A 4-day-old infant presented for an initial well-child visit. His mother was concerned about discoloration on the right side of the infant's face. The discoloration was present at birth and had not changed in color or size. The mother reported that the infant showed no signs of bleeding, pruritus, or pain. He had no other lesions on his body.
The patient was born at full term by spontaneous vaginal delivery following an uncomplicated pregnancy and delivery. His birth weight was 3.19 kg (7 lb). The results of his newborn screening were pending at the time of the clinic visit, but his hearing test findings were normal. The family had no history of similar facial discoloration.
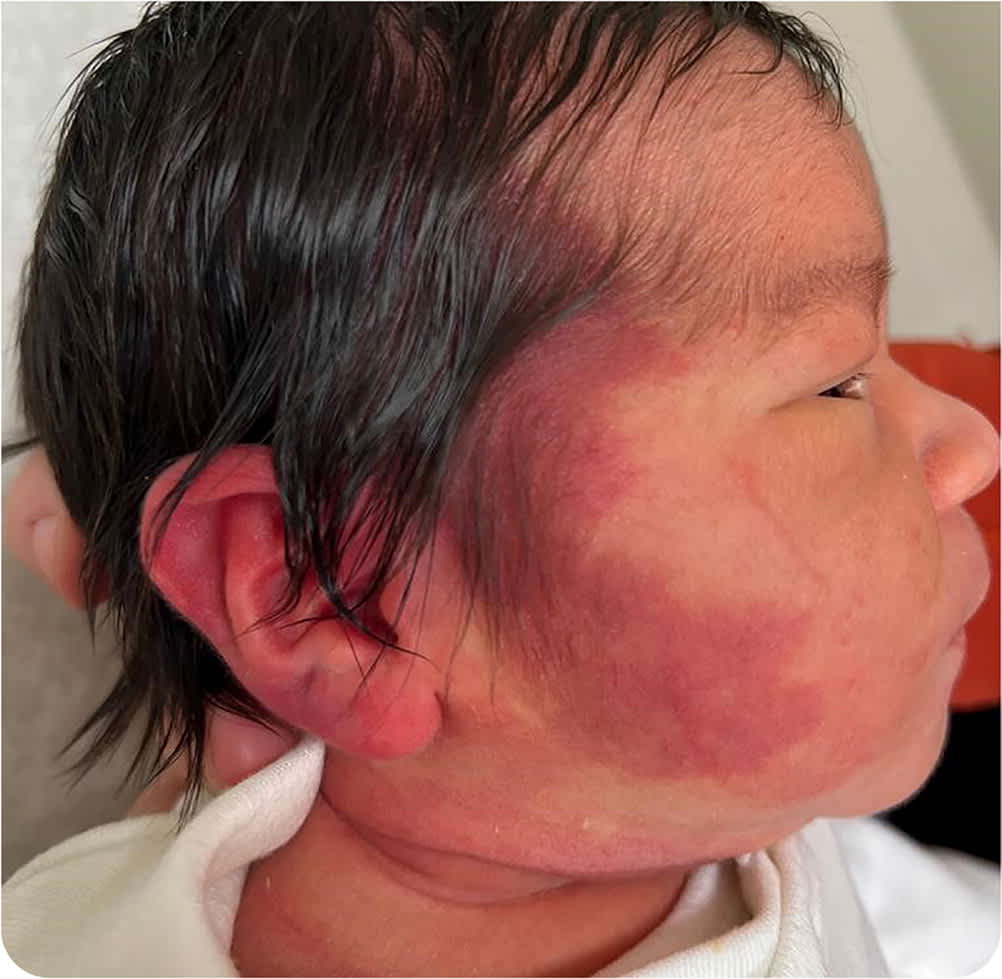
Physical examination revealed a flat, blanchable facial lesion that was purple-red. It was located on the right side of the infant's face with a temporomandibular distribution that included the right ear (Figure 1). No other dysmorphic features were apparent.
FIGURE 1
Question
Based on the patient's history and physical examination, which one of the following is the most likely diagnosis?
