Starting in the 1960s, a new specialty called family practice (later family medicine) emerged as a form of primary care, based on the biopsychosocial model of human health.1 For many, it was an exciting and inspiring time for a type of medicine grounded in care for the whole person. Family medicine, seen as a revolution by its founders in the 1960s and 1970s, was a model of care anchored in trusting relationships, prevention and health promotion, and community chronic disease management.2 It was health care for the person across their lifespan, not just for treating diseases as they arose. It was a call to be healers in the truest sense by seeing the sanctity of each person and seeking to restore individuals and communities to a sense of wholeness and well-being.3
Extensive research shows that continuous, whole person primary care, as in family medicine, improves health, prevents disease, and keeps costs down.4,5 Yet, the concept of family medicine with continuity of care over the lifespan is in decline.6,7 Corporate interests, financial pressures, and documentation needs now incentivize fragmented care and care delivered in short time frames with emphasis on advances in medical technology, medications, and procedures, which are profitable.4,5,8–11
These advances have been supported by health care policies, US Food and Drug Administration drug approvals, American Medical Association billing codes, and Medicare and Medicaid coverage. There was not, however, a similar rise in reimbursement for the time and teams needed to care for the whole person. Although the Centers for Medicare and Medicaid Services has made modest progress in payments for whole person care, the core drivers of payment tracked by Relative Value Units (RVUs) and Current Procedural Terminology (CPT) codes have not sufficiently changed. Time to build trusting relationships and maintain continuous and comprehensive care, the factors known to reduce costs and improve health over the long term, still is not adequately covered. The rise in direct primary care, whereby clinicians work directly with patients to provide all primary care for a transparent fee that bypasses insurance payment models, is a response to those inadequate changes.12
The decline in whole person care is now fully reflected in the state of our health care system and our nation's health, with decreased patient satisfaction, increased clinician burnout, rising costs, rising rates of chronic disease, and lower life expectancy than other industrialized countries.13–17 The substantial data documenting this decline and its link to the loss of whole person care have been summarized by the National Academy of Medicine.18–20
