal traction successfully reduces the dislocation. Splinting the finger in slight flexion for two weeks should promote proper healing.5 If the dislocation is irreducible or unstable after reduction, referral to an orthopedic or hand subspecialist is advised.