- A. Cavernous hemangioma (deep hemangioma).
- B. Cephalohematoma.
- C. Child abuse.
- D. Nevus flammeus (port-wine stain).
- E. Nevus simplex (macular stain).
Discussion
The correct answer is D: nevus flammeus, also known as port-wine stain. This is a congenital vascular malformation that most commonly affects the face and neck of newborns. It is caused by ectasia of the tubular structure of the blood vessels. There is also a decrease in nerve fibers in the affected blood vessels. Therefore, the lesions are believed to be a result of a neural deficiency of the sympathetic nervous system and are not genetic. They rarely cross the midline.
On examination, lesions are blanchable, flat, pink-to-purple patches with irregular borders. They are smooth at birth but can become papular. The color typically darkens with age. Glaucoma is present in 10% of cases that extend to the eyelids.1,2 Rarely, lesions on the forehead and eyelids can be associated with Sturge-Weber syndrome.3 In these cases, the risk of blindness, focal epilepsy, hemiplegia, and learning disability increases.1,2 Nevus flammeus occurs in approximately 1 out of 300 patients, whereas Sturge-Weber syndrome occurs in about 1 out of 20,000 to 50,000 patients.4
Cavernous hemangiomas, also known as deep hemangiomas of the dermis, have ill-defined borders and appear as slightly raised nodules. They are dilated vessels deep in the dermis. Lesions may appear red, blue, pale, or the same color as the surrounding skin. They are present at birth and spontaneously resolve with age. Cavernous hemangiomas are often associated with Kasabach-Merritt syndrome, a clotting cascade abnormality that increases the risk of coagulopathy.2
Cephalohematoma is caused by injury to the newborn during birth and is more common with forceps- or vacuum-assisted deliveries. The lesion is a subperiosteal collection of blood caused by the rupture of vessels over the parietal or occipital bone. It presents as swelling that does not cross suture lines and may be accompanied by discoloration. If necessary, computed tomography or magnetic resonance imaging can confirm the subperiosteal location of the cephalohematoma. The condition is a risk factor for hyperbilirubinemia; closefollow-up is recommended. Most cephalohematomas resolve spontaneously over a few weeks without intervention. Potential complications include calcified hematomas, infection, osteomyelitis, and sepsis.5
