Key Points for Practice
• Early intervention, family therapy, and supported employment services are important elements of care for first-episode psychosis.
• Schizophrenia is best managed in assertive community care models and can include aerobic activity, yoga, psychotherapy, and supported housing in addition to medication.
• Second-generation antipsychotic medications are the recommended medical therapy. Adverse effects vary, and changing medications can improve tolerability.
• Clozapine is more effective for positive symptoms but should be reserved for treatment-resistant psychosis due to serious adverse effects, including agranulocytosis.
From the AFP Editors
First-episode psychosis commonly presents in males in their early to mid-20s and females in their late 20s and is often triggered by stress. First-episode psychosis can appear as a prodrome to schizophrenia, and management can improve the severity of psychiatric illness later in life. Schizophrenia is a neurodevelopmental disorder that impacts approximately 1% of the U.S. population. Schizophrenia presents with positive symptoms including perceptual distortions, such as hallucinations and delusions, and motor deficits and negative symptoms including diminished emotional expression and significant reduction in goal-directed activities. Negative symptoms are the most important predictor of poor long-term functioning. People with schizophrenia die an average of 15 years earlier than unaffected individuals. The U.S. Department of Veterans Affairs and U.S. Department of Defense (VA/DoD) published new recommendations for diagnosing and managing schizophrenia and first-episode psychosis.
Screening for Psychosis
There are numerous screening and assessment instruments for predicting if a patient with suspected psychosis will transition to psychosis; however, they have low specificity and are recommended only for use in a specialty mental health care environment. There is insufficient evidence to recommend using biomarker screening tools. Although magnetic resonance imaging appears reasonably accurate in small studies of high-risk patients, standardized criteria are not yet available.
Management of First-Episode Psychosis
Patients with a first episode of psychosis should receive early intervention services. Early interventions include 32 evidence-based components, including family interventions and supported employment. Family interventions improve symptoms and functionality and reduce hospitalization length and future relapses compared with individual care. Individual placement and supported employment should be considered, with the goal of participation in employment or education. Use of an antipsychotic other than clozapine for initial treatment based on patient characteristics and adverse effect profiles is recommended. About five patients need to be treated with an antipsychotic for one additional response vs. placebo.
Treatment with early intervention services for 2 years improves the severity of positive and negative symptoms more than usual treatment. Although early intervention services can be extended up to 5 years, there is little evidence to support this prolonged treatment. Nearly two-thirds of people with significant psychiatric illness desire employment, but only 15% are employed. Supported employment programs for people with first-episode psychosis increase employment at 6 months or longer vs. usual treatment.
For patients with comorbid substance use disorders, family therapy reduces the severity of substance use.
Management of Schizophrenia
Treatment should be provided through assertive community care models, which include shared caseload among teams with low patient-to-staff ratios, high frequency of patient contact, direct service provision, and community outreach. This treatment can reduce hospitalizations and rates of relapse. Aerobic exercise can be considered in addition to usual treatment to reduce negative symptoms and improve functioning, and yoga may reduce positive and negative symptoms.
Adding cognitive behavior therapy to medication can improve outcomes, especially in prodromal and early psychosis. Acceptance and mindfulness-based therapy, meta-cognitive therapy, and positive psychology interventions can also be considered. Cognitive remediation training can reduce positive symptoms and improve concentration, memory, and problem solving. Social skills training can be considered, although evidence of benefit is conflicting.
Supported housing improves housing stability but not hospital admissions or medication adherence and has insufficient evidence to be recommended. Weekly telephone-based care management can reduce rehospitalizations and should be considered.
Pharmacologic Treatment of Schizophrenia
Maintenance treatment with antipsychotic medications prevents relapse (NNT = 3) and hospitalization (NNT = 10) compared with placebo. Because second-generation antipsychotics have similar improvement and different adverse effects, a trial of a different medication is recommended if the patient has intolerance or inadequate response to one medication. Long-acting injectable antipsychotics can improve medication adherence and may be considered.
Because of increased risk of serious adverse effects, clozapine should be reserved for patients with treatment-resistant psychosis, defined as an unsuccessful 6-week trial of at least two medications at effective doses. Clozapine has greater improvement in positive symptoms than other antipsychotics. The U.S. Food and Drug Administration requires a risk evaluation and mitigation strategy to ensure that patients who use clozapine are registered and blood testing requirements are met because of the risk of agranulocytosis. If there is an inadequate response to clozapine alone, adding another second-generation antipsychotic may be considered.
Treating Adverse Effects of Antipsychotics
Metformin, topiramate, and aripiprazole can be considered to improve the metabolic adverse effects of antipsychotics, including weight gain. Although some studies suggest that aripiprazole can improve hyperprolactinemia, the benefits appear limited to laboratory values without an improvement in symptoms, and the guidelines do not recommend for or against its use.
The guidelines suggest considering treatment of tardive dyskinesia with vesicular monoamine transporter 2 inhibitors, including deutetrabenazine (Austedo), tetrabenazine (Xenazine), and valbenazine (Ingrezza), which may reduce symptoms, including involuntary movements.
Clozapine can cause sialorrhea, or excessive salivation, which is best treated with diphenhydramine.