Now, more than ever, is the time to reboot family medicine as the nation's primary model for preventive and chronic disease care. The current political milieu represents both a threat and an opportunity. The desire to reduce chronic disease, lower health care costs, and bolster the agency of communities to enhance their own health and well-being cannot be accomplished without a workforce able to do it. Let's take the principles of family medicine from the 1970s and enhance them with the technologies, teams, training, and health promotion science of our modern world.
The activities needed for this revision have been described in three major reports from the National Academies of Science, Engineering, and Medicine and tested in communities of practice.21,22 Those reports show where investments can make America healthy, especially our families and children.23–25 Guideposts from the reports for renewing family medicine and operational principles are described in Table 123–25 and Table 2.22 The main drivers of health in whole person care for chronic disease in practice are listed in Table 3.
TABLE 1. Principles of Whole Person Care

| Seeing and engaging the person around what matters to them in their life goals and how health care can support those on a continuous basis. This is person-centered care, not just patient-centered care. |
| Investing in the science and services of salutogenesis (health creation) by focusing on the drivers of healing and the factors that promote well-being, rather than solely on the treatment of disease, and by giving health promotion and risk reduction equal weight to disease treatment. |
| Assuring that no personal driver of health is ignored. This means asking about and addressing the physical, behavioral, social, emotional, mental, and spiritual dimensions of a person. |
TABLE 2. Operationalizing the Principles of Whole Person Care
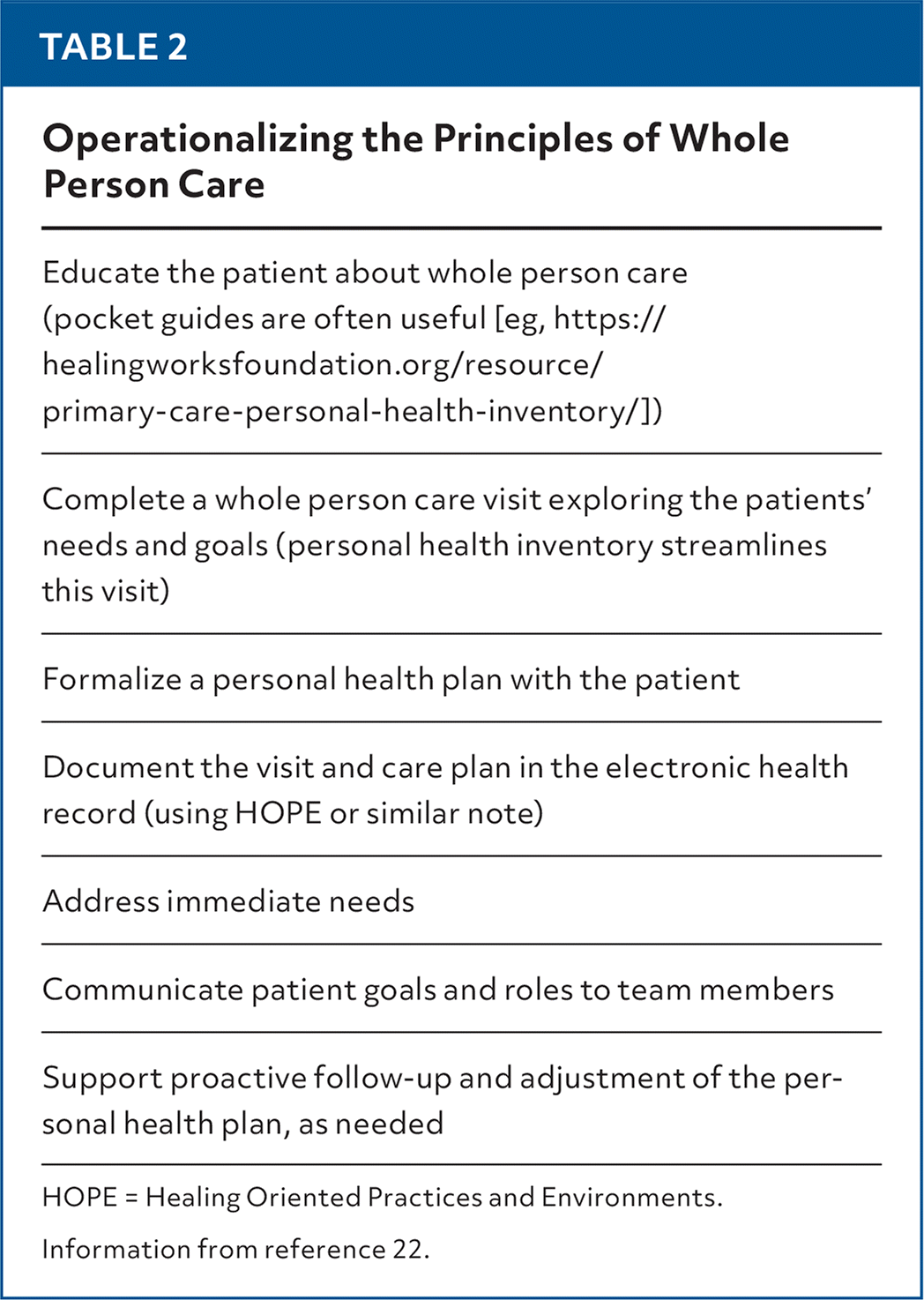
| Educate the patient about whole person care (pocket guides are often useful [eg, https://healingworksfoundation.org/resource/primary-care-personal-health-inventory/]) |
| Complete a whole person care visit exploring the patients' needs and goals (personal health inventory streamlines this visit) |
| Formalize a personal health plan with the patient |
| Document the visit and care plan in the electronic health record (using HOPE or similar note) |
| Address immediate needs |
| Communicate patient goals and roles to team members |
| Support proactive follow-up and adjustment of the personal health plan, as needed |
HOPE = Healing Oriented Practices and Environments.
Information from reference 22.
