Key Points for Practice
• The Canadian CT Head Injury/Trauma Rule is the most accurate clinical decision tool and should be used to determine the need for imaging after a head injury.
• Patients taking anticoagulants require immediate imaging after mild TBI. Observation and repeat imaging are not recommended if initial imaging and neurologic examination are normal.
• Patients at high risk for postconcussive syndrome may benefit from more physical and cognitive limitations and referral for early intervention.
From the AFP Editors
Traumatic brain injuries (TBIs) can be caused by an external force to the head or body or a penetrating injury to the head. These injuries can result in changes in cognition, sensation, language, or emotion. In mild TBI, patients have loss of consciousness for 30 minutes or less, a Glasgow Coma Scale score of 13 to 15 at least 30 minutes after injury, and transient neurologic abnormalities such as posttraumatic amnesia, focal symptoms or signs, or seizure for 24 hours or less. Up to 15% of patients with mild TBI will have evidence of intracranial injury on imaging, with 1% requiring neurosurgical intervention. The American College of Emergency Physicians (ACEP) has published new guidelines for evaluation of mild TBI.
Clinical Decision Tools
The Canadian CT Head Injury/Trauma Rule is the most accurate way to determine the need for imaging after head injury. The rule demonstrated nearly 100% sensitivity and at least 50% specificity in two large validation studies. The New Orleans/Charity Head Trauma/Injury Rule and National Emergency X-Radiography Utilization Study (NEXUS) Head CT instrument have similar sensitivity but significantly lower specificity and would lead to far more unnecessary scans.
Patients Taking Anticoagulants
Patients taking anticoagulants have an increased risk of intracranial hemorrhage after mild TBI, and immediate computed tomography is recommended. Because of a low risk of delayed hemorrhage, the ACEP does not recommend routine observation or repeat imaging if initial imaging and neurologic examination are normal, although other organizations do. Multiple studies of patients taking anticoagulants including aspirin, clopidogrel, direct-acting oral anticoagulants, heparin, and warfarin demonstrate less than 5% risk of delayed intracranial hemorrhage after 24 hours, none requiring neurosurgical intervention. Observation should be considered in older patients on antiplatelet agents who present after loss of consciousness or with amnesia or a Glasgow Coma Scale score of less than 15. Strict return criteria for symptoms of rare hemorrhage and outpatient follow-up to review fall risk and appropriateness of continued anticoagulation are recommended.
Postconcussive Syndrome
Postconcussive syndrome occurs in a subset of patients who experience a prolonged course of decreased function at home, while driving, at work, or during exercise. The most common symptoms of postconcussive syndrome are fatigue and forgetfulness. Certain factors are associated with a higher risk of the syndrome, including acute intoxication, brain injury caused by assault, female sex, Glasgow Coma Scale score of less than 15, loss of consciousness, and previous psychological history (e.g., depression). These patients may benefit from stricter precautions to limit physical and cognitive activities that exacerbate symptoms and referral for early interventions. Biomarkers and imaging findings are not recommended to identify patients at increased risk for postconcussive syndrome.
