Obesity is defined as a chronic, relapsing, multifactorial, neurobehavioral disease in which weight status is measured by body mass index (BMI).1 Obesity is further categorized into classes I, II, and III.1 In 2023, more than one-third of women 20 to 39 years of age had obesity.2 Obesity during pregnancy is associated with adverse pregnancy and neonatal outcomes, including spontaneous abortion, congenital anomalies, gestational diabetes, hypertensive disorders of pregnancy, stillbirth, cesarean delivery, and postpartum hemorrhage.3
Obesity is a complex disease that is often falsely attributed to personal decisions and willpower. It is our responsibility as clinicians to recognize and reduce weight bias. Proactive measures include asking for permission to discuss weight; using patient preferred terms for weight status; using people-first language (eg, patient with obesity rather than obese patient) in communication and documentation; focusing on holistic well-being and health behaviors rather than weight as a number; and recognizing the limitations of BMI as an indirect measure of adiposity, which may not correlate directly with metabolic disease.4
PRECONCEPTION CARE
Health behaviors and interventions that lead to a loss of as little as 5% to 10% total body weight before pregnancy can improve metabolic dysfunction and decrease rates of perinatal complications associated with obesity.5 Motivational interviewing should be used to discuss weight history and goals.
Nutrition recommendations should center around eating patterns and preferences, with a goal of consuming a variety of nutrient-dense foods in appropriate portion sizes.6 Physical activity goals should be individualized, with goals of achieving 150 minutes per week of moderate-intensity exercise, incorporating resistance training, and avoiding prolonged sedentary time.6,7 Anti-obesity medications are contraindicated in pregnancy and should also be avoided in patients who are breast-feeding or trying to become pregnant.8 Contraception should be addressed before prescribing anti-obesity medications, and the medications should be discontinued if pregnancy occurs.
ANTEPARTUM MANAGEMENT
First Trimester
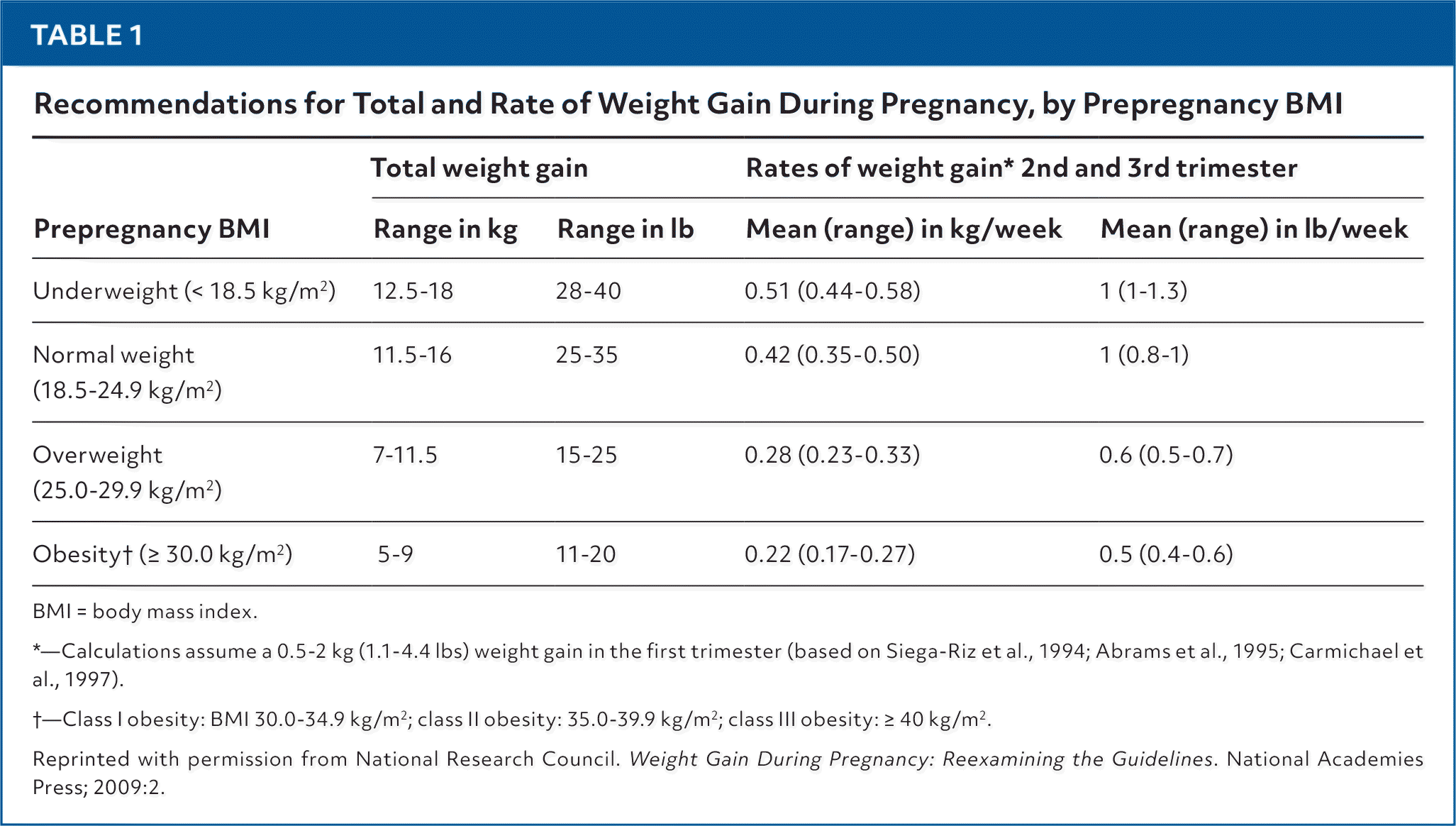
First-trimester ultrasonography can confirm estimated due date in the setting of irregular ovulation. There is insufficient evidence to recommend more than the standard 400 mcg per day of folic acid supplementation, even with the increased risk of congenital malformations associated with obesity.9 Early prenatal care should include assessment of weight status, review of the Institute of Medicine (IOM) pregnancy weight gain guidelines (Table 110), and screening for metabolic risk factors.3 Weight gain guidelines during pregnancy are based on BMI before conception.11
TABLE 1. Recommendations for Total and Rate of Weight Gain During Pregnancy, by Prepregnancy BMI
| Prepregnancy BMI | Total weight gain | Rates of weight gain* 2nd and 3rd trimester | ||
|---|---|---|---|---|
| Range in kg | Range in lb | Mean (range) in kg/week | Mean (range) in lb/week | |
| Underweight (< 18.5 kg/m2) | 12.5–18 | 28–40 | 0.51 (0.44–0.58) | 1 (1–1.3) |
| Normal weight (18.5–24.9 kg/m2) | 11.5–16 | 25–35 | 0.42 (0.35–0.50) | 1 (0.8–1) |
| Overweight (25.0–29.9 kg/m2) | 7–11.5 | 15–25 | 0.28 (0.23–0.33) | 0.6 (0.5–0.7) |
| Obesity† (≥ 30.0 kg/m2) | 5–9 | 11–20 | 0.22 (0.17–0.27) | 0.5 (0.4–0.6) |
BMI = body mass index.