G-TRUST SCORECARD
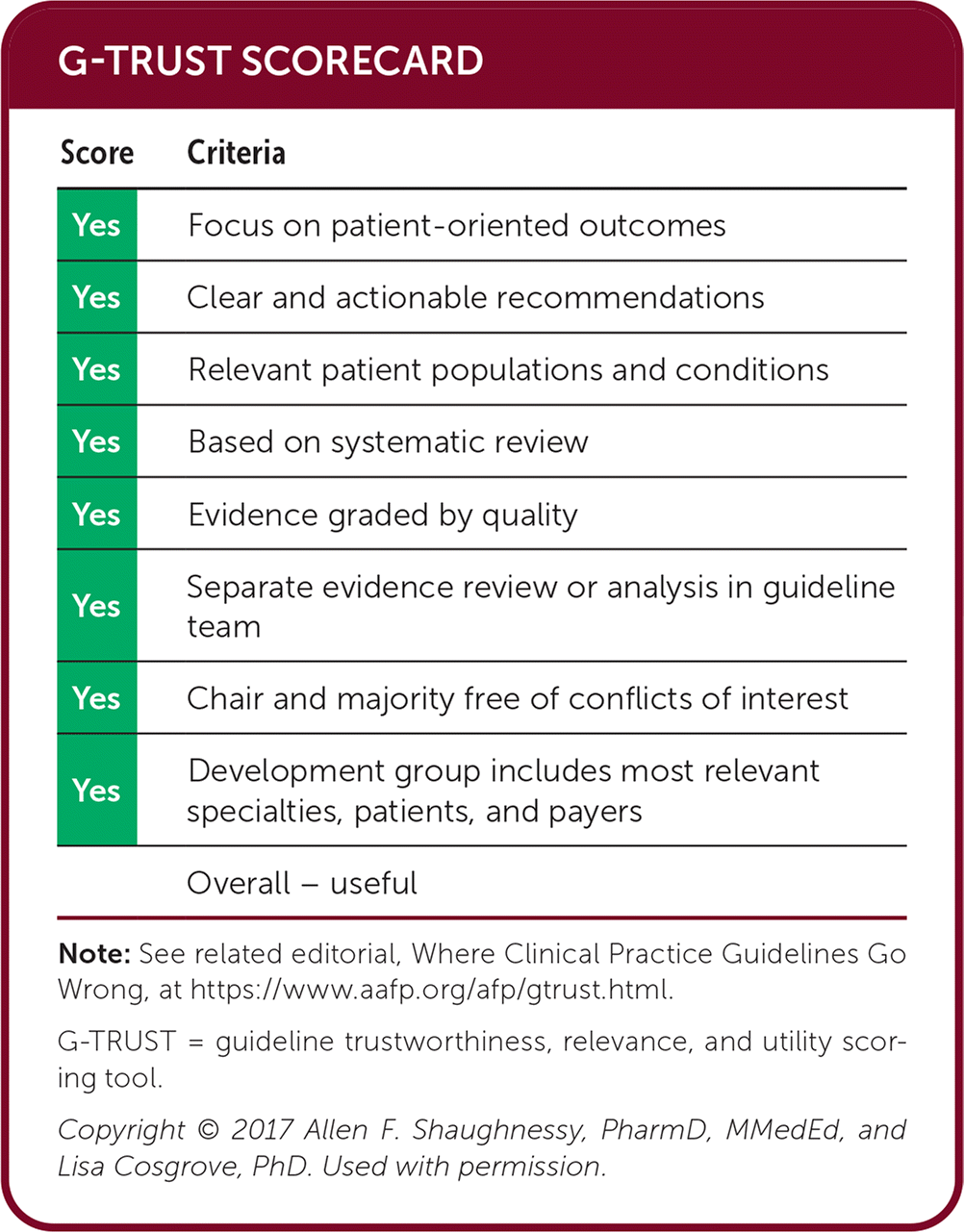
| Score | Criteria |
|---|---|
| Yes | Focus on patient-oriented outcomes |
| Yes | Clear and actionable recommendations |
| Yes | Relevant patient populations and conditions |
| Yes | Based on systematic review |
| Yes | Evidence graded by quality |
| Yes | Separate evidence review or analysis in guideline team |
| Yes | Chair and majority free of conflicts of interest |
| Yes | Development group includes most relevant specialties, patients, and payers |
| Overall – useful |
Note: See related editorial, Where Clinical Practice Guidelines Go Wrong, at https://www.aafp.org/afp/gtrust.html.
G-TRUST = guideline trustworthiness, relevance, and utility scoring tool.
Copyright © 2017 Allen F. Shaughnessy, PharmD, MMedEd, and Lisa Cosgrove, PhD. Used with permission.
Editor's Note: This evidence-based review of care for patients with schizophrenia is the first I have seen. With the current mental health professional shortage, I welcome this review to update my understanding of schizophrenia and first-episode psychosis and how care differs between the two.—Michael J. Arnold, MD, Assistant Medical Editor
The numbers needed to treat reported in this Practice Guideline were calculated by the author based on raw data provided in the original guideline.
The views expressed are those of the author and do not reflect the official policy or position of the Naval Undersea Medical Institute, U.S. Navy, U.S. Department of Defense, or U.S. government.
Guideline source: U.S. Department of Veterans Affairs and U.S. Department of Defense
Published source: VA/DoD clinical practice guideline for management of first-episode psychosis and schizophrenia; April 2023.