G-TRUST SCORECARD
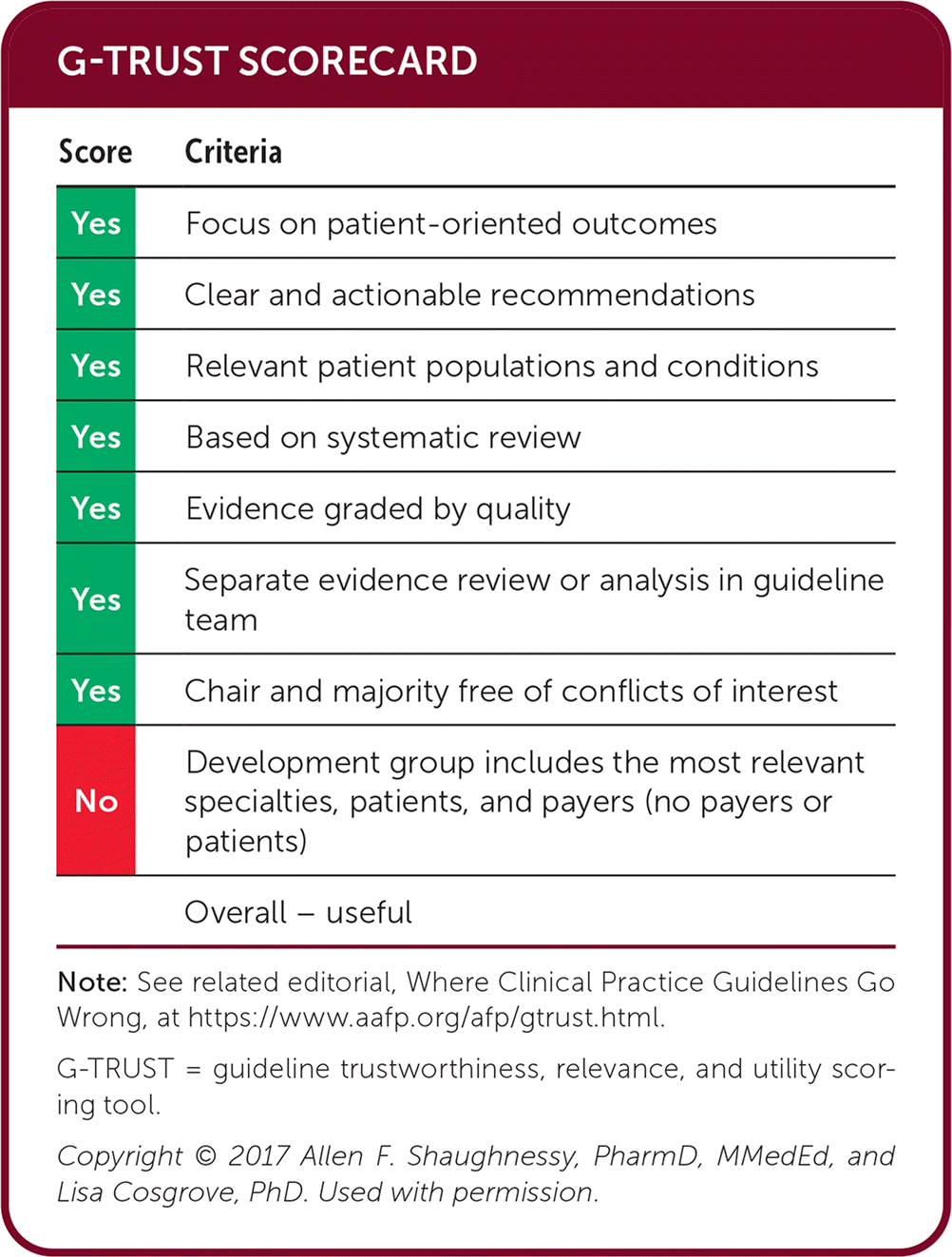
| Score | Criteria |
|---|---|
| Yes | Focus on patient-oriented outcomes |
| Yes | Clear and actionable recommendations |
| Yes | Relevant patient populations and conditions |
| Yes | Based on systematic review |
| Yes | Evidence graded by quality |
| Yes | Separate evidence review or analysis in guideline team |
| Yes | Chair and majority free of conflicts of interest |
| No | Development group includes the most relevant specialties, patients, and payers (no payers or patients) |
| Overall – useful |
Note: See related editorial, Where Clinical Practice Guidelines Go Wrong, at https://www.aafp.org/afp/gtrust.html.
G-TRUST = guideline trustworthiness, relevance, and utility scoring tool.
Copyright © 2017 Allen F. Shaughnessy, PharmD, MMedEd, and Lisa Cosgrove, PhD. Used with permission.
Editor's Note: Although written for the emergency department, these questions can help family physicians in the clinic, urgent care, or the sideline of an athletic field. Using the Canadian CT Head Injury/Trauma Rule can aid in triaging the need for emergent evaluation including imaging. Similarly, the risk factors for postconcussive syndrome can help determine how fast our patients can transition to full activity after head injury.—Michael J. Arnold, MD, Assistant Medical Editor
The views expressed are those of the author and do not necessarily reflect the official policy or position of the Naval Undersea Medical Institute, Uniformed Services University of the Health Sciences, U.S. Navy, U.S. Department of Defense, or the U.S. government.
Guideline source: American College of Emergency Physicians
Published source: Valente JH, Anderson JD, Paolo WF, et al. Clinical policy: critical issues in the management of adult patients presenting to the emergency department with mild traumatic brain injury. Ann Emerg Med. 2023; 81(5): e63–e105.

