A 39-year-old man presented with small nodules that had developed in his tattoos over the previous eight weeks. The nodules were not painful or pruritic. They were present only in the blue portions of the tattoo, but appeared in different tattoos on his arms and upper back (Figures 1 and 2). The tattoos were professionally applied about 12 to 13 years prior at the same tattoo parlor.
Figure 1.
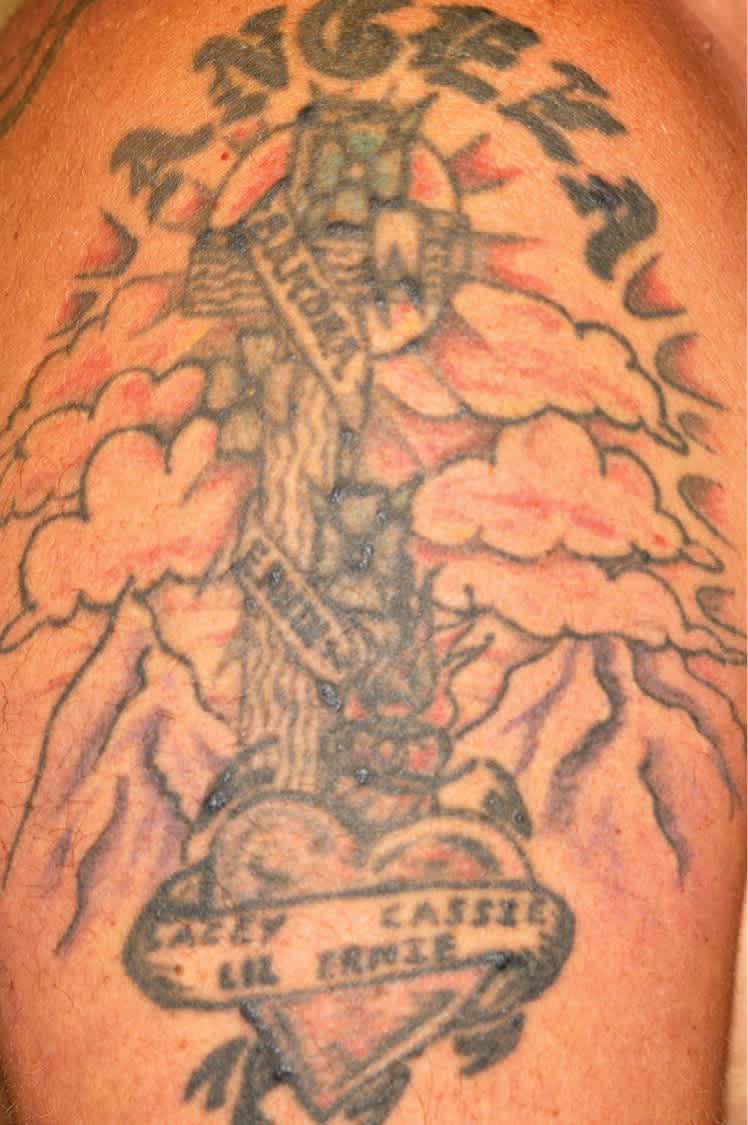
Figure 2.

The patient had diabetes mellitus, hypertension, and gout, which were all well controlled. He was also a smoker. He was taking metformin (Glucophage), glipizide (Glucotrol), allopurinol (Zyloprim), lisinopril (Zestril), and meloxicam (Mobic).
The nodules continued to develop over the next six weeks, after which no significant changes were noted. A biopsy was performed.
Question
Based on the patient’s history and physical examination findings, which one of the following is the most likely diagnosis?
A. Granulomatous reaction.
B. Keloid.
C. Pseudolymphomatous reaction.
D. Pyoderma gangrenosum.
Discussion
The answer is A: granulomatous reaction. A granulomatous reaction is a giant cell reaction, usually from a foreign body too large to be ingested by polymorphonuclear cells or macrophages.1 The patient’s pathology results confirmed a foreign body granulomatous inflammation from carbonaceous material, possibly tattoo pigment. Granulomatous reactions may be localized hypersensitivity reactions2 or local reactions reflecting systemic diseases, such as sarcoidosis.3
Granulomatous reactions from tattoos are thought to be an acquired hypersensitivity reaction to metallic ions in the pigment, and occur in the deeper dermal layers of the skin.4 The reaction may appear several months or years after tattoo application. Granulomas have been reported with both artistic and cosmetic tattooing.5 Treatment of granulomatous reactions to tattoos has variable success. Topical or intralesional corticosteroid injection or laser ablation may be beneficial; however, these treatments may cause areas of hypopigmentation or scarring within the tattoo. Some reactions may resolve spontaneously.
Keloids are caused by an exuberant healing response, in which fibrous scars extend beyond the borders of the original wound months after trauma or surgery. They occur more often in darkly pigmented skin and in slow-healing wounds, such as burns. Areas more susceptible to keloids include the sternum, upper arms, earlobes, and cheeks. Keloids occasionally are tender, pruritic, or painful.6
Pseudolymphomatous reaction can be a delayed hypersensitivity to tattoo pigment, usually red pigment. Most reactions are characterized by flesh-colored to plum or plum-red indurated nodules and plaques. These can appear similar to cutaneous B-cell lymphoma. The pathologic changes differ from those of a granulomatous reaction by the predominance of lymphoid infiltrate, mainly CD3+ T lymphocytes with pseudolymphomatous reactions and the predominance of polymorphonuclear cells or macrophages with granulomatous reactions.7
Pyoderma gangrenosum is an uncommon inflammatory condition of uncertain etiology. It typically begins as a pustule or vesicle that progresses to an ulcer or deep erosion with violaceous overhanging or undermined borders. Pyoderma gangrenosum is characterized by ulcers on the lower extremities, but it may occur anywhere. It is often associated with systemic diseases. It is also associated with ulcerative colitis and diffuse dermal infiltration with neutrophils.8
Summary Table
| Condition | Characteristics |
|---|---|
| Granulomatous reaction | Giant cell reaction from a foreign body too large to be ingested by polymorphonuclear cells or macrophages |
| Keloid | Exuberant healing response occurring months after trauma or surgery; more common in darkly pigmented skin and in slow-healing wounds, such as burns; occasionally tender, pruritic, or painful |
| Pseudolymphomatous reaction | Pseudolymphoma can be a delayed hypersensitivity to tattoo pigment, usually red pigment |
| Pyoderma gangrenosum | Typically begins as a pustule or vesicle that progresses to an ulcer or deep erosion with violaceous overhanging or undermined borders; associated with ulcerative colitis and diffuse dermal infiltration with neutrophils |