The possibility of child abuse is indicated by any lesion on a child younger than 9 months who is not independently mobile. Lesions not located on bony prominences should raise special concern; these areas include buttocks, genitalia, back, trunk, inner thighs, cheeks, ear lobes, and neck. Lesions caused by child abuse often occur in multiple clusters in different stages of healing. Imprints may indicate devices used such as hands, belt buckles, fingernails, hair-brushes, coat hangers, ropes, and cords.6
Nevus simplex, also known as macular stain, is a blanchable, pink-red patch that presents in newborns. These capillary lesions occur in 40% to 60% of infants, most commonly on the eyelid, glabella, and midline of the nape of the neck. Nevus simplex generally fades within one to two years, although lesions on the back of the neck (stork bites) can persist. Rarely, nevi are associated with extracutaneous disorders such as spinal dysraphism, Beckwith-Wiedemann syndrome, or macrocephaly-capillary malformation syndrome.7
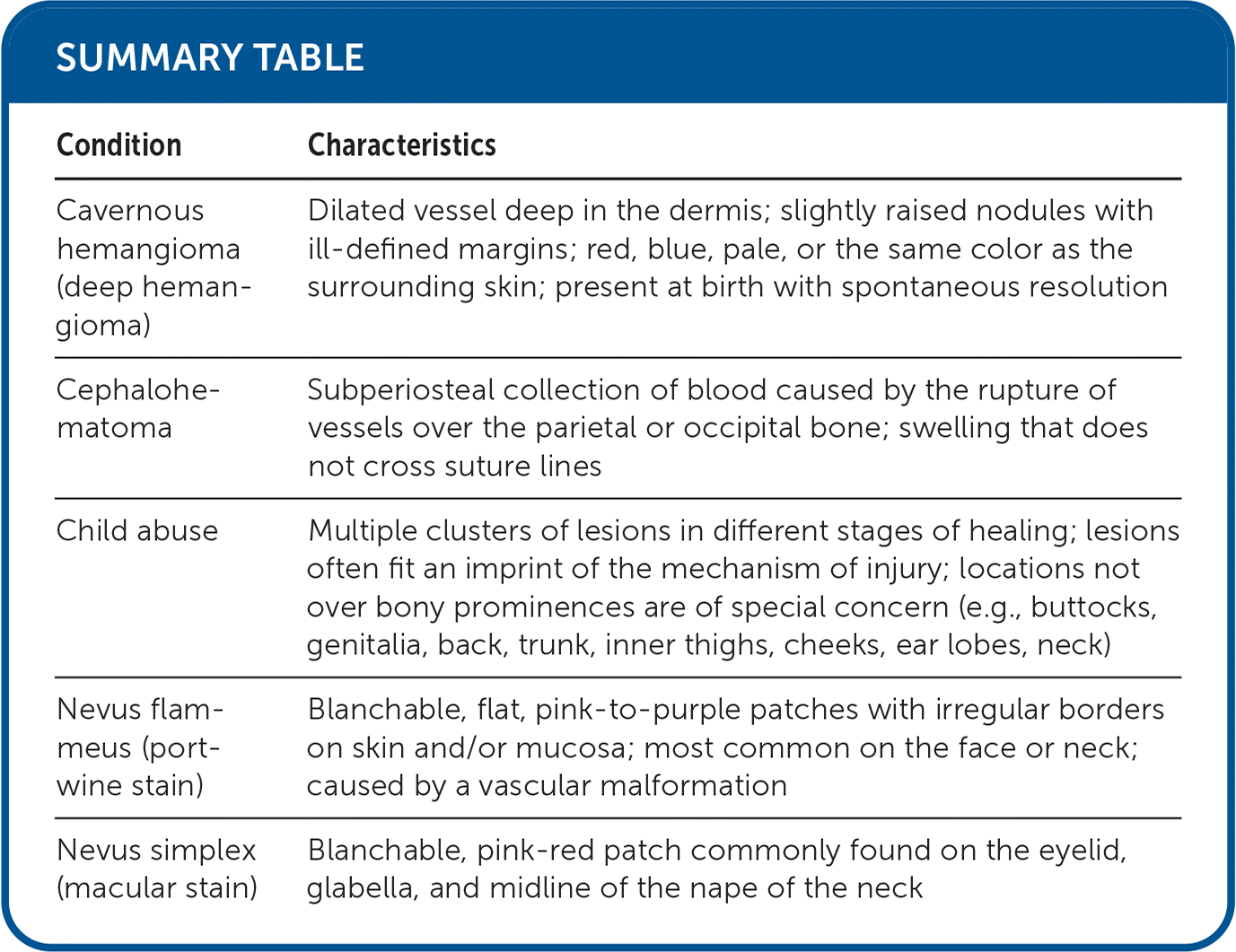
SUMMARY TABLE
| Condition | Characteristics |
|---|---|
| Cavernous hemangioma (deep hemangioma) | Dilated vessel deep in the dermis; slightly raised nodules with ill-defined margins; red, blue, pale, or the same color as the surrounding skin; present at birth with spontaneous resolution |
| Cephalohematoma | Subperiosteal collection of blood caused by the rupture of vessels over the parietal or occipital bone; swelling that does not cross suture lines |
| Child abuse | Multiple clusters of lesions in different stages of healing; lesions often fit an imprint of the mechanism of injury; locations not over bony prominences are of special concern (e.g., buttocks, genitalia, back, trunk, inner thighs, cheeks, ear lobes, neck) |
| Nevus flammeus (port-wine stain) | Blanchable, flat, pink-to-purple patches with irregular borders on skin and/or mucosa; most common on the face or neck; caused by a vascular malformation |
| Nevus simplex (macular stain) | Blanchable, pink-red patch commonly found on the eyelid, glabella, and midline of the nape of the neck |