TABLE 3. Most Common Drivers of Health in Whole Person Care
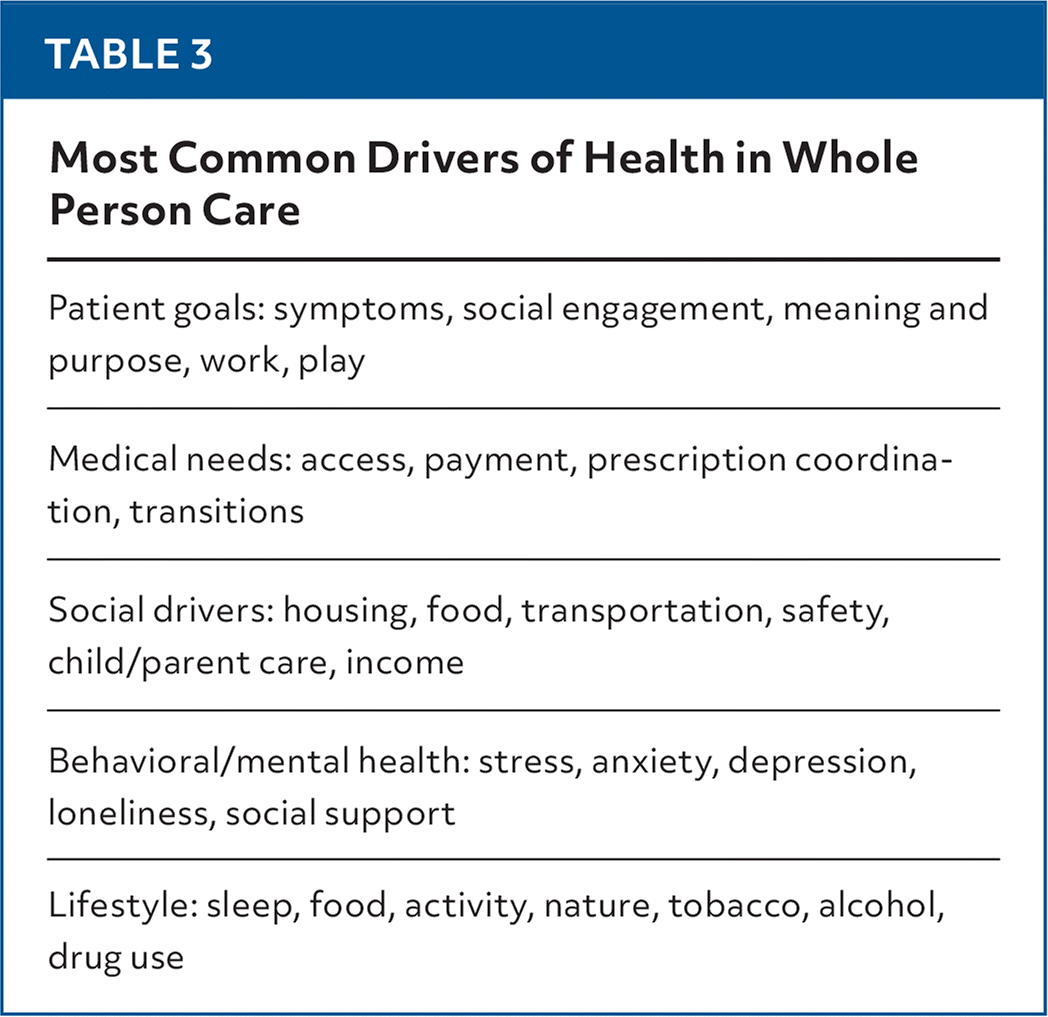
| Patient goals: symptoms, social engagement, meaning and purpose, work, play |
| Medical needs: access, payment, prescription coordination, transitions |
| Social drivers: housing, food, transportation, safety, child/parent care, income |
| Behavioral/mental health: stress, anxiety, depression, loneliness, social support |
| Lifestyle: sleep, food, activity, nature, tobacco, alcohol, drug use |
It is time for family medicine to again take the lead in articulating a renewed vision of whole person health care. Like the family medicine founders did in the 60s and 70s, we need to create a version of family medicine today that will embrace current knowledge, technology, and policy opportunities and show how this vision of care is essential and can be inspiring again.26
Editor’s Note: Dr. Shaughnessy is assistant medical editor for AFP.