*—Calculations assume a 0.5–2 kg (1.1–4.4 lbs) weight gain in the first trimester (based on Siega-Riz et al., 1994; Abrams et al., 1995; Carmichael et al., 1997).
†—Class I obesity: BMI 30.0–34.9 kg/m2; class II obesity: 35.0–39.9 kg/m2; class III obesity: ≥ 40 kg/m2.
Reprinted with permission from National Research Council. Weight Gain During Pregnancy: Reexamining the Guidelines. National Academies Press; 2009: 2.
Weight loss or insufficient weight gain during pregnancy in patients with obesity leads to increased risk of small-forgestational age infants and should not be advised.12 Risks of weight gain in excess of IOM recommendations (independent from prepregnancy BMI) include fetal macrosomia, gestational diabetes, operative vaginal and cesarean delivery, neonatal hypoglycemia, and admission to the neonatal intensive care unit.13
Metabolic assessment includes review of blood pressure; screening for sleep apnea, with a referral for a polysomnography if positive; and screening for pregestational diabetes. A1C measurement is recommended over oral glucose tolerance testing in early pregnancy and is considered an accurate measure of blood glucose before 15 weeks' gestation.14,15 An A1C level of 5.9% or greater is associated with adverse pregnancy and neonatal outcomes, including preeclampsia, macrosomia, shoulder dystocia, perinatal death, and an increased risk of gestational diabetes and the need for insulin treatment.15
Second Trimester
Obesity during pregnancy is associated with increased risk of congenital malformations. Aneuploidy screening should be offered to all patients; however, inconclusive cell-free DNA test results are more likely due to increased plasma volume and decreased fetal fraction associated with increasing BMI.16 An oral glucose tolerance test should be performed between 24 and 28 weeks' gestation for all patients, even if early A1C levels were normal or consistent with prediabetes.17
Third Trimester
Assessing fetal growth with ultrasonography is indicated after 32 weeks' gestation. Suspected macrosomia is not an indication for induction, but cesarean delivery should be offered for estimated fetal weight of 4,500 g or greater in those with diabetes and 5,000 g or greater in those without diabetes.18 The risk of stillbirth increases with increasing maternal BMI (absolute risk = 0.4% for a BMI of 20 kg/m2 and 0.59% for a BMI of 30 kg/m2 per 1,000 pregnancies). The risk is most pronounced for those with a BMI of 40 kg/m2 or greater (up to threefold risk).3 Weekly antenatal fetal surveillance is recommended at 34 weeks' gestation for those with class III obesity and at 37 weeks' gestation for class II obesity.19
INTRAPARTUM APPROACH
Pregnant patients with obesity are admitted earlier in labor, have longer duration of labor from induction through delivery, and have higher rates of induction and cesarean delivery.20,21 Maternal obesity is not an indication for induction before 39 weeks' gestation.22 Median traverse time (duration from 4 to 10 cm dilation) increases with rising BMI; in patients with class III obesity, it may be 2 hours longer than those with normal BMI.23 If an epidural is desired, early placement is recommended to ensure effectiveness and reduce risks associated with general anesthesia in the case of emergent cesarean delivery.3
POSTPARTUM CONSIDERATIONS
Obesity paired with higher cesarean delivery rates is associated with increased risk of postoperative surgical complications, including endomyometritis, wound infection, and wound dehiscence.3 Postpartum thromboprophylaxis is indicated for patients with obesity undergoing cesarean delivery; implementation varies by institution. Strategies include early mobilization, pneumatic leg compression devices, and pharmacologic prophylaxis with weight-based low-molecular-weight heparin for up to 6 weeks postpartum.3,24
Lactation support is important in patients with obesity due to lower breastfeeding initiation rates and shorter duration of exclusive breastfeeding.25 Risk of postpartum depression increases with increasing BMI, with rates as high as 40% in those with class III obesity. Attention should be given to education on and screening for depression during postpartum care.26
Contraception recommendations should follow Centers for Disease Control and Prevention guidelines. Although not contraindicated, combined oral contraceptives are a risk factor for venous thromboembolism, and patch effectiveness may be reduced in those with a BMI of 30 kg/m2 or greater.27

